As men age, they are more likely to visit doctors, primarily because of chronic disease.1 Reproductive health also deteriorates with advancing age, as significant numbers of men are affected by prostate disease, erectile dysfunction (ED) and lower urinary tract symptoms (LUTS).2-5 Yet, given the prevalence of reproductive health disorders in middle-aged and older men, treatment rates are strikingly low. For example, studies demonstrate a wide gap between the estimated prevalence of ED and the number of men actively seeking or undergoing treatment.2,3,6
The methods and initial findings from the Men in Australia Telephone Survey (MATeS) have been described previously.2 In brief, between September and December 2003, computer-assisted telephone interviews (CATIs) of a representative sample of men (aged 40 years and over) were undertaken. Respondents were recruited from across all Australian states and territories by random selection of households from the electronic telephone directory (Electronic White Pages), with oversampling in some age groups and geographic regions to ensure proportionate representation. The study was approved by the Southern Health Human Research Ethics Committee, Melbourne.
The CATI included more than 90 questions on sociodemographic, biomedical and lifestyle factors, and knowledge and attitudes about male reproductive health and disorders. The full CATI is available on the Andrology Australia website (http://www.andrologyaustralia.org/docs/Methods_Manual_CATI.pdf).
All information obtained from the interview was self-reported with no check against medical records. Where available, questions from other validated instruments and those previously used in an Australian context were incorporated.2
Age, marital status, country of birth, occupation level and educational attainment were asked of all respondents. Sociodemographic characteristics of the men participating in the study were representative of the Australian population.2 Men of Indigenous (Aboriginal or Torres Strait Islander) origin represented 1% of men born in Australia. Men who were not Australian-born were classified as being of non-English-speaking or English-speaking background, according to their country of birth.
The Accessibility and Remoteness Index of Australia (ARIA) database7 was used to compare the self-reported prevalence of help-seeking behaviour across geographic regions and differentiated into “major cities” and “regional and remote” areas.
