Rotavirus gastroenteritis is an important public health problem throughout the world, causing around 500 000 deaths every year.1 In Australia, death is a rare outcome, but rotavirus infections lead to 10 000 hospitalisations annually.2 In Australia’s Northern Territory, hundreds of children have rotavirus gastroenteritis each year, and many are evacuated from remote communities to regional hospitals at significant social and financial cost.3 A rotavirus outbreak in 2001 was a huge burden on Alice Springs Hospital, with, at one time, over 45% of hospital beds occupied by children with gastroenteritis.3,4
Rotavirus has been notifiable to public health authorities in the NT since 1994, and a report on rotavirus epidemiology based on notification data was published in 2001.5
Laboratories have been required to notify rotavirus detection on faecal specimens to the Centre for Disease Control in the NT since 1994, and there has been reliable reporting since 1995.5 Notification data include date of birth, Indigenous status, sex, community of residence, specimen date and type, collection and notification dates, laboratory and diagnostic method. Indigenous status is self-defined by patients or caregivers, and reported to clinical or administrative staff in clinics and hospitals. Notification data are held in the NT Notifiable Diseases System at the Centre for Disease Control.
Rotavirus notifications are periodic, and total numbers are quite variable from year to year, as shown in Box 1. A second-yearly pattern was suggested by increases in rotavirus notifications in 1997, 1999 and 2001, but did not continue in 2003. The total number of notifications in 2004 is the sum of two separate peaks.
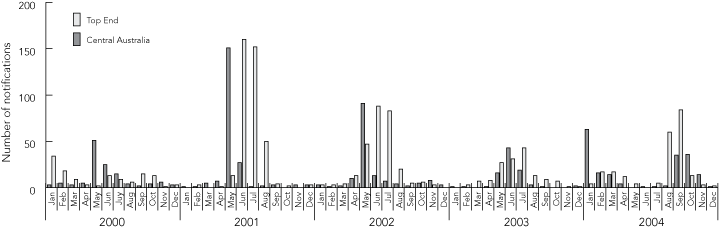
Further breakdown of notifications by month and region for 2000 to 2004 is shown in Box 2. There was no consistent seasonal or regional pattern over 5 years. In most years, peaks of notifications occur in the cooler months of May to August and progress northwards through the NT, from Central Australia to the Top End.
Box 3 shows notification rates per 100 children aged under 5 years per year by Indigenous status, region, and urban or rural place of residence for 1995–2004.
The highest notification rate (Box 3) was among Central Australian urban Indigenous children, and this was significantly higher than the rate among Central Australian rural Indigenous children. The RR for Central Australian urban Indigenous children compared with Central Australian rural Indigenous children was 1.25 (95% CI, 1.09–1.43).
For all of the NT in 1995–2004 (excluding 1997 because of the significant number of notifications involving patients with unknown Indigenous status), the notification rate for Indigenous children was nearly three times that for non-Indigenous children (Box 3). The RR for Indigenous children compared with non-Indigenous children was 2.17 (Box 3).
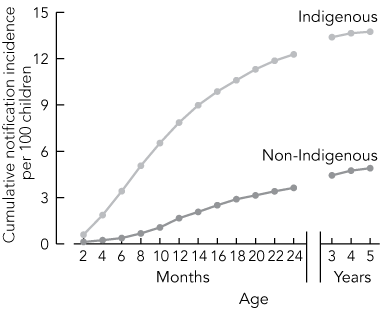
NT-wide data on the cumulative incidence of rotavirus notification to age 5 years in 1995–2004 are shown in Box 4. Infants aged less than 1 year accounted for 56% of notifications (1106/1977; 95% CI, 0.54–0.58) of Indigenous children, and infants aged less than 6 months accounted for 24% (480/1977; 95% CI, 0.22–0.26). The median age of Indigenous people with notified cases of rotavirus was 11 months. Among non-Indigenous people with notified cases of rotavirus, 31% (348/1137; 95% CI, 0.28–0.33) were aged less than a year, and only 7% (78/1137; 95% CI, 0.05–0.08) were aged less than 6 months. The median age for non-Indigenous people with notified cases of rotavirus was 16 months.
As the NT is the only Australian jurisdiction where rotavirus gastroenteritis was notifiable during the study period, comparative data are available only from another NT study for 1995 to mid 2001.6 The RR for rotavirus notification of Indigenous compared with non-Indigenous children over 1995–2004 was 2.17. This is less than the RR of 5–8 reported in 2001 in the other NT study.5 The marked decrease may reflect a true decrease, or be a result of the data cleaning and improved ascertainment of Indigenous status.
