Mammal bite injuries include puncture wounds, lacerations, avulsions and crush injuries,1 and may result in infection,1-4 disease transmission,2,3,5,6 disfigurement,7 serious injury or death.1,7 The nature and severity of bite injuries vary with the type of animal involved7-10 as well as with the characteristics of the victim, such as age and height.7,8,10,11 The different types of wounds8,12 and likelihood and nature of any infection3,8 resulting from the various mammal species have a significant effect on patient management. Additionally, the injuries caused by dog and cat bites can result in considerable expense because of the need for long-term intravenous antibiotics, surgery and other medical treatments.1 Finally, such injuries represent a preventable public health burden that may be reduced by public education about responsible pet ownership, and regulations regarding animal control.13
We studied a retrospective case series of patients who sustained mammal bite injuries in Victoria between 1998 and 2004, inclusive. Victoria has a population of about 5 million people with a median age of 36.8 years.14 Its geography and land use vary widely and it supports a diversity of domestic, introduced and native mammal species.
Injury and death data were obtained from the Victorian Emergency Minimum Dataset (VEMD) (1998–2004) and the National Coroners Information System (NCIS) (1 July 2000 – 1 June 2006), respectively. The VEMD injury data collection is administered by the Victorian Injury Surveillance Unit at Monash University Accident Research Centre. All Victorian public hospital emergency departments (EDs) running a 24-hour department now submit data.15
Nature of main injury coded as either “bite (non-venomous)” or “bite (not otherwise specified)”.
External injury coded as “horse related”, “dog related”, “other animal related”; or, for human bites, “struck by or collision with person”.
Description of injury event included bite and/or animal related words.
During the study period, 1 544 094 patients received treatment at the participating EDs, with 12 982 (0.8%) presenting with mammal bite injuries. Dogs, humans and cats inflicted almost all the bites (95.6%) (Box 1). A wide range of other mammals were involved including native, domestic, pet and exotic species. Native Australian animals caused 128 injuries (1.0%).
The median age (interquartile range) of the patients was 27 (11–42) years. Younger patients predominated, with the toddler age group (1–4 years) comprising 1528 patients (11.8%). As shown in Box 2, bites from dogs and “other” mammals (all other mammals except dogs, cats and humans) were most common among children, but there was a downwards trend in these bites among those over 30 years of age. In contrast, human and cat bites peaked in people in early and mid adulthood.
Males accounted for 7236 patients (55.7%), and more males than females were bitten by dogs (56.3%) and humans (73.7%) (Box 3). On the other hand, more females were bitten by cats (64.1%) and “other” mammals (55.6%).
Overall, hand and wrist injuries were the most common (Box 4). Dog bite injuries most commonly involved the hands/wrists, face/head or legs. Human bite injuries were most common on the hands/wrists, arms or face/head. In contrast, cat and “other” mammal bite injuries were relatively uncommon on the face and head.
The proportion of mammal bite injuries among ED presentations (0.8%) is consistent with the findings of other reports.2,7,8 However, differing inclusion criteria and indigenous mammal species make comparisons with other reports difficult.9,10,13,14,16-20 In our study, dogs were responsible for almost 80% of all injuries. Similar proportions have been reported elsewhere, although these vary between 50% and 90%.2,3,8-10,21 We found human bite injuries were more common than those from cats, consistent with findings in some reports,2,21,22 but not in others.6,8
Clear patterns exist between patient age and each important mammal species. The large numbers of young children with dog bite injuries have been well documented.3,12,13,16,17,23 Children are particularly vulnerable to dog attacks, due to their size and the proximity of their face to the dog’s mouth, and attacks are frequently associated with interaction with the dog (possibly provocative) before the attack.11,17 Very young children were also often bitten by mammals other than dogs, cats and humans. Horses and rats were commonly implicated in bite injuries in children aged under 10 years. However, the “other” mammals group was heterogeneous and should be examined further before firm conclusions are drawn. Finally, large numbers of human bite injuries among young adults have also been reported elsewhere4 and may be associated with the social interactions of this age group.