Sample proportions were weighted according to age and state of residence, with weighting based on the age distribution of Australian men in the 2001 census.8 Descriptive analyses were performed using SPSS software (SPSS Inc, Chicago, Ill, USA). Multivariable logistic regression analysis estimated the joint contribution of age, marital status, education, occupation level, geographic location and cultural (non-Australian-born or Indigenous) background to each help-seeking behaviour. Sampling weights were not incorporated into the logistic regression analyses as the outcomes of interest were the associations between measured variables, rather than prevalence estimates. Logistic regression analyses were performed using Stata statistical software, release 9.1 (StataCorp, College Station, Tex, USA).
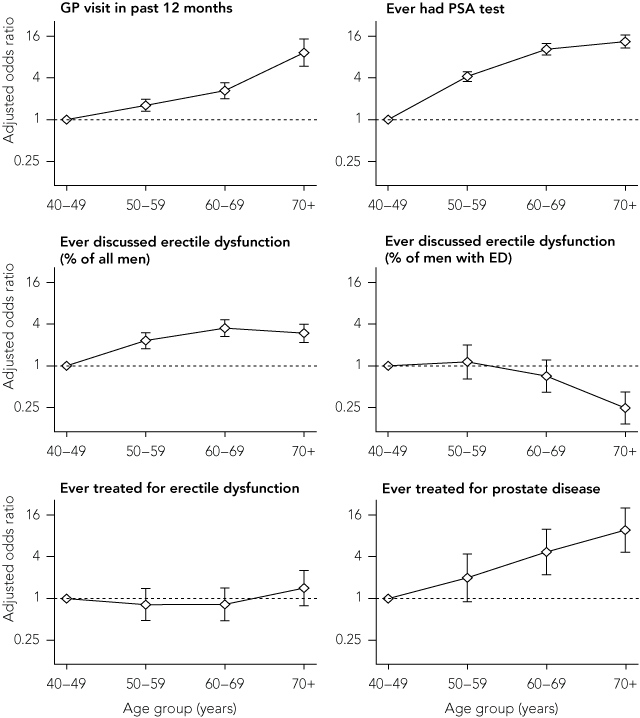
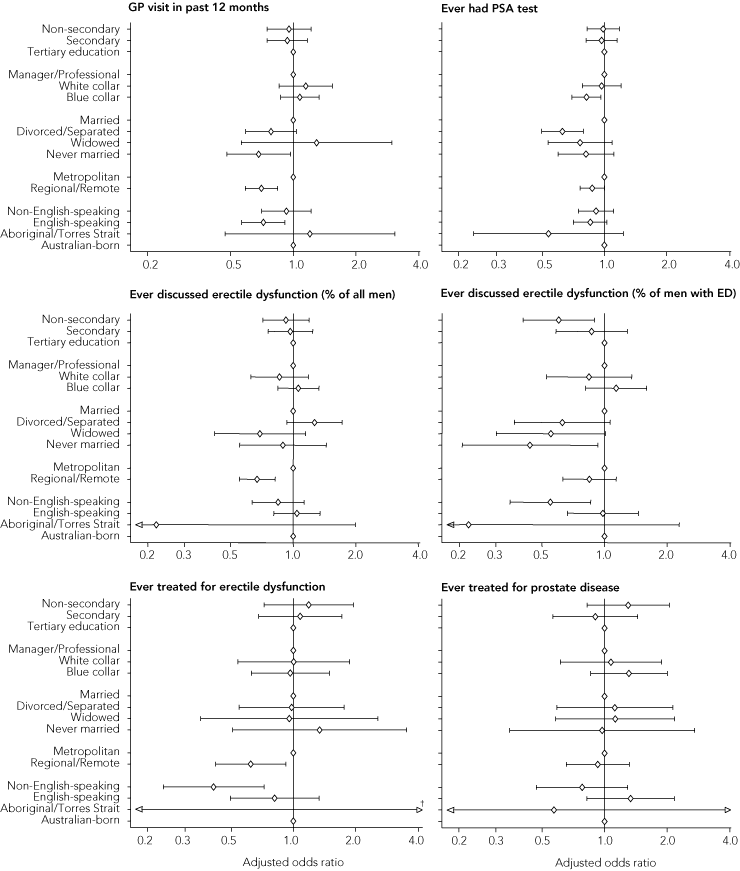
When controlling for all predictor variables, age was a strong predictor for all help-seeking behaviour examined, except treatment for ED (Box 1). The associations of educational attainment, occupation level, marital status, geographic location and cultural (non-Australian-born or Indigenous) background with help-seeking behaviour are shown in Box 2.
Overall, about 88% of men surveyed had visited a doctor in the past 12 months, with health service utilisation increasing with age (Box 1). Controlling for other predictor variables, men who had never married or who were living in regional or remote locations were less likely to have visited a doctor in the previous 12 months (odds ratio [OR], 0.68 [95% CI, 0.48–0.97], P = 0.03; and OR, 0.70 [95% CI, 0.59–0.84], P = 0.001, respectively). Educational attainment and occupational level did not influence visiting a doctor (Box 2).
In this study, 49% of men reported having had a prostate-specific antigen (PSA) test, with the proportion increasing with age (Box 1). Being divorced or separated was an independent predictor of lower uptake of PSA testing (OR, 0.63 [95% CI, 0.50–0.79], P < 0.001). Likewise, men employed in a trade, labouring or related work (that is, “blue collar” workers) were less likely to undergo PSA testing (OR, 0.82 [95% CI, 0.70–0.96], P = 0.02). Educational attainment, geographic location, non-English-speaking background and Indigenous background were not independently predictive of having a PSA test (Box 2).
Of all men surveyed, irrespective of whether they had erectile problems, 11% indicated they had spoken to a health professional about ED. Overall, 21% of men reported moderate to severe ED (“sometimes” or “never” being able to get and maintain an erection), of whom 38% (ie, 8% of all men) had spoken to a health professional about their condition. Older men as a whole were more likely to discuss erectile problems with a health professional but, among men with ED, older men were less likely to do so (Box 1). Living in a regional or remote location was independently associated with a reduced likelihood of consulting a health professional about ED generally (OR, 0.67 [95% CI, 0.55–0.82], P < 0.001). However, geographic location was not a significant predictor for those men with moderate to severe ED (Box 2).
