The United Kingdom’s National Institute for Clinical Excellence has recommended a structure for management of haematological malignancies, which includes guidelines for referral to secondary care of patients who have or may have these disorders.1 However, haematologists have a wide range of additional responsibilities, and guidelines for referral in these situations must be worked out locally. Improved access to laboratory investigations, combined with population ageing, means that many patients with minor laboratory abnormalities or early forms of low-grade or premalignant disease, such as chronic lymphocytic leukaemia or monoclonal gammopathy of uncertain significance, are now being identified. No treatment is necessary for many of these disorders and the number of patients far outstrips the available capacity for all to be seen by a haematologist.2
The South Island of New Zealand is about twice the size of Tasmania and has a population of one million. The haematology service in its principal city, Christchurch, provides all haematology services for 50% of this population, intensive treatments such as induction of acute leukaemia for an additional 20%, and haematopoietic stem cell transplantation for the entire population.3 The five specialist haematologists in the service participate in a roster that triages newly referred patients according to clinical need.
Other patients with written referrals from primary or secondary care were triaged as not needing to be seen in the hospital, and received prompt WA instead. For the purposes of this study, the actual waiting time between the first contact from the referring doctor and the patient’s first assessment or posting of WA was used to classify patients into three management groups: those seen within 28 days (early assessment); those seen beyond 28 days (delayed assessment); and those who were managed with WA. Diagnoses were grouped based on previously described categories.4
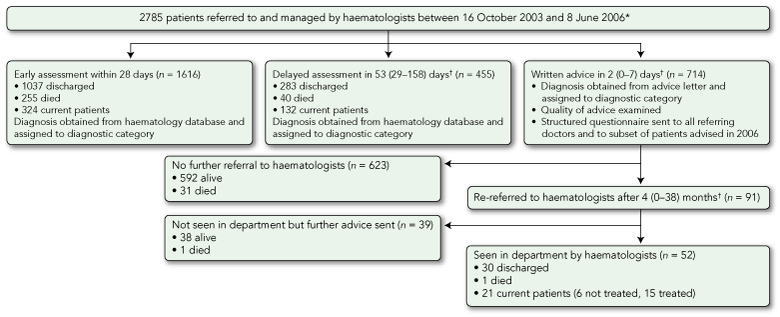
Patient outcomes are presented in Box 1. The median follow-up period of those patients still alive was 23 months (range, 8–40 months). Overall, 26% of referrals (714/2785) were managed with WA within a median time of 2 days (range, 0–7 days), while 16% (455/2785) received the alternative of delayed assessment. Patients managed with WA had been referred from both primary care (77%; 550/714) and secondary care (23%; 164/714). Most (87%; 618/714) resided within the district for which the department provides all levels of haematology services.
The diagnostic categories for patients in each management group are presented in Box 2. All patients referred with aggressive presentations, such as acute leukaemia, were managed with early assessment. The most frequent diagnostic category, “thrombosis-related” (34%; 949/2785), largely represented patients who had presented to hospital with venous thromboembolic disease and been discharged for early-stage anticoagulation therapy. Some patients (6%; 164/2785) who had early or delayed assessment were found to have no haematological diagnosis.
Seventy-two per cent of referring doctors (232/324) returned the questionnaire; their opinions are shown in Box 3. Of the responding doctors, 125 (54%) provided additional comments; two of these pointed out that the process of WA could make it more difficult to access specialist investigations rapidly for patients with non-specific haematological abnormalities. All other comments emphasised satisfaction with the process. Opinions of the 29% of patients recently managed with WA (32/112) who responded to the questionnaire are also presented in Box 3.
WA in response to selected referrals has previously been shown to be effective in the well defined circumstance of one specialist managing one condition (eg, lipid abnormalities5). Our findings support those of a review of a general haematology service in the UK, where general practitioners were satisfied with receiving WA from one of their specialists for selected referrals, with 121 of 274 patients referred over 14 months being managed in this manner.4
We extended this work to review the subsequent course of patients managed with WA and found that 7% were ultimately seen by a specialist after re-referral. The initial diagnosis occasionally required revision and, overall, 2% of all patients managed with WA went on to receive treatment. Deaths among patients managed with WA occurred less frequently than among patients who received early or delayed assessment (Box 1) and were not due primarily to haematological disease. From the limited information received from patients managed with WA, they shared their doctors’ satisfaction with the process.
To gauge whether our study had captured the majority of patients we expected to be referred, we estimated the incidence of chronic myeloid leukaemia in our region, on the assumption that all patients with this diagnosis for whom we provide all haematology services should be registered. The incidence of chronic myeloid leukaemia was 0.8, similar to the incidence of 1.1 in south-east England,6 suggesting our data do include all appropriate haematology referrals, at least for this condition.
The proportion of referrals managed with WA in this study (26%) is lower than that reported in the previous study (44%4), but that study only included patients referred for outpatient assessment and not those referred from within the hospital for management of acutely presenting haematological conditions or anticoagulant management. Reanalysis showed that we provided WA to 44% of patients referred for outpatient assessment in 2006 (data not shown). The proportion of patients managed with WA in each diagnostic category was similar to that found previously,4 however we used WA more frequently for the diagnoses of chronic lymphocytic leukaemia, lymphadenopathy and paraprotein.
