Cardiovascular disease is the leading cause of death in Australia, causing more than 40% of all deaths in 1998.1
Cardiac rehabilitation programs aim to help participants achieve lifestyle changes that will modify risk factors, using a combination of exercise, education, counselling and support. Systematic literature reviews of randomised controlled trials assessing the benefits of cardiac rehabilitation have shown that patients attending rehabilitation after myocardial infarction have a 25% decrease in all-cause mortality.2,3 Most participants in these trials were men under 65 years of age, and follow-up varied between 1 and 5 years.
Current recommendations suggest that cardiac rehabilitation should be offered to all patients after cardiac surgery or acute myocardial infarction.4 Studies assessing cardiac rehabilitation attendance rates are few, and are local rather than population-based. A cross-sectional study in the United States found 11% attendance at rehabilitation after myocardial infarction, compared with 23% attendance after cardiac bypass.5 Women and individuals over the age of 65 were poor attendees.5 An Australian pilot study, which was based on data linkage using attendance records from rural hospital-based programs and the state hospital morbidity database, found rates of participation double those of the US study, but was limited in scope.6
Our aim was to develop a prospective, anonymised, population-based data collection of cardiac rehabilitation attendance from throughout Victoria, and (1) calculate cardiac rehabilitation attendance as a proportion of cardiac events, and (2) compare survival rates between attendees and non-attendees and with published survival rates.
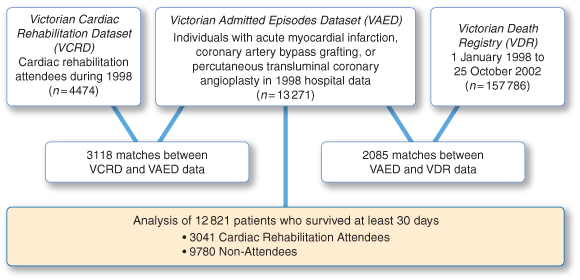
Box 1 shows the databases used and the linkages performed for data extraction. The Victorian Cardiac Rehabilitation Dataset is based on attendance data collected from 66 outpatient cardiac rehabilitation programs for the 12 months January to December 1998. For the purposes of this study, participation was defined as attending at least one session of a rehabilitation program. We estimate that 75% of these attendees completed a full 6–8-week program.
The Victorian Admitted Episodes Dataset (VAED) is a minimum dataset of acute public and private hospital separations throughout Victoria.7 This is an anonymous case-based dataset useful for longitudinal hospital admission follow-up. For each hospital separation, there are 12 diagnosis fields (ICD-9-CM)8 and 12 procedure fields. Data can be grouped to link episodes of care for each individual within the healthcare system.
The Victorian Deaths Registry contains information on all deaths in Victoria, including cause of death.
Bivariate analyses were performed between attendance at cardiac rehabilitation and various characteristics of patients. Subsequently, a multiple logistic regression model was fitted with rehabilitation attendance status as the outcome.
To assess whether there was a difference in survival between cardiac rehabilitation attendees and non-attendees, stratified Kaplan–Meier survival analyses were calculated. These were repeated for subjects who had survived the first year beyond their cardiac diagnosis or procedure. To assess survival benefit after adjusting for the covariates that were related to attendance at cardiac rehabilitation, a Cox proportional hazards model was fitted.
All analyses were conducted using SAS 8.2.9
Seventy per cent (3118/4474) of the cardiac rehabilitation attendees were matched to VAED data (Box 1). The attendees not matched to the VAED did not differ in age or sex from those who did match. (The 1998 rehabilitation attendance dataset included those not represented in 1998 VAED data, as their cardiac event and acute admission occurred late in 1997, and those who attended rehabilitation in Victoria after hospitalisation in another state.) There were 2085 deaths from the initial 13 271 patients with AMI, CABG, or PTCA. Only data for the 12 821 patients who survived at least 30 days after their initial hospitalisation were retained for further analysis.
Although there is no record of known links among these datasets to which we could compare our matches, we were able to estimate the false positive rate for the VAED–death registry linkage based on the time sequence between the date of cardiac diagnosis or procedure and the ascribed date of death in linked records. There were no links in which this time sequence was incorrect, indicating a low false positive rate.
