Somatization, a tendency to experience and communicate somatic distress in response to psychosocial stress and to seek medical help for it, poses a major medical, social, and economic problem . . . Its persistent form is especially costly and difficult to prevent and manage.1
Somatic symptoms are a frequent presentation of distress in general practice, and up to 30% of common somatic symptoms go undiagnosed.2 Somatisation comprises the three elements of: (i) unexplained physical symptoms in the context of psychosocial stress; (ii) an attribution of physical illness; and (iii) medical help-seeking. Recent practice has tended to pay particular attention to “medically unexplained symptoms”,3 although there has been encouragement for us to focus less on “symptom count” and more on the psychopathology4 — the bodily preoccupation and somatic conviction.
One of the interesting issues in somatisation is its relationship to depression and anxiety. Psychoanalytical thinking saw somatisation as a “conversion” of emotional stress into somatic distress. In many eastern countries, the diagnosis of depression is not common, while neurasthenia (characterised by predominant fatigue) is a common diagnosis.5 Studies in Western countries, however, have shown a correlation between somatic complaints and depression or anxiety.2 Emotional and somatic complaints may be alternate ways that humans show distress.
Patient questionnaires sought information on basic demographic details and included the following:
The Patient Health Questionnaire (PHQ-15), a 15-item scale that measures somatic symptom severity.6 It enquires about 15 common somatic symptoms, inviting a response of “not bothered at all”, “bothered a little” or “bothered a lot”, scored 0–2. The highest possible score for women is 30, and for men is 28 (one item pertains to menstrual problems). The PHQ-15 does not ascertain whether symptoms are medically explained or unexplained, although a high score is strongly associated with physician-rated somatoform disorder symptom counts.7,8 Total scores in the ranges 0–4, 5–9, 10–14 and 15–30 on the PHQ-15 define “minimal”, “low”, “medium” and “high” somatic symptom severity.6
The seven-item version of the Whiteley Index (Whiteley-7), which measures hypochondriasis (health anxiety, fears of illness and the tendency to make somatic attributions).9 Each item invites a “yes” or “no” response (scored one and zero, respectively), with people scoring three or more being considered high scorers.10,11
The Kessler Psychological Distress Scale (K10), which measures psychological distress, and specifically symptoms of depression and anxiety in the previous 30 days. Its 10 questions have response options ranging from “none of the time” to “all of the time” on a five-point Likert-style scale scored 1–5. We used a score of 30 or more to define “probable caseness”, this being the cut-off used in the Australian National Survey of Mental Health and Wellbeing.12 Such a score indicates ten times the population risk for meeting diagnostic criteria for anxiety or depression.13
Cases missing more than 20% of the patient-survey data were removed from the sample.14 GPs performed the audit on two separate occasions, resulting in some patients being included twice: data from repeat visits were removed. Multivariate outliers across the three self-report measures were identified by means of the calculation of Mahalanobis distance and removed from the sample. We ran separate missing value analyses using the multiple imputation method14 to impute missing values in each of the three measures within the patient survey.
Differences between groups were examined with χ2 tests for categorical data and Student’s t test for dimensional variables. Analysis of covariance (ANCOVA) was used to examine for the effect of sex, with partial eta squared (ηp2) indicating size of effect. Cohen’s kappa (κ)15 was used to examine the agreement between GPs’ audit forms and patient questionnaires on the assessment of somatisation.
Characteristics of the final sample are shown in Box 1. There were significantly more women than men in the final sample (68.9% v 31.1%; χ2 = 1505.33; P < 0.001), and the women were significantly younger than the men (t[10 489] = 11.68; P < 0.001).
Descriptive statistics for the three psychometric measures (PHQ-15, Whiteley-7 and K10) are shown in Box 2. About 30% of the sample had medium to high somatic symptom severity (PHQ-15); a similar percentage had high hypochondriasis (Whiteley-7); and 9.5% had high psychological distress (K10).
One-way ANCOVAs were conducted to examine the effect of sex, while controlling for age, on the three psychometric measures (see Box 3).
Women had significantly more severe somatic symptoms (PHQ-15) than men after controlling for age; however, the size of the effect was small (F[1,10 488] = 174.55; P < 0.001; ηp2 = 0.016). In addition, there was a weak though significant relationship between age and PHQ-15 (ηp2 = 0.016).
0.567 for PHQ-15 scores and Whiteley-7 scores;
0.619 for PHQ-15 scores and K10 scores; and
0.493 for Whiteley-7 scores and K10 scores.
