Coronary heart disease (CHD) is a major cause of morbidity and mortality in Australia and is associated with significant cost.1 Australian guidelines recommend that all patients with an acute coronary syndrome (ACS) participate in secondary prevention,2 incorporating risk-factor management including lifestyle change and the use of vasoprotective medications. This is an effective means of extending overall survival, reducing the occurrence of non-fatal cardiovascular events, decreasing the need for coronary revascularisation and improving quality of life.3 Cardiac rehabilitation is a widely recognised form of secondary prevention,4 but participation rates are low (10%–30%)5,6 because of transport difficulties, work and social commitments, lack of perceived need,7 and functional impairment.8 Therefore, despite short-term benefits for attendees, large groups of patients are not benefiting, presenting an opportunity and challenge to improve overall CHD care.8
There are limited data reporting the risk-factor profile of patients not accessing cardiac rehabilitation,9 and, to the best of our knowledge, there are no studies reporting both risk-factor prevalence and knowledge of risk factors in this group. Knowledge of risk factors is an essential basis for active participation in lifestyle changes, medication adherence10,11 and improved quality of life12 — all important aspects of optimal secondary prevention. Patients’ knowledge may be suboptimal,13 and, in this study, we aimed to quantify the CHD risk profile and knowledge of risk factors of outpatients not accessing cardiac rehabilitation after an ACS.
All patients admitted to a metropolitan tertiary referral hospital in Sydney with an ACS between April 2003 and February 2004 were identified using diagnosis-related groups (DRG) codes14 for unstable angina (F72A, F72B), myocardial infarction (F41A, F41B, F60A, F60B) and chest pain (F74Z). Hospital medical records were reviewed to determine secondary prevention eligibility. Reasons for ineligibility included living more than 20 km from the hospital; insufficient understanding of English to give informed consent; and uncontrolled congestive heart failure, severe comorbidity, or death.
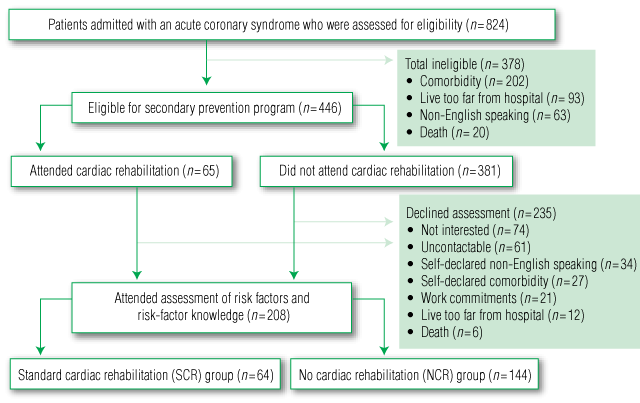
Of the total of 824 admissions, 378 patients (46%) were ineligible for participation in a formal cardiac rehabilitation program (reasons given in Box 1). All 446 eligible patients were contacted by mail and telephone within 12 months of admission and invited to volunteer for research investigating CHD prevention; 235 declined (reasons given in Box 1) and three were excluded because they had previously attended cardiac rehabilitation. Altogether, 208 patients attended for an assessment (Box 1), 64 of whom were about to commence cardiac rehabilitation (standard cardiac rehabilitation [SCR] group) and 144 were not (no cardiac rehabilitation [NCR] group). Reasons for not attending cardiac rehabilitation included: transport problems (19%); work commitments (16%); doing own exercise (8%); not interested (10%); and not referred (47% — due to patient/physician preference and/or scarcity of resources). Risk factors for all eligible patients who did not attend face-to-face assessment were extracted from medical records to permit comparison of risk factors with those who attended assessment.
CHD risk-factor prevalence and level, overall risk profile and knowledge of risk factors were evaluated during a face-to-face assessment at 4.5 ± 0.2 months (mean ± SEM) after admission for an ACS. For 83% of patients accessing standard cardiac rehabilitation, assessment was conducted before the initial appointment and commencement of cardiac rehabilitation. Lipids were measured on a fasting blood sample. Resting blood pressure was measured with an Omron automatic blood pressure monitor (Omron Healthcare Inc, Illinois, USA).15 Smoking status was measured by self-report and confirmed with the aid of a carbon monoxide meter (Air-Met Scientific Micro Smokerlyzer, Melbourne, Vic).16 Physical activity was assessed using the international 7-day physical activity recall questionnaire,17 and depressive mood was assessed using the cardiac depression scale.18 The Medical Outcome Short Form Health Survey (SF-36) (version 2)19,20 was used to assess quality of life, and socioeconomic status was compared between the groups using the socioeconomic index for areas scores (lower values represent regions of greater disadvantage).21
Cutoff points for determining the number of modifiable risk factors were:
total cholesterol level, > 4.0 mmol/L;
systolic blood pressure, ≥ 140 mmHg;
current smoking;
physical inactivity score;17
body mass index, ≥ 30 kg/m;
known diabetes; and
cardiac depression scale score, ≥ 90 for depression.18
The LIPID risk score22 was used to calculate each patient’s relative cardiac risk. This score was developed for use in secondary prevention, and the aggregate score classifies patients as having low (score, ≤ 4), medium (5–6), high (7–9) or very high risk (≥ 10).
