In its 1998 report on the Australian obstetrics and gynaecology workforce, the Australian Medical Workforce Advisory Committee (AMWAC) concluded that the workforce was in balance, assuming a growth in demand of only 0.4%. It recommended an increase in the number of trainees from 54 to 58 per year, representing an increase from 12 to 14 for Victoria.1 More recent reports give a more sombre assessment.2-4
The AMWAC report in 2004 expressed mild alarm.5 It found evidence of an increase in the proportion of specialists who had ceased obstetrics to focus exclusively on gynaecology. Further, it noted increased participation by women in the obstetric workforce, with reduced hours worked by both men and women. The proportion of female trainees stood at 61%. The number of all trainees entering the specialty was below that recommended by AMWAC because of a lack of suitable applicants and training positions. The report’s final recommendations are noteworthy. One was to increase the number of training places to between 66 and 78, which by AMWAC’s own admission seemed unachievable. Another was to consider “alternative models of care”, a strategy that is unlikely to resolve rural issues, where consultant support is more difficult to maintain. The final major recommendation was for “collaboration to develop alternative training pathways for obstetrics” — including expanding the role of GPs, which perhaps ignores the lack of current workforce capacity within rural or urban general practice to meet any shortfall in obstetric services.
In providing comprehensive health care for families, GPs may be involved in all levels of obstetric care, from before conception to postnatal care. Up to the late 1990s, large numbers of GPs were involved in intrapartum care across all geographical areas.6 In the past decade, significant changes have affected the GP obstetric workforce, including rising indemnity costs and high-profile medicolegal obstetrics cases.7 In areas where there are few consultant specialists, GPs play a larger role.
If the Australia-wide predictions of a 2002 report in this Journal are applied to the Victorian situation, the future of consultant obstetrics is not sound.2 This article reported that, of the 72% of Fellows then practising obstetrics, 66% intended to be doing so after 1 year, 44% after 5 years, and only 24% after 10 years. The projected decreases were “for both public and private practice and across all age groups, although the proportion intending to cease practising was higher among older respondents”. This article was written at the height of the indemnity “crisis”. A 2003 article confirmed that the projected participation rate in obstetrics of 66% was correct, and that specialists were following their intentions.4
Postal surveys were sent to all 961 Diplomates and 317 Fellows listed on the Vic-torian database in September 2003. A modified Dillman protocol was implemented.8 We determined locality information for the towns in which respondents worked using an Internet-based community information database, Echidna: health service profiles for Victorian rural regions.9
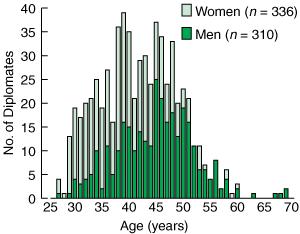
Diplomates constituted 15% of the calculated full-time-equivalent GPs in Victoria (Ms Luisa Abiuso, Senior Policy Officer, Workforce Policy Service and Workforce Planning, Department of Human Services, Victoria, personal communication). Diplomates comprised 52% women and 48% men. Compared with the overall sex distribution of Victorian GPs, Diploma training is more likely to attract women (odds ratio [OR], 2.0; 95% CI, 1.1–3.5).10 The age distribution of Diplomates was not uniform (z = 2.04; P < 0.000). Their median age was 42 years (Box 1), and Diplomates aged under 45 years were more likely to be female (OR, 4.2; 95% CI, 2.9–5.9).
Based on the Rural, Remote and Metropolitan Areas (RRMA) classification,11 GP obstetricians constituted between 11.7% and 23.0% of the GP population in each RRMA region. The percentage of Diplomates in the workforce increased with degree of rurality. GP Diplomates in rural areas (RRMA 4–7) were more likely to be male (OR, 3.2; 95% CI, 2.3–4.5) and aged over 45 years (OR, 1.51; 95% CI, 1.05–2.16).
GP obstetricians: Of the Victorian Diplomate respondents, 20% (129) were involved in obstetric practice, 49% had been involved in managing women in labour in the past, but were not currently practising, and the remaining 31% had never managed women in labour. Of the 129 Diplomates who were practising procedural obstetrics, 21.7% (28) lived in metropolitan Melbourne; 57% of these were aged over 45 years. Most procedural obstetric practitioners in rural areas were in towns classified as RRMA 4 and 5 (Box 2). For rural Diplomates (RRMA 4–7), there was no statistical difference between the age distributions of all rural Diplomates and the subgroup of procedural rural Diplomates (z = 1.48; P = 0.14).
