In 2001, the President of the Royal Australian and New Zealand College of Obstetricians and Gynaecologists estimated that 30% of specialist obstetricians did not practise obstetrics.1 To date, the cessation of obstetric practice has been particularly high among general practitioners and rural specialists — in a survey conducted in 2000, 34 of 200 rural Australian specialist obstetricians had recently left rural practice and 46 of the remaining obstetricians planned to move on within five years.2 Furthermore, in a 2001 survey, 24% of 109 new Fellows and Members in their final two years of training stated that they did not intend to perform any obstetric work.3 The main reasons cited for choosing to avoid obstetric practice were the cost of medical indemnity (25%) and fear of litigation (20%).
An impending crisis in obstetrics owing to a shortage of practitioners has been foreshadowed for many years.4 Many factors may contribute to the decline in the number of practitioners, including long and unsociable hours, disruption to family life and lack of adequate backup by other practitioners.3
More recently, the rapidly escalating cost of medical indemnity insurance has become a major precipitating factor. In 1980, indemnity to practise specialist obstetrics and gynaecology could be obtained for $100. In 2001, the base rate for indemnity offered by Australia's largest indemnity provider, United Medical Protection, ranged from $20 970 in the Northern Territory to $54 315 in New South Wales (Richard Wilson, Senior Medical Advisor, United Medical Protection, personal communication).
There is a lack of current data about how Australian obstetricians are coping with their current working conditions. We report here the outcomes of a survey of Australian Fellows of the Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG) to determine their reasons for ceasing obstetric practice. As information on litigation and its outcomes is not readily available, we also sought details of specialists' personal experience in this area.
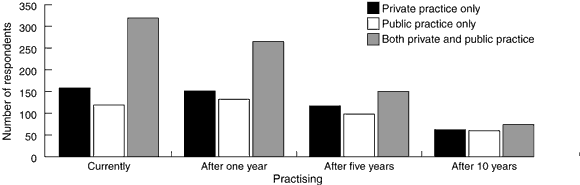
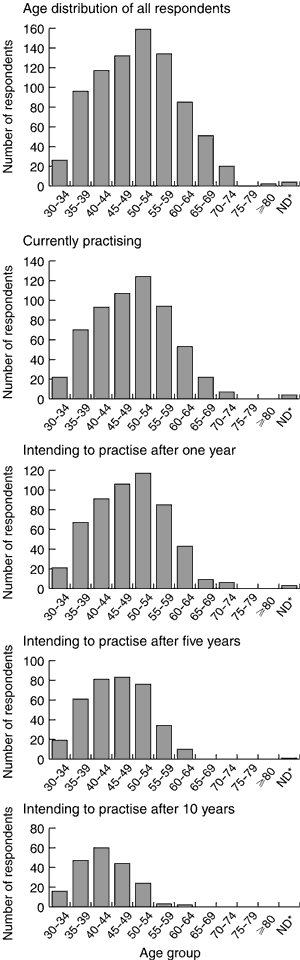
The reported intentions of the respondents suggest that the number practising obstetrics will fall over the next 10 years for both public and private practice (Box 1) and across all age groups, although the proportion intending to cease practising was higher among older respondents (Box 2).
Of the 388 respondents who had already ceased public practice, the median time since ceasing was six years; of the 349 respondents who had already ceased private practice, the median time since ceasing was five years. The reasons given for ceasing public and private practice were, respectively, to specialise in gynaecology (34% and 38%), fear or trauma of litigation (25% and 39%), indemnity insurance cost (20% and 41%), practice cost (10% and 27%), disruption to family (37% and 21%), and long and late hours (37% and 40%) (more than one reason could be given by each respondent).
In Australia, in the 12-month period prior to our survey, the median annual insurance premium for those practising obstetrics was $35 515 (taking into account any extra call made by the insurance or indemnity organisation), and varied according to the State or Territory in which they practised (Box 3). Of the 432 respondents who had a public practice, 143 paid their own insurance, 58 were partially subsidised and 231 did not pay for insurance. Of the 477 respondents who had a private practice, 449 paid their own insurance, 14 were partially subsidised and 14 did not pay for insurance.
Sixty eight per cent (557/818) of obstetricians were aware of the possibility of litigation against them at some point in their obstetric careers.
Among the 32% (262/815) of respondents who had at some time received documents from a court formally initiating an obstetric claim, there were 401 claims reported (Box 4). The full outcomes were not provided for all claims reported, as some are ongoing.
After receipt of documents formally commencing a court action against them, 46% of respondents had experienced depression and 3% had considered suicide, and 37% stated that it interfered with their work. Seventy-seven per cent of respondents currently practising obstetrics indicated that the present state of litigation encourages higher rates of caesarean section. Forty-five per cent of respondents would like a no-fault publicly funded scheme introduced to compensate patients for any adverse medical event or condition; a further 17% would approve of a such scheme if limited to obstetric events only. Others would prefer a scheme limited to children with a disability from birth (18%), children with a severe neurological disorder (8%), or children on a cerebral palsy register (4%), and 4% are opposed to introducing any no-fault compensation scheme.