Additional significant predictors were also identified for men with ED to discuss the problem with a health professional. Marital status independently modified the help-seeking behaviour, with never-married men significantly less likely to discuss ED with a health professional (OR, 0.44 [95% CI, 0.21–0.93], P = 0.03). Men from a non-English-speaking background and those with below-secondary school education were also less likely to discuss ED with a health professional (OR, 0.55 [95% CI, 0.35–0.86], P = 0.009, and OR, 0.60 [95% CI, 0.41–0.89], P = 0.01, respectively) (Box 2).
Overall, the treatment rate for ED (58% of men who had spoken with a health professional about ED) was similar to that for prostate disease (61% of men with a diagnosis of prostate disease). While older men were more likely to be treated for prostate disease, age itself was not an independent predictor of treatment for ED (Box 1). Indeed, age was the only independent predictor of prostate disease treatment, with no association seen with educational attainment, occupation level, marital status, geographic location and cultural (non-Australian-born or Indigenous) background (Box 2). In contrast, men from a non-English-speaking background and those living in regional or remote locations were less likely to receive treatment for ED (OR, 0.41 [95% CI, 0.24–0.72], P = 0.002, and OR, 0.62 [95% CI, 0.42–0.92], P = 0.02, respectively) (Box 2).
We already know that ED and prostate disease are widespread problems affecting significant numbers of middle-aged and older Australian men (21% and 14%, respectively, of men aged 40 years and over),2 with an increased prevalence in older age groups.2-5 Education strategies directed at both the general public and health professionals, highlighting that significant numbers of men are affected by these conditions, will help reduce the barriers to men accessing information and health services, and facilitate discussion of these issues.
However, our research shows that these reproductive health problems are often not explicitly discussed with a health professional. Various factors appear to influence help-seeking behaviour for the different conditions, as reflected to some degree by the high proportion of men undertaking testing for prostate disease, while fewer seek treatment for ED.3,9 The presence of LUTS, which men may erroneously associate with prostate cancer, may prompt many to have PSA testing.10 In contrast, ED is not a significant motivator for seeking treatment, as many of the oldest men regard the condition as a normal part of ageing.9 Focusing education campaigns on the association between ED, cardiovascular disease and diabetes, and providing high-quality, evidence-based information on ED, may help influence men to seek treatment for erectile problems. Similarly, education is needed to prompt medical practitioners to opportunistically enquire about reproductive health as part of a general health assessment, with older men benefiting from ongoing medical surveillance in areas of sexual behaviour and lifestyle issues.
We also found that 49% of the men surveyed had had a PSA test, with the proportion increasing with age. Despite the lack of a national policy on population screening for prostate cancer, the prevalence of de facto screening with PSA testing appears relatively high in Australia.2,11 General practitioners assume a key role in a patient’s decision to undergo PSA testing, with a focus on shared decision making after discussion of the benefits and limitations of PSA screening.12 Conversely, we found that sexual health is often not discussed in primary care, particularly for older men,13 a phenomenon at least partly attributable to doctors’ perceptions that older people have low sexual interest and activity,14 and partly to the fact that many older men view ED as a normal part of ageing.9 However, as ED may be a harbinger of chronic medical conditions, such as diabetes, depression and cardiovascular disease,15 and is of great concern to men,2 medical practitioners should be encouraged to actively enquire into this area of reproductive health, irrespective of age or sexual desire.
In this study, marital status was a predictive factor for health service utilisation, particularly speaking to a health professional about ED, highlighting the influence of partners in help-seeking specifically for reproductive health disorders. As the presence of a conjugal partner appears to influence uptake of health services,16 targeted education and health promotion strategies for men without long-term partners need to be considered. Indeed, women are often regarded as the custodians of family health, including influencing men’s access to health services.16,17
We also found clear rural–urban gradients in help-seeking behaviour, independent of other predictors. For men living in regional or remote locations, more limited access to health services18 may be an involuntary barrier to health service utilisation. Likewise, treatment for erectile problems may be influenced by limited opportunities for discreet consultations in smaller communities.19 Similarly, speaking to a health professional about ED is influenced by cultural background, with men of non-English-speaking and Indigenous background less likely to speak to a health professional about the condition.2 Education strategies for health professionals working with these population groups also need to recognise the impact of cultural beliefs on sensitive personal health issues.
