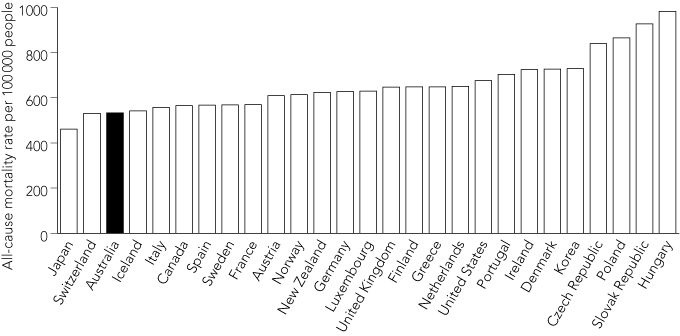
By the beginning of the 21st century, Australia had leapfrogged a group of developed countries — including Sweden, France, Italy, Iceland, Canada and Spain — to rival Switzerland for second ranking behind Japan on all-cause mortality rates (Box 1).1 Closely related to these are our rankings on total life expectancy and healthy life expectancy at birth,2 which are also among the best in the world.
Currently, Australia’s rate of reduction in death rates parallels Japan’s, and the gap in life expectancy between the two nations has also narrowed from a peak in the late 1980s.1 But our overall position is diminished somewhat by premature deaths from several potentially preventable conditions and by inequalities in their distribution. In contemporary health policy, performance in these respective areas is conceptualised as contributions to “goodness” (absolute measures of our total rates) and “fairness” (the relative distribution of health within populations).3 The interaction between the two is considerable — disadvantaged Australians die younger, principally from preventable causes. To show the impact of inequalities on our overall position, we have examined the potential gains from reducing those inequalities on the same basis as we have for the major causes of death.
In 1990, Armstrong4 introduced to broader population health research the notion of “Arcadian normals” — the lowest mortality rates being achieved in European and other developed countries whose people are of predominantly European background (the United States, Canada, Australia and New Zealand). He compared prevailing Australian rates with those in the best-performing country and deemed the excess to be the “proportion preventable in Australia”.
We indexed the difference in the age-standardised mortality rates between Australia and Japan to equal 100 points. We then calculated the number of points that could be gained by equalling the best-performing countries on a range of selected conditions. Rates in the “best-performing country” are not meant to imply finite limits. For example, while Australia’s death rate from accidental falls is the lowest in the world, current evidence suggests there is substantial scope for improvement,5 and the same probably applies in the leading country for each of the selected conditions. While these comparisons require appropriate caveats around the consistency of cause-of-death coding across OECD countries and the effect on subsequent death rates from other causes when fatal events are averted, this approach reveals many opportunities for improvement in Australia.
We also examined several known inequalities within Australia — between Indigenous and non-Indigenous people, males and females, and high and low socioeconomic groups — and expressed these using the same set of points. We ranked geographical areas and grouped them into quintiles (fifths of the population) according to the Australian Bureau of Statistics Index of Relative Socio-economic Disadvantage,6 and into deciles (tenths) according to all-cause mortality rates.
An update of Armstrong’s original comparisons is shown in Box 2, and an inequality dimension is added in Box 3. Both analyses use 100 points to compare the potentials for reducing or eliminating the gap between Australia and Japan. Circulatory conditions, diabetes, selected cancers and suicide provide the greatest potential for reduction in mortality. For most of the conditions selected, at least one other country is achieving a rate better than halfway between Australia and the world’s best.
Several aspects of inequality in mortality rates within Australia are shown in Box 3 and Box 4.
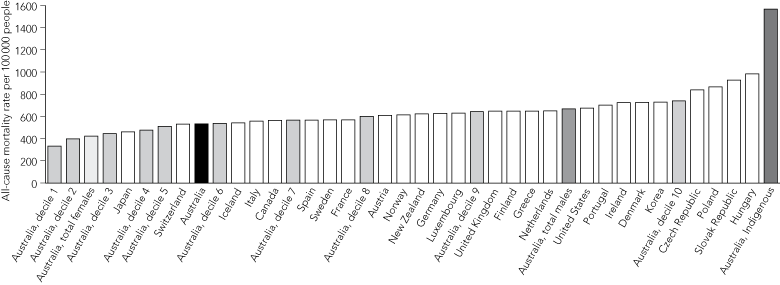
The potential for reducing excess death rates among Indigenous Australians is striking: studies using socioeconomic indexes demonstrate significant mortality gradients between our least and most disadvantaged areas (Box 3).
When the various geographical areas of Australia — in this case, aggregations of Statistical Local Areas into HealthWIZ Areas7 — are ranked by all-cause mortality rates, there is a twofold difference between the top and bottom deciles (Box 3, Box 4).
Reducing the male : female mortality ratio to Iceland’s level would reduce the overall gap with Japan by almost 40%. There appears to be more potential to reduce female than male mortality (Box 3).
