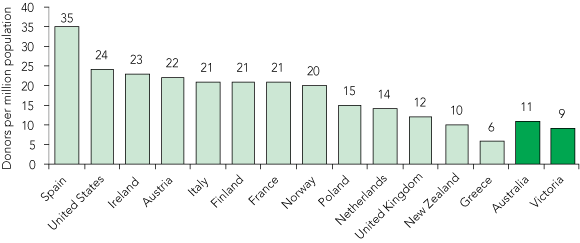
Australia has one of the highest transplantation success rates but a relatively low organ donation rate compared with other developed countries (Box 1).1 In 2004, there were 218 deceased donors, from whom 789 people received a transplant. Many of the 1663 people on the transplant waiting list will have died awaiting a transplant.1
A prospective audit by medical record review was conducted of all hospital deaths from January 2002 until October 2004. The audit included most metropolitan public teaching hospitals and two regional hospitals in the state of Victoria (Box 2).
Each hospital approved the audit as a quality assurance activity.
Apart from living donation of kidneys and, very rarely, liver, solid organ donation is possible only after death has occurred. In Australia, death may be legally declared when there is irreversible cessation of either circulation of blood or all function of the brain. The latter is termed “brain death”, and its certification is a legal requirement if removal of organs for transplantation is to occur while respiration is being maintained artificially. Brain death may be diagnosed by demonstrating absent brain function with clinical brainstem tests (including apnoea) or by demonstrating absent intracranial blood flow using perfusion imaging.4
For the purpose of this audit, potential donors were defined as patients with confirmed brain death, or those who were likely to progress to brain death within 24 hours if supportive treatment continued, and who were medically suitable for organ donation. Medical suitability for organ donation was defined by the guidelines of the Transplantation Society of Australia and New Zealand.5
It was not the role of this audit to determine the potential number of non-heart-beating donors (donation after cardiac death), who currently comprise fewer than 2% of cadaveric donors.1
A: Confirmed brain death through formal clinical brain-death testing or a cerebral angiogram or radionuclide brain scan;
B: Brain death not formally diagnosed, but the patient was likely to have fulfilled criteria for brain death;
C: Potential to progress to brain death within 24 hours if supportive treatment, such as ventilation, had been continued; or
D: Low potential to progress to brain death.
Category A, B and C patients were considered to be unrealised potential donors.
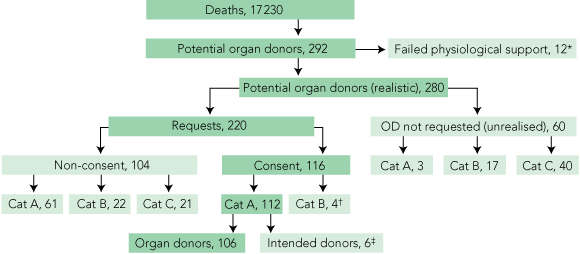
There were 17 230 deaths in the 12 hospitals between January 2002 and October 2004 (Box 3). In Hospital D, data collection was discontinued in mid-2002 after review of 193 deaths, as the hospital denied ongoing access to medical records.
The option of organ donation was discussed with the next-of-kin in 220 cases (Box 3).
Consent for organ donation was given for 116 patients: 112 of these either had confirmed brain death or went on to develop brain death. It is not known whether organ donation was discussed with the next-of-kin before or after the diagnosis of brain death. Of these patients, 106 proceeded to organ donation. There was an unavoidable loss of 10 potential donors (9%) because of failed physiological support, lack of suitable recipients or other medical reasons (Box 3).
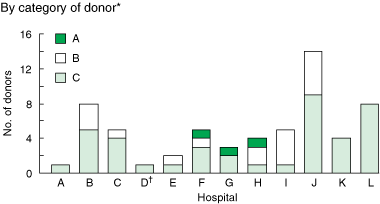
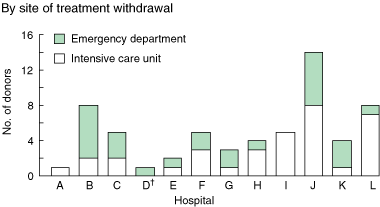
Of the 128 patients reviewed at intensivists’ meetings, 60 were categorised as unrealised potential donors: three as category A (confirmed brain death); 17 as category B (brain death likely but not formally diagnosed); and 40 as category C (potential to progress to brain death within 24 hours if supportive treatment had continued) (Box 3). These unrealised potential donors occurred across all hospitals, and in both intensive care units (ICUs) and emergency departments (EDs) (Box 4).
The three unrealised category A potential donors were from different hospitals (Box 4):
A previously well 57-year-old patient with an intracranial haemorrhage had brain death confirmed in the ED. As no ICU bed was available, and ventilatory support could not be continued in the ED (as it was busy and on bypass, with ambulances being redirected for all but emergencies), the patient was extubated.
