Diabetes mellitus is a major health problem in Western countries, and is one of the most common chronic diseases in young people. There is considerable variation in disease onset, clinical course and risk of premature mortality.1,2 While there has been greater focus on the more common type 2 diabetes, people with type 1 diabetes also have an increased mortality risk compared with the general population.3-6
Measures to reduce mortality in people with type 1 diabetes hinge on our knowledge of the exact causes of death, thereby allowing appropriate prevention and treatment strategies. While many mortality studies in young people with type 1 diabetes have been published in the United Kingdom and Europe,3-5,7-15 few have been performed in Australia.6
An important subgroup of deaths among young people with type 1 diabetes is sudden unexpected death in the absence of a clear cause (eg, hypoglycaemia or cardiac autonomic dysfunction). Little is known about the extent of this problem, although isolated reports suggest a particular type of sudden death, referred to as “dead-in-bed” syndrome.9,16 Typically, these people are in good health when they retire to bed, only to be found dead the next morning. The bed is most often undisturbed, suggesting no seizure activity.
This study was performed to identify the causes of death in young Australians with type 1 diabetes in a large postmortem series, with a particular focus on sudden death.
We retrospectively reviewed all autopsies performed at the Department of Forensic Medicine in Sydney, New South Wales, from 1 January 1994 to 31 December 2006.
All studies and data review were performed in accordance with the Sydney South West Area Health Service human ethics guidelines. The NSW Deputy State Coroner gave permission for the study.
We selected autopsies of deceased people known to have type 1 diabetes mellitus by searching the ISYS Query database system (ISYS Search Software, Sydney, NSW) at the Department of Forensic Medicine. Autopsy reports containing the words “diabetes” or “diabetic” were identified, and the records extracted. All available demographic, clinical and autopsy data were collected for each individual. People with secondary diabetes or diabetes insipidus were excluded. In autopsy reports that only mentioned diabetes mellitus, the type was classified using the following criteria:
Type 1: People who were taking insulin and were aged 40 years or younger at their first insulin use, or who were aged 40 years or younger at the time of diabetes diagnosis; a body mass index less than 28 kg/m2 was consistent with type 1 diabetes.17
Type 2: People whose diabetes was controlled by diet and/or oral hypoglycaemic drugs, or whose diabetes was insulin-treated but who were aged over 40 years at their first insulin injection.
For comparison with the group of young people with type 1 diabetes (≤ 40 years), all postmortem data on individuals without diabetes were also collected (from the same forensic department over the same period). The control group consisted of people aged 40 years or younger and was sex-matched to the group with type 1 diabetes.
We reviewed 26 682 autopsy reports for the study period. There were 1914 people known to have had diabetes mellitus, 400 with type 1 and 1514 with type 2 diabetes (Box 1). Among those with type 1 diabetes, 67 were aged 40 years or younger and 333 were aged over 40 years (Box 1).
For the whole group, cardiovascular disease (CVD) was the most common underlying cause of death (45%), followed by unnatural deaths (14%), respiratory causes (10%) and acute complications of diabetes (9%). The distribution of causes of death in individuals at all ages with type 1 diabetes is shown in Box 2. CVD was not the most common cause of mortality in those aged 40 years or less (Box 3, A). The three most common causes of death in this age group were acute diabetic complications (27%), unnatural deaths (28%), and sudden unexpected deaths (22%), while CVD accounted for only 13% (Box 3, A; P < 0.001 in all comparisons with those aged > 40 years).
In those aged over 40 years, CVD was responsible for the majority of deaths (51%; P < 0.001 v those aged ≤ 40 years). Furthermore, acute diabetic complications, unnatural deaths, and sudden unexpected deaths were less frequent (5%, 11%, and 5%, respectively) than in those aged 40 years or younger (Box 3, A).
The causes of death in those aged 40 years or less with type 1 diabetes were then compared with a sex-matched control group of people in the same age range without diabetes (n = 6990). Sixty-four individuals without diabetes were excluded from the control group because the cause of death was not available. In the group without diabetes (Box 3, B), unnatural deaths dominated as the Coroner’s ascribed cause of death (72%), a percentage similar to the combined causes of sudden unexpected death, acute diabetic complications and unnatural death in the group with type 1 diabetes (Box 3, B). Importantly, the frequency of sudden unexpected death in the young population with type 1 diabetes (22%) was significantly higher than that in the group without diabetes (5%; P < 0.001 v type 1 diabetes; Box 3, B).
