Diabetes is a common and increasingly prevalent chronic disease that currently affects at least one million adults in Australia.1 Structured care of patients with diabetes, often by multidisciplinary teams, is associated with improved health outcomes.2,3 Australian general practitioners play an important role, managing diabetes in 3.5 per 100 patient encounters.4 In 1999, the Australian Government introduced GP rebates for enhanced primary care (EPC) multidisciplinary care planning. The guidelines stated that care planning required collaboration between GPs, other providers and patients with chronic illnesses.5 Initial uptake of EPC care plans was slow.6 During this period, many GPs found care planning difficult to incorporate into their usual practice.7
In 2004, the Allied Health and Dental Care Initiative was introduced, allowing patients with a care plan to access Medicare rebates for five allied health or dental services a year. This led to a doubling in the number of claims for care plans.8 In 2005, GP management plans (GPMPs) and team care arrangements (TCAs) replaced EPC care plans. GPMPs are indicated for any patient with a chronic illness who would benefit from structured care. TCAs are intended for patients with complex care needs, require collaboration among providers, and allow patients to claim rebates for allied health and dental care. In financial year 2005–06, GPs prepared more than 645 000 GPMPs and almost 300 000 multidisciplinary care plans (EPCs and TCAs).8
Much of the existing research into care planning predates these more recent changes. It focused on GPs’ reaction to EPC care plans,7,9 practical difficulties associated with their use,7 and facilitators of uptake.10,11 Our previous record audit study found that diabetes care delivery improved in the year following a care plan. However, we were unable to prove that this was due to care planning.12 To measure whether care planning affects health care delivery or patient health outcomes, it is first necessary to understand more precisely how care plans are being used, and in particular how they affect usual care of people with chronic illness. Therefore, our aim in this study was to explore current care planning practices for people with diabetes, with a particular focus on the role of collaboration.
Our study was conducted using grounded theory methodology, which provides a means for understanding processes like care planning from the perspectives of the people who are involved in them.13 This methodology does not start with a preconceived model for how care plans should be used, nor does it seek to discover the extent to which current practice adheres to this model. Instead, the aim was to allow participants to describe care planning in their own terms.
Initial sampling was purposeful, aiming to include GPs, diabetes-related AHPs, endocrinologists, and patients with diabetes from a range of settings within NSW to provide different perspectives on the care planning process. Subsequent sampling was guided by theory development, and continued until saturation of the major concepts was achieved.13
Interviews were tape-recorded, fully transcribed and de-identified, then entered into NVivo version 2.0 qualitative software (QSR International, Melbourne, Vic) for analysis. Grounded theory methodology acknowledges that the researcher influences data collection and analysis.13 T S was responsible for data collection and coding. He met with both GP and non-GP members of the research team on several occasions to simultaneously code sections of interviews. These meetings broadened the perspective of the analysis by increasing sensitivity to concepts in the data. They were also used to refine the coding framework.14 Analysis was by constant comparison using a coding matrix.13
GP02: It certainly helps me in generating in one sitting my thought processes about the sort of care processes she [the patient] needs.
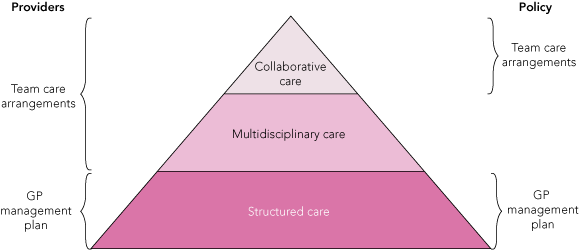
GPs rarely collaborated with other health care providers when preparing multidisciplinary care plans, and most providers did not believe that collaboration would improve care for the majority of their patients, including patients they identified as having complex needs. This suggests that a difference may exist between Australian policymakers’ and providers’ definitions of complex needs. For providers in this study, patients had complex needs and were eligible for TCAs because they required care from two or more additional providers. They felt that only a small proportion of these patients had problems so complex as to require collaboration beyond that which already occurs through referral and feedback letters. This clearly differs from the policy requirement that all TCAs involve active discussion between the GP and other providers at the time of their development (Box).15
Many GPs used care plans to provide patients with general education about the clinical goals and tasks of diabetes care, and referred patients to AHPs for more specific self-management support. Self-management is enhanced by collaborative goal-setting, which in turn relies upon an understanding of the patient’s needs and preferences.16,17 GPs could therefore assist AHPs by including more personalised patient information in their written care plans, such as potential barriers to achieving evidence-based targets.
Many patients with chronic illnesses benefit from multidisciplinary care.18 This study suggests that care planning plays an important role both in prompting and in facilitating referrals to AHPs. Policymakers should consider clarifying the eligibility criteria for TCAs to better reflect current practice (with its limited collaboration), bearing in mind that future restrictions on patients’ access to AHP rebates is likely to adversely affect GPs’ use of care planning and multidisciplinary care.
Future research into the effect of care planning needs to take note of the various purposes for which GPs use care plans, as these purposes affect the process and outcomes of care planning in different ways. Studies in other countries have begun to explore this issue; however, most research in this field has been done in the United States in managed care settings that do not translate easily to the Australian context.19,20 Australian studies are needed to help clarify which patients would most benefit from true collaboration in the provision of their multidisciplinary care.
- Timothy D Shortus1
- Suzanne H McKenzie1
- Lynn A Kemp2
- Judith G Proudfoot3,4
- Mark F Harris2
- 1 School of Public Health and Community Medicine, University of New South Wales, Sydney, NSW.
- 2 Centre for Primary Health Care and Equity, University of New South Wales, Sydney, NSW.
