The increasingly high profile of complementary and alternative therapies is undeniable.1,2 By spending billions on therapies that rarely have strong evidence of efficacy,3 or have been disproven,4 patients clearly are seeking something different to standard medical care, without demanding the kind of information about efficacy and risk now routinely requested of doctors.
There are complex societal factors influencing the use of complementary and alternative therapies.5 Reasons for their popularity include a pragmatic pursuit of better outcomes for chronic health problems,6 which may relate to “effectiveness gaps” in medical care;7 a preference for self-care, and “holistic” or “natural” approaches to health;8,9 and beliefs about disease causation that differ from the medical paradigm.10
The use of complementary and alternative therapies mostly occurs in parallel with medical care.2,11 It can be viewed as a form of health consumerism.12 Health consumerism has interlinked facets, which include a market-based approach promoting individual choice; advocacy for the inclusion of consumer perspectives within health care;13 and formal mechanisms for protecting consumers’ rights.
Increasingly, health consumerism may not just challenge the doctor–patient relationship, but sidestep it altogether. This occurs when medications are sold directly via the Internet, or “natural” health products and do-it-yourself diagnostic kits are bought over the counter or in supermarkets. Many consumers have misplaced expectations about consumer protection mechanisms and assume (wrongly) that these products are independently tested for efficacy before being marketed.2 These developments create new challenges — how is a doctor’s duty of care for his or her patients affected when patients “treat” their health problems outside the medical setting?14
Here, we explore the doctor’s role in the dichotomy between the doctor–patient relationship within standard medical care, and consumers taking non-prescribed complementary or alternative treatments outside the medical setting. We propose the concept of the “therapeutic footprint” in which the balance between potential risks and the evidence supporting a treatment allows standard medical care to be compared with complementary and alternative therapies — approaches that are otherwise “incommensurable”.5
Complementary and alternative therapies include a diversity of practices.15 However, we should not lose sight of the distinction between the concepts “complementary” and “alternative”. The often-used acronym “CAM” (complementary and alternative medicine) obscures important differences between therapies that are complementary to medicine (eg, aromatherapy to lessen discomfort after surgery) and therapies that are used as alternatives or substitutes for medical treatments (eg, a diet recommended as a treatment for cancer instead of undergoing chemotherapy for a chemoresponsive cancer). Ultimately, however, the intention of the provider and/or user of a therapy may determine whether a treatment is complementary or alternative. Alternative therapies that replace conventional medical care, and are promoted as such, present specific risks and problems, which vary according to the health context of the user.
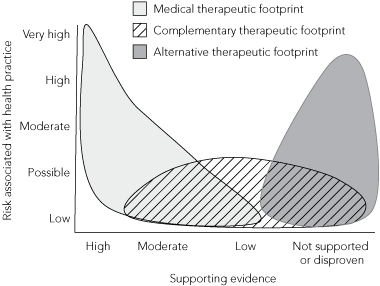
The therapeutic footprint is a conceptual model that “plots” medical therapies and complementary and alternative therapies in relationship to one another and to their levels of risk and supporting evidence. The balance between evidence and risk (Box 1) distinguishes standard medical practice from complementary therapies and even more so from alternative therapies. While risks associated with complementary and alternative therapies may be minimal,16 even a low risk of a severe adverse event is less acceptable if related to a treatment whose benefits are small or unproven.17 The model acknowledges that any discussion of risks of complementary and alternative therapies would be disingenuous without including the hazards associated with standard medical care.
Complementary therapies are frequently “high touch, low tech” (lots of personal contact and little use of high technology products)18 and inherently less risky, as the complementary therapeutic footprint suggests. Nonetheless, ingested products19 and unusual diets have quantifiable potential risks, as do physical therapies like chiropractic or acupuncture. Negative outcomes are generally less frequent and severe than many of those associated with medicine.16 Methodological, economic and cultural issues related to studying complementary therapies mean that, despite investment in research, evidence for the efficacy of complementary therapies will continue to be incomplete.20 Increasingly, however, rigorously generated evidence exists for the efficacy of specific complementary therapies, assisting their integration into standard medical care.21
The alternative therapeutic footprint may be either low risk, or associated with significant risk — especially when therapies are invasive, or preclude proven treatments, like some alternative cancer therapies. Risky alternative therapies are frequently unproven, or disproven,4 but maintain market share because they promise to cure disease. Examination of Internet sites promoting alternative therapies (easily found by searching the Web for “cancer treatments”) reveals common features that magnify risk (Box 2). In our experience, patients consulting alternative practitioners whose practice has these characteristics often tolerate significant physical and financial burden in the hope of relief or cure.
