Modern hospitals and health services are organisationally complex entities,1 employing several thousand staff working in professional, functional and geographic groups. Each group has an internal, usually hierarchical, structure, and orientates its work by the views held within its dominant professional or organisational membership. Groups cherish their autonomy, so that medical or surgical divisions view the world from their medical or surgical perspective.
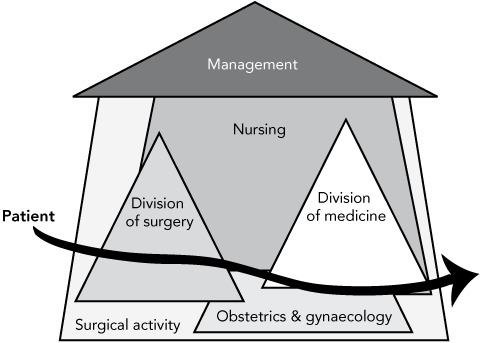
Patients, however, move horizontally across hospitals (Box 1). Their journeys take them from unit to unit, receiving care from different groups as they go. The patient is the only person who sees the whole journey. Staff only see the component for which they are responsible, and no single staff member oversees all the steps in a patient’s journey. The result is that poor coordination of the patient journey is common.
Mapping the patient journey needs careful planning and facilitation to prevent the “blame game” (ie, each group blaming other groups for the problems within the journey).2 The first rule of a mapping session is that it must record what the process is, not what people think it should be. Subsequently, the views of individuals need to be confirmed with data in order to distinguish between rhetoric and fact.
Patients who make the journeys are the only ones who can identify the problems from their perspective. The experiences of patients and carers need to be captured in the mapping stage, and patients and carers must also participate in solution design. This can be through combined staff–patient working parties, or by having separate consumer working parties. In more recent projects in New South Wales, each redesign team has been asked to interview 10 patients and carers about their experiences and analyse their stories for themes reflecting the eight dimensions identified by the Picker Institute.3 The redesign teams then use this information to design their solutions, and remeasure the patient and carer experiences at a later date to ensure there have been sustained improvements.
why a particular step occurs;
what can be changed;
what steps really add value and have an impact on patient outcomes; and
what steps do not add value and can be eliminated.
We need to question in whose interest the current system is organised. Processes are often organised around traditional staff roles or to compensate for equipment inadequacy, rather than to serve patients’ needs. In the example in Box 2, the step of paging the equipment officer did not add value and was easily changed. While allowing nurses to order an x-ray in a case of suspected fracture will reduce patient delays, it will provoke debate, and will only be supported if the patient perspective takes priority over entrenched practices. These kinds of debates are an essential part of the education of staff as to why the changes should be made. The best criterion to diffuse disagreement is “if this was your mother, what would you want to happen?”.
The mapping process also facilitates moving the focus from the part of the patient’s body that is affected, or the professions involved in the patient’s care to that of the horizontal journey, and allows new groupings related to the process or journey to emerge. “Patient-care families” are groups of patients whose journeys share many of the same process steps, even though the specifics of their clinical care may differ. The article in this supplement from Flinders Medical Centre (FMC) (→ Redesigning care at the Flinders Medical Centre: clinical process redesign using lean thinking) describes an approach to clinical process redesign that is centred on patient-care families and the development of streams of care (or value streams) for designated patient-care families.4
Redesign may challenge conventional wisdom. For some years, Australian emergency departments (EDs) have used the Australasian Triage Scale5 to prioritise the order in which patients are seen so that patients are attended to in triage order, rather than the order of presentation. Clearly, this makes sense in relation to critically ill patients. However, it leads to patients in lower triage categories having extended waits. At the FMC ED, staff allocate a triage category to all patients, identifying the relatively small number of patients with time-critical threats to life and limb who take priority. All other patients are seen in order of arrival, no matter what their allocated triage category. They are divided into those who are likely to go home directly from the ED, and those likely to be admitted, with each group being seen by a different team of doctors and nurses.
This approach has improved access to care and reduced overall waiting times in the ED without compromising the care of the critically ill.6 The move away from the strict use of the triage scale is quite confronting to many staff, and sustaining such changes requires committed leadership and ongoing monitoring.
NSW Health piloted clinical process redesign in one hospital (John Hunter in Newcastle) in 2002, and implemented it in 10 Sydney hospitals (Westmead, Nepean, Prince of Wales, Liverpool, St George, Canterbury, Royal North Shore, Gosford, Campbelltown and Wollongong in the financial year 2004–05). After significant success at most sites, the NSW Government funded a 3-year, statewide program. At its peak, the Clinical Services Redesign Program (CSRP) included 75 separate redesign projects in 60 hospitals (Box 3).
More details of redesign projects in 23 hospitals and their outcomes are to be found in the appendix to this supplement.
A panel of national consulting firms (Accenture, KPMG, PricewaterhouseCoopers and PA Consulting) was retained to provide expert advice to AHSs on undertaking process re-engineering and to facilitate redesign working parties. The firms also assisted in coaching local hospital managers to give them the skills necessary to implement the solutions. They brought a range of business process redesign and re-engineering methods to the CSRP, including “lean thinking”, “six sigma” and the “theory of constraints”.7-9 Staff appreciated the neutrality of external facilitators who were often able to overcome territorial behaviours.