Rates of attendance varied by cardiac diagnosis and procedure. Attendance rates peaked in the 50–59-year age group at 29% and declined after the age of 70 years.Box 2 shows the factors that also influenced attendance. In a multiple logistic regression model (Box 2), age and cardiac diagnosis or procedure were the strongest predictors of attendance, although other factors reached statistical significance.
During follow-up, 243 (8%) of the 3041 cardiac rehabilitation attendees died, compared with 1858 (19%) of the 9780 non-attendees.
At 5 years after an initial cardiac diagnosis or procedure, there was a significant difference between attendees and non-attendees in the probability of survival (Box 3). This difference narrowed when subjects dying in the first year were excluded from the Kaplan–Meier analysis, but remained statistically significant. Adjusting for potential measured confounders with a proportional hazards model revealed that attendance at cardiac rehabilitation showed a difference in survival of 35% (adjusted hazard ratio [HR], 0.65; 95% CI, 0.56–0.75). The survival difference remained when limiting the analysis to patients who survived the first year (HR, 0.70; 95% CI, 0.60–0.82).
Our analysis brought together three diverse datasets to provide insight into attendance rates at cardiac rehabilitation after major cardiac events and the benefit of such participation in terms of survival. In the sample of 12 821 patients with AMI, CABG or PTCA, 24% attended cardiac rehabilitation. This attendance rate is similar to that identified in other studies, but remains poor in terms of uptake of a potentially beneficial therapy. Reasons for poor uptake were not identified in this study and require investigation.
A sharp decline in attendance occurred after the age of 70 years, despite the fact that 45% of our sample were over this age. Women also attended less often, even after controlling for other factors. Admission to a teaching or private hospital also appeared to be related to better attendance.
Attendance at cardiac rehabilitation was associated with a difference in survival in our analysis. This association was stronger than that found in randomised controlled trials and existed across all groups, including the elderly and patients with comorbidities.
Our analysis was subject to information bias due to misclassification. The linkage rate between the VAED and cardiac rehabilitation datasets was 70%, so up to 30% of those who attended cardiac rehabilitation could have been misclassified as non-attendees. (The cardiac rehabilitation dataset includes attendees referred for indications other than AMI, CABG or PTCA [eg, angina and post-cardiac catheterisation].) This suggests that absolute attendance rates may be underestimated. At a maximum, the attendance rate in Victoria may be 35% (4474 attendees, 12 821 cardiac patients surviving at least 30 days). The relative attendance rates in groups of covariates (eg, by age group) and their statistical difference remain meaningful.14
Our observational analysis was subject to confounding due to the non-random assignment of treatment. Thus, the strength of outcome associated with cardiac rehabilitation in our analysis may have been influenced by factors other than cardiac rehabilitation. Nevertheless, the implications of our findings remain strong. Cardiac rehabilitation attendance is underutilised by groups that may benefit most from it: the elderly, women, people with comorbid conditions and those without access to teaching hospitals and private hospitals. Additionally, the reason for the difference in attendance rates after CABG and AMI bears further investigation.
