Depression is characterised by persistent depressed mood or loss of interest in activities.1 It is a relapsing or recurring disorder — relapse is defined as early return of symptoms before full recovery, while recurrence is a later return of symptoms after a period of remission.2 The relapse rate of depression in primary care ranges from about 37% to 45%, and up to 20% of people with depression have a chronic course.3,4 An important role of primary care is long-term mental health care, including relapse prevention.5-7
An integrated primary care depression relapse prevention program called “Keeping the blues away” (KBA) has been developed for the general practice setting.8 KBA aims to improve outcomes for patients by reducing the severity and relapse rate of depression, and improving quality of life.
We undertook a pilot cluster randomised controlled trial to test the hypothesis that KBA would provide a 50% relative reduction of depression relapse (ie, from an estimated 40% relapse rate down to 20%), compared with usual care. We also anticipated that KBA would improve the process of care.
During preclinical and exploratory phases, resources for the study were developed and studied to ensure acceptability.9
A randomised controlled trial in South Australian general practices was then conducted to compare usual care with KBA. Randomisation by practice was chosen to reduce the likelihood of treatment contamination (where the control group learns of the intervention) between groups.10 Stratified randomisation was used to ensure equal proportions of rural and urban practices, and small versus large practices (> 3 doctors), in each arm of the study. Random allocation was performed using computer-generated random numbers.
The study’s primary outcome was reduction in the rate of depression relapse. Secondary outcomes were reduction in the severity of depression and improvements in quality of life. The use of both quantitative and qualitative approaches was important to enable measurement of depression levels and relapses, and to elicit information about patients’ and general practitioners’ experiences of KBA.
Five South Australian Divisions of General Practice were contacted in February 2004, and a letter inviting GPs to participate was sent to about 400 GP members. A total of 45 GPs from 23 urban and rural practices responded and agreed to participate.
GP recruitment of patients began in May 2004, and the study ended in December 2005. GPs identified patients aged 18 years or older who met diagnostic criteria for a depressive disorder according to the Diagnostic and statistical manual of mental disorders, fourth edition (DSM-IV).1 Other patient inclusion criteria were availability to be followed up for the next 12 months, and ability to give informed consent. Patients were excluded if they were known to be undergoing a separate treatment program, were suffering from psychoses, or were unable to complete the English-language questionnaires or interview.
Sample size calculations indicated that 120 patients would be required in each of the intervention and control groups (95% confidence, 80% power, assuming a design effect of 1.5 due to clustering).10
KBA is based on the literature, current thinking and clinical experience.8 Medication is used as clinically indicated, and the program is started once the patient’s depression has been stabilised by initial treatment. KBA involves a novel, multimodal, skills-based approach. It incorporates 10 steps and utilises a range of evidence-based psychosocial strategies, such as problem solving (Box 1).12,13
Intervention-group GPs and patients were provided with resources including a GP training manual or patient manual and a purpose-designed relaxation CD.14,15 GPs in the intervention group completed 20 hours of training, conducted by a GP and a psychologist. Their training kit contained information on depression, the study protocol, assessment tools, and skills training related to the KBA program. GPs in the control group completed a 3-hour training session on the study protocol.
GPs were asked to administer psychological assessment tools to their participating patients at baseline, 3 months and 12 months. Depression severity was assessed with the self-rating Depression Anxiety Stress Scales (DASS),16 and quality of life with the World Health Organization Quality of Life scale (WHOQOL-BREF).17
At the end of the trial, a series of semistructured interviews were conducted to gather information about GP and patient experiences. A purposive sampling technique was used to select a representative range of GPs to be interviewed by a project officer (W L N).18 These GPs then contacted a number of patients to be interviewed. Interview data were analysed using content analysis.19
Characteristics of practices, GPs and patients in the intervention and control groups are shown in Box 2. The characteristics of practices involved in the trial were relatively balanced. There were more urban than rural practices recruited to the study, and most were group practices. More female than male GPs participated, and the mean age of GPs in each arm of the study was 45 years.
A total of 110 patients participated in the study — a smaller sample size than required. Balanced numbers of female and male patients were recruited into each arm of the study, with ages in the intervention group ranging from 18 to 62 years (mean, 39 years), and from 19 to 74 years in the control group (mean, 40 years). Patients in the intervention group had more severe depression at the outset of the study (Box 2). Pathways of participants within the trial are shown in Box 3.
