To the Editor: Little is known about the epidemiology of respiratory syncytial virus (RSV) in arid, desert regions generally, and in central Australia in particular. We performed a 5-year retrospective study from 2000 to 2004, inclusive, of children aged less than 2 years who were admitted to Alice Springs Hospital and identified as having RSV infection. RSV was detected using direct immunofluorescence (Light Diagnostics SimulFluor; Millipore, Billerica, Mass, USA) on nasopharyngeal secretions. The test has a reported sensitivity of 92%.1 We extracted demographic data from case notes and obtained population data from the Northern Territory Department of Health2 and the Australian Bureau of Statistics.3
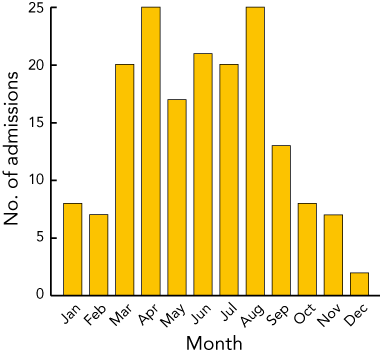
From case notes over the 5 years, we identified 173 eligible children with RSV infection. The annual incidence rate was 21.4 per 1000 children under 2 years old. The rate in Aboriginal children was 30.9 per 1000, and the rate in non-Aboriginal children 11.6 per 1000 (P < 0.0001). The monthly distribution of cases is shown in the Box. Cases occurred throughout the year, and in every month, but there was a peak in admissions from March to August, which covers the Australian winter.
Because Alice Springs Hospital is the only large hospital in the region, and almost all children needing hospital admission for RSV infection will be admitted there, our incidence rates of hospitalisation for RSV infection closely approximate population rates. However, we may have under-estimated the incidence because we only included children in hospital with proven infection, so we may have missed children who were not tested, or whose immunofluorescence test results were falsely negative. There may have been selection bias regarding admissions. Nevertheless, we found that Aboriginal children were more likely than non-Aboriginal children to be hospitalised with RSV infection, a finding in keeping with the known high incidence of pneumonia and bronchiectasis in Aboriginal children.4,5 While the incidence of RSV infection peaked in winter in central Australia, infections occurred throughout the year, and the winter predominance was less marked than is the case in temperate Australia.6 These data provide valuable information about RSV infection in an arid, desert region and can inform decisions about active or passive immunisation against RSV infection in central Australia.
- Apakasimaka Dede1
- David Isaacs2
- Paul J Torzillo3
- John Wakerman4
- Rob Roseby5
- Rose Fahy5
- George Clothier5
- Andrew White4
- Paula Kitto4
- 1 Hervey Bay Hospital, Hervey Bay, QLD.
- 2 Department of Immunology and Infectious Diseases, The Children’s Hospital at Westmead, Sydney, NSW.
- 3 Prince Alfred Hospital, Sydney, NSW.
- 4 Centre for Remote Health, Alice Springs, NT.
- 5 Alice Springs Hospital, Alice Springs, NT.
- 1. Gregson D, Lloyd T, Buchan S, Church D. Comparison of the RSV respi-strip with direct fluorescent-antigen detection for diagnosis of respiratory syncytial virus infection in pediatric patients. J Clin Microbiol 2005; 43: 5782-5783.
- 2. Zhao Y, Paice J, Murtagh D, et al. Population estimates for the Indigenous health zones in the Northern Territory. Darwin: Department of Health and Community Services, Northern Territory 2007. http://www.nt.gov.au/health/docs/Health_Zones_Internals.pdf (accessed Nov 2007).
- 3. Australian Bureau of Statistics. Regional statistics, Northern Territory, 2005. Canberra: ABS, 2005. (ABS Catalogue No. 1362.7). http://www.abs.gov.au/AUSSTATS/abs@.nsf/ProductsbyReleaseDate/2BF72BBF4AB2CB38CA2572120015F3A3?OpenDocument (accessed Nov 2007).
- 4. Torzillo PJ, Hanna JN, Morey F, et al. Invasive pneumococcal disease in central Australia. Med J Aust 1995; 162: 182-186.
- 5. Chang AB, Grimwood K, Mulholland EK, Torzillo PJ, for the Working Group on Indigenous Paediatric Respiratory Health. Bronchiectasis in indigenous children in remote Australian communities. Med J Aust 2002; 177: 200-204. <MJA full text>
- 6. Roche P, Lambert S, Spencer J. Surveillance of viral pathogens in Australia: respiratory syncytial virus. Commun Dis Intell 2003; 27: 117-122.