From the 1920s, Alyawarr and Anmatyerr people lived near homesteads associated with the “Utopia” pastoral station, north-east of Alice Springs. In 1976, clan groups gained freehold title to Utopia and dispersed to their traditional lands1 when the Aboriginal Land Rights (Northern Territory) Act 1976 (Cwlth)2 and the Pastoral Land Act 1992 (NT)3 enabled a broader homelands movement. Thus, the Utopia community is made up of 16 outstations, dispersed over an area of about 10 000 km2. There is no centralised settlement, with outstations, administrative offices, a clinic and store located up to 100 km apart.1 The community-controlled Urapuntja Health Service (UHS) provides primary health care, including outreach services to outstations.
Previous studies showed that decentralisation is associated with prevention of diabetes and, on outstations remote from a store, obesity.4 These are major, but elusive, aims of public health programs worldwide because of the high risk of cardiovascular disease (CVD) associated with these conditions. Such results provide vindication for policies that support outstation living, although such policies have been criticised as unrealistic.5,6
Given this success in management of important CVD risk factors at the population level, we hypothesised that mortality and morbidity from CVD in the UHS population would be lower than for the wider Indigenous population of the Northern Territory, for whom incidence of diabetes and CVD is very high.7,8 The social, environmental and clinical factors aiding prevention of chronic diseases are also likely to manifest as resilience to a range of other conditions. Thus, we aimed to follow up the cohort of participants in the 1995 health survey of the Utopia community to examine all-cause and CVD mortality and hospitalisation rates for CVD; to compare the rates with those for Indigenous people in the NT as a whole; and to examine the outcomes in light of earlier trends in risk factor prevalence.
Risk factor surveys were conducted in 1988 and 1995 at this and other communities, and aggregate results have been reported.1,9,10 We have collected 10-year follow-up data on mortality and hospitalisation from cardiovascular causes relating to a cohort of all 296 participants in the 1995 survey at Utopia. This UHS cohort is the first completed arm of a larger, ongoing cohort study, which aims to identify clinical predictors of CVD events. The project was approved by the Central Australian Human Research Ethics Committee and the University of Melbourne Human Research Ethics Committee.
Individuals were identified by name, known aliases, date of birth, next-of-kin details, address and, when necessary, confirmation of identity with local clinic staff. Vital status was ascertained through a search of hospital information systems and primary health care (PHC) records, and through interviews with relevant informants. Mortality data were obtained by review of death certificates, hospital and PHC records, and autopsy findings. Cause of death was coded as recorded on the death certificate in 20 cases, or as determined from coroner’s records (four cases) or local medical officer (one case). A single investigator was responsible for final determination. Cause-of-death classifications were predetermined according to standardised definitions.11 Two people (aged 89 years and 91 years) had unspecified cause of death. One person with a history of congestive cardiac failure was known to have died, but the date of death was unknown; this person was known to be alive 3 months before the end of the study period.
Selected socioeconomic indicators from the 2006 Census of Population and Housing were examined for the NT Indigenous population and the Urapuntja Outstations Indigenous location, as these potential epidemiological confounders may contribute to differential health outcomes.12
Trends in risk factor prevalence for 1988–1995 were tested using the Mantel–Haenszel age-weighted χ2 test: these data are a subset of a larger study reported previously.4 Confidence intervals were calculated assuming a binomial distribution.
Blood pressure was measured by mercury sphygmomanometer in 1988 and using a Dinamap automated monitor in 1995 (the former values were adjusted using the formula (0.905 × diastolic blood pressure) + 4.636.13 Current smoking was assessed by yes/no questionnaire.
Crude mortality rates for March 1995 to December 2004 were expressed as deaths per 100 000 person-years. For comparison, rates reported for the Indigenous population of the NT were indirectly standardised for age and sex using the UHS cohort demographic structure as a reference population. Registration of Indigenous deaths in the NT is reported as 94% complete,14 and the NT Indigenous population size is estimated using adjustments to census counts for failure to participate and non-response to the question about Indigenous status. Thus, the 2001 census count for Indigenous people in the NT was adjusted upwards by 12%.15 Standardised mortality ratios (SMRs) and mid-P exact 95% confidence intervals were determined using an online calculator.16 Statistical significance was taken as P < 0.05 or, for mortality data, when SMR confidence intervals did not overlap unity.