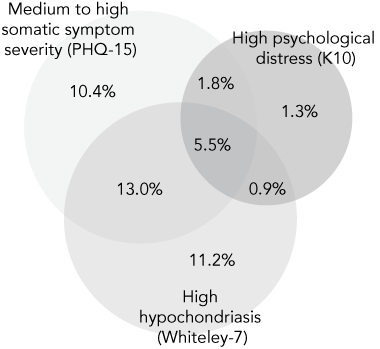
Box 4 shows the overlap between the psychometric measures based on dichotomised scores. Distress in at least one of the three domains affected 44.1% of the population exhibited, while 21.2% exhibited distress in at least two domains. Only 1.3% had high psychological distress without either medium to high somatic symptom severity or hypochondriasis — that is, depression and anxiety symptoms were uncommon without hypochondriasis or significant somatic symptoms. On the other hand, hypochondriasis and somatic symptoms alone were not uncommon (11.2% and 10.4%, respectively).
Box 5 presents a 2 × 2 table showing the agreement between GP attribution of somatisation and patients identified as somatisers by the psychometric measures on the patient questionnaire. Overall agreement was 74% (κ = 0.132; P ≤ 0.001). Although statistically significant, this κ value (which gives a chance-corrected measure of agreement15) indicates only slight agreement.16 GPs correctly identified only 25.1% of the patients identified as somatisers by the questionnaires. For patients who also expressed emotional distress (ie, had a K10 score of ≥ 30), GP recognition of somatisation was slightly higher (33.5% of distressed somatisers v 21.8% in the non-distressed).
Somatisation is one of the commonest psychiatric disorders in the community, although its prevalence has been difficult to measure. In this study, we used the generally accepted three-part definition of somatisation, including multiple physical symptoms, hypochondriasis (fear of illness and tendency towards somatic attribution) and help-seeking (in this case, attending a GP). We did not conduct an independent medical assessment and could not ascertain whether physical symptoms were medically unexplained. However, high somatic symptom counts do correlate with somatoform symptoms,17 and combining somatic symptom severity with hypochondriasis, each independently a good measure of somatisation, produces a fairly conservative measure. It might appear somewhat surprising therefore that 18.5% of our sample were considered somatisers. However, this finding is similar to that of a very large international study conducted by the World Health Organization that found somatisation in 20% of primary care attenders.18 Other studies have also reported similar figures.19,20
Much emphasis in general practice is given to finding the disease underlying a physical symptom. We know that many symptoms (around 30%) presenting to GPs do not have a cause identified.2,21 Many of these resolve within a few weeks,22 but some persist up to 5 years.23 The WHO study found that patients with five or more somatic symptoms had significantly increased morbidity and physical disability at follow-up, with little difference in outcome between patients with medically explained and unexplained symptoms.24 Thus, although finding or excluding organic disease is important, it is not the end of the story.
An important issue in general practice is whether “distress” is recognised. Unfortunately, most patients with depression and anxiety who present to GPs complain of somatic symptoms rather than volunteering psychological symptoms. On the other hand, most patients with depression and anxiety will admit to psychological symptoms if specifically asked about them.25 However, somatisation does significantly reduce the likelihood of GPs recognising depression or anxiety.26 The recognition rate in our study (25%) was a little lower than those in studies from the United Kingdom (39% to 57%)27 and Europe (36% to 48%).28
Patients who somatise are among the most difficult to manage, yet can be helped once the focus is moved away from the physical symptoms and on to the (bodily) concerns and worries — the hypochondriasis.29 A number of things have been shown to be helpful. Reassurance, with good information based on an honest and trusting doctor–patient relationship, and a proper assessment, is critically important. “It is easier to persuade the patient that an illness is not serious if the complaint itself is obviously being considered seriously”.30
Reattribution is a simple technique for moving patients from a somatic preoccupation to a consideration of their emotional distress.31 Early trials suggest it is helpful for many patients, but not for those with a very strong somatic attribution.32-35 Cognitive behaviour therapy and interpersonal psychotherapy are generally effective in reducing illness concerns, anxiety, depression and use of health care services.36-39 There is also evidence from meta-analyses for the efficacy of antidepressant drugs in patients with various somatic syndromes (irritable bowel syndrome, fibromyalgia, low back pain, and others).40-42 Most of these studies have involved tricyclic antidepressants; there is only preliminary evidence for the effectiveness of the newer antidepressants.43
Although these treatments are generally beneficial, there is a group of patients with chronic and polysymptomatic somatisation for whom these treatments do not lead to lasting and clinically significant improvement.44 These patients are best managed in the same way as if they had any chronic illness. Regular appointments help to keep anxieties down and urgent consultations to a minimum. A consultation with a specialist in psychological medicine, with a letter to the GP, can further help bring a sense of control, and has been shown to lead to reduced use of health care.45 Avoiding unnecessary interventions with their associated risk of iatrogenic effects is important.