A 71-year-old inpatient developed an intracranial haemorrhage after elective surgery, and treatment was withdrawn after diagnosis of brain death. The next-of-kin consented to corneal donation. When later questioned, the treating clinician said he/she did not think of organ donation at the time.
A 51-year-old patient developed brain death 10 days after an intracranial haemorrhage. The next-of-kin had been reluctant to withdraw treatment.
Of the 17 unrealised category B potential donors, six had supportive care withdrawn in the ED (Box 5). They comprised:
two trauma patients (aged 30 and 58 years) with severe bleeding requiring ongoing resuscitation;
a 43-year-old with an intracranial haemorrhage who was a renal transplant recipient; liver donation was not considered; and
three patients (aged 61, 73 and 74 years) with large intracranial haemorrhages and dismal prognoses who had withdrawal of supportive treatment recommended at neurosurgical review; in each case, clinical features within 6 hours of presentation were consistent with brain death, including fixed dilated pupils and absence of spontaneous breathing; there were no contraindications to kidney or liver donation.
The 11 patients who had treatment withdrawn in the ICU comprised:
two children with complex medical histories and prolonged ICU admissions;
a child who required substantial cardiovascular support;
a child whose family’s religious affiliation was incorrectly believed by the intensivist to preclude organ donation;
a 20-year-old with a non-survivable head injury who had treatment withdrawn due to futility; the patient’s identity was undetermined at the time;
a 22-year-old who could not undergo clinical brain death testing because of sedative agents and physiological instability; confirmation of brain death by imaging was not pursued;
two patients (aged 40 and 47 years) with hypoxic–ischaemic brain injuries who had treatment limitations set because of poor prognosis; they subsequently developed features of brain death, and physiological support was not provided;
a 52-year-old tourist from overseas with no immediate family available in Victoria; and
two patients aged in their 70s who had treatment withdrawn after the poor prognosis was conveyed to the families; both may have been suitable liver and kidney donors.
The rates of organ donation that are practically achievable for Victoria can be estimated using the current rate of 9 donors per million population and these audit data. The increase from the current 106 organ donors that would result from increased detection of potential donors and/or an increased rate of consent is shown in Box 6.
The audit detected 280 realistic potential donors and 116 potential donors with next-of-kin consent (consent rate, 53%). There was an unavoidable loss of 10 donors (9%), resulting in 106 organ donors (Box 3).
A maximum practically achievable rate (assuming complete detection and support to brain death of all unrealised potential donors), with a 70% or 80% consent rate, is 15 or 17 donors per million population, respectively (Box 6).
This audit suggests that there is limited but real potential to increase the number of organ donors in Victoria. The practically achievable maximum rate of organ donation for Victoria of 15 to 17 donors per million population is similar to that previously reported in Australia,6,7 but substantially lower than actual organ donation rates achieved in some countries.1 This may be due to a smaller organ donor pool in Victoria, as a result of less road and firearm trauma, and differences in the treatment of hypertension and severe brain injury.8
Increasing the consent rate: The consent rate in this study was 53% to 65%, depending on how broadly the potential organ donor was defined. This is higher than rates reported for the United States (54% for patients with confirmed or suspected brain death)9 and the United Kingdom (59% for patients with confirmed brain death),10 but lower than rates reported in Spain (85%).11
Surveys suggest that public support for organ donation in Australia is as high as 77%.12 However, the support expressed in surveys may be higher than that felt by newly bereaved individuals facing the reality of making the decision on behalf of a family member. Other factors, such as the way in which the option of organ donation is raised with families, may also influence the likelihood of consent. In our study, non-consent was more likely when junior doctors, rather than specialists, discussed organ donation with the family. It is known that family consent is more likely if the approach is made by individuals who are informed about and support organ donation.13,14 Intensive care trainees now receive training on how to identify and care for potential organ donors and how to communicate better with the potential donor’s family.15
Increasing identification of potential donors and requests for organ donation: There were only three patients with confirmed brain death for whom organ donation was not requested. This is fewer than 2% of all patients with confirmed brain death and less than 0.02% of hospital deaths. These rates are very low compared with other published audits.9,10,16,17 Avoiding this most obvious type of “missed donor” requires clinicians to ensure that they always discuss the possibility of organ donation with the family.
It is vital that the discussion of organ donation not precede the family’s understanding and acceptance of a prognosis of death. Recommended practice is that the issue not be raised with the family until after brain death has been diagnosed and explained to them.4 However, the audit data demonstrate that, in many instances, organ donation is discussed with the next-of-kin before brain death is diagnosed. Indeed, for category C patients for whom withdrawal of supportive treatment is being considered, there is no other time to raise the issue. If embarked upon, these discussions should be conducted by skilled staff who are knowledgeable about brain death and organ donation. This would require additional resources in the ICU to provide supportive care for potential donors.
5 Unrealised potential donors classified as category B or C (n = 57)
Possibly/probably brain dead (category B) |
Brain death likely within 24 hours (category C) |
||||||||||||||
Received 22 November 2005, accepted 16 May 2006
- Helen I Opdam1,2
- William Silvester1,2
- 1 Department of Intensive Care, Austin Health, Melbourne, VIC.
