In Australia, stillbirth is defined as no sign of life after birth in babies of at least 20 weeks’ gestation or at least 400 g birthweight. In the past 50 years, there has been a decline in the rate of both stillbirths and neonatal deaths in Australia and other developed countries. However, this decline has not been sustained and, in fact, stillbirth rates have remained static for the last 10 years.1 The most recent Australian data from the National Perinatal Statistics Unit (NPSU) reports a stillbirth rate of 7.3 per 1000 births.2 Stillbirths account for two-thirds of all perinatal deaths in Australia, and 28% of these remain unexplained.2
Classification of stillbirth is essential for both understanding and future prevention. In New South Wales, all perinatal deaths are reported to the Midwives Data Collection (MDC).3 Hospital guidelines for review and reporting of perinatal deaths are described in a NSW Department of Health circular.4 After hospital review, perinatal deaths of fetuses of at least 22 weeks’ gestation or 500 g birthweight are reviewed by the Perinatal Outcomes Working Party (POWP), which is a subgroup of NSW Health’s NSW Ministerial Maternal and Perinatal Committee.
New South Wales has been using the Perinatal Society of Australia and New Zealand perinatal death classification (PSANZ-PDC) since 2002.5 This classification system was previously called the Australia and New Zealand antecedent classification of perinatal mortality, and includes both obstetric and fetal factors, as well as autopsy findings and placental abnormality.6 It has reportedly high interobserver reliability, with a κ statistic ranging from 0.83–0.95.6
The NSW MDC is a population-based surveillance system covering all births in NSW public and private hospitals, as well as home births. It encompasses all livebirths and stillbirths of at least 20 weeks’ gestation or at least 400 g birthweight. The MDC relies on the attending midwife or doctor to complete a notification form when a birth occurs. Demographic, maternal health, pregnancy, labour, delivery, and perinatal outcomes data are collected.3
Data analysis was performed with SPSS, version 14.0 (SPSS Inc, Chicago, Illinois, USA). Independent proportions were compared using the χ2 test. Agreement between cause of death classifications by hospital review committees and the POWP was determined with pairwise κ statistics.7 The κ values were interpreted following previously described guidelines.8
Total stillbirths and stillbirth rates for the study period are shown in Box 1. Rates are presented for stillbirths at both 20 or more and 22 or more weeks’ gestation. Stillbirth rates were below 1 per 1000 undelivered pregnancies for gestation periods ranging from for 22–39 weeks; the rate increased markedly at later gestational ages with the rate for 40 weeks’ gestation being 1.56 per 1000, for 41 weeks’ being 7.75 per 1000 and for 42 weeks’ being 10.71 per 1000 undelivered pregnancies.
The classification of cause of death after review by the POWP is shown in Box 2. The most common classification was unexplained antepartum death. Over 60% of the stillbirths were attributable to the three most common classifications: unexplained antepartum death; congenital abnormality; and spontaneous preterm delivery. Fetal growth restriction as a classification of cause of death was attributed in only 3.2% of cases, however, infants in 288 stillbirths (22.8%) had a birthweight below the 10th percentile. This is likely to reflect the fact that further evidence (eg, placental evidence or ultrasound of growth restriction) is required for the classification of fetal growth restriction to be applied.
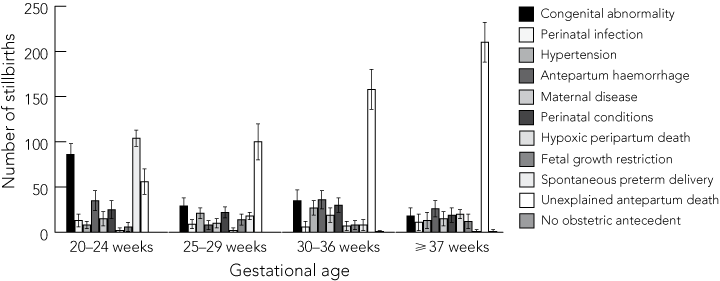
The most common causes of death differed by gestational age group, and are shown in Box 3. For extremely preterm stillbirths at 20–24 weeks’ gestation, the most common classification was spontaneous preterm delivery, whereas for stillbirths at 37 or more weeks’ gestation, unexplained antepartum death was the most common classification.