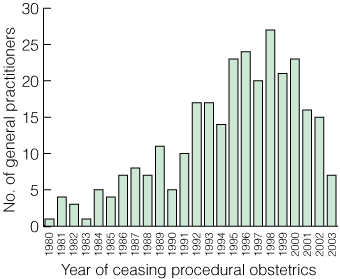
Sustainability of GP obstetrics workforce: Diplomates retired from practice with increasing frequency over the 1990s. During the years 1996 to 1998, the number retiring from obstetric practice exceeded the number of new Diplomates. The number retiring yearly fell from the year 2000 (Box 3). Doctors of all age groups retired from practice. Women doctors who completed the Diploma tended to retire from procedural practice earlier than men; 58% retired in less than 2 years, and 90% in less than 7 years.
The geographical distribution of Diplomates who had retired from procedural practice showed the greatest loss in urban areas (RRMA 1–3), with less loss in rural areas (RRMA 4–7). Numerically, the largest loss of GP obstetricians occurred in Melbourne; of the total 310 Diplomates who retired, 206 were from Melbourne (Box 4).
Of the GPs practising procedural obstetrics, 56% intended to cease within 7 years. This loss of workforce is likely to occur in all geographical areas except in RRMA 7, “other remote areas” (Box 5).
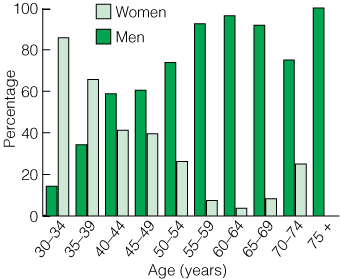
Sixty-nine per cent of Victorian Fellows (168) were male. Box 6 shows the distribution of Victorian specialists by age and sex. The proportion of the female workforce decreased with increasing age. Among Fellows aged under 40 years, the workforce was predominantly female in each age cohort.
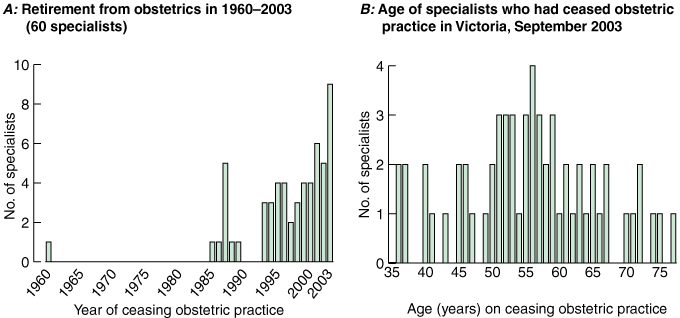
Responses from Fellows showed that 66.7% (162) were currently practising obstetrics, 24.7% (60) had ceased practising obstetrics, and 8.6% (21) had never practised obstetrics. Of the 162 who were currently practising obstetrics, 23.5% (38) were in private practice, 28.4% (46) worked in public obstetrics, and 48.1% (78) worked in both private and public obstetrics. There were 38 specialists (32 men and six women) practising outside the Melbourne metropolitan area; this represented less than 16% of the overall specialist obstetric workforce in Victoria. Of the 60 specialists who had ceased to practise obstetrics, 46.7% (28) did so after 2000 (Box 7A). The age of specialists leaving obstetrics is shown in Box 7B.
Respondents were asked four questions:
Please describe what you enjoy about managing women in labour and attracts you to this type of work;
Please describe the barriers and problems (both clinical and non-clinical) that make managing women in labour difficult;
What steps could be taken to help you resume or commence managing women in labour?; and
What steps could be taken to recruit doctors to manage women in labour (both new graduates and existing doctors)?
Our findings support the prediction that there will “soon be a shortage of experienced practising obstetricians in Australia”.2 Retiring specialists are mainly in older age groups, but specialists of all ages have ceased obstetric practice. Compared with an earlier study that found 8.6% of specialists had never practised obstetrics,12 we found that 33.3% of Victorian specialists had never practised obstetrics, an increase of 24%. There was a high proportion of women within the obstetric workforce, but AMWAC has described how career interruptions for family reasons have the potential to reduce female participation to 74% of that of male obstetricians.13 Thus, a pattern is emerging of increasing retirement from obstetric practice, falling intention to practise obstetrics, and a decrease in the overall obstetric work output because of family commitments.