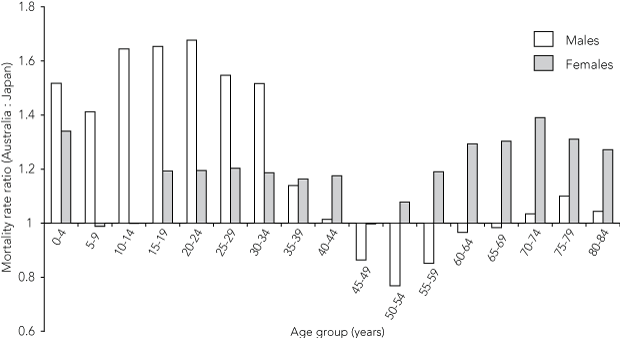
Age-specific comparisons with Japan (Box 5) show higher mortality rates for Australians at virtually every age, with the exception of men in their middle years.
Overall, Australia is already one of the healthiest countries in the world. If each Australian all-cause mortality decile was a hypothetical sovereign nation of about two million people, the first three “nations” would already be healthier than Japan (Box 4). Our first decile would be far and away the healthiest country in the world, while our tenth would fare a little worse than the United Kingdom and the United States, but better than the countries of eastern Europe (Box 4). Collapsing our top five and bottom five deciles into two halves, the top half would still be the healthiest country in the world (Box 3), while the bottom half would be better than two-thirds of the countries in the OECD. While aggregation into deciles masks vast differences in the experiences of individuals and groups within them, these groupings serve to illustrate how well Australia performs overall and the sound base on which we can build.
Nevertheless, there is considerable room for improvement if we want to match the world’s best. Mortality is 100% higher in male blue-collar workers in Australia, and 40% higher in female blue-collar workers, than in their white-collar counterparts,8 though manual/non-manual comparisons show a lesser degree of inequality.9 The gap of 5.2 years between males and females in life expectancy recorded in 2000–2002 has narrowed even further in recent years, and Australia ranks around the middle of developed countries on this indicator. Within the sexes, a persistent 4-year gap in life expectancy between males in the least and most disadvantaged areas and a corresponding 2-year gap in females can be demonstrated.10
There is evidence of recent modest gains in some aspects of Indigenous health,11,12 but there has been relatively little progress in reducing the overall gap between Indigenous and non-Indigenous populations in Australia.13 Although Indigenous Australians account for only about 2.5% of the population, they account for about a third of the total mortality gap between Australia and Japan. Elimination of the 17–18-year difference in life expectancy between Indigenous Australians and their non-Indigenous counterparts would add about 5 months to the total life expectancy of Australians. Massive inequalities persist — around birth, in childhood, in youth and young adulthood — culminating in a fivefold differential by middle age. Both absolute and relative disparities in life expectancy between Indigenous and non-Indigenous populations are larger in Australia than in New Zealand, Canada or the USA.14
Socioeconomic differences in mortality in Australia, particularly among men, are sizeable and have not received sufficient attention. Being male is now the single largest demographic risk factor for early mortality in developed countries,15 and it is clear that much of the widening differential between males and females in the 20th century and the recent narrowing of the sex differential is attributable to cigarette smoking.16 Inequalities between and within the sexes indicate a need for both broadly-based and sex-specific strategies.
Socioeconomic differentials in mortality between manual and non-manual workers in Australia are relatively low compared with other countries. In Australian men aged 20–59 years, the ratio of mortality in manual workers to mortality in non-manual workers was 1.34 in 1991–1995,9 whereas the lowest ratio reported in a European study of men aged 30–59 years in 1991–1995 was 1.46 in Denmark.17 The comparisons are not exact, but unlike most other measures listed in Box 3, we have not found other countries that have smaller socioeconomic differentials in mortality on this measure. Nonetheless, health inequalities in Australia are sizeable, increasing and invariably greatest for preventable conditions and in younger age groups,8 and the non-fatal consequences of these can reduce health trajectories throughout the life course.
These gains in health could be achieved through the application of current knowledge and systemic national effort to improve the societal factors that improve health and prevent “illth”. These measures would not only improve health — they could help contain or defer increasing health costs and enhance the sustainability of the Australian health system. It is interesting to note that Japan, the healthiest country in the world, is estimated to spend less per capita on health than Australia and has a lower annual growth rate in health expenditure, a larger proportion of health expenditure provided from public sources, a lower heart disease death rate, a much lower infant mortality rate, a lower consumption of alcohol and a lower level of obesity.1
1 All-cause mortality rates in selected OECD countries, 2000–2002
 |
|
OECD = Organisation for Economic Cooperation and Development. |
2 If Australia needed to achieve 100 points* to equal the lowest mortality rates in the world, where could they come from?† (specific causes of mortality, Australia v other OECD countries)
3 If Australia needed to achieve 100 points* to equal the lowest death rates in the world, where could they come from? (inequalities within Australia and compared with other OECD countries)†
- Ian T Ring1
- John F O’Brien2
- 1 Centre for Health Service Development, University of Wollongong, Wollongong, NSW.
