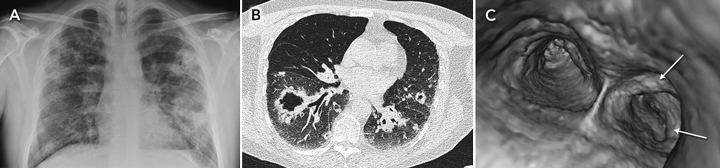
Pulmonary amyloidosis occurs in three forms: tracheobronchial (the most common, which is limited to central airways and which this case exemplifies), diffuse and adenopathy-associated.1 Nearly all cases are of the light-chain type.2 Treatment is difficult and controversial; repeated bronchoscopic resection is conventional,3 but the role of external beam radiotherapy in tracheobronchial amyloidosis has also been described.4
- Kshitij Mankad1
- Michael J Darby2
- Leeds Teaching Hospitals NHS Trust, Leeds, UK.
Correspondence: drmankad@gmail.com
- 1. Gertz MA, Greipp PR. Clinical aspects of pulmonary amyloidosis. Chest 1986; 90: 790-791.
- 2. Cordier JF, Loire R, Brune J. Amyloidosis of the lower respiratory tract: clinical and pathological features in a series of 21 patients. Chest 1986; 90: 827-831.
- 3. Utz JP, Swensen SJ, Gertz MA. Pulmonary amyloidosis. The Mayo Clinic experience from 1980 to 1993. Ann Intern Med 1996; 124: 407-413.
- 4. Neben-Wittich MA, Foote RL, Kalra S. External beam radiation therapy for tracheobronchial amyloidosis. Chest 2007; 132: 262-267.
Online responses are no longer available. Please refer to our instructions for authors page for more information.