There were no statistically significant differences between the two groups in depression relapse rates (χ21 = 1.51; P = 0.23). However, there was a non-significant tendency for relapse to be reduced in the intervention group (RR = 0.77; 95% CI, 0.50–2.05) (Box 4).
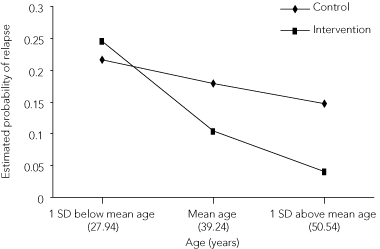
In the final regression model, age was predictive of depression relapse, with increased age associated with decreased risk of relapse. Older patients (≥ 50 years) in the intervention group showed a significantly lower probability of relapse than those in the control group (P = 0.018) (Box 5). “Older” refers to one standard deviation above the mean age (where mean = 39.24 and SD = 11.30). Younger people in either group tended to show similar probability of relapse.
Sex approached significance, with women in both groups less likely to relapse (P = 0.069).
The regression model indicated that the interactions of duration of depressive symptoms, days from baseline, and group were significant predictors of severity of depression.
Baseline depression scores were higher for the intervention group (Box 6). There was a general decrease in scores over time, with patients in the intervention group who had experienced depressive symptoms for < 6 months and those in the control group (regardless of symptom duration) showing similar values. Patients in the intervention group who had experienced depression for > 6 months had higher depression scores at the start of the trial, but by 12 months after baseline their depression scores were indistinguishable from those of most other patients (Box 6). This reduction approached significance (P = 0.06).
This study examining rates of depression relapse in a primary care population undertaking a novel, multifaceted relapse prevention program had some clinically relevant findings. KBA was found to have potential for older patients (aged ≥ 50 years), for those with more severe depression at the outset, and those who had experienced depression for more than 6 months. Even though the primary outcome of reducing depression relapse by 50% was not achieved, KBA was found to be a promising and well accepted program.
This study had a relatively small number of participants, limiting its power. However, recruitment in general practice is often challenging.20 Further, the impact of the intervention may have been disadvantaged by the more severe depression rates in the KBA group at baseline.
A strength of the study is that it was undertaken in multiple and varied general practices, suggesting that the results may be generalisable across a range of practices. The KBA program can be easily incorporated into practice, assisted by its manualised format and associated training program. Future plans include assessing a computer-assisted version of KBA in primary care settings.
This study highlights the potential for interventions such as KBA to be incorporated into the clinical setting, and to have a positive impact on health outcomes. Further research on the KBA program is planned.
1 The “Keeping the blues away” (KBA) program
The KBA program aims to reduce the severity and relapse of depression. It is based on literature, current thinking and clinical experience. The literature supports a range of treatment strategies that help prevent depression relapse, and highlights the need for novel, multifaceted, skills-based treatment approaches.11 KBA incorporates evidence-based strategies and current management guidelines, and involves a multimodal, skills-based treatment approach.
