Because follow-up data are usually unavailable for these patients, there is the potential for unrecognised poor outcomes from lack of treatment. Limited outcome data for DNW patients suggest that they do not have worse outcomes than other ED patients. However, most published studies report small numbers of patients and use retrospective questionnaire-type data collection methods based within one hospital population. There is considerable selection bias because of high rates of non-responders, and data may be missed if patients subsequently present to different hospitals. A study of 419 DNW patients reported that 61% were seen by a doctor within 7 days of the visit, and that only 1.7% were hospitalised.1 Another study found that 61% of DNW patients did not require any treatment after leaving.2 A recent study reported that 12.7% of DNW patients revisited EDs within 7 days of departure, and that 5% were admitted.3
EDIS and the Mortality Database records were linked by the Western Australian Data Linkage Unit by probabilistic matching. This linkage has been described previously.4 Data extraction and handling were performed with SPSS, version 12.0 (SPSS Inc, Chicago, Ill, USA). Univariate descriptive analyses were undertaken using Microsoft Excel (Microsoft, Redmond, Wash, USA), with χ2 testing for significant differences between proportions with the level of significance set at 0.05. Cumulative mortality rates at 2, 7, and 30 days were calculated with reference to the last ED presentation of each patient in the dataset.
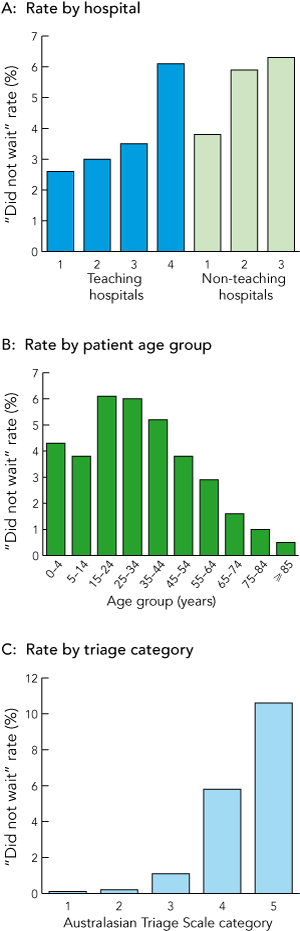
There were 24 988 patients accounting for 28 748 DNW presentations during the 3-year period. There were 368 442 patients who did wait for medical assessment, accounting for 673 025 ED visits; 447 043 (66.4%) of these presentations resulted in discharge after medical assessment. Overall, the DNW rate in metropolitan Perth was 4.1% of all presentations, ranging from 2.6% to 6.3% for the seven hospitals (Box 1A). With the exception of one tertiary hospital with a DNW rate of 6.1%, DNW rates were lower at inner-city tertiary referral hospitals than regional hospitals.
Demographic analysis (Box 1B) showed a higher than average DNW rate in the 15–44-years age group (5.8%; P < 0.001). Male patients were also more likely not to wait (4.4% v 3.8%; P < 0.001). Patients referred by other health care professionals were less likely not to wait (0.5%; P < 0.001). Patients arriving at EDs by private transport had a higher DNW rate (5.0%; P < 0.001), as did those arriving with police (5.8%; P < 0.001). Patients who arrived by ambulance had a lower DNW rate (1.4%; P < 0.001). Of note, two DNW patients had arrived with the Royal Flying Doctor Service, a rural air retrieval service.
Most DNW patients were in ATS categories 4 (67.1%) and 5 (23.4%). There was an inverse relationship between urgency of the need for treatment and DNW rate. The DNW rates in ATS categories 4 and 5 were 5.8% and 10.6%, respectively (P < 0.001; Box 1C). Only 156 patients did not have an ATS category recorded, of whom two did not wait.
Of all DNW patients, 22 964 (91.9%) did not wait on only one occasion (Box 2). The 1483 patients (5.9%) who did not wait on two occasions accounted for most of the remaining DNW patients. There was one patient who did not wait on 75 separate occasions during the 3-year period studied.
There is significant variability in DNW rates across hospitals and countries. Previously published rates for EDs in south-western Sydney are 4.9%,5 5.7%6 and 8.6%.3 International rates range from 0.8% to 8.2%,1,2,7-13 with an average of 4.0%. Higher DNW rates have been reported by major teaching hospitals6,13 and in public versus private hospitals.13 This raises concerns that patients with lesser means to find alternative health care are more likely not to wait.
Patients who did not wait for medical assessment in Perth EDs did so at lower rates than those reported in other major Australian studies from south-western Sydney. Three of the four tertiary teaching hospitals in our study had DNW rates of 3.5% or lower. One tertiary hospital had a rate of 6.1%. The reported New South Wales rates were more typical of the smaller Perth regional hospital EDs, which had DNW rates of 3.8%, 5.9% and 6.3%. This study is the first to report DNW rates that are lower in inner-city tertiary hospitals than in smaller metropolitan non-teaching hospitals. Our rate is also lower than the rate of 6.7% found in a small 4-month study at a single Victorian tertiary hospital ED.14
Characteristics of DNW patients previously identified in the published research include being a young male,5,6,11,12,14 not being married,2,9 having lower socioeconomic 5,6,9,15 and educational15 status, with English not the primary language,6 and not having private health insurance.6,15 Of particular note and interest within Australia are Aboriginals, who are 37% more likely not to wait than other Australians.6
One study found that 73.3% of DNW patients reported that they were suffering from a psychosocial stressor at the time of presentation,8 and another reported a propensity for alcohol–drug presentations and psychiatric presentations.15 The most consistent finding in the literature on DNW presentations was the presence of long waiting times,1,5-14,16 although there are methodological difficulties with reporting waiting times in this group of patients because the time the patient actually leaves is usually not recorded. There were other studies that reported an increase in the DNW rate during the night shift.6,14,17 Furthermore, research suggests that DNW patients present with problems of lower acuity,6,12,14,15 and have a shorter onset of presenting symptoms.2,11
- Jacqui Hall1
- George A Jelinek1,2
- 1 Sir Charles Gairdner Hospital, Perth, WA.