Knowledge management was a key part of the program. It was facilitated by regular meetings of senior executives and clinicians, and by workshops on tackling common problems. The program office presented redesigned models of care in easy-to-grasp formats and regularly broadcast and celebrated successes in redesign. The new models of care were accompanied by implementation toolkits available on the Australian Resource Centre for Healthcare Innovations website.10 In addition, the Human Services Network, developed by the NSW Government,11 was used for establishing communities of common interest.
The FMC Redesigning Care program is described in more detail in a subsequent article in this supplement (→ Redesigning care at the Flinders Medical Centre: clinical process redesign using lean thinking).4 It was initiated after an aggregated root-cause analysis of a series of disturbing patient events indicated a major breakdown in the capacity to provide safe care in the ED and elsewhere in the hospital. This prompted the search for an effective improvement strategy. Lean thinking, with its emphasis on methods for looking at end-to-end processes, the creation of flow, the value of patient time and staff expertise, and the recognition that activities which did not add value to patient outcomes were potentially wasteful,7 approved a good fit with the underlying values of the organisation.
A small team of clinicians and senior managers learned about lean thinking by linking with local and international experts through Lean Enterprise Australia12 and the global Lean Enterprise network, and by contact with staff from the School of Management at the University of South Australia. A program governance group involving senior clinicians and managers, which reported to the FMC hospital management executive, ensured that the Redesigning Care program worked across the whole hospital and was viewed as a major program.
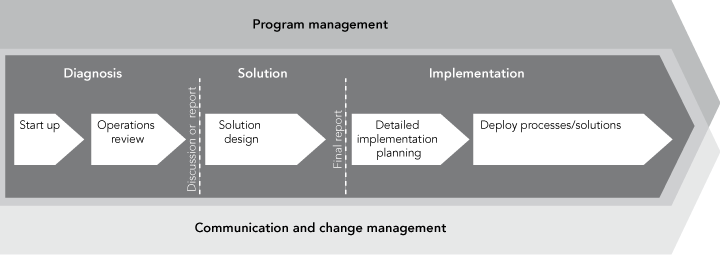
Box 4 outlines the stages involved in redesign programs. It reflects the generic approach arrived at independently by NSW Health’s CSRP and the FMC Redesigning Care program, although specifics vary between settings.
Once the redesign solutions are agreed (and this can involve decisions about “hard” territorial issues, such as reallocation of beds between units), they need to be implemented. It is this step of the process that is, by general agreement, the most difficult. If the solutions are novel, they will require considerable skill in implementation, combining project management skills with managing the human dimension of change in a complex hospital structure (see Box 4). This demands a new skillset for health managers who have previously operated in a “command and control” atmosphere.
1 Hospital organisation and the patient journey*
 | |||||||||||||||
|
* Patients move horizontally through a sectional and hierarchical organisation. | |||||||||||||||
- 1. Ham C, Kipping R, McLeod H. Redesigning work processes in health care: lessons from the National Health Service. Milbank Q 2003; 81: 415-439.
- 2. Keyte B, Locher D. The Complete Lean Enterprise. Value stream mapping for administrative and office processes. New York: Productivity Press, 2005.
- 3. Picker Institute Europe [website]. http://www.pickereurope.org (accessed Sep 2007).
- 4. Ben-Tovim DI, Bassham JE, Bennett DM, et al. Redesigning care at the Flinders Medical Centre: clinical process redesign using “lean thinking”. Med J Aust 2008; 188 (5 Suppl): S27-S31. <MJA full text>
- 5. Considine J, Ung L, Thomas S. Triage nurses’ decisions using the National Triage Scale for Australian emergency departments. Accid Emerg Nurs 2000; 8: 201-209.
- 6. King DL, Ben-Tovim DI, Bassham J. Redesigning emergency department patient flows: application of lean thinking to health care. Emerg Med Australas 2006; 18: 391-397.
- 7. Womack J, Jones D. Lean thinking. Banish waste and create wealth in your corporation. London: Simon and Schuster, 1998.
- 8. Mikel H. Mikel Harry on Six Sigma in healthcare. Interview by Carole S. Guinane. J Healthc Qual 2006; 28: 29-36.
- 9. Goldratt EM. Theory of constraints. New York: North River, 1999. http://www.coba.usf.edu/departments/accounting/faculty/jozsi/presentations%20fall06/TOC.pdf (accessed Sep 2007).
- 10. Australian Resource Centre for Healthcare Innovations [website]. http://www.archi.net.au (accessed Sep 2007).
- 11. Human Services Network [website]. http://bsdp.hsnet.nsw.gov.au/ (accessed Sep 2007).
- 12. Lean Enterprise Australia [website]. http://www.lean.org.au (accessed Aug 2007).





Thanks to Professor John Marley for editorial advice in the preparation of this article and Dr Deborah Lloyd for her work in editing this article and preparing this supplement.
None identified.