In spite of these improvements, the ratio of NT Indigenous to total Australian mortality rates increased, except for a decrease in children aged under 5 years.1,2 Further, NT Indigenous non-communicable disease mortality did not decrease from 1977 to 2000.2 Were there differences between diseases in this large category? Mixed changes in cancer mortality, including increases in smoking-related cancer deaths, have already been reported.3 In this article, we report mortality of the other non-communicable diseases causing the most NT Indigenous deaths4 — ischaemic heart disease (IHD), chronic obstructive pulmonary disease (COPD), cerebrovascular disease (CVD), diabetes mellitus (DM), renal failure (RF) and rheumatic heart disease (RHD).
We used the previously described long-term time series of death and population data for Indigenous people in the NT, extended to include 2001.1 Comparison death and population data for the total Australian population were purchased from the Australian Bureau of Statistics (ABS).
The dataset included deaths coded according to the revision of the World Health Organization’s International classification of diseases used at the time (ICD-8 [8th revision] for deaths registered 1977–1978, ICD-9 for 1979–1996, and ICD-10 for 1997–2002). The ICD groupings for the six diseases in NT government publications were used.5 The comparability of deaths coded according to ICD-10 and ICD-9 was tested by means of an ABS sample of 34 780 Australian deaths coded according to both methods. The comparability factor (ICD-10 deaths/ICD-9 deaths) ranged from 93.4% to 105.1% for five of the six diseases. The much lower comparability factor of 68.8% for chronic RHD was based on a much smaller sample of deaths, and is of uncertain reliability.
Over the 25 years, NT Indigenous mortality rates increased significantly for IHD and DM and fell significantly for COPD (Box 1). There were decreases in CVD and RHD mortality, but these were not statistically significant. RF mortality trends were different for younger and older people. The mortality rate decreased for those aged less than 50 years, but increased for those aged 50 years and older; both trends were statistically significant, but there were only 35 deaths from RF among people aged under 50 years. The change in coding from ICD-9 to ICD-10 did not appear to significantly modify, and thus explain, these mortality trends.
There were differences in the mortality trends for the six diseases between the 1980s and 1990s (Box 2). For COPD, mortality increased before 1990, but decreased thereafter. Mortality from IHD and DM increased throughout the period 1977–2001, but the rate of increase slowed significantly after 1990. Similar differences between the 1980s and 1990s were found in CVD and RHD death rates, but these differences were not statistically significant. The differences between the two periods were not sensitive to changing the end date of the first period.
Trends in both the NT Indigenous and total Australian death rates are shown in Box 3. From 1977 to 2001, the Australian direct standardised rates fell for IHD, CVD, RHD and COPD, remained largely unchanged for DM, and increased for RF. The ratio of NT Indigenous to total Australian mortality rates increased for all six diseases; this increase was statistically significant for all except COPD (Box 4).
It has previously been reported that NT Indigenous death rates from all non-communicable diseases did not change between 1977 and 2000 (there was a 5% increase which was not statistically significant).2
However, recent research on Indigenous mortality trends has reported more optimistic news. Statistically significant Indigenous mortality declines in the 1990s have been reported in non-communicable diseases (and circulatory diseases in particular) in Western Australia, and communicable diseases in males in WA and South Australia.6 Indigenous infant mortality declined in NT, WA and SA in the 1990s.6 Data are of insufficient quality to determine mortality trends in other states.6
The magnitude of the IHD, COPD and DM trends are all larger than the previously reported all-cause mortality trends in NT Indigenous people aged over 5 years. The largest estimated trends (in DM deaths and in COPD deaths in 1990–2001) were even greater than the reported fall in mortality in those aged under 5 years.2
Some misclassification of Indigenous status in the datasets probably occurred, but this is likely to be rare compared with other states and territories. Misclassification of underlying cause of death is known to be a problem in death registrations, including in the NT; deaths from circulatory and respiratory diseases were overcounted and endocrine diseases (mainly DM) were undercounted in a sample of 220 NT Indigenous deaths in 1992.7 However, no information is available on whether this misclassification of diseases was constant over the 25-year period.
The regression models provide the most accurate estimates of the 25-year trends as they use data from the whole period, rather than just comparing death rates at the start and end of the period (which is very sensitive to the endpoints chosen).6 However, the models and their estimates rely on the assumption that the annual percentage change in death rates is constant. This was most clearly untrue for COPD death rates, which increased and then fell. Box 2 and Box 3 indicate where these estimated 25-year trends do not appear to have been constant.
Smoking: In the NT, 20% of Aboriginal adult deaths in 1986–1995 were attributed to smoking.8 COPD, IHD, lung cancer and CVD were the four leading causes. We have shown that COPD peaked in the 1980s and began to decline in the 1990s. Decreased smoking was not responsible, as three large surveys in 1986–1987, 1994 and 2002 showed little change in NT Indigenous smoking rates.9-11 Other possible reasons for the decline in COPD deaths include improved intrauterine growth, fewer childhood infections and less exposure to tobacco, improved nutrition and less overcrowding decades ago, and, more recently, better prevention and management of adult respiratory infections and acute exacerbations of COPD.12
Primary and specialist care: There is some evidence, at least among people with diabetes, that blood pressure screening and control are routinely occurring in NT Indigenous bush communities at similar levels to those in the non-Indigenous population.13,14 Reviews of randomised clinical trials show that blood pressure control leads to a reduction in mortality from CVD at least three times greater than that from IHD.15 This may explain the more modest changes in death rates from CVD than IHD among NT Indigenous people.
