The previous article in this supplement (→ Clinical process redesign for unplanned arrivals in hospitals) discussed redesign solutions for unplanned arrivals at hospitals.1 Here, we will consider the application of the Clinical Services Redesign Program to planned arrivals in NSW hospitals.
As the previous article in this supplement (→ Clinical process redesign for unplanned arrivals in hospitals) shows, unplanned hospital demand is predictable over time, and the degree of randomness or variability is relatively small.1 On the other hand, analysis of the planned hospital demand over time commonly shows large variability in the patient flows on a daily basis.
Smoothing out the variability in the scheduling of planned arrivals will reduce this potential source of capacity stress in hospitals and will improve the overall ability of the hospital to deal with the natural variability of arrivals.2,3
Efficient preadmission and OT processes are necessary to avoid cancellation of planned procedural or operative interventions. Cancellation rates resulting from bed unavailability, patients being medically unfit or not arriving, and emergency surgery load were 10%–15% in some facilities. The resultant financial cost to the system of a fully staffed and equipped OT remaining idle is considerable, and patients and their families bear a significant social and financial burden (Box 1).
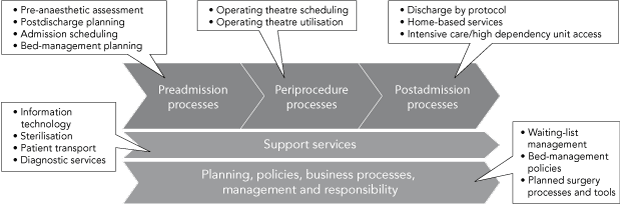
There are multiple steps in the redesign of the journey for a patient being admitted for a planned procedure. The main components for the redesign of the planned patient journey, whether for a short stay or a more prolonged admission, are shown in Box 2. This simple schema covers the patient journey from referral through to discharge.
Waiting list management should ensure that all patients have their procedures in an appropriately prioritised and timely manner. In NSW, major changes were made to waiting list processes as part of the Clinical Services Redesign Program, and resulted in the 2006 publication of NSW Health’s Waiting times and elective patient management policy.4
In addition to this policy, specific guidelines for prioritisation of urgent conditions have been developed, and only patients with these diagnoses are automatically placed in Category 1 by booking-office staff.5 An opt-out system is in place and altered priority categorisation can be organised through the Area Director of Surgery, who is a surgeon. The Area Director makes the final decision, usually after consultation with the clinician concerned.
The Pre-Procedure Preparation Toolkit (PPPT)6 is an essential determinant for success and defines the processes to prepare the patient medically, socially and administratively. In the Clinical Services Redesign Program, it was recognised that patients should not be required to visit the facility for anaesthetic assessment unless absolutely necessary. Thus, a triage system has been adopted which uses a standardised patient health questionnaire — this is an internationally accepted practice.
One way of ensuring that planned demand requirements are met is to use admission configurations more suited to the planned arrivals than the unplanned arrivals. The extended day-only (EDO) model mandates a stay of less than 24 hours with patients being managed according to agreed protocols. Under the EDO model, patients are less likely to have their procedures cancelled and discharge is predetermined by a specific protocol.7
Since the Clinical Services Redesign Program was implemented, theatre staff have been working with surgeons to improve the accuracy of theatre lists so that the number of cases listed is appropriate for the time available (Box 3).
The total waiting list has been reduced from 68 451 in January 2005 to 56 640 in June 2007.
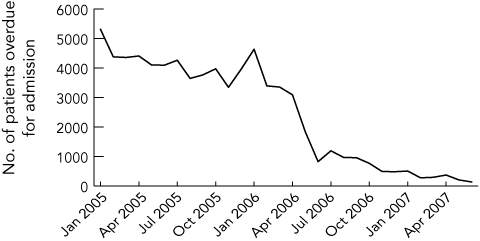
A 97% reduction in the numbers of patients in the Category 1 (admission desirable within 30 days) whose surgery was overdue, from 5308 in January 2005 to 135 in June 2007 (Box 4). This improvement was sustained through the winter period.
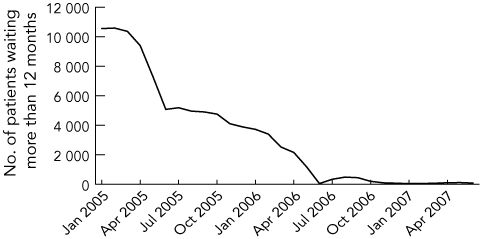
A 99% reduction in the number of patients who have waited more than 365 days for surgery, from 10 551 in January 2005 to 84 in June 2007 (Box 5).
Between January 2005 and June 2007, average waiting times for patients on the waiting list in categories 1, 2 and 3 decreased: Category 1, 70 days to 12 days; Category 2, 141 days to 72 days; and Category 3, 226 days to 122 days.
- 1. O’Connell TJ, Bassham JE, Bishop RO, et al. Clinical process redesign for unplanned arrivals in hospitals. Med J Aust 2008; 188 (5 Suppl): S18-S22. <MJA full text>
- 2. McManus ML, Long MC, Cooper A, et al. Variability in surgical caseload and access to intensive care services. Anesthesiology 2003; 98: 1491-1496.
- 3. Litvak E, Buerhaus PI, Davidoff F, et al. Managing unnecessary variability in patient demand to reduce nursing stress and improve patient safety. Jt Comm J Qual Patient Saf 2005; 31: 330-338.
- 4. NSW Health. Policy directive. Waiting time and elective patient management policy. Sydney: NSW Health, 2006; 7 Mar. (Document no. PD2006_020.) http://www.health.nsw.gov.au/policies/pd/2006/pdf/PD2006_020.pdf (accessed Jul 2007).
- 5. NSW Health. Advice for referring and treating doctors — managing elective patients/waiting lists. Sydney: NSW Health, 2006; 13 Apr. (Information bulletin no. IB2006_011.) http://www.health.nsw.gov.au/policies/ib/2006/pdf/IB2006_011.pdf (accessed Jul 2007).
- 6. NSW Health. Pre-Procedure Preparation Toolkit. Sydney: NSW Health, 2007; 2 Nov. (Guideline no. GL2007_018.) http://www.health.nsw.gov.au/policies/gl/2007/GL2007_018.html (accessed Nov 2007).
- 7. NSW Health. Policy directive. Extended day-only (EDO) admission policy. Sydney: NSW Health, 2007; 7 Aug. (Document no. PD2007_065.) http://www5.health.nsw.gov.au/policies/pd/2007/pdf/PD2007_065.pdf (accessed Jan 2008).





We acknowledge the critical input and advice of Professor John Marley in preparing this article, and Dr Deborah Lloyd for her editorial work on this article and her assistance in preparing this supplement.
None identified.