The results show an aging obstetric workforce. Nineteen per cent of respondents were women, corresponding with a 19% female Fellowship of the RANZCOG in 2001 (source: RANZCOG database). However, 55% of trainees in 2001 were women (source: RANZCOG database) and their equivalent full-time contribution to the future workforce is likely to be less than that of male trainees.
In the years 2000 and 2001, 46 and 49 trainees, respectively, finished their training in obstetrics and gynaecology (source: RANZCOG database). However, given that 24% of all trainees newly elevated to Fellowship say that they do not intend to practise obstetrics at all,3 this leaves about 35 trainees per year intending to practise obstetrics. If this continues, there will be a shortfall in the number of practitioners available to replace those planning to retire over the next 10 years. If the respondents' predictions of the timing of their withdrawal from obstetrics are correct, then a retirement rate from obstetrics of about 50–60 practitioners per year can be expected over the next 10 years. There is likely to be regional variation, with higher retirement rates in New South Wales, where indemnity costs are highest.
Rates of retirement from obstetrics may rise even further if an increasing workload falls to those still practising obstetrics and if indemnity premiums continue to rise. The private sector may lose practitioners more quickly than the parts of the public sector in which the employer pays for indemnity insurance. However, our survey showed that about 44% of currently practising specialist obstetricians in both sectors proposed to cease practice within five years.
Most obstetricians are self-employed, work in private practice and must pay their own indemnity premiums, but indemnity costs are not uniform. Staff specialists employed by the State health departments generally have their indemnity premiums paid for both public and private patients (Richard Wilson, Senior Medical Advisor, United Medical Protection, personal communication), but clinical academics employed by universities often have to pay their own indemnity costs to conduct private practice. Premiums also vary from State to State. Much higher premiums have been foreshadowed for 2002–03. The base rate in New South Wales will be $97 412 in addition to a call (Richard Wilson, Senior Medical Advisor, United Medical Protection, personal communication).
With such high indemnity premiums and low Medicare schedule fees, the economic difficulties of running a private practice become great. These are especially onerous when commencing practice, taking leave, or reducing workload in later years.
Of great concern is the number of obstetricians who felt depressed or contemplated suicide following initiation of a court action, as well as the extent that potential litigation is influencing their work and decisions to perform caesarean sections.
Most respondents would prefer to work under some type of "no-fault" scheme. Many expressed a preference for a publicly funded compensation scheme for all adverse medical events and conditions, along the lines of the New Zealand government's accident compensation scheme. However, a scheme covering all adverse outcomes might increase the number of claims and, unless compensation was capped, could prove expensive. In the United States, it has been estimated that up to 88% of the cost of indemnity and litigation is spent on legal processes and only a small percentage of the total cost is awarded to a small percentage of claimants.5
An adverse event or complication of treatment is not necessarily due to negligence, but without some type of legal or peer review this may not be clear to the public. Some type of independent review system is necessary.
Our survey showed that a majority of obstetric opinions are given by a small number of obstetricians, many of whom have retired from active obstetrics and are not acknowledged by their peers through RANZCOG accreditation as qualified to give medicolegal opinion in this area. This is of concern, as it may lead to inappropriate litigation.
The problems facing the Australian obstetric workforce appear to be multifactorial, and multifaceted solutions may need to be considered to avoid a serious crisis in the delivery of Australia's most precious resource — its children. Some initiatives that could be considered are presented in Box 5.
Until possible long-term solutions have been discussed, enacted and given time to influence recruitment to and retirement from obstetric practice, more immediate, radical, costly and pragmatic policies will be necessary. The public sector must prepare to handle a rapidly increasing number of deliveries as private hospitals cease to offer obstetric services. The metropolitan sector must expect to have to service the rural sector with outlying clinics, and there will be increased transfer of pregnant women to city hospitals. It will be necessary to find more obstetricians and possibly allied staff, such as midwives and anaesthetists, from abroad. In the near future, a reduction in the quality and quantity of obstetric services appears almost inevitable.