The specific causes of death in the sudden unexpected and unnatural categories in those with type 1 diabetes aged 40 years or younger are shown in Box 4.
Of the 15 sudden unexpected deaths in the young type 1 diabetes group, 10 were attributed to dead-in-bed syndrome (Box 4). The mean age (SD) of dead-in-bed syndrome victims was 30.2 (9.4) years, with a male predominance of 4 : 1. The remaining five people had sudden unexpected deaths with no cause identified at autopsy, hence were referred to as undetermined (Box 4).
This autopsy study describes the causes of mortality in a group of young Australians with type 1 diabetes. The distribution of causes varied significantly between older and younger people with type 1 diabetes, with cardiovascular causes being the predominant cause of death in those aged over 40 years, as previously reported.4,14,15 Mortality from acute diabetic complications, unnatural deaths, and sudden unexpected deaths was much higher than from any other specific causes in people aged 40 years or younger. Specifically, sudden unexpected death made up a larger proportion of causes of death in the type 1 diabetes group compared with a control population without diabetes (22% v 5%), with at least some of the difference likely to relate to diabetes-specific causes of dead-in-bed syndrome.
Overall, the causes of death in young people with type 1 diabetes are consistent with previously reported studies. For example, a large fraction of deaths were attributed to acute complications of diabetes.3,4,7,9,12-14 Most recently, a report on early mortality in type 1 diabetes in Europe identified 141 deaths, with diabetes-related deaths accounting for 35%, consistent with our rate of 27%.18 In the same study, 2.1% fulfilled the criteria for dead-in-bed syndrome, a rate similar to the 2.5% observed in our type 1 diabetes group.18 Furthermore, suicide accounted for 7.8% of deaths in the European study, compared with 4.4% in our young group. Similarly, a higher incidence of accidents, suicides and homicide in young people with type 1 diabetes (compared with young people without diabetes) has also been previously reported.7 In addition, some risk-taking behaviour in young people with type 1 diabetes may contribute to deaths from acute diabetes complications, including deaths due to diabetic ketoacidosis where insulin omission and delayed presentation for medical care are recognised factors in its pathogenesis.11
A strongly statistically significant and clinically important finding in our study was the high incidence of sudden unexpected death in young people with type 1 diabetes. The greatest percentage of unexpected deaths as a cause of death clearly occurred in people with type 1 diabetes who were aged 40 years or less, compared with either older people or with younger people who did not have diabetes. Ten of these sudden deaths met the criteria for dead-in-bed syndrome.16 These deaths amounted to 67% of all sudden unexpected deaths, similar to the previously reported incidences of dead-in-bed syndrome.16,19,20
Dead-in-bed syndrome was first described in 14 people with type 1 diabetes in 1991.16 The syndrome is poorly understood, with little information available on the prevalence, aetiology, triggers and overall pathogenesis.
Acute hypoglycaemia may play a role.16,19-21 However, hypoglycaemia is a common occurrence among patients with type 1 diabetes, but it rarely results in sudden death.16 This implies that other mechanisms are likely to be involved. For example, patients with long-standing type 1 diabetes may have reduced parasympathetic activity and increased sympathetic activity.22 These effects have been associated with lowered baroreceptor-cardiac reflex sensitivity in individuals with type 1 diabetes, which could result in increased susceptibility to ventricular arrhythmias.23 Moreover, the risk of such ventricular arrhythmias is compounded by nocturnal episodes of hypoglycaemia — research has demonstrated that patients with type 1 diabetes, with normal or abnormal cardiac autonomic function, have a prolonged QTc (corrected QT) interval during hypoglycaemia.24,25
As a further consideration, genetic predisposition to prolonged QTc interval prolongation is well recognised in the general community. Considering this, it is possible that multiple factors in one person — type 1 diabetes, a genetic predisposition to QT interval prolongation, cardiac autonomic neuropathy and acute severe hypoglycaemia — collectively cause arrhythmia and lead to dead-in-bed syndrome.
In studies currently in progress, we are examining DNA samples for changes in sodium and potassium ion channel genes for such genetic predisposition to life-threatening arrhythmia in those with type 1 diabetes who had sudden unexpected death.
Limitations of this study included possible under-reporting of diabetes at postmortem examination, insufficient clinical history (eg, duration of diabetes), and difficulties with establishing the exact cause of death in people with diabetes, who often have multiple concurrent pathological abnormalities.