The young age of Indigenous children with notified cases of rotavirus in the NT is important because of the greater severity of disease and greater likelihood of hospitalisation of younger children.1 To have greatest impact on reducing infection rates in these children, a vaccine should be effective from before 6 months of age.
Disease notification is limited to cases where the illness is presented to health care facilities, a specimen is collected, the test has adequate sensitivity to detect the infection, the result is positive, and the positive result is forwarded to the public health unit. Collection of stool specimens in primary health care services is not in the standard NT patient management protocol,7 so rotavirus infection may be under-recognised, especially outside hospitals, and notification rates may not be a true indication of disease incidence rates.
Further research is needed to interpret the pattern and rates of notification of rotavirus gastroenteritis in the NT. Since 2005, rotavirus detection by laboratories has been notifiable in Queensland,8 and future work will be able to compare rates in Queensland with those in the NT.
Received 1 February 2006, accepted 27 June 2006
- Rosalie Schultz1
- Department of Health and Community Services, Centre for Disease Control, Alice Springs, NT.
I thank Dr Peter Markey, Head of Surveillance, Centre for Disease Control, Darwin, who assisted with obtaining data on ages of children with notified cases, and Dr Ahmed Latif, who helped with the statistical analysis.
None identified.
- 1. Parashar UD, Hummelman EG, Bresee JS, et al. Global illness and deaths caused by rotavirus disease in children. Emerg Infect Dis 2003; 9: 565-572.
- 2. Carlin JB, Chondros P, Masendycz P, et al. Rotavirus infection and rates of hospitalisation for acute gastroenteritis in young children in Australia, 1993–1996. Med J Aust 1998; 169: 252-256. <MJA full text>
- 3. Williams G, Zerna L. Rotavirus outbreak in central Australia. Aust Infect Control 2002; 7: 51-58.
- 4. Kirkwood C, Bogdanovic-Sakran N, Barnes G, Bishop R. Rotavirus serotype G9P[8] and acute gastroenteritis outbreak in children, Northern Australia. Emerg Infect Dis 2004; 10: 1593-1600.
- 5. Armstrong P. Rotaviral gastroenteritis in the NT: a description of the epidemiology 1995–2001 and future directions for research. NT Dis Control Bull 2001; 8: 1-5.
- 6. Heymann DL, editor. Control of communicable diseases manual. 18th ed. Washington, DC: American Public Health Association, 2004.
- 7. Central Australian Rural Practitioners Association. CARPA standard treatment manual. 4th ed. Alice Springs: CARPA, 2003.
- 8. Queensland Parliamentary Counsel. Queensland Public Health Regulation 2005. Reprinted as in force on 19 May 2006. Reprint No. 1A. http://www.legislation.qld.gov.au/LEGISLTN/CURRENT/P/PubHealR05.pdf (accessed Sep 2006).





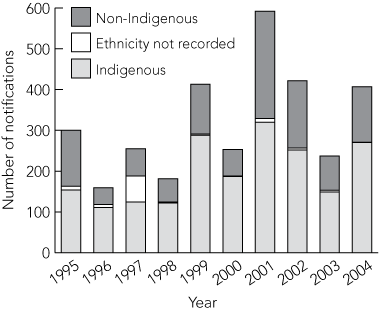
Abstract
Objective: To present data on rotavirus notifications in the Northern Territory to provide knowledge about the local epidemiology of rotavirus gastroenteritis that can be used to inform the use and funding of rotavirus vaccines.
Design: Retrospective analysis of data from the Northern Territory Notifiable Diseases Database.
Participants and setting: Patients with cases of rotavirus infection notified to the NT Centre for Disease Control from 1 January 1995 to 31 December 2004.
Main outcome measures: Patterns of rotavirus notifications over time; infection rates in Indigenous versus non-Indigenous children aged 0–5 years; age groups infected with rotavirus.
Results: Numbers of rotavirus notifications over the period 1995–2004 show annual, monthly and regional variability. The rotavirus notification rate for Indigenous children aged 0–5 years was 2.75 per 100 per year, compared with 0.98 for non-Indigenous children, with a relative risk for Indigenous children of 2.17 (95% CI, 1.97–2.39) over the 10 years. Indigenous children infected with rotavirus were younger than non-Indigenous children, with median ages of 11 months and 16 months, respectively. Rotavirus gastroenteritis occurred in outbreaks, transmitted over months throughout the NT.
Conclusion: Large numbers of cases of rotavirus gastroenteritis affecting Indigenous and non-Indigenous children in the NT are notified every year. The rate in Indigenous children may be decreasing relative to non-Indigenous children. An effective rotavirus vaccine could prevent significant morbidity.