3: Indemnity premiums for obstetric practitioners over the previous 12 months, by State/Territory (based on participants' responses)
State/Territory |
25th percentile |
Median |
75th percentile |
Maximum |
|||||||
New South Wales |
$35 750 |
$55 000 |
$67 000 |
$138 000 |
|||||||
Victoria |
$32 000 |
$35 530 |
$45 000 |
$80 000 |
|||||||
Queensland |
$1 500 |
$31 800 |
$39 250 |
$70 000 |
|||||||
South Australia |
$4 850 |
$28 000 |
$33 000 |
$35 000 |
|||||||
Western Australia |
$24 250 |
$48 000 |
$52 580 |
$60 000 |
|||||||
Tasmania |
$14 850 |
$15 000 |
$15 000 |
$16 000 |
|||||||
Northern Territory |
$763 |
$11 900 |
$24 500 |
$25 000 |
|||||||
Australian Capital Territory |
$47 750 |
$61 000 |
$73 000 |
$156 000 |
|||||||
Total |
$20 000 |
$35 515 |
$52 000 |
$156 000 |
|||||||
4: Outcome of litigation commenced against respondents (between 1978 and 2001)
Number of claims commenced in the courts |
401 |
Number of claims settled before trial |
256 |
Number of claims settled during trial |
23 |
Number of claims in which a trial was completed |
26 |
Number of claims in which trial verdict was in favour of defendant |
19 |
Number of claims in which trial verdict was in favour of plaintiff |
4 |
Median value of settled claims (range) |
$60 000 |
5: Initiatives that could be considered to redress the declining numbers of obstetric practitioners
A "no-fault" compensation system for neurologically disabled children.
A scheme of structured awards rather than a single lump-sum payment.
The selection of expert witnesses by the court rather than the plaintiff or the defendant.6
Payment of indemnity premiums to practise private obstetrics in hospitals or in regions where this is required or desirable.
Improvement in working conditions for obstetricians, with reasonable rostered hours achieved through group private practice or increased hospital staff appointments.
Encouragement of team obstetric and midwifery practice.
Greater public education and realistic expectations of the rates of perinatal and maternal mortality and morbidity, including birth defects.
Better access to dispute resolution processes before civil litigation.
The training of specialists specifically to practise only obstetrics or only gynaecology.
Lowering of the statutory time limit in which litigation can occur after birth.
Received 6 March 2002, accepted 28 March 2002
- Alastair H MacLennan1
- Michael K Spencer2
- Department of Obstetrics and Gynaecology, The University of Adelaide, Women's and Children's Hospital, North Adelaide, SA.
Our study was supported by funding from the Australian Medical Association and the National Association of Specialist Obstetricians and Gynaecologists. We thank the Fellows of the Royal Australian College of Obstetricians and Gynaecologists for their responses.
None declared.
- 1. Campbell J. Out of the trenches II. O&G 2001; 3: 199-202. (A quarterly publication by RANZCOG.)
- 2. Bates J, Child A, Woinowski J, et al. RANZCOG/NASOG workforce 2000 survey. O&G 2001; 3: 11-25. (A quarterly publication by RANZCOG.)
- 3. Practice intentions of new Fellows and Trainees. O&G 2001; 3: 140-142. (A quarterly publication by RANZCOG.)
- 4. MacLennan AH. Who will deliver the next generation? Med J Aust 1993; 159: 261-263.
- 5. Ransom SB, Dombrowski MP, Shephard R, Leonardi M. The economic cost of the medical-legal tort system. Am J Obstet Gynecol 1996; 174: 1903-1909.
- 6. The Right Honourable the Lord Woolf. Access to justice. Final report to the Lord Chancellor on the civil justice system in England and Wales. London: HMSO, July 1996.





Abstract
Objectives: To assess the intentions of Australia's specialist obstetricians to cease practice and their reasons for abandoning this specialty.
Design: A structured questionnaire posted to Fellows of the Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG), issued 11 July 2001 with a return date of 31 July 2001 (in practice, responses were accepted up to 31 August 2001).
Participants: Australian specialists holding a Fellowship of the RANZCOG.
Main outcome measures: Demographic data (eg, age, sex); type and location of practice; past, current and intended future obstetric practice; reasons for stopping practice; cost of indemnity premiums; experience of litigation and its influence on practice; and experience in giving medicolegal opinion.
Results: The response rate was 74% (829/1116), with 826 responses fulfilling our selection criteria. The median number of years since admission as a Fellow was 17 (range, 1–47 years), and 19% (158/817) of respondents were women (9 people did not specify their sex). Of the 826 respondents, 596 (72%) were currently practising obstetrics, 548 (66%) intended to still be practising after one year, 365 (44%) intended to be practising after five years, and 196 (24%) intended to be practising after 10 years. The median indemnity premium in 2001–02 was $35 515 (range, nil to $156 000) for practising obstetricians. The main reasons given for ceasing obstetrics were intention to specialise in gynaecology, fear of litigation, high indemnity costs, family disruption, and long working hours. About two-thirds of respondents (557/818) had experienced the threat of litigation, and almost all (768/803) desired some type of "no-fault" indemnity scheme. Thirty-three of the 314 respondents who had given medicolegal opinions accounted for 71% of the total number of opinions. Many of these were non-practising obstetricians who were not accredited RANZCOG expert witnesses.
Conclusion: There will soon be a shortage of experienced practising obstetricians in Australia.