In addition, it should be noted that this was a single-centre postmortem-based analysis. These results do not represent the mortality of the total population with diabetes, but only those referred to the Coroner for medicolegal investigation. Such deaths include any suspicious or potentially unnatural deaths, sudden unexpected deaths where the cause of death is not readily apparent and deaths following or as a result of anaesthesia. However, the referral rate seems to be high. According to the Australian National Diabetes Register, about 46 people with type 1 diabetes younger than 40 years died over a 6-year period in NSW.2 In our study, 67 deaths were reported over the 12-year period. This suggests that more than 50% of such deaths in people with type 1 diabetes aged less than 40 years are reported to the Coroner.
Our findings highlight the ongoing need to optimise clinical management approaches in young people with type 1 diabetes, using a multidisciplinary team approach to address specific issues in young people. This includes prevention of acute metabolic complications by improving drug treatments and compliance, identification of psychosocial problems that may predispose to risk-taking behaviour, and further clinical and genetic research studies to unravel the precise mechanisms involved in dead-in-bed syndrome.
1 Flow diagram showing the classification of autopsy reports by diabetes status, New South Wales, 1994–2006
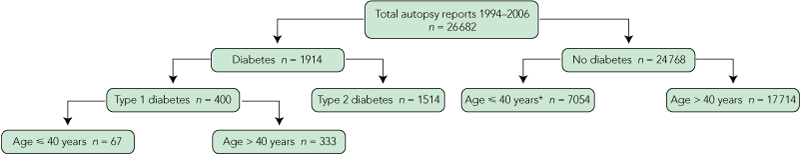
* Sixty-four reports in this category were excluded because cause of death was not available.
2 Cause of death in people with type 1 diabetes, New South Wales, 1994–2006
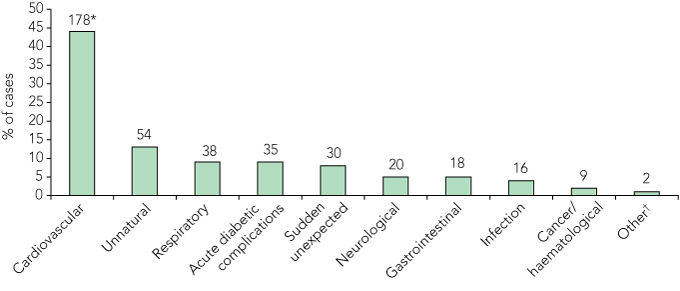
* Numbers above columns represent the number of deaths in each category.
† Other = deaths that could not be categorised (eg, hypothermia, intravascular coagulation).
3 Cause of death by age and diabetes status, New South Wales, 1994–2006
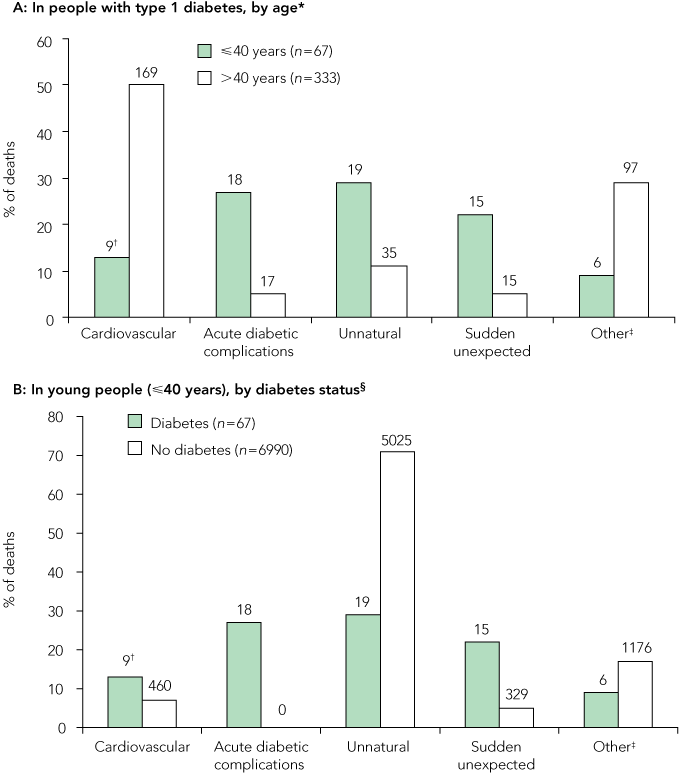
* For all comparisons shown, P < 0.001. † Numbers above columns represent the number of deaths in each category. ‡ “Other” includes respiratory, neurological, gastrointestinal, cancer/haematological, infection, and deaths that could not be categorised (eg, hypothermia, intravascular coagulation). § P < 0.001 for all comparisons shown, except Cardiovascular and Other, for which P < 0.05.