A stepped care model may be beneficial.46 The condition of some patients will improve with a careful assessment and reassurance. Reattribution, with or without screening for depression and anxiety, followed by appropriate treatment will help a further group. Finally, there is a group of patients with persistent somatisation who require continued monitoring, support and case management. Inevitably, a number will go on to manifest disease, and GPs need to remain vigilant.
This is the first large study of somatisation in Australian general practice. The results are consistent with overseas research indicating that somatisation is more prevalent than other better recognised psychiatric diagnoses. Its nature makes it difficult to recognise and to treat. As a consequence, it places an exaggerated burden on both generalist and specialist health services. Patients who somatise use about twice as much outpatient and inpatient medical care and cost twice as much in medical care annually as patients who do not somatise.8,17 Some work has been done to develop models of care that can cope with this complexity, the aim of which is, as with other chronic diseases, “to cure sometimes, to relieve often, to comfort always”.47 The reduction of intrusive physical symptoms, anxiety and depression, and an increase in daily function is a realistic hope for patients who somatise.48 Effective strategies need to be developed and trialled, and health professionals need to be educated if we are to reduce the suffering of this group of patients, and the frustration of their health carers.
2 Total and dichotomised scores for the sample of 10 507 patients on the Patient Health Questionnaire (PHQ-15), Whiteley Index (Whiteley-7) and the Kessler Psychological Distress Scale (K10)
3 Scores for the sample of 10 507 patients on the Patient Health Questionnaire (PHQ-15), Whiteley Index (Whiteley-7) and the Kessler Psychological Distress Scale (K10), adjusted and unadjusted for age
Mean score adjusted for age (SE) |
|||||||||||||||
4 Venn diagram showing the overlap between affected proportions of the sample on the three psychometric measures*
 | |||||||||||||||
Received 29 April 2008, accepted 13 August 2008
- David M Clarke1
- Leon Piterman1
- Claire J Byrne1
- David W Austin2
- 1 Monash University, Melbourne, VIC.
- 2 Swinburne University of Technology, Melbourne, VIC.
This study was supported by a grant from Wyeth Pharmaceuticals and was conducted in parallel with a national educational program funded by Wyeth known as Time Efficient Mental Health.
Wyeth provided financial support for this study, but did not contribute to the design, data analysis, interpretation or writing of the study.
- 1. Lipowski ZJ. Somatization: the concept and its clinical application. Am J Psychiatry 1988; 145: 1358-1369.
- 2. Kroenke K, Spitzer RL, Williams JBW, et al. Physical symptoms in primary care: predictors of psychiatric disorders and functional impairment. Arch Fam Med 1994; 3: 774-779.
- 3. Sharpe M. Medically unexplained symptoms and syndromes. Clin Med 2002; 2: 501-504.
- 4. Fink P. Somatization: beyond symptom count. J Psychosom Res 1996; 40: 7-10.
- 5. Yen S, Robins CJ, Lin N. A cross-cultural comparison of depressive symptom manifestation: China and the United States. J Consult Clin Psychol 2000; 68: 993-999.
- 6. Kroenke K, Spitzer RL, Williams JBW. The PHQ-15: validity of a new measure for evaluating the severity of somatic symptoms. Psychosom Med 2002; 64: 258-266.
- 7. Kroenke K, Spitzer RL, deGruy FV 3rd, Swindle R. A symptom checklist to screen for somatoform disorders in primary care. Psychosomatics 1998; 39: 263-272.
- 8. Barsky AJ, Orav EJ, Bates DW. Somatization increases medical utilization and costs independent of psychiatric and medical co-morbidity. Arch Gen Psychiatry 2005; 62: 903-910.
- 9. Fink P, Ewald H, Jensen J, et al. Screening for somatization and hypochondriasis in primary care and neurological in-patients: a seven-item scale for hypochondriasis and somatization. J Psychosom Res 1999; 46: 261-273.