Obstetrics and gynaecology is witnessing an increase in the proportion of women participating in the specialty. Between 2000 and 2003, the specialty has seen the percentage of women increase from 18.8% to 23.5%, while the overall percentage of women in the specialist workforce only increased from 18.0% to 19.7%.14 Of those in training for specialist obstetrics and gynaecology, 62.5% were women.4
The AMWAC survey of female participation in the medical workforce, published in 1996, was devoted specifically to the potential impact of demographic changes.13 With 50% of graduates being women, the report predicted that the preference of women for urban general practice would accelerate the uneven distribution of GPs. This prediction may also be valid for specialist obstetricians. The underlying assumption is that female practitioners are unlikely to enter rural practice where the time and on-call demands of an obstetric practice may not be compatible with family and childcare responsibilities.
In 1996, there were 52 provincial Fellows; we found that number had decreased to 38 in 2003. The 2000 RANZCOG/National Association of Specialist Obstetricians and Gynaecologists workforce study reported its findings on 226 provincial specialists in Australia and New Zealand.3 It determined that 32% of specialists had left provincial practice after 5 years or less, and 40% of specialists still in provincial practice saw 5 years as the maximum they were prepared to work outside a major city.
Current policy considers that the emerging workforce will be adequate to provide obstetric services. We believe this policy needs to be revised urgently. There can be no doubt that the substantial reduction in the number of Australian medical graduates since the early 1990s has had a profound impact on the medical workforce of today. While the numbers of Australian graduates are now being increased, it will take at least another decade for the impact to be felt. Factors such as the larger proportion of women in medical schools (who may interrupt their careers to care for family), the move to part-time work by both men and women in medical practice,15 and the loss of doctors aged under 40 years in rural areas and from the medical workforce overall,16,17 have a net result of reducing the number of full-time-equivalent doctors.
The recruitment of overseas-trained specialists has not had a significant impact on rural practice. Indeed, our data suggest that most overseas-trained doctors practise in Melbourne. Staff specialist positions protect doctors from the requirement to work in an “Area of Need”. Overseas-trained doctors are subject to Medicare provider number restrictions under sections 19AA and 19AB of the Health Insurance Act 1973 (Cwlth).18 To deliver a service that receives a Medicare rebate, doctors can apply for an exemption to work in an Area of Need, often in a rural location. Hospital appointments lie outside these legislative restrictions. Overseas-trained doctors also represent a small percentage of the overall Diplomate workforce and are unlikely to make a significant contribution to the workforce shortage in obstetrics.
1 Age and sex distribution of 646 Diplomates of the Royal Australian and New Zealand College of Obstetricians and Gynaecologists in Victoria, September 2003
2 General practitioner obstetricians, Diplomates and full-time-equivalent GPs by Rural, Remote and Metropolitan Area classification11 in Victoria, September 2003
Rural, Remote and Metropolitan Area classification |
|||||||||||||||
4 Involvement of general practitioner Diplomates in obstetric practice by Rural, Remote and Metropolitan Area classification11 in Victoria, September 2003
Rural, Remote and Metropolitan Area classification |
|||||||||||||||
Received 17 April 2006, accepted 29 August 2006
- Cameron S Loy1
- R Bruce Warton2
- James A Dunbar3
- Greater Green Triangle University Department of Rural Health, Flinders and Deakin Universities, Warrnambool, VIC.
We acknowledge funding provided by the Department of Human Services Victoria, Workforce Policy Service and Workforce Planning Division, and assistance from the Royal Australian and New Zealand College of Obstetricians and Gynaecologists for access to their database. We thank Dr Rodney Carr, designer of XLStatistics, Deakin University, Warrnambool, and the members of the steering committee, the Royal Australian College of General Practitioners, RANZCOG, General Practice Registrars Australia and the Department of Human Services, Victoria.
None identified.
- 1. Australian Medical Workforce Advisory Committee. The obstetrics and gynaecology workforce in Australia. AMWAC report 1998.6. Sydney: AMWAC, 1998.
- 2. MacLennan AH, Spencer MK. Projections of Australian obstetricians ceasing practice and the reasons. Med J Aust 2002; 176: 425-428. <MJA full text>
- 3. The Royal Australian and New Zealand College of Obstetricians and Gynaecologists/National Association of Specialist Obstetricians and Gynaecologists Workforce Working Group. RANZCOG/NASOG Workforce 2000 survey. O&G 2001; 3: 11-25. http://www.ranzcog.edu.au/publications/o-g_pdfs/OG-2000-2003/OG-March-2001.pdf (accessed Aug 2006).
- 4. Bell R. The 2003 RANZCOG workforce survey. O&G 2003; 5: 174-178. http://www.ranzcog.edu.au/publications/o-g_pdfs/OG-2000-2003/OG-Sept-2003.pdf (accessed Aug 2006).