2: Characteristics of patients attending cardiac rehabilitation, and results of multiple logistic regression
|
|
Total number |
Number attending cardiac rehabilitation (%) |
Odds ratio |
|||||||
Entire sample |
|
12 821 |
3041 (24%) |
|
|||||||
Age (years) |
40–49 |
1 065 |
275 (26%) |
1.00 |
|||||||
50–59 |
2 435 |
701 (29%) |
1.06 (0.89–1.25) |
||||||||
60–69 |
3 802 |
1065 (28%) |
1.02 (0.86–1.20) |
||||||||
70–79 |
3 986 |
878 (22%) |
0.79 (0.66–0.93) |
||||||||
80–89 |
1 394 |
121 (9%) |
0.37 (0.29–0.48) |
||||||||
≥ 90 |
139 |
1 (1%) |
0.04 (0.01–0.28) |
||||||||
Sex |
Male |
8 991 |
2327 (26%) |
1.11 (0.99–1.25) |
|||||||
Female |
3 830 |
714 (19%) |
1.00 |
||||||||
Marital status |
Currently married |
9 047 |
2411 (27%) |
1.00 |
|||||||
Never married |
720 |
147 (20%) |
0.77 (0.63–0.93) |
||||||||
Previously married |
2 671 |
426 (16%) |
0.77 (0.68–0.87) |
||||||||
Unknown |
383 |
57 (15%) |
0.52 (0.38–0.69) |
||||||||
Cardiac diagnosis or procedure |
AMI |
4 213 |
612 (15%) |
1.00 |
|||||||
AMI + PTCA |
1 243 |
357 (29%) |
1.59 (0.36–1.86) |
||||||||
AMI + CABG |
719 |
304 (42%) |
3.35 (2.81–4.00) |
||||||||
CABG alone |
3 438 |
1282 (37%) |
2.63 (2.29–3.01) |
||||||||
CABG + PTCA |
100 |
51 (51%) |
3.93 (2.60–5.96) |
||||||||
PTCA alone |
3 108 |
435 (14%) |
0.65 (0.56–0.76) |
||||||||
Number of comorbid conditions* |
0 or 1 |
9 249 |
2405 (26%) |
1.00 |
|||||||
2 or more |
3 572 |
636 (18%) |
0.82 (0.72–0.93) |
||||||||
Congestive cardiac failure |
No |
11 026 |
2777 (25%) |
1.00 |
|||||||
Yes |
1 795 |
264 (15%) |
0.78 (0.66–0.92) |
||||||||
Index admission to intensive care unit |
No |
9 404 |
2094 (22%) |
1.00 |
|||||||
Yes |
3 417 |
947 (28%) |
1.01 (0.92–1.12) |
||||||||
Index admission classified as emergency |
No |
6 175 |
1564 (25%) |
1.00 |
|||||||
Yes |
6 646 |
1477 (22%) |
1.40 (1.25–1.56) |
||||||||
Type of hospital for index admission |
Teaching hospital |
7 055 |
1762 (25%) |
1.00 |
|||||||
Private hospital |
3 585 |
958 (27%) |
1.32 (1.17–1.48) |
||||||||
Other† |
2 181 |
321 (15%) |
0.65 (0.56–0.75) |
||||||||
Accessible geographic place of residence‡ |
No |
2 477 |
489 (20%) |
1.00 |
|||||||
Yes |
10 344 |
2552 (25%) |
1.28 (1.13–1.45) |
||||||||
Lowest quartile of economic resources§ |
No |
11 482 |
2841 (25%) |
1.00 |
|||||||
Yes |
1 339 |
200 (15%) |
0.65 (0.55–0.77) |
||||||||
AMI = Acute myocardial infarction. CABG = Coronary artery bypass grafting. PTCA = Percutaneous transluminal coronary angioplasty. |
|||||||||||
3: Survival for attendees and non-attendees of cardiac rehabilitation programs
Survival time (years) |
Probability of survival (95% CI) |
||||||||||
Non-attendees |
Attendees |
||||||||||
All patients |
|||||||||||
0 |
1.000 |
|
1.000 |
|
|||||||
1 |
0.943 |
(0.939–0.948) |
0.985 |
(0.981–0.989) |
|||||||
2 |
0.903 |
(0.898–0.909) |
0.965 |
(0.959–0.972) |
|||||||
3 |
0.866 |
(0.859–0.872) |
0.953 |
(0.945–0.96) |
|||||||
4 |
0.833 |
(0.826–0.84) |
0.933 |
(0.924–0.941) |
|||||||
5 |
0.795 |
(0.786–0.803) |
0.908 |
(0.897–0.92) |
|||||||
Patients who survived at least 1 year |
|||||||||||
1 |
1.000 |
|
1.000 |
|
|||||||
2 |
0.963 |
(0.960–0.967) |
0.982 |
(0.977–0.987) |
|||||||
3 |
0.923 |
(0.918–0.928) |
0.969 |
(0.963–0.975) |
|||||||
4 |
0.888 |
(0.882–0.895) |
0.948 |
(0.941–0.956) |
|||||||
5 |
0.847 |
(0.839–0.856) |
0.924 |
(0.913–0.935) |
|||||||
Received 30 June 2003, accepted 4 November 2003
- Vijaya Sundararajan1
- Stephen Begg2
- Ric Marshall3
- Stephen J Bunker4
- Helen McBurney5
- 1 Department of Human Services, Melbourne, VIC.