- 3 School of Psychiatry, University of New South Wales, Sydney, NSW.
- 4 Black Dog Institute, Sydney, NSW.
We thank all the health care providers and patients who gave their time to participate in this study; the staff of the Bankstown, Macarthur and Riverina Divisions of General Practice; and members of the reference group: Mr Cliff Newman (Consumer Advocate and Chair), Dr Philip Lye (GP), Mr Bradley Marney (Director, Macarthur Diabetes Service) and Dr Christine Walker (Chronic Illness Alliance). The study was funded by a UNSW Faculty Research Grant and Timothy Shortus was supported by a National Health and Medical Research Council Public Health Postgraduate Research Scholarship.
None identified.
- 1. Australian Institute of Health and Welfare. Diabetes: Australian facts 2002. Diabetes Series No. 3. Canberra: AIHW, 2002. (AIHW Cat. No. CVD 20.)
- 2. Renders CM, Valk GD, Griffin S, et al. Interventions to improve the management of diabetes mellitus in primary care, outpatient and community settings. Cochrane Database Syst Rev 2001; (1): CD001481.
- 3. Bodenheimer T, Wagner EH, Grumbach K. Improving primary care for patients with chronic illness: the chronic care model, part 2. JAMA 2002; 288: 1909-1914.
- 4. Britt H, Miller GC, Charles J, et al. General practice activity in Australia 2005–06. General Practice Series No. 19. Canberra: AIHW, 2007. (AIHW Cat. No. GEP19.)
- 5. Australian Government Department of Health and Aged Care. Primary care initiatives: Enhanced Primary Care package. Canberra: The Department, 1999.
- 6. Wilkinson D, McElroy H, Beilby J, et al. Uptake of health assessments, care plans and case conferences by general practitioners through the Enhanced Primary Care program between November 1999 and October 2001. Aust Health Rev 2002; 25: 1-11.
- 7. Blakeman T, Harris MF, Comino EJ, et al. Evaluating general practitioners’ views about the implementation of the EPC Medicare items. Med J Aust 2001; 175: 95-98.
- 8. Medicare Australia. Medicare Benefits Schedule item statistics reports. http://www.medicareaustralia.gov.au/statistics/dyn_mbs/forms/mbs_tab4.shtml (accessed Mar 2007).
- 9. Blakeman T, Zwar N, Harris M. Evaluating general practitioners’ views on the enhanced primary care items for care planning and case conferencing: a one year follow up. Aust Fam Physician 2002; 31: 582-585.
- 10. Coulson ML, Blakeman T, Shortus T, et al. Using a division based diabetes register to target patients for enhanced primary care care planning. Aust Fam Physician 2002; 31: 1064.
- 11. Shortus TD, Coulson ML, Blakeman TM, et al. An aged care liaison nurse can facilitate care planning using the Enhanced Primary Care items. Australas J Ageing 2005; 24: 67-68.
- 12. Zwar NA, Hermiz O, Comino EJ, et al. Do multidisciplinary care plans result in better care for patients with type 2 diabetes? Aust Fam Physician 2007; 36: 85-89.
- 13. Strauss AL, Corbin J. Basics of qualitative research: grounded theory procedures and techniques. Newbury Park: Sage Publications, 1990.
- 14. Barbour RS. Checklists for improving rigour in qualitative research: a case of the tail wagging the dog? BMJ 2001; 322: 1115-1117.
- 15. Medicare Australia. Medicare Benefits Schedule explanatory notes: EPC chronic disease management MBS items (items 721 to 731). http://www.health.gov.au/internet/wcms/publishing.nsf/Content/pcd-programs-epc-chronicdisease (accessed May 2007).
- 16. Glasgow RE, Davis CL, Funnell MM, et al. Implementing practical interventions to support chronic illness self-management. Jt Comm J Qual Saf 2003; 29: 563-574.
- 17. Von Korff M, Glasgow RE, Sharpe M. Organising care for chronic illness. BMJ 2002; 325: 92-94.
- 18. Wagner EH. The role of patient care teams in chronic disease management. BMJ 2000; 320: 569-572.
- 19. Bower P, Gilbody S, Richards D, et al. Collaborative care for depression in primary care. Making sense of a complex intervention: systematic review and meta-regression. Br J Psychiatry 2006; 189: 484-493.
- 20. Katon WJ, Von Korff M, Lin EHB, et al. The Pathways Study: a randomized trial of collaborative care in patients with diabetes and depression. Arch Gen Psychiatry 2004; 61: 1042-1049.





Abstract
Objective: To understand how multidisciplinary care plans are being used in the management of patients with diabetes, and to explore the role of collaboration in care planning.
Design: Grounded theory interview study.
Setting: Primary care, June 2005 to October 2006.
Participants: Thirty-eight people from three New South Wales Divisions of General Practice: 19 general practitioners, eight diabetes-related allied health providers, two endocrinologists, and nine adults with type 2 diabetes. Sampling was purposeful then theoretical.
Results: GPs use care plans to organise clinical care and help patients access allied health providers. Written plans are used to educate patients about their care and to motivate change. GPs rarely discuss care plans with other providers, and providers are unlikely to change their approach to patients on the basis of care plans. Patients do not expect to participate in care planning.
Conclusions: Care planning may increase evidence-based multidisciplinary care for patients with diabetes, but it rarely results in genuine collaboration between providers and patients. This suggests a difference may exist between Australian policymakers’ and providers’ definitions of patients with complex needs. Care plans could facilitate patient self-management by including more personalised information. Further research is needed to clarify which patients would benefit from a truly collaborative approach to their care.