Chronic kidney disease (CKD) refers to progressive injury to the kidneys that results in gradual and irreversible loss of kidney function. Risk factors for onset and progression include diabetes/poor glycaemic control, hypertension, exposure to nephrotoxins and smoking.1 The estimated proportion of Australian adults who have some degree of CKD is 16%,2 of which a small minority will progress to end-stage kidney disease and the requirement for dialysis or a kidney transplant. For the majority, however, the outcome will be premature vascular mortality or a range of complications having a substantial impact on quality of life.3-5
Little is known about recognition and knowledge of CKD in the Australian community. Evidence of the benefits of detecting CKD in its earliest stages is growing, with interventions being effective in reducing morbidity and mortality.6,7 However, poor awareness of risk factors for kidney disease in the general community is a likely barrier to early detection and prevention. Australian clinical practice guidelines recommend opportunistic testing by general practitioners for CKD in people with diabetes, hypertension, or a family history of kidney disease, and in Indigenous Australians.8 Yet about one in two Australian adults with diabetes are undiagnosed,9 and one in three with high blood pressure go untreated.10 This suggests that many people at high risk of CKD or with existing asymptomatic CKD currently escape identification.
We conducted a cross-sectional survey of participants in the Australian Diabetes, Obesity and Lifestyle Study (AusDiab)11 regarding their perceptions of the causes of kidney disease, and asking whether they recalled ever having had their kidney function tested. Our aim was to establish a picture of lay understanding of kidney disease in a cohort of adults taken from the general Australian community.
The AusDiab study, which commenced in 1999, is a longitudinal, nationally representative survey of diabetes mellitus and associated risk factors in Australians over 25 years of age. Selection methods11 and baseline biomedical data collection methods have been reported elsewhere.2,9,10 In 2004, a repeat survey was performed, with 60% (n = 6400) of the original cohort attending a testing site for follow-up data collection.12 At baseline and at follow-up, those who attended the testing site underwent a physical examination that included blood pressure measurements, collection of blood samples after an overnight fast, collection of a random spot morning urine specimen, and a standard 75 g oral glucose tolerance test. Blood and urine samples were transferred to a central laboratory for analysis (baseline: Hitech Pathology, Melbourne, Vic; follow-up: Gribbles Pathology, Melbourne, Vic).12
CKD was defined as either urinary albumin to creatinine ratio ≥ 30 mg/g, or estimated glomerular filtration rate < 60 mL/min/1.73m2 (calculated according to the abbreviated Modification of Diet in Renal Disease Study formula).13,14
Previously diagnosed diabetes was defined as an affirmative response to the question “Have you ever been told by a doctor or nurse that you have diabetes?”.
Treated hypertension was defined as an affirmative response to the question “Are you currently taking tablets for high blood pressure?”.
Untreated hypertension was defined as measured systolic blood pressure > 140 mmHg or diastolic blood pressure > 90 mmHg, excluding those who reported taking blood pressure-lowering medication.
The Stata MRTAB module (for computing one- and two-way tables of multiple responses) was used to calculate Pearson χ2 statistics, assessing whether the proportion giving each response differed significantly between subgroups (men v women, treated hypertension v no hypertension/untreated hypertension, existing diabetes v no diabetes, CKD at baseline v no CKD at baseline).15 P values for significance tests were adjusted for the fact that multiple tests were performed (Bonferroni method).16
The overall and nested cohorts resembled each other in terms of age and sex (Box 1). Baseline prevalence of CKD was also similar between the two cohorts. However, the nested follow-up cohort had slightly lower prevalences of previously diagnosed diabetes, prior stroke and untreated hypertension at baseline. The proportions of people who had completed tertiary education, lived outside a state capital city and were non-smokers were higher for the nested cohort.
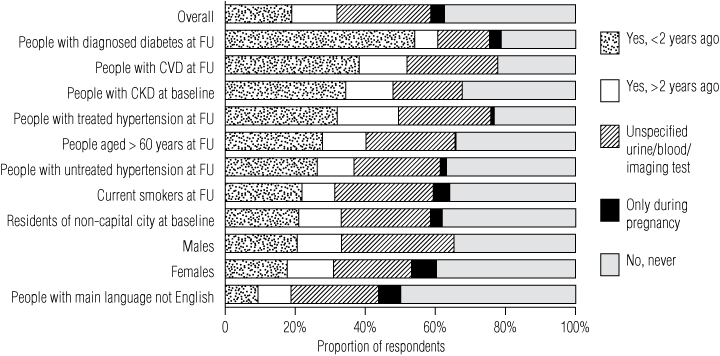
The proportions of respondents in various risk categories who at least suspected they had undergone a kidney function test in the past (other than during the AusDiab study) are shown in Box 4. Those with CKD at the time of the baseline survey more frequently responded that their kidney function had been tested within the previous 2 years (34.4% v 19% overall). Those with known diabetes were the most likely to recall having undergone a test of kidney function within the previous 2 years (54.1%). Women less frequently recalled having had a test of kidney function within the previous 2 years than men (17.7% v 20.6%, respectively), and people whose main language was not English were less likely to recall being tested within the previous 2 years than native English speakers (9.4% v 19.4%, respectively).