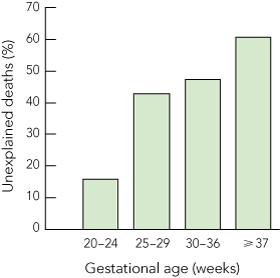
The proportion of stillbirths classified as unexplained antepartum death increased with increasing gestational age (Box 4). Stillbirths classified as unexplained antepartum death were significantly more likely to have had an autopsy performed (221/489 [45%] v 251/697 [36%]; χ2 = 10.1; df = 1; P = 0.001)].
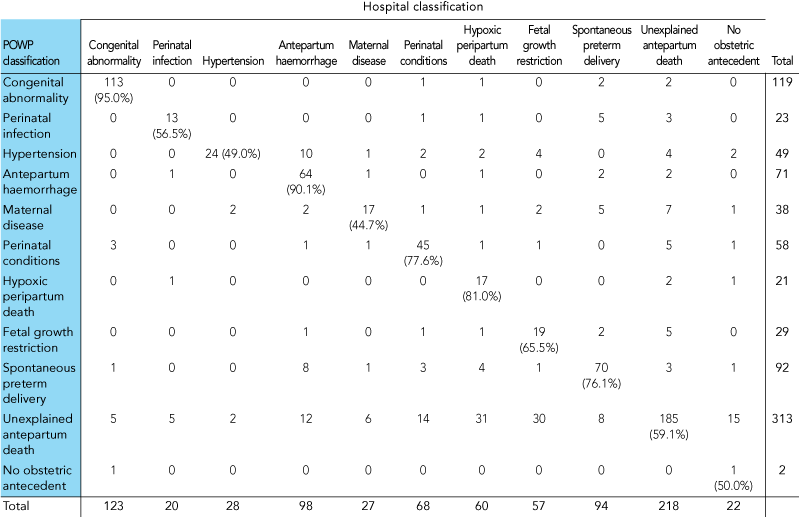
Agreement on classifications of causes of death between the POWP and hospital review committees is shown in Box 5. Agreement varied according to cause of death, with greater than 80% agreement for congenital abnormality, antepartum haemorrhage and hypoxic peripartum death. Stillbirths with these three causes of death were less likely to have had an autopsy performed (96/304 [31.6%] v 376/960 [39.2%]; P = 0.017) or placental abnormality (233/304 [76.6%] v 838/960 [87.3%]; P < 0.001).
In this large population-based study in NSW, unexplained antepartum death was the most common classification of stillbirths near term, and near-term stillborn infants were more likely to have had an autopsy. Although reported interobserver agreement for the PSANZ-PDC is high,6 we found that in practice it is relatively low between hospital perinatal mortality review committees and the POWP, particularly for unexplained stillbirths.
Our population-based cohort of stillbirths was one of the largest studied to date, evaluating 1264 stillbirths from 258 045 births, and a standardised classification system of cause of death was used. Having an expert committee centrally review all deaths and agree on cause of death: (i) means that by the time of review, important information that may change the classification, such as autopsy or placental results, will be available; and (ii) negates the use of official death certificates for cause of death, which may be unreliable. The PSANZ-PDC is used to classify both stillbirths and neonatal deaths, so causes of perinatal deaths overall are presented in national reports.2 It is important to report neonatal deaths and stillbirths separately as we have done in this study, as aetiologies may be quite distinct. Significantly, we assessed cause of death by gestational age group because causes of stillbirths differ depending on gestation period. We were able to assess stillbirth rates because of the linkage to the birth data from the MDC.