Most of the patients were male, born in Australia and were not working (Box 2). Fewer patients in the NCR group than in the SCR group had undergone coronary revascularisation (56% v 86%; P < 0.001), and the mean (± SEM) time between ACS admission and risk-factor assessment was longer in the NCR group (6.3 ± 0.2 months) than the SCR group (3.3 ± 0.2 months). Socioeconomic status was not significantly different between the NCR and SCR groups. Fewer patients in the NCR group than in the SCR group reported taking a statin (69% v 83%, P = 0.02). Other cardiovascular medications were similar in the two groups (Box 3).
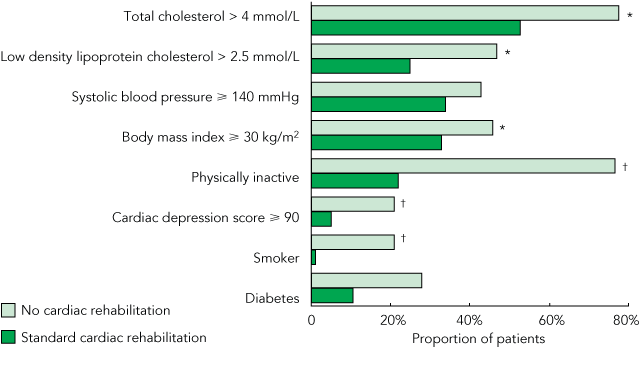
A significantly greater proportion of patients in the NCR group than the SCR group had total cholesterol levels > 4.0 mmol/L, low-density lipoprotein (LDL) cholesterol levels > 2.5 mmol/L, were physically inactive, obese, depressed, and current smokers (Box 4), and had four or more cardiac risk factors. The mean (± SEM) LDL cholesterol level, cardiac depression scale depression score, number of modifiable risk factors and LIPID score were also significantly greater in the NCR than the SCR group (Box 5). Further, the proportion of patients with a LIPID score ≥ 5 (medium-to-high risk) was significantly higher in the NCR than the SCR group (49% v 22%; P < 0.001). Quality of life measured using the SF-36 questionnaire was significantly worse in the NCR group compared with the SCR group in the dimensions: physical functioning (71.6 ± 1.5 v 76.5 ± 2.0; P = 0.008); vitality (50.5 ± 1.5 v 57.3 ± 2.6; P = 0.04); and role-emotional (78.3 ± 2.9 v 93.7 ± 1.8; P = 0.001).
Of the patients in the total cohort with at least one modifiable risk factor, most (137/194, 71%) were unable to state any risk factors. A significantly greater proportion of patients in the NCR group than in the SCR group were unable to state any of their risk factors (75% v 58%; P = 0.013). Also, significantly fewer patients in the NCR group than the SCR group could state nationally recommended targets for total cholesterol level, blood pressure and physical activity (Box 6).
Our study quantifies the CHD risk profile and risk-factor knowledge of patients not accessing cardiac rehabilitation (NCR group) after hospital admission for an ACS. Such patients had a more adverse risk-factor profile and poorer knowledge of cardiac risk factors than those about to commence standard cardiac rehabilitation (SCR group). Although serum cholesterol level is arguably the most important risk factor, fewer patients in the NCR group could state the recommended level and were more likely to have a high total cholesterol level than those in the SCR group. The difference in total cholesterol level between the two groups equates to a predicted increase in CHD risk of about 24%.23
Patients in the NCR group were more likely to be physically inactive, a trait that clusters with other risk factors such as obesity, smoking or depression.1 Patients may decline to take part in an exercise-based program fearing overexertion, or because of self-consciousness resulting from inactivity or obesity. Therefore, an exercise-based approach may not be the most appropriate form of secondary prevention for all patients.
Surprisingly, ACS survivors had very poor knowledge of cardiac risk factors. Over 70% of patients were unable to state any of their own modifiable risk factors. In agreement with our study, a point prevalence study investigating patients’ awareness of risk factors found that only 14/71 patients (20%) could define a cardiac risk factor and, overall, patients had “very little understanding” of their own risk factors.13 Therefore, information about risk factors is not being processed, retained or provided during or after admission. We also found that risk-factor knowledge of patients in the NCR group was significantly inferior to those in the SCG group, while at the same time, the number of risk factors and the risk-factor level was significantly worse.