- 10. Hansen MS, Fink P, Frydenberg M, et al. Complexity of care and mental illness in medical inpatients. Gen Hosp Psychiatry 2001; 23: 319-325.
- 11. Hansen MS, Fink P, Søndergaard L, Frydenberg M. Mental illness and health care use: a student among new neurological patients. Gen Hosp Psychiatry 2005; 27: 119-124.
- 12. Australian Bureau of Statistics. Information paper: use of the Kessler Psychological Distress Scale in ABS health surveys. Canberra: ABS, 2003. (ABS Cat. No. 4817.0.55.001.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/productsbyCatalogue/B9ADE45ED60E0A1CCA256D2D0000A288?OpenDocument (accessed Oct 2008).
- 13. Andrews G, Slade T. Interpreting scores on the Kessler psychological distress scale (K10). Aust N Z J Public Health 2001; 25: 494-497.
- 14. Roth P. Missing data: a conceptual review for applied psychologists. Pers Psychol 1994; 47: 537-560.
- 15. Cohen J. A coefficient of agreement for nominal scales. Educat Psychol Measure 1960; 20: 37-46.
- 16. Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics 1977; 33: 159-174.
- 17. Barsky AJ, Orav EJ, Bates DW. Distinctive patterns of medical care utilization in patients who somatise. Med Care 2006; 44: 803-811.
- 18. Gureje O, Simon GE, Ustun TB, Goldberg DP. Somatization in cross-cultural perspective: a World Health Organization study in primary care. Am J Psychiatry 1997; 154: 989-995.
- 19. Toft T, Fink P, Oernboel E, et al. Mental disorders in primary care: prevalence and co-morbidity among disorders. Results from the Functional Illness in Primary care (FIP) study. Psychol Med 2005; 35: 1175-1184.
- 20. de Waal MW, Arnold IA, Eekhow JA, van Hemert AM. Somatoform disorders in general practice: prevalence, functional impairment and co-morbidity with anxiety and depressive disorders. Br J Psychiatry 2004; 184: 470-476.
- 21. Khan AA, Khan A, Harezlak J, et al. Somatic symptoms in primary care: etiology and outcome. Psychosomatics 2003; 44: 471-478.
- 22. Kroenke K, Jackson JL. Outcome in general medical patients presenting with common symptoms: a prospective study with a two-week and three-month follow-up. Fam Pract 1998; 15: 398-403.
- 23. Jackson JL, Passamonti ML. Symptoms in primary care: outcomes at five years [abstract]. J Gen Intern Med 2001; 16 Suppl 1: 142.
- 24. Kisely S, Simon G. An international study comparing the effect of medically explained and unexplained somatic symptoms on psychosocial outcome. J Psychosom Res 2006; 60: 125-130.
- 25. Simon GE, Von Korff M, Piccinelli M, et al. An international study of the relation between somatic symptoms and depression. N Engl J Med 1999; 341: 1329-1335.
- 26. Herrán A, Vázquez-Barquero JL, Dunn G. Recognition of depression and anxiety in primary care: patient attributional style is important. BMJ 1999; 318: 1558.
- 27. Peveler R, Kilkenny L, Kinmonth A-L. Medically unexplained physical symptoms in primary care: a comparison of self-report screening questionnaires and clinical opinion. J Psychosom Res 1997; 42: 245-252.
- 28. Fink P, Sørensen L, Engberg M, et al. Somatization in primary care: prevalence, health care utilization, and general practitioner recognition. Psychosomatics 1999; 40: 330-338.
- 29. Blackwell B, De Morgan NP. The primary care of patients who have bodily concerns. Arch Fam Med 1996; 5: 457-463.
- 30. Kessel N. Reassurance. Lancet 1979; 1: 1128-1133.
- 31. Gask L. Management in primary care. In: Mayou R, editor. The treatment of functional somatic symptoms. Oxford: Oxford University Press, 1995: 391-409.
- 32. Morriss RK, Gask L, Ronals C, et al. Clinical and patient satisfaction outcomes of a new treatment for somatized mental disorder taught to general practitioners. Br J Gen Pract 1999; 49: 263-267.
- 33. Larisch A, Schweickhardt A, Wirsching M, Fritzsche K. Psychosocial interventions for somatizing patients by the general practitioner: a randomized controlled trial. J Psychosom Res 2004; 57: 507-514.
- 34. Rosendal M, Olesen F, Fink P, et al. A randomized controlled trial of brief training in the assessment and treatment of somatization in primary care: effects on patient outcome. Gen Hosp Psychiatry 2007; 29: 364-373.