The considerable expansion of primary care (clinical, disease prevention and health promotion) services for Indigenous people in the NT from 1977 to 2001,16,17 combined with more recent increasing attention to chronic disease prevention and management,18 may have contributed to improving control of hypertension over the period.
Hospital care can prevent deaths from CVD or IHD by improving survival immediately after a stroke or acute myocardial infarction (AMI). Indigenous people experience significant and dangerous delays in access to NT hospitals after an AMI.19 NT Indigenous IHD hospital separation rates increased only slightly faster than IHD deaths from 1979 to 1991, whereas CVD hospitalisations nearly trebled when death rates were stable,20 possibly contributing to the better CVD than IHD mortality trends.
Birthweight: Low birthweight and poor infant growth are associated with chronic disease mortality, although the mechanisms and public health significance of this association remain contested.21 NT Indigenous birthweights improved over the study period,22 but it is not possible to describe with similar accuracy the birthweight trends of earlier periods, when those dying of chronic diseases in 1977–2001 were born.
Underlying social determinants of health: Accompanying (and often driving) the gradual improvements in access to health care have been enormous social, economic and political changes for Indigenous peoples in the NT since the political struggles of the 1960s. Changing experiences of racism and social exclusion in parallel with these political changes, together with improvements in absolute, but not relative, incomes23 and educational outcomes,24 may have helped reduce mortality from all diseases.
2 Comparison of estimated annual change in Northern Territory Indigenous mortality rates in 1977–1989 and 1990–2001*
Per cent average annual change (95% CI) |
|||||||||||||||
3 Northen Territory Indigenous and total Australian death rates, 1977–2001*
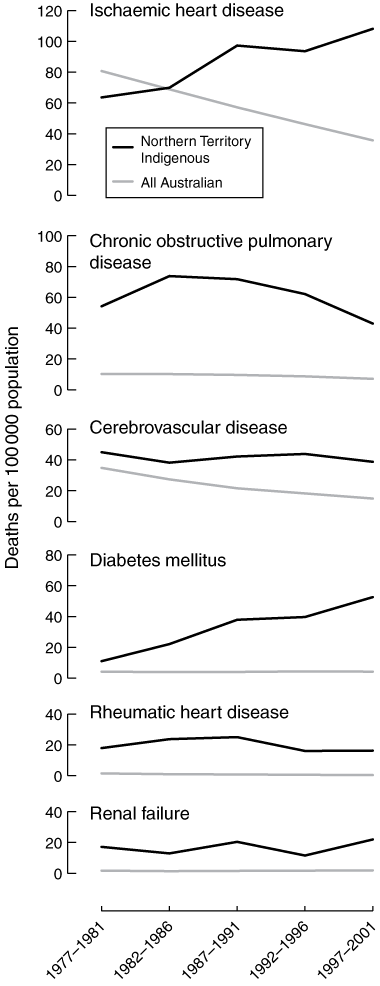
* Direct age-standardised and sex-standardised to the 2001 NT Indigenous population.
Received 5 December 2005, accepted 14 June 2006
- David P Thomas1,2
- John R Condon1
- Ian P Anderson2
- Shu Q Li3
- Stephen Halpin1
- Joan Cunningham1
- Steven L Guthridge3
- 1 Menzies School of Health Research, Darwin, NT.
- 2 Onemda VicHealth Koori Health Unit, Centre for Health and Society, University of Melbourne, Melbourne, VIC.
- 3 Health Gains Planning Unit, Department of Health And Community Services, Darwin, NT.
David Thomas and John Condon are supported by an NHMRC Population Health Capacity Building Grant. Joan Cunningham is supported by an NHMRC Career Development Award. Core funding for Onemda VicHealth Koori Health Unit (in the Centre for Health and Society) is provided by the Victorian Health Promotion Foundation and the Commonwealth Department of Health and Ageing.
None identified.
- 1. Condon J, Barnes T, Cunningham J, Smith L. Demographic characteristics and trends of the Northern Territory Indigenous population, 1966 to 2001. Occasional paper. Darwin: Cooperative Research Centre for Aboriginal Health, 2004.
- 2. Condon J, Barnes T, Cunningham J, Smith L. Improvements in Indigenous mortality in the Northern Territory over four decades. Aust N Z J Public Health 2004; 28: 445-451.
- 3. Condon J, Barnes T, Cunningham J, Armstrong B. Long-term trends in cancer mortality for Indigenous Australians in the Northern Territory. Med J Aust 2004; 180: 504-507. <MJA full text>
- 4. Dempsey K, Condon J. Mortality in the Northern Territory 1979–1997. Darwin: Territory Health Services, 1999.