- 2 Department of Cardiac Rehabilitation, National Heart Foundation, West Melbourne, VIC.
- 3 Department of Physiotherapy, La Trobe University, Melbourne, VIC.
We wish to acknowledge the significant contribution of Jane Reid to data collection and management.
None identified.
- 1. Australian Institute of Health and Welfare. Heart, stroke, and vascular diseases -— Australian facts 2001. Canberra: AIHW, National Heart Foundation of Australia, National Stroke Foundation of Australia, 2001. (AIHW Catalogue No. CVD 13; Cardiovascular Disease Series No. 14.)
- 2. Oldridge NB, Guyatt GH, Fischer ME, Rimm AA. Cardiac rehabilitation after myocardial infarction. Combined experience of randomized clinical trials. JAMA 1988; 260: 945-950.
- 3. Jolliffe JA, Rees K, Taylor RS, et al. Exercise-based rehabilitation for coronary heart disease. Cochrane Database Syst Rev 2001: CD001800.
- 4. National Heart Foundation of Australia: recommendations for cardiac rehabilitation. Canberra: National Heart Foundation of Australia, 1998.
- 5. Thomas RJ, Miller NH, Lamendola C, et al. National survey on gender differences in cardiac rehabilitation programs. Patient characteristics and enrolment patterns. J Cardiopulm Rehabil 1996; 16: 402-412.
- 6. Bunker S, McBurney H, Cox H, Jelinek M. Identifying participation rates at outpatient cardiac rehabilitation programs in Victoria, Australia. J Cardiopulm Rehabil 1999; 19: 334-338.
- 7. Acute Health Division. The Victorian Admitted Episodes Dataset: an overview. April 2000. Melbourne: Acute Health Division, Victorian Department of Human Services, 2000.
- 8. Commission on Professional and Hospital Activities. The international classification of diseases. 9th revision. Clinical modification (ICD-9-CM). 8th ed. Ann Arbor, MIch: Edwards Brothers, Inc, 1989.
- 9. SAS [computer program]. Version 8.2. Cary, NC: SAS Institute Inc, 2002.
- 10. Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 1987; 40: 373-383.
- 11. Deyo RA, Cherkin DC, Ciol MA. Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 1992; 45: 613-619.
- 12. Measuring remoteness: Accessibility/Remoteness Index of Australia (ARIA). Occasional Papers: New Series No. 14. Canberra: Commonwealth Department of Health and Aged Care, October 2001.
- 13. Australian Bureau of Statistics. Information paper: 1996 census of population and housing — socioeconomic indexes for areas, Australia. Canberra: ABS, 1998. (Catalogue No. 2039.0.)
- 14. Mertens TE. Estimating the effects of misclassification. Lancet 1993; 342: 418-421.





Abstract
Objective: To describe the patterns of use of cardiac rehabilitation in Victoria and to assess whether the survival benefits predicted in clinical trials have been realised in the community.
Design: Cohort study based on data linkage.
Participants: All patients admitted for acute myocardial infarction (AMI), coronary artery bypass grafting (CABG) or percutaneous transluminal coronary angioplasty (PTCA) in Victoria in 1998 (n = 12 821).
Interventions: Attendance at one of 66 participating outpatient cardiac rehabilitation centres in Victoria.
Main outcome measures: Rates of attendance at rehabilitation based on key factors such as diagnosis, age, sex, and comorbidity. Five-year survival for attendees compared with non-attendees.
Results: Rates of participation in rehabilitation were 15% for AMI, 37% for CABG, and 14% for PTCA. Rehabilitation attendance rates dropped sharply after 70 years of age. Attendees had a 35% improvement in 5-year survival (hazard ratio for death associated with rehabilitation attendance, 0.65 [95% CI, 0.56–0.75]).
Conclusions: Attendance rates at cardiac rehabilitation are suboptimal, even though attendance confers a clinically significant difference in 5-year survival. The elderly, women, and those with comorbid conditions may benefit measurably from increased rates of attendance.