While no distinctive associations were identified for help-seeking behaviour of men of Indigenous background, this can be partly explained by their small numbers in the survey, and the correspondingly wide confidence intervals. However, with high rates of cardiovascular disease and diabetes among Indigenous men,20 anecdotal evidence suggests that ED is probably more prevalent than currently appreciated. The trends seen suggest that more strategic research and culturally appropriate health services need to be considered for Indigenous men.21
General practitioners, while often seen as the primary source of contact for reproductive health problems, are often reluctant to initiate discussions with older patients about sexual health.13,22 However, as middle-aged and older Australian men do attend doctors, education strategies for health professionals need to focus on making better use of the medical consultation to opportunistically engage men in discussing under-recognised reproductive health problems. Finally, community education strategies that raise awareness and understanding of male reproductive health disorders will help reduce the stigma associated with these conditions and reinforce help-seeking behaviour and the prospects for effectively addressing men’s reproductive health concerns.
Received 21 February 2006, accepted 3 August 2006
- Carol A Holden1
- Damien J Jolley2
- Robert I McLachlan3
- Marian Pitts4
- Robert Cumming5
- Gary Wittert6
- David J Handelsman7
- David M de Kretser1
- 1 Andrology Australia, Monash University, Melbourne, VIC.
- 2 Monash Institute of Health Services Research, Monash University, Melbourne, VIC.
- 3 Prince Henry's Institute, Melbourne, VIC.
- 4 Australian Research Centre in Sex, Health and Society, La Trobe University, Melbourne, VIC.
- 5 Centre for Education and Research on Ageing and School of Public Health, University of Sydney, Sydney, NSW.
- 6 Department of Medicine, University of Adelaide, Adelaide, SA.
- 7 Concord Hospital and ANZAC Research Institute, University of Sydney, Sydney, NSW.
The Australian Government Department of Health and Ageing provided financial support for Andrology Australia but had no role in the study design, collection, analysis or interpretation of data, or writing or publication of this article. We thank the Hunter Valley Research Foundation, NSW, for assistance in survey administration and data collection; Dr Megan Cock for constructive criticism of the manuscript; and Professor Graeme Hugo and Mr Errol Bamford (National Centre for Social Applications of Geographic Information Systems [GISCA], University of Adelaide, SA) for providing the Accessibility and Remoteness Index of Australia (ARIA) database.
None identified.
- 1. Bayram C, Britt H, Kelly Z, Valentin L. Male consultations in general practice in Australia 1999-00. Canberra: Australian Institute of Health Welfare, 2002. (AIHW Cat. No. GEP 11, General Practice Series No. 11.)
- 2. Holden CA, McLachlan RI, Pitts M, et al. Men in Australia Telephone Survey (MATeS): a national survey of the reproductive health and concerns of middle-aged and older Australian men. Lancet 2005; 366: 218-224.
- 3. Rosen RC, Fisher WA, Eardley I, et al. The multinational Men’s Attitudes to Life Events and Sexuality (MALES) study: 1. Prevalence of erectile dysfunction and related health concerns in the general population. Curr Med Res Opin 2004; 20: 607-617.
- 4. Pinnock CB, Marshall VR. Troublesome lower urinary tract symptoms in the community: a prevalence study. Med J Aust 1997; 167: 72-75. <MJA full text>
- 5. Garraway WM, Collins GN, Lee RJ. High prevalence of benign prostatic hypertrophy in the community. Lancet 1991; 338: 469-471.
- 6. Ansong KS, Lewis C, Jenkins P, Bell J. Help-seeking decisions among men with impotence. Urology 1998; 52: 834-837.
- 7. Department of Health and Aged Care; University of Adelaide. Measuring remoteness: accessibility/remoteness index of Australia (ARIA). Occasional Papers: new series no. 6. Canberra: Commonwealth of Australia, 1999.
- 8. Australian Bureau of Statistics. Population by age and sex, 2001 Census edition. Canberra: ABS, 2003. (ABS Cat. No. 3201.0.)
- 9. Shabsigh R, Perelman MA, Laumann EO, Lockhart DC. Drivers and barriers to seeking treatment for erectile dysfunction: a comparison of six countries. BJU Int 2004; 94: 1055-1065.