The percentage of unexplained stillbirths in our cohort was 41.5%. Previous literature on unexplained stillbirth has reported proportions of unexplained stillbirths from around 10% up to as high as 70%. The contribution of unexplained deaths varies considerably depending on the classification system used. Classification systems that have a particular focus, for example, on placental causes or growth restriction have low proportions of unexplained deaths.9,10 Older classification systems, which are widely used in both developed and developing countries (eg, the extended Wigglesworth or modified Aberdeen classifications11-13), have very high proportions of unexplained deaths. The PSANZ-PDC definition of unexplained antepartum deaths states: “deaths of normally formed fetuses before the onset of labour where no predisposing factors are considered likely to have caused the death”. This definition of unexplained death does not include autopsy findings and, coupled with the low autopsy rate in our cohort, means that many of these unexplained deaths were also unexplored.
The proportion of unexplained deaths has been shown to be lower in studies with an extensive test protocol and higher autopsy rates.14,15 Tests and autopsy findings lead to deaths that might have been classified as unexplained being classified in an explained category. In the datasets we used, unexplained deaths had more autopsies performed, suggesting that there was more of an attempt to investigate stillbirths with no apparent cause than those that were otherwise explained.
It is known (and is also clear from our data) that the principal causes of death differ by gestational age group.16 Despite this, standard investigation protocols usually request the full gamut of suggested tests for all stillbirths regardless of gestational age. The PSANZ Perinatal Mortality Audit Guidelines recommend a “non-selective” approach to investigation.5 From our data, it would appear that, for early stillbirths, investigations that focus on known or suspected causes of preterm birth (eg, infection) would be most important. Later stillbirths that are more likely to be unexplained require as full a set of investigations as possible, including an autopsy.
The interobserver agreement on the PSANZ-PDC between hospital committees and the POWP varied substantially, and is lower in our study than in previous reports.6 This may be because when interobserver reliability of the system was initially reported, all those using the system had a high degree of experience in perinatal mortality audit. National consensus to use the PSANZ-PDC at the PSANZ Congress in Adelaide in 2005 has not been followed by a widespread local hospital implementation program, and the poor interobserver agreement seen in our study may reflect that. However, it does provide useful information to guideline developers about which perinatal death classifications may require more explanation for classifiers, and could help determine educational strategies to help hospital perinatal audit groups use the system.
2 Causes of death for stillbirths reviewed by the Perinatal Outcomes Working Party according to the perinatal death classification of the Perinatal Society of Australia and New Zealand
3 Classification of causes of death by gestational age for 1264 stillbirths reviewed by the Perinatal Outcomes Working Party
Received 19 August 2007, accepted 17 December 2007
- Adrienne Gordon1
- Heather E Jeffery2
- 1 Newborn Care, Royal Prince Alfred Hospital.
- 2 University of Sydney, Sydney, NSW.
The authors are grateful to Lee Taylor and the Centre for Epidemiology and Research at the NSW Department of Health for record linkage and providing the MDC and perinatal death data. Adrienne Gordon was supported by a National Health and Medical Research Council public health scholarship.
None identified.
- 1. Australian Bureau of Statistics. Causes of death, Australia 2002. Canberra: ABS, 2003. (ABS Cat. No. 3303.0.) http://144.53.252.30/AUSSTATS/abs@.nsf/allprimarymainfeatures/6030D5CB60FAF6DDCA256FB10078C4D6?opendocument (accessed Apr 2008).
- 2. Laws PJ, Abeywardana S, Walker J, Sullivan EA. Australia’s mothers and babies 2005. Perinatal Statistics Series No. 20. Sydney: AIHW National Perinatal Statistics Unit, 2007. (AIHW Cat. No. PER 40.) http://www.aihw.gov.au/publications/per/amb05/amb05.pdf (accessed Apr 2008).
- 3. Centre for Epidemiology and Research. NSW Department of Health. New South Wales mothers and babies, 2005. NSW Public Health Bull 2007; 18 (S-1): 1-137. http://www.health.nsw.gov.au/pubs/2007/pdf/mdc05.pdf (accessed Apr 2008).