- 2 Epidemiology Services Unit, Health Information Centre, Queensland Health, Brisbane, QLD.
None identified.
- 1. Organisation for Economic Cooperation and Development. OECD health data, 2004, 2005, 2006. http://www.oecd.org/els/health/data (accessed Sep 2007).
- 2. Mathers C, Murray C, Salomon J, et al. Healthy life expectancy: comparison of OECD countries in 2001. Aust N Z J Public Health 2003; 27: 5-11.
- 3. Broome J. Fairness, goodness and levelling down. In: Murray C, Salomon J, Mathers C, Lopez A, editors. Summary measures of population health: concepts, ethics, measurement and applications. Geneva: World Health Organization, 2002: 135-138.
- 4. Armstrong B. Morbidity and mortality in Australia: how much is preventable? In: McNeil JJ, King R, Jennings G, Powles J, editors. A textbook of preventive medicine. Melbourne: Edward Arnold,1990.
- 5. Tinetti M. Preventing falls in elderly persons. N Engl J Med 2003; 348: 42-49.
- 6. Australian Bureau of Statistics. Socio-Economic Indexes for Areas 2001. http://www.abs.gov.au/Websitedbs/D3110124.NSF/f5c7b8fb229cf017c a256973001fecec/d8f7e0b7b36c2023ca256de3 0081bea2!OpenDocument (accessed Sep 2007).
- 7. HealthWIZ: The national social health database. HealthWIZ statistical areas. Canberra: Prometheus Information, 2002.
- 8. Draper G, Turrell G, Oldenburg B. Health inequalities in Australia: mortality. Canberra: Queensland University of Technology and Australian Institute of Health and Welfare, 2004. (AIHW Cat. No. PHE 55.)
- 9. Australian Institute of Health and Welfare. Australian health inequalities 2: trends in male mortality by broad occupational group. Canberra: AIHW, 2005. (AIHW Cat. No. AUS 58.)
- 10. New South Wales Department of Health. Report of the New South Wales Chief Health Officer. Socioeconomic status. Life expectancy. Sydney: NSW Department of Health, 2006. http://www.health.nsw.gov.au/public-health/chorep/ses/ses_lomidhilex.htm (accessed Aug 2007).
- 11. Australian Institute of Health and Welfare; Australian Bureau of Statistics. The health and welfare of Australia’s Aboriginal and Torres Strait Islander peoples 2005. Canberra: AIHW and ABS, 2005. (AIHW Cat. No. IHW 14; ABS Cat. No. 4704.0.)
- 12. Thomas D, Condon J, Anderson I, et al. Long-term trends in Indigenous diseases in the Northern Territory: a foot on the brake, a foot on the accelerator. Med J Aust 2006; 185: 145-149. <MJA full text>
- 13. Wilson T, Condon J, Barnes T. Northern Territory Indigenous life expectancy improvements, 1967–2004. Aust N Z J Public Health 2007; 31: 184-188.
- 14. Bramley D, Hebert P, Jackson R, Chassin M. Indigenous disparities in disease-specific mortality, a cross country comparison: New Zealand, Australia, Canada and the United States. N Z Med J 2004; 117: U1215.
- 15. Kruger D, Nesse R. Sexual selection and the male : female mortality ratio. Evol Psychol 2004; 2: 66-85.
- 16. Pampel F. Cigarette use and the narrowing sex differential in mortality. Popul Dev Rev 2002; 28: 77-104.
- 17. Mackenbach J, Bos V, Andersen O, et al. Widening socioeconomic inequalities in mortality in six Western European countries. Int J Epidemiol 2003; 32: 830-837.





Abstract
Objective: To highlight recent reductions in mortality rates in Australia and identify conditions and population groups with the greatest potential for further reduction in mortality rates.
Design: International benchmarking and intranational comparisons of mortality rates were used to identify areas with the greatest potential for improvement.
Results: Latest data from Organisation for Economic Cooperation and Development (OECD) countries confirm that, while Japan’s death rates remain the lowest in the world, Australia’s are decreasing rapidly and we now rival Switzerland for second overall ranking. When the contributions of specific conditions are compared, the areas with the greatest potential for reductions are circulatory diseases (especially ischaemic heart disease); suicide; injury and violence; smoking-related conditions; and cancers amenable to prevention/early detection. Intranational comparisons show considerable scope for reduction in inequalities, especially those between Aboriginal and Torres Strait Islander peoples and other Australians, between males and females, and between low and high socioeconomic groups. These conditions and inequalities are highly interrelated, as differentials in health status are often mediated through broader societal inequalities.
Conclusions: Australia should aim to become the country with the lowest mortality rate in the world. This could realistically be achieved by benchmarking performance nationally and internationally, applying current knowledge and available interventions, matching policies with funding, and implementing systemic national programs and activities to promote health and prevent “illth”.