- 2 Discipline of Emergency Medicine, University of Western Australia, Perth, WA.
We acknowledge and appreciate the assistance of Nick Gibson in linking and extracting the data, and Associate Professor Peter Sprivulis, Dr Sandra Neate and Dr Tracey Weiland for comments on the manuscript. This study was presented at the Annual Scientific Meeting of the Australasian College for Emergency Medicine (South Australian Faculty) in May 2006.
None identified.
- 1. Dos Santos LM, Stewart G, Rosenberg NM. Pediatric emergency department walk-outs. Pediatr Emerg Care 1994; 10: 76-78.
- 2. Gibson G, Maiman LA, Chase AM. Walk-out patients in the hospital emergency department. JACEP 1978; 7: 47-50.
- 3. Mohsin M, Forero R, Ieraci S, et al. A population follow-up study of patients who left an emergency department without being seen by a medical officer. Emerg Med J 2007; 24: 175-179.
- 4. Sprivulis P, Da Silva J-A, Jacobs I, et al. ECHO: the Western Australian emergency care hospitalisation and Outcome linked data project. Aust N Z J Public Health 2006; 30: 123-127.
- 5. Mohsin M, Bauman A, Ieraci S. Is there equity in emergency medical care? Waiting times and walkouts in South Western Sydney hospital emergency departments. Aust Health Rev 1998; 21: 133-149.
- 6. Mohsin M, Young L, Ieraci S, Bauman AE. Factors associated with walkouts of patients from New South Wales hospital emergency departments, Australia. Emerg Med Australas 2005; 176: 434-442.
- 7. Arendt KW, Sadosty AT, Weaver AL, et al. The left-without-being-seen patients: what would keep them from leaving? Ann Emerg Med 2003; 42: 317-323.
- 8. Fernandes CM, Daya MR, Barry S, Palmer N. Emergency department patients who leave without being seen by a physician: the Toronto hospital experience. Ann Emerg Med 1994; 24: 1092-1096.
- 9. Weissberg MP, Heitner M, Lowenstein SR, Keefer G. Patients who leave without being seen. Ann Emerg Med 1986; 15: 813-817.
- 10. Goldman RD, Macpherson A, Schuh S, et al. Patients who leave the paediatric emergency department without being seen: a case–control study. CMAJ 2005; 172: 39-43.
- 11. Khanna R, Chaudry MA, Prescott M. Emergency department patients who leave the department without being seen by a doctor. Eur J Emerg Med 1999; 6: 233-235.
- 12. Goodacre S, Webster A. Who waits longest in the emergency department and who leaves without being seen? Emerg Med J 2005; 22: 93-96.
- 13. Stock LM, Bradley GE, Lewis RJ, et al. Patients who leave emergency departments without being seen by a physician: magnitude of the problem in Los Angeles County. Ann Emerg Med 1994; 23: 294-298.
- 14. Lee G, Endacott R, Flett K, Bushnell R. Characteristics of patients who did not wait for treatment in an emergency department: a follow-up study. Accid Emerg Nurs 2006; 14: 56-62.
- 15. Wartman SA, Taggart MP, Palm E. Emergency room leavers: a demographic and interview profile. J Community Health 1984; 9: 261-268.
- 16. McNamara KJ. Patients leaving the ED without being seen by a physician: is same-day follow-up indicated? Am J Emerg Med 1995; 13: 136-141.
- 17. Bindman AB, Grumbach K, Keane D, et al. Consequences of queuing for care at a public hospital emergency department. JAMA 1991; 266: 1091-1096.





Abstract
Objective: To determine characteristics and outcomes of patients who did not wait to see a doctor in emergency departments (EDs).
Design and setting: Population-based outcome study using probabilistically linked ED and Western Australian death records, with ED records from all seven Perth public hospitals that have EDs from 1 July 2000 to 30 June 2003.
Main outcome measures: Rates of “did not wait” (DNW) presentations, overall and for individual hospitals; characteristics of DNW patients; mortality rates among DNW patients at 2, 7 and 30 days.
Results: DNW rates varied from 2.6% to 6.3% (average, 4.1%) and were generally lower in tertiary teaching hospitals. DNW patients had conditions of lower urgency, predominantly Australasian Triage Scale category 4 (67.1%) and 5 (23.4%). The DNW rates in these categories were 5.8% and 10.6%, respectively (P < 0.001). Patients referred by health care providers had lower DNW rates (0.5%; P < 0.001). DNW patients were more frequently male (4.4% v 3.8%; P < 0.001), and young to middle-aged adults (15–44 years; 5.8%; P < 0.001). Patients with a higher than average DNW rate were more likely to arrive by private transport (5.0%; P < 0.001) or with police (5.8%; P < 0.001), re-present for review (8.6%; P < 0.001) or have social or behavioural problems (7.7%; P < 0.001). Most patients (91.9%) did not wait on only one occasion. The 30-day mortality rate among DNW patients was significantly lower than for patients seen by a doctor and discharged (0.14 v 0.20%; P = 0.026), and for all patients seen in the ED (1.28%; P < 0.001).
Conclusions: Patients who did not wait for medical assessment in Perth EDs had conditions of lower acuity and had lower mortality rates than those who waited for assessment.