- 2 LIFEGift, Victorian Organ Donation Service, Melbourne, VIC.
This study was funded by the Department of Human Services through LIFEGift, the Victorian Organ Donation Service.
None identified.
- 1. Excell L, Russ G, Wride P, editors. Australia and New Zealand Organ Donation Registry report. Adelaide: ANZOD, 2005.
- 2. International Registry Organ Donation and Transplantation. Available at: http://www.tpm.org/registry/reg_mondo.asp (accessed Apr 2006).
- 3. Australian Institute of Health and Welfare. Australian hospital statistics 2003-04. Canberra: AIHW, 2005. (AIHW Cat. No. HSE 37; Health Series No. 23.)
- 4. Australian and New Zealand Intensive Care Society. Recommendations on brain death and organ donation. 2nd ed. Melbourne: ANZICS, 1998.
- 5. Transplantation Society of Australia and New Zealand. Organ allocation protocols. Sydney: TSANZ, 2000. Last update, Aug 2004. Available at: http://www.racp.edu.au/tsanz/oapmain.htm (accessed Jan 2005).
- 6. Hibberd AD, Pearson IY, McCosker CJ, et al. Potential for cadaveric organ retrieval in New South Wales. BMJ 1992; 304: 1339-1343.
- 7. Opdam HI, Silvester W. Identifying the potential organ donor: an audit of hospital deaths. Intensive Care Med 2004; 30: 1390-1397.
- 8. Australian Transport Safety Bureau. Transport accident fatalities: Australia compared with other OECD countries, 1980-1999. Available at: http://www.atsb.gov.au/publications/2004/Int_Comp_5.aspx (accessed May 2006).
- 9. Sheehy E, Conrad SL, Brigham LE, et al. Estimating the number of potential organ donors in the United States. N Engl J Med 2003; 349: 667-674.
- 10. Barber K, Falvey S, Hamilton C, et al. Potential for organ donation in the United Kingdom: audit of intensive care records. BMJ 2006; 332: 1124-1127.
- 11. Miranda B, Vilardell J, Grinyo JM. Optimizing cadaveric organ procurement: the Catalan and Spanish experience. Am J Transplantation 2003; 3: 1189-1196.
- 12. Pfizer Australia. Health report, 23 August 2004. Australians accept animal organ transplants but under-informed. Available at: http://www.pfizer.com.au/Media/Transplants.aspx (accessed Mar 2005).
- 13. Siminoff LA, Gordon N, Hewlett J, et al. Factors influencing families’ consent for donation of solid organs for transplantation. JAMA 2001; 286: 71-77.
- 14. Gortmaker SL, Beasley CL, Sheehy E, et al. Improving the request process to increase family consent for organ donation. J Transpl Coord 1998; 8: 210-217.
- 15. Gillott J, Berriman M. ADAPT. Australasian Donor Awareness Programme: final report for the Australian Government Department of Health and Ageing. Financial year 2004–2005. Canberra: Department of Health and Ageing, 2005.
- 16. Siminoff LA, Arnold RM, Caplan AL, et al. Public policy governing organ and tissue procurement in the United States. Results from the National Organ and Tissue Procurement Study. Ann Intern Med 1995; 123: 10-17.
- 17. Gore SM, Cable DJ, Holland AJ. Organ donation from intensive care units in England and Wales: two year confidential audit of deaths in intensive care. BMJ 1992; 304: 349-355.





Abstract
Objective: To determine the potential for organ donation in 12 Victorian hospitals.
Design and setting: Prospective audit of all deaths in 12 major public hospitals in the state of Victoria between January 2002 and October 2004.
Main outcome measures: Number of organ donors and potential organ donors (patients with brain death or likely to progress to brain death within 24 hours if supportive treatment continued), requests for organ donation and consents. Unrealised potential donors (organ donation not requested) were categorised by an independent panel of intensivists as category A (brain death formally diagnosed); B (brain death not formally diagnosed but criteria likely to be fulfilled); and C (potential to progress to brain death within 24 hours).
Results: There were 17 230 deaths, 280 potential organ donors and 220 requests for organ donation. The 60 unrealised potential organ donors were classified as category A (3), B (17) and C (40). Consent rate was 53% to 65%, depending on the definition of potential donor (categories A, B and C or category A only). Consent rate was lower when discussions about organ donation were held by trainees or registrars (21%) than when specialists were present (57%) (P = 0.004). A maximum practically achievable organ donation rate for Victoria was estimated to be 15 to 17 donors per million population (current rate, 9 per million population).
Conclusions: The potential for organ donation in Victoria is limited by a small organ donor pool. There is potential to increase the number of organ donors by increasing the consent rate (lower than expected from public surveys), the identification of potential organ donors (particularly those likely to progress to brain death if supportive treatment is continued), and requests for organ donation.