KBA is based on 10 steps that can be tailored to the individual patient:
1. Medical and psychosocial assessment, goal-setting and monitoring progress
2. Information about depression and anxiety, and relapse prevention
3. Healthy lifestyle issues (nutrition, exercise, sleep, managing stress)
4. Useful coping skills (mood diary, problem solving, relaxation techniques and dealing with panic episodes)
5. Helpful thinking or cognitive strategies (thought monitoring, analysis and challenging, mindfulness-based cognitive behavioural approaches)
6. Dealing with psychological issues (self-esteem, loss and grief, anger and guilt, hopelessness and suicidal thoughts, finding hope and meaning)
7. The benefits of activity (activity scheduling, humour, giving)
8. Fostering social support and skills (connectedness, assertiveness, relationship issues and unemployment)
9. Developing a plan to manage early symptoms of relapse
10. Reassessment, review and helpful resources
2 Baseline characteristics of general practices and participants in each study group
Characteristic |
Intervention |
Control |
|||||||||||||
General practices |
|||||||||||||||
Urban |
9 |
8 |
|||||||||||||
Rural |
3 |
3 |
|||||||||||||
Total |
12 |
11 |
|||||||||||||
General practitioners |
|
||||||||||||||
Male |
8 |
5 |
|||||||||||||
Female |
14 |
18 |
|||||||||||||
Total |
22 |
23 |
|||||||||||||
In group practice |
17 |
21 |
|||||||||||||
In solo practice |
4* |
1* |
|||||||||||||
Mean age in years (range) |
45 (33–58) |
45 (30–60) |
|||||||||||||
Patients |
|
|
|||||||||||||
Male |
16 |
8 |
|||||||||||||
Female |
46 |
40 |
|||||||||||||
Total |
62 |
48 |
|||||||||||||
Mean age in years (range) |
39 (18–62) |
40 (19–74) |
|||||||||||||
Past history of depression |
42 |
37 |
|||||||||||||
Mean DASS depression score |
33 (extreme) |
28 (severe) |
|||||||||||||
|
DASS = Depression Anxiety Stress Scales. * One GP from each group withdrew early in the study due to work commitments or distance to travel for training. | |||||||||||||||
3 Pathway of participants through the study
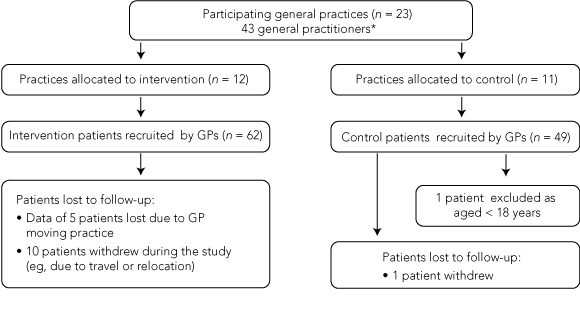 | |||||||||||||||
|
* Two of the 45 GPs who agreed to participate withdrew early in the study due to work stress and the distance to travel for training. | |||||||||||||||
4 Number and proportion of patients with and without depression relapse in each study group
|
Control |
Intervention |
Total |
||||||||||||
No relapse |
33 (40.2%) |
49 (59.8%) |
82 |
||||||||||||
Relapse |
15 (53.6%) |
13 (46.4%) |
28 |
||||||||||||
Total |
48 |
62 |
110 |
||||||||||||
6 Severity of depression over time, by group and duration of depressive symptoms
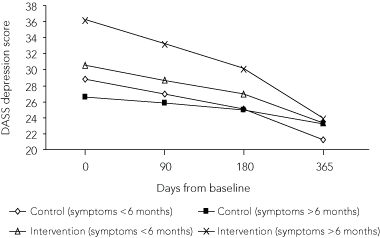 | |||||||||||||||
|
DASS = Depression Anxiety Stress Scales. | |||||||||||||||
- Catherine A Howell1
- Deborah A Turnbull2
- Justin J Beilby3
- Charlotte A Marshall4
- Nancy Briggs1
- Wendy L Newbury1
- 1 Discipline of General Practice, University of Adelaide, Adelaide, SA.
- 2 School of Psychology, University of Adelaide, Adelaide, SA.
- 3 Faculty of Health Sciences, University of Adelaide, Adelaide, SA.
- 4 Adelaide North East Division of General Practice, Adelaide, SA.
Thank you to Melissa Opolski and to the Discipline of General Practice, University of Adelaide, Primary Health Care Research Evaluation and Development Program, beyondblue: the national depression initiative, Royal Australian College of General Practitioners, and Spencer Gulf Rural Health School, who provided funding for the study.
None identified.
- 1. American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4th ed. Washington, DC: APA, 1994.
- 2. Kupfer DJ, Frank E, Perel JM. The advantage of early treatment intervention in recurrent depression. Arch Gen Psychiatry 1989; 46: 771-775.
- 3. Katon W, Rutter C, Ludman EJ, et al. A randomized trial of relapse prevention of depression in primary care. Arch Gen Psychiatry 2001; 58: 241-247.
- 4. Wilson I, Duszynski K, Mant A. A 5-year follow-up of general practice patients experiencing depression. Fam Pract 2003; 20: 685-689.
- 5. Andrews G. Should depression be managed as a chronic disease? BMJ 2001; 322: 419-421.