This highlights a crucial gap in the delivery of care — the patients with the greatest need and poorest knowledge are not accessing formal secondary prevention. Risk factor knowledge has been shown to correlate with greater adherence to lifestyle changes,11 enhanced orientation of patients towards activity, and better health status and quality of life.12 Alternative secondary prevention programs, such as the COACH study,24 or a modular program25 for patients who do not access exercise-based cardiac rehabilitation could improve outcomes by closing this gap in knowledge.
2 Demographic and clinical characteristics of patients with an acute coronary syndrome not attending (NCR group) or attending (SCR group) cardiac rehabilitation. Data are number (%) unless otherwise indicated
History of transient ischaemic attack/cerebrovascular accident/peripheral vascular disease |
|||||||||||||||
3 Medications taken by patients not attending (NCR group) or attending (SCR group) standard cardiac rehabilitation after an acute coronary syndrome
4 Proportion of patients with various risk factors not attending (NRC group) or attending (SCR group) cardiac rehabilitation after an acute coronary syndrome
5 Modifiable cardiac risk factors in patients not attending (NCR group) or attending (SCR group) cardiac rehabilitation after an acute coronary syndrome. Data are mean ± SEM or number (%)
Received 20 March 2006, accepted 4 September 2006
- Julie Redfern1
- Elizabeth R Ellis1
- Tom Briffa2
- S Ben Freedman3,3
- 1 University of Sydney, Sydney, NSW.
- 2 Curtin University of Technology, Perth, WA.
- 3 Department of Cardiology, Concord Repatriation General Hospital, Sydney, NSW.
We wish to thank the participating patients and staff at Concord Hospital in the Cardiology and Medical Records departments. This work was supported by the National Heart Foundation of Australia in the form of a Grant-In-Aide and a Postgraduate Clinical Research Scholarship for Julie Redfern. We also thank the University of Sydney (1 year scholarship for Julie Redfern) and the Cardiac Society of Australia and New Zealand (travel grant for Julie Redfern).
None identified.
- 1. Australian Institute of Health and Welfare. Heart, stroke and vascular diseases, Australian facts 2004. Cardiovascular disease series No. 22. Canberra: AIHW, 2004. (AIHW Catalogue No. CVD 27.)
- 2. Acute Coronary Syndrome Guidelines Working Group. Guidelines for the management of acute coronary syndromes 2006. Med J Aust 2006; 184 (8 Suppl): S1-S32. <MJA full text>
- 3. McAlister FA, Lawson FME, Teo KK, Armstrong PW. Randomised trials of secondary prevention programs in coronary heart disease: systematic review. BMJ 2001; 323: 957-962.
- 4. Taylor RS, Brown A, Ebrahim S, et al. Exercise-based rehabilitation for patients with coronary heart disease: a systematic review and meta-analysis of randomized trials. Am J Med 2004; 116: 682-697.
- 5. Bunker S, McBurney H, Cox H, Jelinek M. Identifying participation rates at outpatient cardiac rehabilitation programs in Victoria, Australia. J Cardiopulm Rehabil 1999; 19: 334-338.
- 6. Scott IA, Lindsay KA, Harden HE. Utilisation of outpatient cardiac rehabilitation in Queensland. Med J Aust 2003; 179: 341-345. <MJA full text>
- 7. Evenson KR, Fleury J. Barriers to outpatient cardiac rehabilitation participation and adherence. J Cardiopulm Rehabil 2000; 20: 241-246.
- 8. Harlan WR, Sandler SA, Lee KL, et al. Importance of baseline functional and socioeconomic factors for participation in cardiac rehabilitation. Am J Cardiol 1995; 76: 36-39.
- 9. Sundararajan V, Bunker SJ, Begg S, et al. Attendance rates and outcomes of cardiac rehabilitation in Victoria, 1998. Med J Aust 2004; 180: 268-271. <MJA full text>
- 10. Czar M, Engler M. Perceived learning needs of patients with coronary artery disease using a questionnaire assessment tool. Heart Lung 1997; 26: 109-117.
- 11. Alm-Roijer C, Stagmo M, Uden G, Erhardt L. Better knowledge improves adherence to lifestyle changes and medication in patients with coronary heart disease. Eur J Cardiovasc Nurs 2004; 3: 321-330.
- 12. Brody DS, Miller SM, Lerman CE, et al. Patient perception of involvement in medical care: relationship to illness attitudes and outcomes. J Gen Intern Med 1989; 4: 506-511.
- 13. Momtahan K, Berkman J, Sellick J, et al. Patients’ understanding of cardiac risk factors: a point-prevalence study. J Cardiovasc Nurs 2004; 19: 13-20.