Complementary and alternative therapies respond to consumer demand. When people choose to use these therapies outside a medical setting, their rights and responsibilities are not defined by the doctor–patient relationship, but by protections and safeguards for consumers. They are buying a product, and the only limitation is their capacity to pay. Some health-specific protections exist — for instance, regulation by the Office of Complementary Medicines within the Therapeutic Goods Administration22 — but these barely keep pace with the growth in complementary and alternative therapies. Consumerist mechanisms protect choice, but result in greater risk being borne directly by the consumer. Consumers are protected by a safety net, which mainly comes into effect after a problem has occurred, eg, via complaint mechanisms and product recalls. In contrast, informed consent is proactive — identifying and deciding about the degree of risk or burden patients are likely to encounter or willing to accept if they elect to have a particular treatment. One reason for the success of complementary and alternative therapies is that, because a culture of informed consent is lacking, consumers believe they are inherently safe,18 compared with medicine where risk is appropriately brought to the foreground.
Doctors practising as alternative therapists may have stepped outside their professional boundaries, as their medical status may gain credibility for alternative therapies. Doctors who provide or endorse unproven or unorthodox treatments have the same duties and responsibilities as those in standard medical care,23 and thus consumers harmed by these treatments have more avenues for redress than those treated by non-medical therapists.
However, the push to professionalise specific complementary therapies is likely to redefine practitioners’ responsibilities, creating an ethical context closer to that of medicine in terms of informed consent, provider accountability, and potential for redress if harm results from a treatment.24
The integrative medicine movement argues for complementary therapies to be blended with standard medical care where sufficient evidence exists to support particular practices. Integration further implies that these practices can be incorporated within a professional model of health care, and that usual professional responsibilities would then apply. Boundaries between medicine and complementary therapies are being continually redefined, and the process by which therapies are accepted as part of standard care is subject to debate, particularly regarding what kinds and levels of evidence are acceptable.25
The prevalence of complementary and alternative therapy use presents doctors with significant professional challenges (Box 3). Problems often relate to boundaries between complementary therapies and standard medical care. Discussing these issues with patients can be challenging. However, these conversations provide opportunities to explore patients’ concerns, and discuss and review goals of treatment. This in itself is a valuable outcome with the potential to improve the therapeutic relationship.
1 The “therapeutic footprint”: a theoretical model of standard medical care compared with complementary and alternative therapies
2 Characteristics of alternative therapy practices likely to magnify consumer risks
Focus is on cure — this is regardless of the disease being treated; the therapy may be presented as a universal panacea
Denial of responsibility — promotes treatments in terms of inherent goodness, naturalness or safety without acknowledging any potential for risk or treatment failure. Adverse effects or failure of therapy may be explained as patients’ failure to follow the therapy regimen properly or starting therapy too late
Exclusive relationships — highlights opposition of standard medicine to alternative therapy and discourages use of some or all standard medical care
Exploitative relationships — encourages psychological dependence in treatment users
No objective scrutiny of outcomes — existing evidence about the therapy is discounted and the “medical model” and its basis in scientific knowledge is discredited
3 Doctors’ duty of care towards users of complementary and alternative therapies — four clinical scenarios, related issues and key medical responsibilities
- Christine R Sanderson1
- Bogda Koczwara2
- David C Currow3
- 1 Southern Adelaide Palliative Services, Adelaide, SA.
- 2 Department of Medical Oncology, Flinders Medical Centre, Adelaide, SA.
- 3 Department of Palliative and Supportive Services, Flinders University, Adelaide, SA.
None identified.
- 1. MacLennan AH, Wilson DH, Taylor AW. The escalating cost and prevalence of alternative medicine. Prev Med 2002; 35: 166-173.
- 2. MacLennan AH, Myers SP, Taylor AW. The continuing use of complementary and alternative medicine in South Australia: costs and beliefs in 2004. Med J Aust 2006; 184: 27-31. <MJA full text>
- 3. Cassileth BR, Deng G. Complementary and alternative therapies for cancer. Oncologist 2004; 9: 80-89.
- 4. Vickers A. Alternative cancer cures: “unproven” or “disproven”? CA Cancer J Clin 2004; 54: 110-118.