Primary causes of death were: CVD (8 deaths); accident and trauma (8); respiratory disease (4); renal failure (2); cancer (2); infection other than respiratory (1); and unknown (2). The number of deaths occurring in each age group (Box 1) as a proportion of total deaths did not differ significantly to that reported for Indigenous people in the NT for 2004 (χ2 = 2.5; df = 3; P = 0.468).14 The all-cause mortality rate for the cohort was significantly lower than that reported for Indigenous people in the NT, and remained so if it was assumed that the individual with unknown date of death died before 31 December 2004 (Box 1), but was significantly higher than for non-Indigenous people aged 15 years or older in the NT (SMR, 2.11; 95% CI, 1.42–3.03).
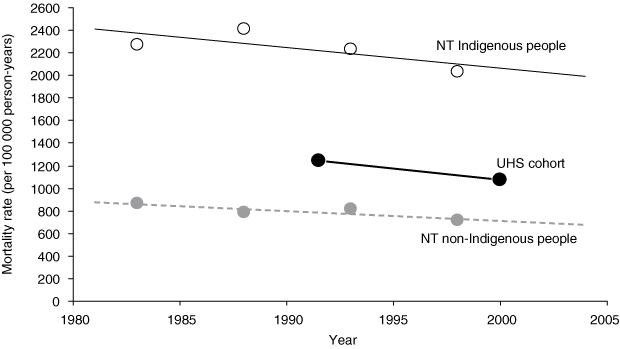
Trends in mortality (for people aged 25 years or older) since 1980 in the NT are shown in Box 2.8 Mortality at the Utopia community was substantially lower than for Indigenous people in the NT as a whole, but somewhat higher than for non-Indigenous people in the NT.
Of eight deaths from CVD, there were five heart attacks, two strokes, and one case of bacterial endocarditis. Six of the eight CVD deaths were among people aged 45 years or older. For people aged 25 years or older, the CVD mortality rate for the UHS cohort was lower than that reported for Indigenous people in the NT (Box 1) and not significantly different to that for non-Indigenous people (SMR, 1.29; 95% CI, 0.56–2.54).8 The age-standardised Indigenous CVD mortality rate for the NT, Western Australia, South Australia and Queensland was 421 per 100 000 person-years (SMR, 0.69; 95% CI, 0.30–1.37).17
For the 277 people for whom we reviewed hospital records, there were 35 hospital admissions with CVD as the primary cause (13.4 admissions per 1000 person-years). This was significantly lower than for Indigenous people in the NT (age-standardised hospitalisation rate with CVD coded as the primary cause of admission among people 15 years or older in 2002–2004, 33.4 per 1000 person-years; χ2 = 31.1; df = 1; P < 0.001) and similar to that for non-Indigenous people in the NT (14.8 per 1000 person-years; χ2 = 0.41; df = 1; P = 0.522).18
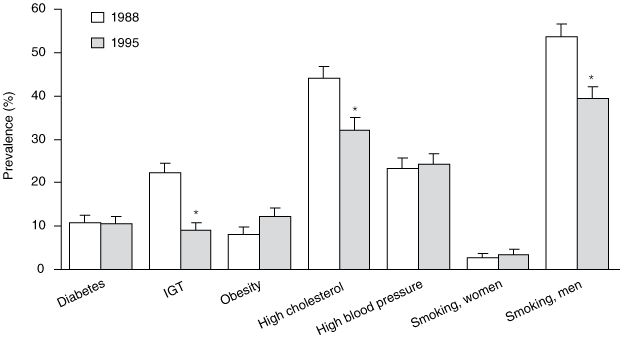
For the 8 years before the commencement of the cohort study, there were no significant changes in the prevalence of obesity (P = 0.125), diabetes (P = 0.907), hypertension (P = 0.983) or, for women, smoking (P = 0.931) (Box 3). There were significant reductions in the prevalence of impaired glucose tolerance (P < 0.001), hypercholesterolaemia (P = 0.003) and smoking among men (P = 0.034).