Others have also reported that males are more often victims of dog bites2,9,11,13,18 and females of cat bites.2,3,9
The admissions and deaths reported in our study indicate the severity of many bite injuries. The varying patterns of injury site for each mammal group are consistent with other reports.6,8,9,11 The common upper-limb injuries may have resulted from direct handling, or from attempts to separate fighting animals or aid injured ones.1
The home was clearly the most common location for bites to occur, and this is consistent with other reports.1 However, additional data, especially “time of exposure”, are required to further explore location patterns.
Our study has important limitations. The data are likely to underestimate injury incidence,2,8 as they do not account for bites not requiring medical attention, and those treated by general practitioners and other doctors, and at private or non-VEMD EDs. Furthermore, there may be an inherent selection bias in that bites from some animals (eg, dogs) may be more severe and more likely to require ED management. The VEMD is a relatively reliable and valid dataset,24 although there are identification and coding errors as well as missing data.
Mammal bite injuries represent a considerable public health burden, and ongoing prevention strategies are indicated. These should include public educational programs,25 the separation of young children from dogs, avoidance of high-risk dogs by parents, neutering and regulatory reinforcement (ie, restriction of ownership and breeding of high-risk dog breeds), and appropriate restraint of animals in public places.17 Research into bite injury rates (injuries per person-hour of contact) would better clarify the risk of injury for each species and is recommended.
2 Main mammal species causing bite injuries in Victoria, 1998–2004, by patient age
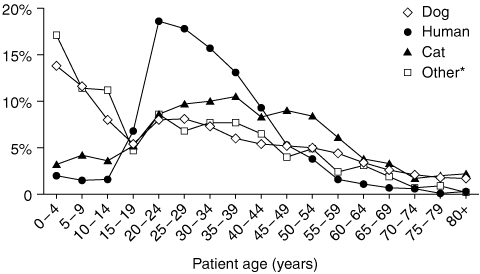
* For a complete list of mammals involved in bites, see Box 1.
3 Patient sex by main mammal species causing bite injuries in Victoria, 1998–2004
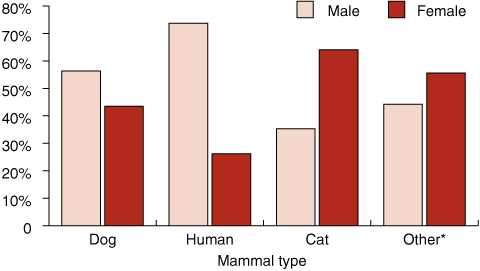
* For a complete list of mammals involved in bites, see Box 1.
- Catherine E MacBean1
- David McD Taylor1,2
- Karen Ashby3
- 1 Emergency Department, Royal Melbourne Hospital, Melbourne, VIC.
- 2 Emergency Department, Austin Hospital, Melbourne, VIC.
- 3 Monash University Accident Research Centre, Melbourne, VIC.
None identified.
- 1. Benson LS, Edwards SL, Schiff AP, et al. Dog and cat bites to the hand: treatment and cost assessment. J Hand Surg [Am] 2006; 31: 468-473.
- 2. Goldstein EJC. Bite wounds and infection. Clin Infect Dis 1992; 14: 633-640.
- 3. Stump JL. Animal bites. http://www.emedicine.com/emerg/topic60.htm (accessed Feb 2006).
- 4. McNamara RM. Human bites. http://www.emedicine.com/emerg/topic61.htm (accessed Feb 2006).
- 5. Managing bites from humans and other mammals. Drug Ther Bull 2004; 42: 67-71.
- 6. Pretty IA, Anderson GS, Sweet DJ. Human bites and the risk of human immunodeficiency virus transmission. Am J Forensic Med Pathol 1999; 20: 232-239.
- 7. Smith PF, Meadowcroft AM, May DB. Treating mammalian bite wounds. J Clin Pharm Ther 2000; 25: 85–99.
- 8. Griego RD, Rosen T, Orengo IF, et al. Dog, cat, and human bites: a review. J Am Acad Dermatol 1995; 33: 1019-1029.
- 9. Ostanello F, Gherardi A, Caprioli A, et al. Incidence of injuries caused by dogs and cats treated in emergency departments in a major Italian city. Emerg Med J 2005; 22: 260-262.