Awareness of risk factors for kidney disease was low in the cohort surveyed. Most end-stage kidney disease in Australia is attributable to diabetic nephropathy, hypertension and glomerulonephritis (with a range of inflammatory and immune causes).17 However, only a small proportion of respondents identified diabetes or hypertension as risk factors for kidney disease. The prevailing understanding appears to be that kidney disease is related to alcohol misuse, which may stem from recognition of the role of the kidneys in excreting wastes and toxins, or simply confusion between toxicity to the kidneys and toxicity to the liver. This perception is supported by only a small and somewhat conflicting evidence base.18,19 Poor diet was also commonly identified by respondents as being related to the development of kidney disease, implying general recognition of the significance of lifestyle factors.
Our survey was modest in scale, and the loss of many original participants to follow-up between baseline and the 5-year follow-up survey limits the degree to which our findings can be generalised. Compared with the general Australian population, adults aged 25–44 years and those aged 75 years or over were under-represented in our study cohort. Age distribution in the nested cohort was: 32.0% aged 25–44 years, 62.4% aged 45–74 years and 5.5% aged ≥ 75 years (compared with 42.5%, 47.9% and 9.6%, respectively, for the overall Australian population).20 Our study participants had a higher rate of high school completion than the general population over 25 years (64.3% v 45.5%). In addition, fewer people in the nested cohort had diabetes, untreated hypertension or a history of cardiovascular events, or were smokers at baseline, than in the overall cohort (and likely in the general population).
2 Frequency of the most popular responses to the question “What sort of things do you think may lead to a person developing kidney disease?”, overall and by sex*
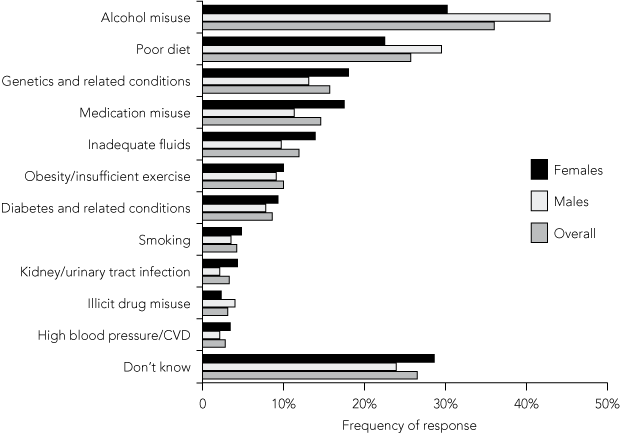 | |||||||||||||||
Received 28 May 2007, accepted 4 October 2007
- Sarah L White1
- Kevan R Polkinghorne2
- Alan Cass1
- Jonathan Shaw3
- Robert C Atkins2
- Steven J Chadban4
- 1 Renal Division, The George Institute, Sydney, NSW.
- 2 Monash Medical Centre, Melbourne, VIC.
- 3 International Diabetes Institute, Melbourne, VIC.
- 4 Department of Transplantation, Royal Prince Alfred Hospital, Sydney, NSW.
None identified.
- 1. Levey AS, Coresh J, Balk E, et al. National Kidney Foundation practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Ann Intern Med 2003; 139: 137-147.
- 2. Chadban SJ, Briganti EM, Kerr PG, et al. Prevalence of kidney damage in Australian adults: the AusDiab kidney study. J Am Soc Nephrol 2003; 14 (7 Suppl 2) : S131-S138.
- 3. Keith DS, Nichols GA, Gullion CM, et al. Longitudinal follow-up and outcomes among a population with chronic kidney disease in a large managed care organization. Arch Intern Med 2004; 164: 659-663.
- 4. Go AS, Chertow GM, Fan D, et al. Chronic kidney disease and the risks of death, cardiovascular events, and hospitalization. N Engl J Med 2004; 351: 1296-1305.
- 5. Chow FY, Briganti EM, Kerr PG, et al. Health-related quality of life in Australian adults with renal insufficiency: a population-based study. Am J Kidney Dis 2003; 41: 596-604.
- 6. Johnson DW. Evidence-based guide to slowing the progression of early renal insufficiency. Intern Med J 2004; 34: 50-57.
- 7. Trivedi HS, Pang MM, Campbell A, Saab P. Slowing the progression of chronic renal failure: economic benefits and patients’ perspectives. Am J Kidney Dis 2002; 39: 721-729.
- 8. Harris M, Bailey L, Bridges-Webb C, et al. Guidelines for preventive activities in general practice. 6th ed. Melbourne: Royal Australian College of General Practitioners, 2005. http://www.racgp.org.au/Content/NavigationMenu/ClinicalResources/RACGPGuidelines/TheRedBook/2005Redbook_6th_ed.pdf (accessed Dec 2007).