Based on data from the 2006 census, conventional socioeconomic indicators of health were generally worse for the Utopia community than for Indigenous people in the NT: participation in the labour force (age 15–64 years), 29% v 52% for NT; gross weekly income < $400 (age ≥ 15 years), 86% v 72% for NT; households with more than three residents per bedroom, 25% v 8% for NT; Year 12 completion (age ≥ 15 years), 0 v 9% for NT; did not go to school (age ≥ 15 years), 21% v 7% for NT.12
In considering the precision of these comparisons with data published for the NT, we note the different methods used to calculate mortality rates. We have followed a group of individuals over time and achieved a very high rate of follow-up, giving what we believe is an accurate and precise figure. In estimating mortality rate for the NT, the Australian Bureau of Statistics (ABS) uses registered deaths of Indigenous people as the numerator, and the estimated resident population based on census data as the denominator (see Methods). To account for the differential mortality rates reported here, the census would need to underestimate the NT Indigenous population by at least 30% (and by far more to account for the difference in CVD hospitalisation rates), but we cannot exclude the possibility of a bias (of unclear magnitude and direction) in the reported NT data. However, the Indigenous mortality rate reported by the ABS for the NT in 2000–2004 is similar to or less than that observed in a cohort study of Aboriginal adults living on centralised settlements over the years 1987–1995 (1750 per 100 000 person-years).10 Taken together, these results suggest the lower than expected mortality rate observed here is a true reflection of lower risk.
The relatively low rate of hospitalisation for CVD (similar to that for non-Indigenous NT residents) is consistent with the relatively low prevalences of obesity, diabetes and smoking (for women) observed in earlier surveys, but may also indicate a degree of unmet need for medical treatment. Nevertheless, the mortality rate from CVD in the UHS cohort was lower than for Indigenous people in the NT and, in age-standardised terms, not significantly greater than for non-Indigenous people in the NT (although we note the limited statistical power of these comparisons). Mortality from ischaemic heart disease for Indigenous people in the NT has increased since 1977, while mortality from stroke has remained roughly constant.19
Conventional measures of employment, income, housing and education did not account for this health differential. The factors associated with the particularly good outcomes here are likely to include outstation living, with its attendant benefits for physical activity and diet and limited access to alcohol, as well as social factors, including connectedness to culture, family and land, and opportunities for self-determination.18,20-22 At the direction of the Health Council, UHS conducts regular outreach to homeland communities. This involves extensive travel to deliver acute and chronic care, and preventive activities, including well persons’ health checks. We caution against assumptions of expense associated with supporting outstations, given the savings to health care systems when successful primary prevention is achieved, and a broader (positive) economic context of outstation living related to activities such as art, food procurement and land management.23 A stereotype of outstation communities as cultural museums that prevent health and social gains for Aboriginal people5 is not supported by the present evidence, nor is forcible imposition of interventions on communities and the removal of freehold land title from Aboriginal ownership.24 However, mortality rates for these communities are not yet equivalent to those for Australians generally, and room for major improvements in housing and other infrastructure and service sectors remains.
2 All-cause mortality in the Northern Territory since 1980 for Indigenous and non-Indigenous people aged ≥ 25 years8 and the Urapuntja Health Service (UHS) cohort10
 | |||||||||||||||
|
Data are indirectly standardised for age and sex using the UHS cohort as the reference population. | |||||||||||||||
Received 6 August 2007, accepted 19 November 2007
- Kevin G Rowley1,2
- Kerin O’Dea2,3
- Ian Anderson1
- Robyn McDermott4
- Karmananda Saraswati5
- Ricky Tilmouth5
- Iris Roberts3,6
- Joseph Fitz3
- Zaimin Wang7
- Alicia Jenkins2
- James D Best2,8
- Zhiqiang Wang7
- Alex Brown3,6
- 1 Onemda VicHealth Koori Health Unit, Centre for Health and Society, School of Population Health, University of Melbourne, Melbourne, VIC.