4 Sudden unexpected and unnatural deaths in people with type 1 diabetes aged ≤ 40 years, New South Wales, 1994–2006
Cause of death |
No. |
||||||||||||||
Sudden and unexpected |
|
||||||||||||||
Dead-in-bed syndrome |
10 |
||||||||||||||
Undetermined |
5 |
||||||||||||||
Total |
15 |
||||||||||||||
Unnatural |
|
||||||||||||||
Fall |
1 |
||||||||||||||
Drowning |
1 |
||||||||||||||
Motor vehicle accident |
1 |
||||||||||||||
Narcotic overdose |
11 |
||||||||||||||
Other accidents |
2 |
||||||||||||||
Suicide |
3 |
||||||||||||||
Total |
19 |
||||||||||||||
Received 30 October 2007, accepted 7 February 2008
- Emily Tu1,2
- Stephen M Twigg2,3
- Johan Duflou4,5
- Christopher Semsarian1,2,6
- 1 Agnes Ginges Centre for Molecular Cardiology, Centenary Institute, Sydney, NSW.
- 2 Central Clinical School, Faculty of Medicine, University of Sydney, Sydney, NSW.
- 3 Department of Endocrinology, Royal Prince Alfred Hospital, Sydney, NSW.
- 4 Department of Forensic Medicine, Sydney, NSW.
- 5 Department of Pathology, University of Sydney, Sydney, NSW.
- 6 Department of Cardiology, Royal Prince Alfred Hospital, Sydney, NSW.
Emily Tu is the recipient of a National Heart Foundation of Australia postgraduate scholarship. Christopher Semsarian is the recipient of a National Health and Medical Research Council Practitioner Fellowship. This study was supported by project grants from the National Heart Foundation of Australia.
None identified.
- 1. Krolewski A, Warram J, Christlieb AR. Onset, course, complications and prognoses of diabetes mellitus. In: Marble A, Krall LP, Bradley RF, et al, editors. Joslin’s diabetes mellitus. 12th ed. Philadelphia: Lea & Febiger, 1985: 251-277.
- 2. Catanzariti L, Faulks K, Waters A-M. National Diabetes Register: statistical profile 1999–2005. Canberra: Australian Institute of Health and Welfare, 2007. (AIHW Cat. No. CVD 39. Diabetes Series No. 7.)
- 3. Joner G, Patrick S. The mortality of children with type 1 (insulin-dependent) diabetes mellitus in Norway, 1973-1988. Diabetologia 1991; 34: 29-32.
- 4. Laing SP, Swerdlow AJ, Slater SD, et al. The British Diabetic Association Cohort Study, II: cause-specific mortality in patients with insulin-treated diabetes mellitus. Diabet Med 1999; 16: 466-471.
- 5. McNally PG, Raymond NT, Burden ML, et al. Trends in mortality of childhood-onset insulin-dependent diabetes mellitus in Leicestershire: 1940–1991. Diabet Med 1995; 12: 961-966.
- 6. Riley MD, McCarty DJ, Couper DJ, et al. The 1984 Tasmanian insulin treated diabetes mellitus prevalence cohort: an eight and a half year mortality follow-up investigation. Diabetes Res Clin Pract 1995; 29: 27-35.
- 7. International evaluation of cause-specific mortality and IDDM. Diabetes Epidemiology Research International Mortality Study Group. Diabetes Care 1991; 14: 55-60.
- 8. Asao K, Sarti C, Forsen T, et al. Long-term mortality in nationwide cohorts of childhood-onset type 1 diabetes in Japan and Finland. Diabetes Care 2003; 26: 2037-2042.
- 9. Dahlquist G, Kallen B. Mortality in childhood-onset type 1 diabetes: a population-based study. Diabetes Care 2005; 28: 2384-2387.
- 10. Edge JA, Ford-Adams ME, Dunger DB. Causes of death in children with insulin dependent diabetes 1990–96. Arch Dis Child 1999; 81: 318-323.
- 11. Laing SP, Swerdlow AJ, Slater SD, et al. The British Diabetic Association Cohort Study, I: all-cause mortality in patients with insulin-treated diabetes mellitus. Diabet Med 1999; 16: 459-465.
