To the Editor: Meningitis is one of the most serious infections in young children. The annual incidence of Haemophilus influenzae type b (Hib) meningitis between 1984 and 1988 was 150 per 100 000 population in Aboriginal children and 27 per 100 000 in non-Aboriginal children younger than 5 years.1 A conjugate Hib vaccination program was introduced in Western Australia in January 1993, before a nationwide program commenced in July 1993. Subsequent marked declines in incidence of Hib meningitis have been reported.2-4 However, there are no recent reports on trends in overall admissions for meningitis.
The WA Data Linkage System (WADLS) encompasses statewide population-based record linkage of the statutory birth and death registers, midwives’ notification system, and hospital morbidity database,5 and is one of few such resources worldwide. As part of a larger study to determine the burden of infection in a cohort of births between 1990 and 2000 using the WADLS, we investigated hospitalisation for all-cause meningitis (International classification of diseases, 9th revision, diagnosis codes 003.21, 036.0, 047, 049.0, 054.72, 320-322) in 17 296 Aboriginal and 252 775 non-Aboriginal children younger than 2 years between 1992 and 2000.
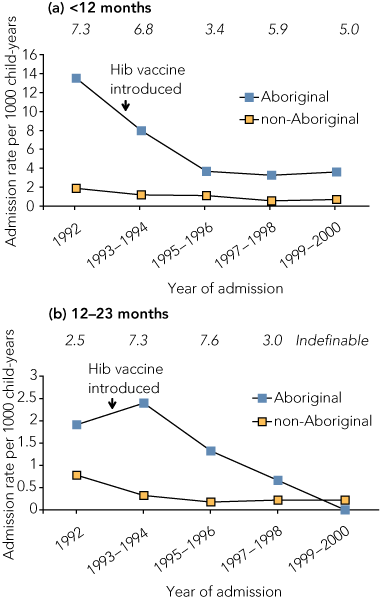
In Aboriginal infants (< 12 months), the meningitis rate fell by 41% between 1992 and 1993–1994 and by a further 54% in 1995–1996, and has remained stable since (Box). In Aboriginal children aged 12–23 months, rates declined by 44% between 1993–1994 and 1995–1996 and again by 50% in 1997–1998, and no meningitis admissions were reported in 1999–2000.
With the decline in meningitis admissions, the disparity between Aboriginal and non-Aboriginal children has narrowed: the relative rate (RR) of Aboriginal to non-Aboriginal meningitis admissions fell from 7.3 in 1992 to 5.0 in 1999–2000 in infants, while in children aged 12–23 months, the RR was > 7.0 in 1993–1996, fell to 3.0 in 1997–1998, and was indefinable in 1999–2000 (Box). In the absence of other relevant interventions, we attribute declines in meningitis admissions to the introduction of Hib vaccine. This is supported by other studies showing a reduction in Hib meningitis following vaccination.2-4
- Hannah C Moore1
- Deborah Lehmann1
- Telethon Institute for Child Health Research, Centre for Child Health Research, University of Western Australia, Perth, WA.
- 1. Hanna JN, Wild BE. Bacterial meningitis in children under five years of age in Western Australia. Med J Aust 1991; 155: 160-164.
- 2. Bower C, Condon R, Payne J, et al. Measuring the impact of conjugate vaccines on invasive Haemophilus influenzae type b infection in Western Australia. Aust N Z J Public Health 1998; 22: 67-72.
- 3. Horby P, Gilmour R, Wang H, et al. Progress towards eliminating Hib in Australia: an evaluation of Haemophilus influenzae type b prevention in Australia, 1 July 1993 to 30 June 2000. Commun Dis Intell 2003; 27: 324-341.
- 4. Brotherton J, McIntyre P, Puech M, et al. Vaccine preventable diseases and vaccination coverage in Australia 2001 to 2002. Commun Dis Intell 2004; 28 Suppl 2: vii-S116.
- 5. Holman CD, Bass AJ, Rouse IL, et al. Population-based linkage of health records in Western Australia: development of a health services research linked database. Aust N Z J Public Health 1999; 23: 453-459.