- 6. Hickie IB. An approach to managing depression in general practice. Med J Aust 2000; 173: 106-110. <MJA full text>
- 7. Rost K, Nutting P, Smith JL, et al. Managing depression as a chronic disease: a randomised trial of ongoing treatment in primary care. BMJ 2002; 325: 934.
- 8. Howell CA. Preventing depression relapse: a primary care approach. Prim Care Mental Health 2004; 2: 151-156.
- 9. Campbell M, Fitzpatrick R, Haines A, et al. Framework for design and evaluation of complex interventions to improve health. BMJ 2000; 321: 694-696.
- 10. Torgerson DJ. Contamination in trials: is cluster randomisation the answer? BMJ 2001; 322: 355-357.
- 11. Segal ZV, Pearson JL, Thase ME. Challenges in preventing relapse in major depression. Report of a National Institute of Mental Health Workshop on state of the science of relapse prevention in major depression. J Affect Disord 2003; 77: 97-108.
- 12. Mynors-Wallis LM, Gath DH, Day A, Baker F. Randomised controlled trial of problem solving treatment, antidepressant medication, and combined treatment for major depression in primary care. BMJ 2000; 320: 26-30.
- 13. Paykel ES, Scott J, Teasdale JD, et al. Prevention of relapse in residual depression by cognitive therapy: a controlled trial. Arch Gen Psychiatry 1999; 56: 829-835.
- 14. Howell CA. Keeping the blues away: a guide to reducing the relapse of depression. Adelaide: University of Adelaide, 2007.
- 15. Howell CA. Keeping the blues away: relaxation CD. Adelaide: University of Adelaide, 2007.
- 16. Lovibond SH, Lovibond PF. Manual for the Depression Anxiety Stress Scales. Sydney: Psychology Foundation of Australia, 1995.
- 17. Murphy B, Herrman H, Hawthorne G, et al. The World Health Organization Quality of Life (WHOQOL) Study: Australian WHOQOL-100, WHOQOL-BREF and CA-WHOQOL instruments user’s manual and interpretation guide. Melbourne: WHOQOL Field Study Centre, Department of Psychiatry, University of Melbourne and St Vincent’s Mental Health Service, 2000.
- 18. Murray SA, Boyd K, Kendall M, et al. Dying of lung cancer or cardiac failure: prospective qualitative interview study of patients and their carers in the community. BMJ 2002; 325: 929-932.
- 19. Pope C, Ziebland S, Mays N. Analysing qualitative data. In: Pope C, Mays N, editors. Qualitative research in health care. 2nd ed. London: BMJ Books, 1999: 75-87.
- 20. Veitch C, Hollins J, Worley P, Mitchell G. General practice research. Problems and solutions in participant recruitment and retention. Aust Fam Physician 2001; 30: 399-406.





Abstract
Objectives: To determine the effectiveness of “Keeping the blues away” (KBA), a manualised depression relapse prevention program for general practice, in reducing the relapse of depression compared with usual care (with the aim of halving the relapse rate), and in reducing depression severity and improving the process of care.
Design and setting: A cluster randomised controlled trial conducted in 2004–2005 in South Australian general practices.
Participants: 43 general practitioners from 23 urban and rural practices recruited 110 patients with depression (age range, 18–75 years).
Intervention: GP training manual or patient manual and relaxation CD; 20 hours of training on depression, the study protocol, assessment tools and skills.
Main outcome measures: Relative risk (RR) of depression relapse; depression severity and quality of life scores.
Results: There were no significant differences in relapse rates between the groups (χ21 = 1.51; P = 0.23), although there was a non-significant tendency for relapse to be reduced in the KBA group (RR = 0.77; 95% CI, 0.50–2.05). Older patients (≥ 50 years) in the KBA group showed a significantly lower probability of relapse than those in the control group (P = 0.018). There was a decrease in depression scores in both groups. KBA participants had more severe depression at baseline, and the reduction in severity in those with symptoms for > 6 months was nearly significant (P = 0.06). KBA was positively received by GPs and patients.
Conclusions: Although this pilot study of a small sample did not achieve its primary outcome of reducing depression relapse by 50%, KBA was found to be a promising program for older patients and for those with more severe or persistent symptoms.