In Australia, over the past decade, considerable research and many government programs have focused on ways to increase medical workforce supply, recruitment and retention.1-5 The limited success achieved to date in redressing rural and remote medical workforce undersupply has stimulated a call for “a continuing and holistic overview of what is actually happening at the grassroots level in providing rural and remote communities with appropriate and safe health care”, rather than any more surveys on recruitment and retention.6
The problem of how to provide accessible, sustainable, appropriate health care services is most acute in small rural and remote communities, where the increased costs and difficulties of workforce recruitment and retention are compounded by the lack of economies of scale associated with servicing small populations dispersed over vast distances. Research on the need to ensure the provision of sustainable health services has been limited.7-10
For this reason, our systematic review identifying the key requirements underpinning sustainable health care services to meet the diverse health needs of small rural and remote communities in Australia is timely.11 Here we present the highlights of our review.
Geographically large countries like Australia and Canada face enormous problems in servicing the health needs of their populations.12,13 In Australia, various health care models have evolved to meet the needs of non-metropolitan inhabitants. Where populations are insufficient to meet the range and threshold requirements necessary to support local health care services, consumers have to travel long distances to larger regional centres or depend on visiting services at irregular intervals, with emergency care provided by the Royal Flying Doctor Service or air ambulance.14 Alternatively, consumers forgo care or present late — factors that arguably contribute to the poorer health status of rural and remote residents.15,16
While the role of general practice within PHC services is central, the dominant doctor-centred, fee-for-service model may not necessarily be the optimal service delivery model in rural and remote areas.17 Increasingly, the need to adopt a comprehensive PHC model involving multidisciplinary teams is recognised. Indeed, Starfield has argued that a PHC approach yields the best health outcomes, particularly in situations of limited resources.18,19
Our methodology, outlined in detail elsewhere,11 identified 68 of some 5391 initial meta-database “hits” that met the search criteria — namely, English-language reports on Australian rural and remote PHC models based on primary or secondary evidence about structural and financial aspects of sustainable service provision.
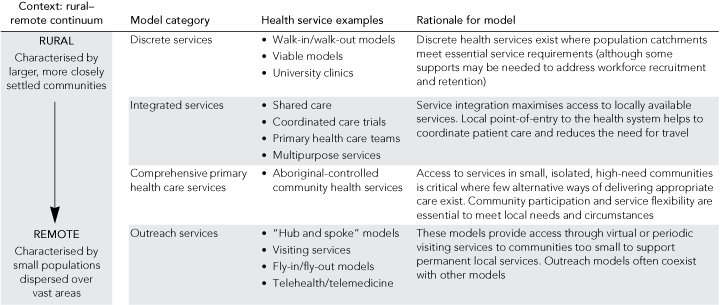
Our review identified several rural and remote PHC models (Box 1). In recognition of the diversity of rural and remote regions, the actual health service configurations differ significantly. Communities with sufficient population size are able to support discrete health care services, while smaller, more dispersed populations depend on integrated or outreach arrangements.11
Each successful primary health service model, regardless of its specific design, is characterised by common inter-related and interdependent factors that underpin its sustainability (Box 2). These requirements comprise macro-scale environmental enablers and specific requirements operating at the service level.
At the macro level, the policy environment must be conducive to facilitating services that take account of the specific health needs and circumstances of rural and remote communities that are not adequately met through mainstream programs and models. Small rural communities often suffer because national and state policies do not fit every case. In a federated political system, governments at all levels need to agree on outcomes that guide the purpose and nature of the health service in order to avoid unnecessary duplication of function, responsibility and funding of the service, and at the same time allow flexibility. The Primary Health Care Access Program and the Aboriginal Coordinated Care Trials are examples of approaches that have allowed for cashing out and pooling of funds in order to meet specific circumstances.11 Concurrent with this flexibility, local community involvement with planning, development and evaluation of a service is crucial to ensure acceptance and harmonious working relationships and to maximise the use of services.
Firstly, the inter-relationship between the essential service requirements of sustainable PHC services highlights the need for a systems approach in which components of sustainability are identified and their inter-relationships measured.8 Focusing solely on individual components (such as workforce supply) without regard to their relationship to, and the importance of, related parts has had limited impact. Sustainable solutions depend on systematically addressing all the requirements outlined in Box 2.
Secondly, the provision of appropriate, sustainable PHC services in small rural and remote communities requires fitting local solutions within a wider conducive political environment.20 The importance of macro-scale health policies and funding paradigms that underpin the environment of what is possible and what is likely to be supported should not be underestimated. Micro-scale service interventions that are not congruent with macro-scale policies are unlikely to yield sustainable results. Within a rapidly changing health environment, rural and remote health services need to maximise their ability to capitalise on new policy and program opportunities that facilitate local flexibility and make management changes necessary to meet local needs. The importance of developing a harmonious relationship between governments, health services, practitioners and communities that is characterised by effective communication and shared goals is especially vital in developing and maintaining appropriate, sustainable health services in small rural and remote communities.