- 4. NSW Department of Health. Circular 2002/6. Hospital procedures for review and reporting of perinatal deaths. http://www.health.nsw.gov.au/policies/pd/2006/PD2006_006.html (accessed Apr 2008).
- 5. Perinatal Society of Australia and New Zealand. Perinatal Mortality Group. PSANZ Perinatal mortality audit guideline incorporating psychological and social aspects of perinatal bereavement. http://www.psanzpnmsig.org/guideline.html (accessed Apr 2008).
- 6. Chan A, King JF, Flenady V, et al. Classification of perinatal deaths: development of the Australian and New Zealand classifications. J Paediatr Child Health 2004: 40; 340-347.
- 7. Fleiss JG. Statistical methods for rates and proportions. New York: Wiley, 1981: 225–232.
- 8. Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics 1977; 33: 159-174.
- 9. Korteweg FJ, Gordijn SJ, Timmer A, et al. The Tulip classification of perinatal mortality: introduction and multidisciplinary inter-rater agreement. BJOG 2006; 113: 393-401.
- 10. Gardosi J, Kady SM, McGeown P, et al. Classification of stillbirth by relevant condition at death (ReCoDe): population based cohort study. BMJ 2005; 331: 1113-1117.
- 11. Wigglesworth JS. Monitoring perinatal mortality. A pathophysiological approach. Lancet 1980; 2: 684-686.
- 12. Cole SK, Hey EN, Thomson AM. Classifying perinatal death: an obstetric approach. Br J Obstet Gynaecol 1986; 93: 1204-1212.
- 13. Hey EN, Lloyd DJ, Wigglesworth JS. Classifying perinatal death: fetal and neonatal factors. Br J Obstet Gynaecol 1986; 93: 1213-1223.
- 14. Petersson K, Bremme K, Bottinga R, et al. Diagnostic evaluation of intrauterine fetal deaths in Stockholm 1998–1999. Acta Obstet Gynecol Scand 2002; 81: 284-292.
- 15. Pauli RM, Reiser CA Wisconsin Stillbirth Service Program: II. Analysis of diagnoses and diagnostic categories in first 1000 referrals. Am J Med Genet 1994; 50: 135-153.
- 16. Fretts RC, Boyd ME, Usher RH, Usher HA. The changing pattern of fetal death 1961–1988. Obstet Gynecol 1992; 79: 35-39.





Abstract
Objective: To describe the pattern of stillbirths by cause and gestation period in New South Wales since the introduction of the Perinatal Society of Australia and New Zealand perinatal death classification (PSANZ-PDC); and to assess the agreement between classifications on cause of death between local hospital committees and the Perinatal Outcomes Working Party (POWP — a subgroup of the NSW Department of Health Ministerial Maternal and Perinatal Committee).
Design, participants and setting: Population-based retrospective cohort study of all 258 045 births in NSW and all 1264 stillbirths classified by the POWP in 2002–2004, based on linked data on perinatal deaths from the NSW Midwives Data Collection and the NSW Ministerial Maternal and Perinatal Committee.
Main outcome measures: Pattern of stillbirths by cause and gestation period; and interobserver agreement on classification of cause of death (according to the PSANZ-PDC) between local hospital review committees and the POWP.
Results: The most common classification was unexplained antepartum death, comprising 41.5% of the cohort and 60% of stillbirths of ≥ 37 weeks’ gestation. These unexplained stillbirths were more likely to have had an autopsy performed than the explained stillbirths (45% v 36%; χ2 = 10.1; df = 1; P = 0.001). Agreement on cause of death differed by cause of death classification, with an overall κ statistic of 0.638.
Conclusion: Unexplained antepartum death is the most common classification of stillbirths near term, and these stillbirths are more likely to have had an autopsy. Although reported interobserver agreement is high for PSANZ-PDC, in practice it is relatively low between hospital mortality review committees and the POWP.