- 5. Li SQ, Guthridge SL. Mortality in the Northern Territory 1981–2000. Part 1. Key indicators and overview. Darwin: Department of Health and Community Services, 2004.
- 6. Australian Bureau of Statistics and Australian Institute of Health and Welfare. The health and welfare of Australia’s Aboriginal and Torres Strait Islander peoples 2005. Canberra: ABS, 2005. (Cat. No. 4704.0.)
- 7. Weeramanthri T. A medical cause of death: validation study of adult Aboriginal deaths in the Northern Territory of Australia in 1992. Public Health 1997; 111: 429-433.
- 8. Measey M, d’Espaignet E, Cunningham J. Adult morbidity and mortality due to tobacco smoking in the Northern Territory, 1986–1995. Darwin: Territory Health Services, 1998.
- 9. Watson C, Fleming J, Alexander K. A survey of drug use patterns in Northern Territory Aboriginal communities: 1986–1987. Darwin: Northern Territory Department of Health and Community Services Drug and Alcohol Bureau, 1988.
- 10. Cunningham J. Cigarette smoking among Indigenous Australians, 1994. Canberra: Australian Bureau of Statistics, 1997. (Occasional paper 4701.0.)
- 11. Australian Bureau of Statistics. National Aboriginal and Torres Strait Islander Social Survey 2002. Canberra: ABS, 2004. (Cat. No. 4714.0.)
- 12. Maguire GP. Respiratory health and disease in Aboriginal Australians in the Northern Territory [PhD thesis]. Sydney: University of Sydney, 2004.
- 13. McDermott R, Tulip F, Schmidt B. Diabetes care in remote northern Australian Indigenous communities. Med J Aust 2004; 180: 512-516. <MJA full text>
- 14. Bailie R, Si D, Robinson G, et al. A multifaceted health-service intervention in remote Aboriginal communities: 3-year follow-up of the impact on diabetes care. Med J Aust 2004; 181: 195-200. <MJA full text>
- 15. Cutler JA, MacMahon SW, Furberg CD. Controlled clinical trials of drug treatment for hypertension: a review. Hypertension 1989; 13 Suppl: I36-I44.
- 16. House of Representatives Standing Committee on Aboriginal Affairs. Aboriginal health. Canberra: AGPS, 1979.
- 17. Territory Health Services. Annual report 2000/2001. Darwin: Government Printer of the Northern Territory, 2001.
- 18. Weeramanthri T, Morton S, Hendy S, et al. Northern Territory preventable chronic disease strategy — overview and framework. Darwin: Territory Health Services, 1999.
- 19. Ong M, Weeramanthri T. Delay times and management of acute myocardial infarction in indigenous and non-indigenous people in the Northern Territory. Med J Aust 2000; 173: 201-204.
- 20. Plant AJ, Condon JR, Durling G. Northern Territory health outcomes, morbidity and mortality 1979–1991. Darwin: Northern Territory Department of Health and Community Services, 1995.
- 21. Kuh D, Ben-Shlomo Y, editors. A life course approach to chronic disease epidemiology. Oxford: Oxford University Press, 1997.
- 22. Markey P, d’Espaignet E, Condon J, Woods M. Trends in the health of mothers and babies, Northern Territory, 1986–95. Darwin: Territory Health Services, 1998.
- 23. Taylor J. Indigenous economic futures in the Northern Territory: the demographic and socioeconomic background. Canberra: Centre for Aboriginal Economic Policy Research, 2003. (Discussion paper no. 246.)
- 24. Northern Territory Department of Education. Learning lessons: an independent review of Indigenous education in the Northern Territory. Darwin: Northern Territory Department of Education, 1999.





Abstract
Objective: To examine trends in Northern Territory Indigenous mortality from chronic diseases other than cancer.
Design: A comparison of trends in rates of mortality from six chronic diseases (ischaemic heart disease [IHD], chronic obstructive pulmonary disease [COPD], cerebrovascular disease [CVD], diabetes mellitus [DM], renal failure [RF] and rheumatic heart disease [RHD]) in the NT Indigenous population with those of the total Australian population.
Participants: NT Indigenous and total Australian populations, 1977–2001.
Main outcome measures: Estimated average annual change in chronic disease mortality rates and in mortality rate ratios.
Results: Death rates from IHD and DM among NT Indigenous peoples increased between 1977 and 2001, but this increase slowed after 1990. Death rates from COPD rose before 1990, but fell thereafter. There were non-significant declines in death rates from CVD and RHD. Mortality rates from RF rose in those aged ≥ 50 years. The ratios of mortality rates for NT Indigenous to total Australian populations from these chronic diseases increased throughout the period.
Conclusions: Mortality rates from IHD and DM in the NT Indigenous population have been increasing since 1977, but there is evidence of a slower rise (or even a fall) in death rates in the 1990s. These early small changes give reason to hope that some improvements (possibly in medical care) have been putting the brakes on chronic disease mortality among Aboriginal and Torres Strait Islander peoples.