- 14. Commonwealth Department of Health and Ageing. Australian refined diagnosis related groups (AR-DRGs). AR-DRGs version 4.1 (Vol 1). Canberra: The Department, 1998. http://www.health.gov.au/internet/wcms/publishing.nsf/Content/health-casemix-ardrg1.htm (accessed Oct 2006).
- 15. El Assaad MA, Topouchian J, Asmar RG. Evaluation of two devices for self-measurement of blood pressure according to the international protocol: the Omron MS-I and the Omron 705IT. Blood Press Monit 2003; 8: 127-133.
- 16. Cunningham AJ, Hormbrey P. Breath analysis to detect recent exposure to carbon monoxide. Postgrad Med J 2002; 78: 233-237.
- 17. Booth M. Assessment of physical activity: an international perspective. Res Q Exerc Sport 2000; 71: S114-S120.
- 18. Hare DL, Davis CR. Cardiac depression scale: validation of a new depression scale for cardiac patients. J Psychosom Res 1996; 40: 379-386.
- 19. Ware JE, Sherbourne CD. The MOS 36-item short-form health survey (SF36). I: Conceptual framework and item selection. Med Care 1992; 30: 473-483.
- 20. Ware JE, Snow KK, Kosinski M, Gandek B. SF-36® health survey manual and interpretation guide 1993. Boston, MA: New England Medical Center, The Health Institute, 1993.
- 21. Australian Bureau of Statistics. 1996 Census of population and housing: socio-economic indexes for areas (SEIFA), Australia. Canberra: ABS, 1998. (Catalogue No. 2033.0.30.001.)
- 22. Marschner IC, Colquhoun D, Simes RJ, et al. Long-term risk stratification for survivors of acute coronary syndromes. J Am Coll Cardiol 2001; 38: 56-63.
- 23. Simes JR, Marschener IC, Hunt D, et al, on behalf of the LIPID Study Investigators. Relationship between lipid levels and clinical outcomes in the Long-term Intervention with Pravastatin in Ischaemic Disease (LIPID) trial: to what extent is the reduction in coronary events with pravastatin explained by on-study lipid levels? Circulation 2002; 105: 1162-1169.
- 24. Vale M, Jelinek M, Best JD, Santamaria JD. Coaching patients with coronary heart disease to achieve the target cholesterol: a method to bridge the gap between evidence-based medicine and the “real world” — randomized controlled trial. J Clin Epidemiol 2002; 55: 245-252.
- 25. Redfern J, Ellis E, Briffa T, Freedman SB. Modular prevention of heart disease following acute coronary syndrome (ACS) [ISRCTN42984084]. BMC Cardiovasc Disord 2006; 6: 26.





Abstract
Objective: To document the risk-factor profile and risk-factor knowledge of patients with an acute coronary syndrome (ACS) not attending standard cardiac rehabilitation.
Design and setting: Cross-sectional comparison in a tertiary hospital.
Participants: Patients admitted to hospital with an ACS, residing within 20 km of the hospital, and without severe comorbidity who did not access cardiac rehabilitation (NCR) were compared with a group about to commence standard cardiac rehabilitation (SCR).
Main outcome measures: Risk-factor profile, knowledge of risk factors via face-to-face assessment, quality of life.
Results: Of the 446 patients eligible for cardiac rehabilitation, 208 attended for assessment (NCR: n = 144; SCR: n = 64). The NCR group had higher mean (± SEM) low-density lipoprotein (LDL) cholesterol levels (2.6 ± 0.1 v 2.3 ± 0.1; P = 0.02), and were more likely than the SCR group to have a total cholesterol level of > 4.0 mmol/L (78% v 53%; P < 0.001) and an LDL cholesterol level > 2.5 mmol/L (47% v 25%; P = 0.01). They were more likely than the SCR group to be physically inactive (77% v 22%; P < 0.001); obese (46% v 33%; P = 0.04); depressed (21% v 5%; P < 0.001); or current smokers (21% v 1%; P < 0.001). Compared with the SCR group, the NCR group also had higher risk scores (LIPID risk score) (4.5 v 2.1; P < 0.001); lower quality of life (Medical Outcome Short Form [SF-36] Health Survey); and significantly poorer knowledge of risk factors. Among patients with at least two modifiable cardiac risk factors, the NCR group were less likely than the SCR group to be able to state at least one risk factor (24% v 38%; P < 0.001).
Conclusions: Patients not participating in cardiac rehabilitation after an ACS have more adverse risk profiles and poorer knowledge of risk factors compared with those about to commence cardiac rehabilitation. Alternate models for secondary prevention are required to improve health outcomes in patients not attending cardiac rehabilitation.