- 35. Rief W, Martin A, Rauh E, et al. Evaluation of general practitioners’ training: how to manage patients with unexplained physical symptoms. Psychosomatics 2006; 47: 304-311.
- 36. Barsky AJ, Ahern DK. Cognitive behavioural therapy for hypochondriasis: a randomized controlled trial. JAMA 2004; 291: 1464-1470.
- 37. Kroenke K, Swindle R. Cognitive-behavioural therapy for somatization and symptom syndromes: a critical review of controlled clinical trials. Psychother Psychosom 2000; 69: 205-215.
- 38. Guthrie E, Creed F, Dawson D, Tomensen B. A randomised controlled trial of psychotherapy in patients with refractory irritable bowel syndrome. Br J Psychiatry 1993; 163: 315-321.
- 39. Reuber M, Burness C, Hoelett S, et al. Tailored psychotherapy for patients with functional neurological symptoms: a pilot study. J Psychosom Res 2007; 63: 625-632.
- 40. O’Malley PG, Balden E, Tomkins G, et al. Treatment of fibromyalgia with antidepressants: a meta-analysis. J Gen Intern Med 2000; 15: 659-666.
- 41. Jackson JL, O’Malley PG, Tomkins G, et al. Treatment of functional gastrointestinal disorders with antidepressant medications: a meta-analysis. Am J Med 2000; 108: 65-72.
- 42. Salerno SM, Browning R, Jackson JL. The effect of antidepressant treatment on chronic back pain: a meta-analysis. Arch Intern Med 2002; 162: 19-24.
- 43. Kroenke K. Efficacy of treatment for somatoform disorders: a review of randomized controlled trials. Psychosom Med 2007; 69: 881-888.
- 44. Allen LA, Escobar JI, Lehrer PM, et al. Psychosocial treatments for multiple unexplained physical symptoms: a review of the literature. Psychosom Med 2002; 64: 939-950.
- 45. Smith GR, Rost K, Kashner TM. A trial of the effect of a standardised psychiatric consultation on health outcomes and costs in somatising patients. Arch Gen Psychiatry 1995; 52: 238-243.
- 46. Kroenke K. Patients presenting with somatic complaints: epidemiology, psychiatric co-morbidity and management. Int J Methods Psychiatr Res 2003; 12: 34-43.
- 47. Gordon J. Medical humanities: to cure sometimes, to relieve often, to comfort always. Med J Aust 2005; 182: 5-8. <MJA full text>
- 48. Janca A, Isaac M, Ventouras J. Toward better understanding and management of somatoform disorders. Int Rev Psychiatry 2006; 18: 5-12.





Abstract
Objective: To measure the prevalence of somatisation (multiple somatic symptoms and hypochondriasis) among Australian general practice attendees, its recognition by general practitioners, and its relationship with symptoms of depression and anxiety.
Design, setting and participants: Self-reported questionnaires completed by 10 507 consecutive patients aged ≥18 years attending 340 GPs enrolled in a 6-hour national mental health program of continuing professional development who accepted invitations to participate; audit form completed by GPs for each patient during the period March 2004 to December 2006.
Main outcome measures: Somatic symptom severity (measured with the 15-item Patient Health Questionnaire [PHQ-15]); hypochondriasis (measured with the Whiteley Index [Whiteley-7]; depression and anxiety (measured by the Kessler Psychological Distress scale [K10]); prevalence of “somatisers” (defined by medium to severe somatic symptom severity and hypochondriasis); GP recognition of somatisation (determined by their responses on audit forms to questions on whether patient’s complaints were most likely to have a physical or psychological explanation).
Results: 18.5% of patients were classified as somatisers and 9.5% as probable cases of depression or anxiety. While 29.6% of somatisers had high anxiety or depression scores, 57.9% of people with anxiety or depression were also somatisers. Sex and age asserted significant but weak effects on psychometric scores. GPs identified somatic complaints as “mostly explained by a psychological disturbance” in 25.1% of somatisers.
Conclusions: Somatisation is common in general practice, and more prevalent than depression or anxiety. While a minority of somatisers have significant anxiety and depression, most patients with depression and anxiety have a significant degree of somatisation. Recognition of depression and anxiety can be hindered by a somatic presentation and attribution. On the other hand, managing somatisation does not just involve recognising depression and anxiety, but also dealing with the health anxieties that underpin hypochondriasis.