- 2 Department of Medicine (St Vincent’s Hospital), University of Melbourne, Melbourne, VIC.
- 3 Menzies School of Health Research, Darwin, NT.
- 4 University of South Australia, Adelaide, SA.
- 5 Urapuntja Health Service, Utopia, NT.
- 6 Centre for Indigenous Vascular and Diabetes Research, Baker Heart Research Institute, Alice Springs, NT.
- 7 School of Population Health, University of Queensland, Brisbane, QLD.
- 8 Faculty of Medicine, Dentistry and Health Sciences, University of Melbourne, Melbourne, VIC.
We thank Elders of the Alyawarr and Anmatyerr Nations: Kumantjayi Kunoth, Hugh Heggie, and Sabina Knight. David Thomas, Dallas English, Allison Hodge, and Margaret Kelaher provided statistical advice; and Leah Johnston, Paul Rickards and Stacey Swenson provided technical assistance. This work was funded by the National Health and Medical Research Council and a VicHealth Public Health Research Fellowship to Kevin Rowley. Onemda is funded by VicHealth and the Australian Government Department of Health and Ageing.
None identified.
- 1. Gault A, O’Dea K, Rowley KG, et al. Abnormal glucose tolerance and other coronary heart disease risk factors in an isolated Aboriginal community in central Australia. Diabetes Care 1996; 19: 1269-1273.
- 2. Indigenous Studies Program. Agreements, treaties and negotiated settlements project: Aboriginal Land Rights (Northern Territory) Act 1976 (Cth). Melbourne: University of Melbourne, 2007. http://www.atns.net.au/agreement.asp?EntityID=381 (accessed Jan 2008).
- 3. Indigenous Studies Program. Agreements, treaties and negotiated settlements project: Pastoral Land Act 1992 (NT). Melbourne: University of Melbourne, 2007. http://www.atns.net.au/agreement.asp?EntityID=2571 (accessed Jan 2008).
- 4. Rowley K, Gault A, McDermott R, et al. Reduced prevalence of impaired glucose tolerance and no change in prevalence of diabetes despite increasing BMI among Aboriginal people from a group of remote homeland communities. Diabetes Care 2000; 23: 898-904.
- 5. Vanstone A. Beyond conspicuous compassion: Indigenous Australians deserve more than good intentions. In: Wanna J, editor. A passion for policy: ANZOG lecture series 2005–2006. Canberra: ANU Press, 2007.
- 6. Stafford A. Threat to cut funds for remote Aborigines. The Age (Melbourne) 2006; 6 Dec: 2.
- 7. Daniel M, Rowley KG, McDermott R, et al. Diabetes incidence in an Australian Aboriginal population. An 8-year follow-up study. Diabetes Care 1999; 22: 1993-1998.
- 8. Li SQ, Guthridge S. Mortality in the Northern Territory 1981–2000. Part 1: key indicators and overview. Darwin: NT Department of Health and Community Services, 2004.
- 9. Rowley KG, Iser DM, Best JD, O’Dea K. Albuminuria in Australian Aboriginal people: prevalence and associations with components of the metabolic syndrome. Diabetologia 2000; 43: 1397-1403.
- 10. McDermott R, O’Dea K, Rowley K, et al. Beneficial impact of the Homelands Movement on health outcomes in central Australian Aborigines. Aust N Z J Public Health 1998; 22: 653-658.
- 11. Tunstall-Pedoe H, Kuulasmaa K, Amouyel P, et al. Myocardial infarction and coronary deaths in the World Health Organization MONICA Project. Circulation 1994; 90: 583-612.
- 12. Australian Bureau of Statistics. 2006 Census data. Canberra: ABS, 2007. http://www.censusdata.abs.gov.au/ (accessed Nov 2007).