- 10. Weller D, Pinnock C, Silagy C, et al. Prostate cancer testing in SA men: influence of sociodemographic factors, health beliefs and LUTS. Aust N Z J Public Health 1998; 22: 400-402.
- 11. Coory MD, Baade PD. Urban–rural differences in prostate cancer mortality, radical prostatectomy and prostate-specific antigen testing in Australia. Med J Aust 2005; 182: 112-115. <MJA full text>
- 12. Pinnock CB. PSA testing in general practice: can we do more now? Med J Aust 2004; 180: 379-381. <MJA full text>
- 13. Gott M, Hinchliff S, Galena E. General practitioner attitudes to discussing sexual health issues with older people. Soc Sci Med 2004; 58: 2093-2103.
- 14. Holden CA, McLachlan RI, Cumming R, et al. Sexual activity, fertility and contraceptive use in middle-aged and older men: Men in Australia, Telephone Survey (MATeS). Hum Reprod 2005; 20: 3429-3434.
- 15. Feldman HA, Goldstein I, Hatzichristou DG, et al. Impotence and its medical and psychosocial correlates: results of the Massachusetts Male Aging Study. J Urol 1994; 151: 54-61.
- 16. Norcross WA, Ramirez C, Palinkas LA. The influence of women on the health care-seeking behavior of men. J Fam Pract 1996; 43: 475-480.
- 17. Tudiver F, Talbot Y. Why don’t men seek help? Family physicians’ perspectives on help-seeking behavior in men. J Fam Pract 1999; 48: 47-52.
- 18. Johnston G, Wilkinson D. Increasingly inequitable distribution of general practitioners in Australia, 1986-96. Aust N Z J Public Health 2001; 25: 66-70.
- 19. Warr D, Hillier L. “That’s the problem with living in a small town”: privacy and sexual health issues for young rural people. Aust J Rural Health 1997; 5: 132-139.
- 20. Wenitong M. Indigenous male health: a report for Indigenous males, their families and communities, and those committed to improving Indigenous male health. Canberra: Office of Aboriginal and Torres Strait Islander Affairs, Commonwealth Department of Health and Ageing, 2002.
- 21. Adams M, de Kretser D, Holden C. Male sexual and reproductive health among the Aboriginal and Torres Strait Islander population. Rural Remote Health 2003; 3: 153.
- 22. Gott M, Galena E, Hinchliff S, Elford H. “Opening a can of worms”: GP and practice nurse barriers to talking about sexual health in primary care. Fam Pract 2004; 21: 528-536.





Abstract
Objective: To identify sociodemographic factors associated with help-seeking behaviour for reproductive health disorders in middle-aged and older Australian men.
Design: A cross-sectional, population-based, computer-assisted telephone interview exploring sociodemographic factors and general and reproductive health.
Participants and setting: Analysis of data from the Men in Australia Telephone Survey (MATeS) of 5990 Australian men aged 40 years and older interviewed between September and December 2003.
Main outcome measures: Self-reported diagnosis of prostate disease and erectile dysfunction (ED), help-seeking behaviour (including visiting a doctor, prostate-specific antigen testing, treatment of prostate disease, speaking to a health professional about ED and treatment of ED).
Results: Age was a significant predictor of all help-seeking behaviour studied, other than treatment for ED. Controlling for all predictor variables, never-married status predicted a lower likelihood of visiting a doctor (odds ratio [OR], 0.68 [95% CI, 0.48–0.97]) or speaking to a health professional about ED (OR, 0.44 [95% CI, 0.21–0.93]), while divorced/separated status predicted lower likelihood of having a prostate-specific antigen test (OR, 0.63 [95% CI, 0.50–0.79]). Living in a regional or remote area or being from a non-English-speaking background predicted lower likelihood of receiving treatment for ED (ORs, 0.62 [95% CI, 0.42–0.92] and 0.41 [95% CI, 0.24–0.72], respectively), but did not influence screening for prostate disease.
Conclusion: Seeking advice or treatment for male reproductive health disorders is predicted by sociodemographic factors specific to different reproductive health problems. As middle-aged and older men do attend doctors, opportunities exist for health professionals to optimise their consultations by routinely discussing reproductive health with all men, to identify under-reported male reproductive health disorders.