Our process followed the ethical principle that doctors have a responsibility to provide the best standards of service possible within the limits of the resources available to them.7 There are no medicolegal reasons why a specialist should not consider other ways of dealing with referrals, when the alternative is to have the patient wait for delayed assessment or indefinitely. We found that WA shortened the time to management by many weeks compared with delayed assessment. Once the advice was offered, the duty of care returned to the referring doctor, and ongoing management was between the referring doctor and the patient. An invitation for re-referral was not explicitly offered in 60% of WA, and we have since changed our practice to automatically include this invitation. Our referring doctors demonstrated that they could safely follow up patients using the advice given, and we are not aware of any patients managed with WA who were not re-referred in a timely fashion when necessary.
2 Diagnostic categories of patients by management group
Patients managed with written advice and subsequently re-referred |
|||||||||||||||
Myelodysplastic/myeloproliferative diseases and related presentations* |
|||||||||||||||
3 Frequency of opinions of referring doctors and patients about the written advice process
Received 1 June 2007, accepted 13 September 2007
- Peter S Ganly1,2
- Helen Keeman2
- Ruth L Spearing1
- Mark P Smith1
- Nigel Patton1,3
- Eileen G Merriman1
- Steve S Gibbons1
- 1 Department of Haematology, Canterbury Health Laboratories and Christchurch Hospital, Christchurch, New Zealand.
- 2 University of Otago, Christchurch, New Zealand.
- 3 Division of Haematology, Institute of Medical and Veterinary Science, Adelaide, SA.
We acknowledge the helpful contributions of Dr Andrew Fairgray and Dr Paul O’Gorman, both general practitioners, to the design of this study. Ms Janine Keats and Ms Melanie Brown provided unstinting help with computerised databases, and Ms Karen Hawke in the Referrals Centre mailed and collated our referring doctor and patient questionnaires. Helen Keeman was supported by a Summer Studentship from the University of Otago while she contributed to collecting and analysing data.
None identified.
- 1. National Institute for Clinical Excellence. Guidance on cancer services. Improving outcomes in haematological cancers. The manual. London: NICE, Oct 2003. http://www.nice.org.uk/nicemedia/pdf/NICE_HAEMATOLOGICAL_CSG.pdf (accessed Nov 2007).
- 2. Smith AG, Bhavnani M. Haematology: sustainability, modernising, managing capacity and achieving cancer plan objectives. Bull R Coll Pathol 2006; 136: 44-46.
- 3. Guidelines on the provision of facilities for the care of adult patients with haematological malignancies (including leukaemia and lymphoma and severe bone marrow failure). British Committee for Standards in Haematology Clinical Haematology Task Force. Clin Lab Haematol 1995; 17: 3-10.
- 4. Tso A, Harris L, Littlewood T. Are written responses to some referrals to a general haematology clinic acceptable? BMJ 2004; 329: 946-947.
- 5. Stuart W, Smellie A. Do we need lipid clinics? Shifting the balance between secondary and primary care. Ann Clin Biochem 2005; 42: 463-467.
- 6. Phekoo KJ, Richards MA, Moller H, Schey SA; South Thames Haematology Specialist Committee. The incidence and outcome of myeloid malignancies in 2,112 adult patients in southeast England. Haematologica 2006; 91: 1400-1404.
- 7. St George IM. Ethical guidelines for doctors’ duties in an environment of competition or resource limitation. In: St George IM, editor. Cole’s medical practice in New Zealand. Wellington: Medical Council of New Zealand, 2001: 91.





Abstract
Objective: To measure the safety and acceptability of providing written advice (WA) for selected patients referred to a haematology service, as an alternative to inpatient or outpatient assessment.
Design, setting and participants: Review of the initial management and subsequent course of patients newly referred to a tertiary referral hospital in Christchurch, New Zealand, between 16 October 2003 and 8 June 2006. Structured questionnaires were sent to all referring doctors and patients recently managed with WA.
Main outcome measures: Numbers and diagnoses of patients managed with WA, early assessment or delayed assessment; re-referral and treatment details; characteristics of WA letters; and opinions of referring doctors and their patients on the WA process.
Results: 26% of new referrals (714/2785) were managed with prompt WA, while 16% (455/2785) received the alternative of delayed assessment. After a median follow-up of 23 months (range, 8–40 months), 13% of those managed with WA (91/714) were re-referred back to the same haematologists; 7% (52/714) were assessed in hospital and 2% (15/714) eventually required treatment. There were no deaths due to haematological causes. Over 90% of responding referring doctors said the WA process was rapid and effective, and 77% of recently managed patients were pleased to be treated by their own doctors.
Conclusions: Using WA to manage a substantial minority of patients referred to haematologists can be rapid and safe. It is widely accepted by referring doctors.