- 5. Australian Medical Workforce Advisory Committee. The specialist obstetrics and gynaecology workforce — an update 2003–2013. AMWAC Report 2004.2. Sydney: AMWAC, 2004.
- 6. Gunn J, Lumley J, Young D. Involvement of Victorian general practitioners in obstetric and postnatal care. Aust Fam Physician 1998; 27 Suppl 2: S78-S83.
- 7. Watts RW, Marley JE, Beilby JJ, et al. Training, skills and approach to high-risk obstetrics in rural GP obstetricians. Aust N Z J Obstet Gynaecol 1997; 37: 424-426.
- 8. Dillman D. Mail and internet surveys: the tailored design method. 2nd ed. New York: John Wiley & Sons, 2000.
- 9. Monash University. Medicine, Nursing and Health Sciences. Echidna: health service profiles for Victorian rural regions. http://www.med.monash.edu.au/srh/resources/echidna/ (accessed Nov 2006).
- 10. Australian Institute of Health and Welfare. Medical labour force 2001. National health labour force series No. 28. Canberra: AIHW, 2003. (AIHW Catalogue No. 28.)
- 11. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remoteness classifications. Canberra: AIHW, 2004. (AIHW Catalogue No. PHE 53.) http://www.aihw.gov.au/publications/index.cfm/title/9993 (accessed Sep 2006).
- 12. Practice intentions of new Fellows and trainees. O&G 2001: 2: 140-142. http://www.ranzcog.edu.au/publications/o-g_pdfs/OG-2000-2003/OG-June-2001.pdf (accessed August 2006).
- 13. Australian Medical Workforce Advisory Committee/Australian Institute of Health and Welfare. Female participation in the Australian Medical Workforce. AMWAC Report 1996.7. Sydney: AMWAC/AIHW, 1996.
- 14. Australian Institute of Health and Welfare. Medical labour force 2003. National health labour force series No. 32. Canberra: AIHW 2005. (AIHW Catalogue No. HWL 32.)
- 15. The Royal Australian and New Zealand College of Obstetricians and Gynaecologists. 2005 annual report. Melbourne: RANZCOG, 2005. http://www.ranzcog.edu.au/about/pdfs/annualreport2005.pdf (accessed Aug 2006).
- 16. Australian Medical Workforce Advisory Committee/Australian Institute of Health and Welfare. The characteristics of students entering Australian medical schools 1989–1997. AMWAC report 1997.7. Sydney: AMWAC/AIHW, 1997.
- 17. Conn W. Medical workforce participation: males and females 1981, 1986 and 1991. Canberra: Australian Institute of Health and Welfare, 1995.
- 18. Health Insurance Act 1973 (Cwlth). http://www.austlii.edu.au/au/legis/cth/consol_act/hia1973164/ (accessed Aug 2006).





Abstract
Objective: To provide a contemporary picture of the general practitioner and specialist obstetric workforce in Victoria.
Design, participants and setting: Postal census by questionnaire of all 317 Fellows and 961 Diplomates on the Victorian database of the Royal Australian and New Zealand College of Obstetricians and Gynaecologists in September 2003.
Main outcome measures: Sex, age and geographical distributions and patterns of retirement from and recruitment to the GP and specialist obstetric workforce in Victoria.
Results: 244 Fellows (77.0%) and 652 Diplomates (67.8%) participated. The average age of Diplomates was 42 years; only 20% were involved in procedural obstetrics. Of GPs practising procedural obstetrics, 56% intended to cease within 7 years. Two-thirds of specialist obstetricians continued to practise obstetrics. Among those ceasing obstetrics, almost half had done so since 2000. Among Fellows ceasing obstetric practice, there is a peak in the 50–60-years age group, but cessation of obstetric practice occurred across all age groups.
Conclusion: The proportion of GPs involved in procedural obstetrics has fallen markedly over the past decade, with half of those ceasing practice in the 40–50-years age group. New GPs entering the workforce with the Diploma and overseas doctors are unlikely to meet the procedural workforce shortfall. Attracting the large cohort of doctors aged 40–50 years back to obstetric practice must be a priority. Given the pattern of retirements from obstetrics, there will be insufficient numbers of specialists to maintain current levels of service. The reasons include non-participation in obstetrics by new graduates and international medical graduates, the inadequate number of new graduates, and the predominance of women among specialists aged under 40 years, whose work output tends to be affected by family commitments.