2 Enablers and requirements of sustainable rural and remote primary health care services
- John S Humphreys1
- John Wakerman2
- Robert Wells3,4
- Pim Kuipers2
- Judith A Jones1
- Phil Entwistle2
- 1 School of Rural Health, Monash University, Bendigo, VIC.
- 2 Centre for Remote Health (a joint centre of Flinders University and Charles Darwin University), Alice Springs, NT.
- 3 Menzies Centre for Health Policy, Canberra, ACT.
- 4 College of Medicine and Health Sciences, Australian National University, Canberra, ACT.
None identified.
- 1. Holub L, Williams B. The General Practice Rural Incentives Program, development and implementation: progress to date. Aust J Rural Health 1996; 4: 117-127.
- 2. Humphreys JS, Lyle D, Wakerman J, et al. Roles and activities of the Commonwealth Government university departments of rural health. Aust J Rural Health 2000; 8: 120-133.
- 3. Joyce CM, Stoelwinder JU, McNeil JJ, et al. Riding the wave: current and emerging trends in graduates from Australian university medical schools. Med J Aust 2007; 186: 309-312. <MJA full text>
- 4. Lawson KA, Chew M, Van Der Weyden MB. A revolution in rural and remote Australia: bringing health education to the bush. Med J Aust 2000; 173: 618-624. <MJA full text>
- 5. Productivity Commission. Australia’s health workforce. Research report. Canberra: Productivity Commission, 2005.
- 6. Kamien M, Cameron WI. Solving the shortage of general practitioners in remote and rural Australia: a Sisyphean task? Med J Aust 2006; 185: 652-653. <MJA full text>
- 7. Bryant L, Strasser R. The delivery of sustainable rural and remote health services. Background paper for the Regional Australia Summit. Canberra: Department of Transport and Regional Services, 1999. http://www.infrastructure.gov.au/regional/forum/summit/back_sub/background_papers/pdf/strasser_paper.pdf (accessed Aug 2007).
- 8. Humphreys JS, Wakerman J, Wells R. What do we mean by sustainable health services? Implications for rural health research. Aust J Rural Health 2006; 14: 33-35.
- 9. Kamien M. The viability of general practice in Australia. Med J Aust 2004; 180: 318-319. <MJA full text>
- 10. Rural Doctors’ Association of Australia and Monash University School of Rural Health. Viable models of rural and remote practice. Canberra: RDAA, 2003.
- 11. Wakerman J, Humphreys J, Wells R, et al. A systematic review of primary health care delivery models in rural and remote Australia 1993–2006. Canberra: Australian Primary Health Care Research Institute, 2006. http://www.anu.edu.au/aphcri/Domain/RuralRemote/Final_25_Wakerman.pdf (accessed Aug 2007).
- 12. Humphreys JS, Dixon J. Access and equity in Australian rural health services. In: Healy J, McKee M, editors. Accessing health care: responding to diversity. Oxford: Oxford University Press, 2004: 89-107.
- 13. Romanow RJ, commissioner. Building on values: the future of health care in Canada. Final report. Ottawa: Commission on the Future of Health Care in Canada, 2002.
- 14. Humphreys JS. Health service models in rural and remote Australia. In: Wilkinson D, Blue I, editors. The new rural health: an Australian text. Oxford: Oxford University Press, 2002: 273-296.
- 15. Australian Health Ministers’ Advisory Council and National Rural Health Alliance. Healthy horizons: a framework for improving the health of rural, regional and remote Australians. Canberra: National Rural Health Policy Sub-committee and National Rural Health Alliance, 2002.
- 16. Australian Institute of Health and Welfare. Rural, regional and remote health — indicators of health. Canberra: AIHW, 2005. (AIHW Cat. No. PHE 59; Rural Health Series No. 5.)
- 17. McDonald J, Hare L. The contribution of primary and community health services. Sydney: University of New South Wales, 2004.
- 18. Starfield B. Primary care: is it essential? Lancet 1994: 344: 1129-1133.
- 19. Starfield B. Primary care: balancing health needs, services and technology. Oxford: Oxford University Press, 1998.
- 20. Kingdon JW. Agendas, alternatives, and public policies. New York: Longman, 2003.





Abstract
Successful, “innovative” primary health care (PHC) models exist that have adapted to the specific circumstances of their rural and remote context.
A typology of discrete, integrated, comprehensive and outreach rural and remote services exists rather than a “one coat fits all” PHC health service model.
Successful models are characterised by macro-scale environmental enablers (supportive health policy, federal–state relations, and community readiness) and five essential service requirements (workforce organisation and supply; funding; governance, management and leadership; linkages; and infrastructure).
Service sustainability depends on ensuring that key systemic service requirements are met at the local level in ways that accord with, and are supported by, the broader macro-scale environmental enablers.
Based on these principles, these model types are amenable to generalisation and evaluation in other regions.