- 5. Coulter ID, Willis EM. The rise and rise of complementary and alternative medicine: a sociological perspective. Med J Aust 2004; 180: 587-589. <MJA full text>
- 6. Kelner M, Wellman B. Health care and consumer choice: medical and alternative therapies. Soc Sci Med 1997; 45: 203-212.
- 7. Thompson T, Feder G. Complementary therapies and the NHS. BMJ 2005; 331: 856-857.
- 8. Astin JA. Why patients use alternative medicine: results of a national study. JAMA 1998; 279: 1548-1553.
- 9. Siahpush M. Why do people favour alternative medicine? Aust N Z J Public Health 1999; 23: 266-271.
- 10. Yates PM, Beadle G, Clavarino A, et al. Patients with terminal cancer who use alternative therapies: their beliefs and practices. Sociol Health Illn 1993; 15: 199-216.
- 11. Adams J, Sibbritt D, Young AF. Naturopathy/herbalism consultations by mid-aged Australian women who have cancer. Eur J Cancer Care (Engl) 2005; 14: 443-447.
- 12. Lupton D. Consumerism, reflexivity and the medical encounter. Soc Sci Med 1997; 45: 373-381.
- 13. Neuberger J. The educated patient: new challenges for the medical profession. J Intern Med 2000; 247: 6-10.
- 14. Ernst E, Cohen MH, Stone J. Ethical problems arising in evidence based complementary and alternative medicine. J Med Ethics 2004; 30: 156-159.
- 15. National Center for Complementary and Alternative Medicine; National Institutes of Health. What is complementary and alternative medicine? http://nccam.nih.gov/health/whatiscam/ (accessed Jul 2006).
- 16. Myers SP, Cheras PA. The other side of the coin: safety of complementary and alternative medicine. Med J Aust 2004; 181: 222-225. <MJA full text>
- 17. Shekelle PG, Morton SC, Suttorp MJ, et al. Challenges in systematic reviews of complementary and alternative medicine topics. Ann Intern Med 2005; 142 (12 Pt 2): 1042-1047.
- 18. Ernst E. The role of complementary and alternative medicine. BMJ 2000; 321: 1133-1135.
- 19. Huxtable RJ. The myth of beneficent nature: the risks of herbal preparations. Ann Intern Med 1992; 117: 165-166.
- 20. Ernst E. Obstacles to research in complementary and alternative medicine [editorial]. Med J Aust 2003; 179: 279-280. <MJA full text>
- 21. Royal Australian College of General Practitioners; Australasian Integrative Medicine Association. Joint position statement on complementary medicine. 29 September 2004. http://www.aima.net.au/documents/media/RACGP-AIMA%20Position%20Statement%20on%20CM%20May %202005.pdf (accessed Aug 2006).
- 22. Australian Government Department of Health and Ageing. Therapeutic Goods Administration, Office of Complementary Medicines. http://www.tga.gov.au/docs/html/ocmstaff.htm (accessed Jul 2006).
- 23. New South Wales Medical Board. Complementary health care (policy statement). December 2004. http://www.nswmb.org.au/index.pl?page=58 (accessed Aug 2006).
- 24. Cohen MH, Hrbek A, Davis RB, et al. Emerging credentialing practices, malpractice liability policies, and guidelines governing complementary and alternative medical practices and dietary supplement recommendations: a descriptive study of 19 integrative health care centres in the United States. Arch Intern Med 2005; 165: 289-295.
- 25. Park CM. Diversity, the individual, and proof of efficacy: complementary and alternative medicine in medical education. Am J Public Health 2002; 92: 1568-1572.





Abstract
Complex societal factors unrelated to evidence of efficacy influence the increasing use of complementary and alternative therapies, which can be viewed as one form of health consumerism.
The “therapeutic footprint” is a conceptual model that “plots” medical therapies and complementary and alternative therapies in relationship to one another and to their levels of risk and supporting evidence, acknowledging that medical therapies also entail risks.
Philosophies about management of risk and adverse effects differ between complementary and alternative therapies and standard medical care, due to fundamental differences between professionalism within medicine and the demands of health consumerism.
In standard medical care, patients’ risks are mediated prior to treatment via the doctor–patient relationship and informed consent. With complementary and alternative therapies, protection mechanisms for consumers come into effect mainly after a problem has occurred. Understanding this difference helps doctors whose patients are using complementary or alternative therapies to define the boundaries between these therapies and professional medicine and provide appropriate disclosure of risks.
Discussing complementary and alternative therapies and how they differ from standard medical care can provide opportunities to explore patients’ concerns and improve the therapeutic relationship.