- 13. Briganti EM, Shaw JE, Chadban SJ, et al. Untreated hypertension among Australian adults: the 1999–2000 Australian Diabetes, Obesity and Lifestyle Study (AusDiab). Med J Aust 2003; 179: 135-139. <MJA full text>
- 14. Australian Bureau of Statistics. Deaths, Australia, 2004. Canberra: ABS, 2004. (ABS Catalogue No. 3302.0.)
- 15. Australian Bureau of Statistics. Experimental estimates and projections, Aboriginal and Torres Strait Islander Australians. Canberra: ABS, 2004. (ABS Catalogue No. 3238.0.)
- 16. Sullivan KM, Soe MM. SMR analysis, version 4.11.19 [online calculator]. Atlanta: Rollins School of Public Health of Emory University, 2005. http://www.sph.emory.edu/~cdckms/exact-midP-SMR.html (accessed Nov 2007).
- 17. Australian Bureau of Statistics. The health and welfare of Australia’s Aboriginal and Torres Strait Islander Peoples 2005. Canberra: ABS, 2005. (ABS Catalogue No. 4704.0.)
- 18. Australian Health Ministers’ Advisory Council. Aboriginal and Torres Strait Islander health performance framework report 2006. Canberra: AHMAC, 2006. http://www.health.gov.au/internet/wcms/publishing.nsf/Content/health-oatsih-pubs-framereport (accessed Jan 2008).
- 19. Thomas DP, Condon JR, Anderson IP, et al. Long-term trends in Indigenous deaths from chronic diseases in the Northern Territory: a foot on the brake, a foot on the accelerator. Med J Aust 2006; 185: 145-149. <MJA full text>
- 20. O’Dea K. Marked improvement in carbohydrate and lipid metabolism in diabetic Australian Aborigines after temporary reversion to traditional lifestyle. Diabetes 1984; 33: 596-603.
- 21. Chandler M, Proulx T. Changing selves in changing worlds: youth suicide on the fault-lines of colliding cultures. Arch Suicide Res 2006; 10: 125-140.
- 22. Pitjarra J, Kamarra OF, Ngala SR, et al. “You just can’t hold us up again!” In: Moody R, editor. The Indigenous voice: visions and realities. London: Zed Books, 1988: 383-384.
- 23. Altman J, Buchanan G, Biddle N. Measuring the ‘real’ Indigenous economy in remote Australia using NATSISS 2002. Aust J Labour Economics 2006; 9: 17-31.
- 24. Brough M. National emergency response to protect Aboriginal children in the NT. Media release, 21 June 2007. Canberra: Parliament of Australia, 2007. http://parlinfoweb.aph.gov.au/piweb/Repository1/Media/pressrel/8ZFN60.pdf (accessed Jan 2008).





Abstract
Objective: To examine mortality from all causes and from cardiovascular disease (CVD), and CVD hospitalisation rate for a decentralised Aboriginal community in the Northern Territory.
Design and participants: For a community-based cohort of 296 people aged 15 years or older screened in 1995, we reviewed hospital and primary health care records and death certificates for the period up to December 2004 (2800 person-years of follow-up).
Main outcome measures: Mortality from all causes and CVD, and hospitalisation with CVD coded as a primary cause of admission; comparison with prior trends (1988 to 1995) in CVD risk factor prevalence for the community, and with NT-specific Indigenous mortality and hospitalisation rates.
Results: Mortality in the cohort was 964/100 000 person-years, significantly lower than that of the NT Indigenous population (standardised mortality ratio [SMR], 0.62; 95% CI, 0.42–0.89). CVD mortality was 358/100 000 person-years for people aged 25 years or older (SMR, 0.52; 95% CI, 0.23–1.02). Hospitalisation with CVD as a primary cause was 13/1000 person-years for the cohort, compared with 33/1000 person-years for the NT Indigenous population.
Conclusion: Contributors to lower than expected morbidity and mortality are likely to include the nature of primary health care services, which provide regular outreach to outstation communities, as well as the decentralised mode of outstation living (with its attendant benefits for physical activity, diet and limited access to alcohol), and social factors, including connectedness to culture, family and land, and opportunities for self-determination.