- 9. Dunstan DW, Zimmet PZ, Welborn TA, et al. The rising prevalence of diabetes and impaired glucose tolerance: the Australian Diabetes, Obesity and Lifestyle Study. Diabetes Care 2002; 25: 829-834.
- 10. Briganti EM, Shaw JE, Chadban SJ, et al. Untreated hypertension among Australian adults: the 1999–2000 Australian Diabetes, Obesity and Lifestyle Study (AusDiab). Med J Aust 2003; 179: 135-139. <MJA full text>
- 11. Dunstan DW, Zimmet PZ, Welborn TA, et al. The Australian Diabetes, Obesity and Lifestyle Study (AusDiab) — methods and response rates. Diabetes Res Clin Pract 2002; 57: 119-129.
- 12. Barr ELM, Magliano DJ, Zimmet PZ, et al. AusDiab 2005: the Australian Diabetes, Obesity and Lifestyle Study. Melbourne: International Diabetes Institute, 2006. http://www.diabetes.com.au/pdf/AUSDIAB_Report_Final.pdf (accessed Dec 2007).
- 13. Levey AS, Bosch JP, Lewis JB, et al. A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Modification of Diet in Renal Disease Study Group. Ann Intern Med 1999; 130: 461-470.
- 14. Levey AS, Greene T, Kusek JW, et al. A simplified equation to predict glomerular filtration rate from serum creatinine [abstract]. J Am Soc Nephrol 2000; 11: A0828.
- 15. Jann B. Tabulation of multiple responses. Stata J 2005; 5: 92-122.
- 16. Wright SP. Adjusted p-values for simultaneous inference. Biometrics 1992; 48: 1005-1013.
- 17. McDonald S, Chang S, Excell L. New patients. In: McDonald S, Chang S, Excell L, editors. ANZDATA registry report 2006. Adelaide: Australia and New Zealand Dialysis and Transplant Registry, 2006.
- 18. Schaeffner ES, Kurth T, de Jong PE, et al. Alcohol consumption and the risk of renal dysfunction in apparently healthy men. Arch Intern Med 2005; 165: 1048-1053.
- 19. Shankar A, Klein R, Klein BE. The association among smoking, heavy drinking, and chronic kidney disease. Am J Epidemiol 2006; 164: 263-271.
- 20. Australian Bureau of Statistics. Census tables, 2006. Canberra: ABS, 2007. (ABS Cat. No. 2068.0.) http://www.abs.gov.au/ausstats/abs@.nsf/productsbytitle/A6D6129396973B5A CA257306000D4DB9?OpenDocument (accessed Dec 2007).





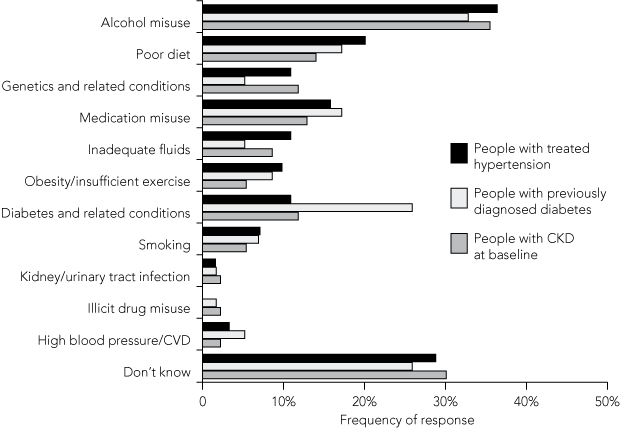
Abstract
Objectives: To explore awareness of the causes of kidney disease and recollection of kidney function testing in a cohort of Australian adults.
Design, setting and participants: An interviewer-administered cross-sectional survey, conducted from October to December 2004 as a nested study within the 5-year follow-up phase of the Australian Diabetes, Obesity and Lifestyle Study (AusDiab); 852 subjects who attended a testing site in New South Wales were interviewed.
Main outcome measures: Responses to the questions “What sort of things do you think may lead to a person developing kidney disease?” and “Has a doctor or health care worker ever tested your kidney function, outside of the AusDiab study?”
Results: Respondents most commonly believed that kidney disease was caused by alcohol misuse or poor diet, with few identifying diabetes or high blood pressure. Awareness of risk factors was no greater in respondents identified as having chronic kidney disease (CKD). A third of respondents with CKD recalled having undergone a test of kidney function within the previous 2 years, while another third replied they had never had their kidney function tested. Of participants with previously diagnosed diabetes or treated hypertension, 54.1% and 32.0%, respectively, reported having their kidney function tested within the previous 2 years.
Conclusions: Knowledge of risk factors for kidney disease and recall of kidney function testing were both limited, even among subgroups of the cohort who were at greatest risk of CKD. Prevention efforts may benefit from public and patient education to improve recognition of risk factors for CKD.