- 10. Matter HC; Sentinella Arbeitsgemeinschaft. The epidemiology of bite and scratch injuries by vertebrate animals in Switzerland. Eur J Epidemiol 1998; 14: 483-490.
- 11. Patrick GR, O’Rourke KM. Dog and cat bites: epidemiologic analyses suggest different prevention strategies. Public Health Rep 1998; 113: 252-257.
- 12. Bower MG. Managing dog, cat, and human bite wounds. Nurse Pract 2001; 26: 36-38, 41-42, 45-47.
- 13. Ashby K. Dog Bites. Victorian injury surveillance system. Hazard 1996; 26; 7-13.
- 14. Australian Bureau of Statistics. Population by age and sex, Australian states and territories, Jun 2005. Canberra: ABS, 2005. (ABS Catalogue No. 3201.0.)
- 15. Victorian Emergency Minimum Dataset. http://www.health.vic.gov.au/hdss/vemd (accessed Jan 2006).
- 16. Centers for Disease Control and Prevention. Nonfatal dog bite-related injuries treated in hospital emergency departments — United States, 2001. MMWR Morb Mortal Wkly Rep 2003; 52: 605-610.
- 17. Ozanne-Smith J, Ashby K, Stathakis VZ. Dog bite and injury prevention — analysis, critical review, and research agenda. Inj Prev 2001; 7: 321-326.
- 18. Thompson PG. The public health impact of dog attacks in a major Australian city. Med J Aust 1997; 167: 129-132. <MJA full text>
- 19. Weiss HB, Friedman DI, Coben JH. Incidence of dog bite injuries treated in emergency departments. JAMA 1998; 279: 51-53.
- 20. Bernardo LM, Gardner MJ, Rosenfield RL, et al. A comparison of dog bite injuries in younger and older children treated in a pediatric emergency department. Pediatr Emerg Care 2002; 18: 247-249.
- 21. Aghababian RV, Conte JE. Mammalian bite wounds. Ann Emerg Med 1980; 9: 79-83.
- 22. Klaassen B, Buckley JR, Esmail A. Does the Dangerous Dogs Act protect against animal attacks: a prospective study of mammalian bites in the accident and emergency department. Injury 1996; 27: 89-91.
- 23. Australian Bureau of Statistics. National health survey: injuries, Australia. Canberra: ABS, 2003. (ABS Catalogue No. 4384.0.)
- 24. Stokes M, Ozanne-Smith J, Harrison J, et al. Validation of an injury surveillance epidemiological data system used within emergency departments. Inj Control Saf Promot 2000; 7: 219-232.
- 25. Chapman S, Cornwall J, Righetti J, et al. Preventing dog bites in children: randomised controlled trial of an educational intervention. BMJ 2000; 320: 1512-1513.





Abstract
Objective: To describe the epidemiology of mammal (human and non-human) bite injuries in Victoria.
Participants, design and setting: Retrospective case series of injuries recorded in the Victorian Emergency Minimum Dataset (VEMD) (1998–2004) and deaths recorded in the National Coroners Information System (1 July 2000 – 1 June 2006).
Main outcome measures: Frequency, nature and outcome of injury as a function of mammal, victim demographics and season.
Results: Of 12 982 bite injuries identified in the VEMD, dogs, humans, and cats were implicated in 79.6%, 8.7%, and 7.2% of cases, respectively. Dog bite injuries were commonly sustained to the hands/wrists (31.3%) and face/head (25.4%); cat bites to the hands/wrists (67.6%) and arms (16.0%); and human bites to the hands/wrists (37.1%), arms (20.5%) and face/head (20.4%). Males comprised 73.7% and 56.3% of human and dog bite victims, respectively, while females comprised 64.1% of cat bite victims. A third of dog bite victims (33.4%) were children aged 14 years or less. Most human bite victims (79.8%) were adults aged 20–49 years, inclusive. More injuries were sustained on weekends and during the summer, 55.4% of injuries occurred in the home, and 11.6% of patients required hospital admission. Dog bites resulted in three deaths.
Conclusions: Mammal bite injuries are common and often require inpatient care. Patterns of bite injuries relate to the type of mammal involved. These epidemiological data will inform prevention initiatives to decrease the incidence of mammal bites.