- 12. Podar T, Solntsev A, Reunanen A, et al. Mortality in patients with childhood-onset type 1 diabetes in Finland, Estonia, and Lithuania: follow-up of nationwide cohorts. Diabetes Care 2000; 23: 290-294.
- 13. Schober E, Schneider U, Friedl HP, et al. Early mortality in childhood diabetes in Austria — a population based cohort study. Eur J Pediatr 1997; 156: 15-17.
- 14. Skrivarhaug T, Bangstad HJ, Stene LC, et al. Long-term mortality in a nationwide cohort of childhood-onset type 1 diabetic patients in Norway. Diabetologia 2006; 49: 298-305.
- 15. Soedamah-Muthu SS, Fuller JH, Mulnier HE, et al. All-cause mortality rates in patients with type 1 diabetes mellitus compared with a non-diabetic population from the UK general practice research database, 1992–1999. Diabetologia 2006; 49: 660-666.
- 16. Tattersall RB, Gill GV. Unexplained deaths of type 1 diabetic patients. Diabet Med 1991; 8: 49-58.
- 17. Balasubramanyam A, Garza G, Rodriguez L, et al. Accuracy and predictive value of classification schemes for ketosis-prone diabetes. Diabetes Care 2006; 29: 2575-2579.
- 18. Patterson CC, Dahlquist G, Harjutsalo V, et al. Early mortality in EURODIAB population-based cohorts of type 1 diabetes diagnosed in childhood since 1989. Diabetologia 2007; 50: 2439-2442.
- 19. Sartor G, Dahlquist G. Short-term mortality in childhood onset insulin-dependent diabetes mellitus: a high frequency of unexpected deaths in bed. Diabet Med 1995; 12: 607-611.
- 20. Borch-Johnsen K, Helweg-Larsen K. Sudden death and human insulin: is there a link? Diabet Med 1993; 10: 255-259.
- 21. Thordarson H, Sovik O. Dead in bed syndrome in young diabetic patients in Norway. Diabet Med 1995; 12: 782-787.
- 22. Weston PJ, Gill GV. Is undetected autonomic dysfunction responsible for sudden death in type 1 diabetes mellitus? The “dead in bed” syndrome revisited. Diabet Med 1999; 16: 626-631.
- 23. Weston PJ, James MA, Panerai R, et al. Abnormal baroreceptor-cardiac reflex sensitivity is not detected by conventional tests of autonomic function in patients with insulin-dependent diabetes mellitus. Clin Sci (Lond) 1996; 91: 59-64.
- 24. Bellavere F, Ferri M, Guarini L, et al. Prolonged QT period in diabetic autonomic neuropathy: a possible role in sudden cardiac death? Br Heart J 1988; 59: 379-383.
- 25. Marques JL, George E, Peacey SR, et al. Altered ventricular repolarization during hypoglycaemia in patients with diabetes. Diabet Med 1997; 14: 648-654.





Abstract
Objective: To determine the causes of death in Australians with type 1 diabetes mellitus who died aged 40 years or younger.
Design and setting: Retrospective review of autopsy reports at the Department of Forensic Medicine, Sydney, New South Wales, 1 January 1994 – 31 December 2006.
Main outcome measure: Causes of mortality in people with type 1 diabetes aged ≤ 40 years.
Results: Of the 26 682 autopsy reports, 1914 were for individuals with diabetes (type 1, 400; type 2, 1514). Cardiovascular disease accounted for 51% of deaths (169/333) in people with type 1 diabetes aged > 40 years, versus 13% among those aged ≤ 40 years (9/67; P = 0.001). Acute complications of diabetes (27%; 18/67), unnatural deaths (28%; 19/67), and sudden unexpected deaths (22%; 15/67) were the predominant causes of death in young individuals with diabetes. Sudden unexpected death was more common in those with type 1 diabetes compared with a sex-matched control population in the same age range (22% v 5%; χ2 P < 0.001). Of the sudden unexpected deaths, 10 people were found dead in an undisturbed bed with no cause of death found at autopsy (“dead-in-bed” syndrome; mean age [SD], 30.2 [9.4] years; males : females = 4 :1).
Conclusions: In deceased young people with type 1 diabetes examined by the Coroner, acute diabetic complications, unnatural causes, and sudden unexpected deaths were the predominant causes of death. The relatively high frequency of sudden unexpected deaths, such as dead-in-bed syndrome, requires further investigation.