Critics of medical negligence litigation frequently decry its excesses. However, medicolegal research into the relationship between iatrogenic injury, negligence, and litigation highlights a serious problem of a different kind: the vast majority of patients who sustain injury due to negligent medical care never sue,1-3 and certain subgroups of injured patients — primarily, patients who are elderly, poor, and uninsured — are especially unlikely to seek damages.3,4 The reasons for this “underclaiming” phenomenon are unclear. One commonly cited explanation is that, in negligence-based systems, patients who desire compensation confront a variety of barriers, including difficulties finding or paying for legal representation, time costs associated with litigation, and secrecy among providers about errors and their consequences.5
The prospect of fewer such barriers, and better linkage of compensation to injuries, has fuelled interest in alternative approaches to medical injury compensation.6,7 Commentators in Australia,8,9 the United States,6,7,10 including the Institute of Medicine,11 and the United Kingdom12 have eyed New Zealand’s no-fault system of compensation13 as a promising alternative. In Australia, a major review of medical indemnity arrangements in the mid 1990s rejected the no-fault model;14 a more recent review of the law of negligence noted that a significant body of opinion supports implementation of such a system, but made no recommendation.15
Baseline data on a random sample of patients who had experienced adverse events came from the NZQHS. As previously described,16 NZQHS used a two-stage sampling process to develop a representative sample of 6579 medical records of patients discharged from publicly funded acute care hospitals in 1998, excluding psychiatric and same-day discharges. Trained reviewers assessed each case for the presence of an adverse event. Following previous research in the US,17,18 Australia,19 and NZ,16 adverse events were defined as an unintended injury caused by health care management, rather than the underlying disease process, that resulted in disability.
The compensation criteria have changed over time. Between 1992 and 2005, injuries were compensable if they met either of two criteria:13,20 (i) a “medical mishap”, defined as a consequence of treatment properly given that is rare (occurring in no more than 1% of cases) and severe (hospitalisation for more than 14 days, significant disability lasting more than 28 days, or death); or (ii) “medical error”, defined as a failure to provide treatment with reasonable care and skill. On 1 July 2005, “medical mishap” and “medical error” were replaced with a new concept of “treatment injury”.21,22 This change broadened coverage to include all personal injuries sustained while receiving treatment from health professionals. Our study was conducted before the legislative change, and compensability determinations focused on the mishap/error criteria.
Claims relating to episodes of care in 1998 may have been (or might be) filed later than 30 June 2004, the date the claims data were extracted, although this is unlikely. Virtually all claims are filed within 2 years of the date of the alleged injury, and the adjudication time frame averages 6 months,23 with a statutory time limit of 9 months. Therefore, the 5.5-year claiming window we allowed is conservative.
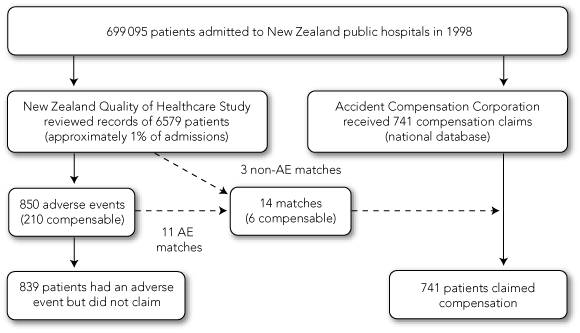
The analyses are descriptive. We compared characteristics of patients who filed a claim for compensation (“claimants”) with characteristics of patients from the NZQHS who experienced an adverse event and did not claim (“non-claimants”). The overlapping or “match” patients — that is, patients from the NZQHS sample whose care involved an adverse event and who subsequently claimed compensation for that event — were classified as claimants. Box 1 shows the derivation of the two populations.
A determination of “compensability” was available within both the NZQHS and the ACC data. For each adverse event identified in NZQHS, reviewers had judged whether it met the statutory criteria for compensation. Among claims, compensable events were those so judged by the ACC. A pilot study established good inter-rater reliability between NZQHS and ACC determinations of compensability (κ, 0.66).24
Data were analysed using the SAS statistical software package, version 9.0 (SAS Institute Inc, Cary, NC, USA), and Stata, version 8.0/SE (Stata Corp, College Station, Tex, USA). We used t tests and χ2 tests to conduct bivariate comparisons of characteristics of the claimant and non-claimant groups. We investigated predictors of failure to claim despite having experienced an adverse event using multivariate logistic regression. The dependent variable in the regression analysis distinguished claimants from non-claimants. The independent variables were sex, ethnicity (Māori;, Pacific, non-Māori;/non-Pacific), patient age (< 1 year, 1–17 years, 18–44 years, 45–64 years, and ≥ 65 years), disability (temporary, permanent with < 50% impairment, permanent with > 50% impairment, death), and whether or not the event was compensable. An additional covariate provided a measure of the patient’s socioeconomic status using the NZ Index of Deprivation Score.25,26 This index, based on small area mesh blocks (a micro-level breakdown of geographic boundaries), combines nine census variables reflecting aspects of material and social deprivation; as has been done previously,27 index scores were separated into quintiles for analysis.
To account for the stratified two-stage cluster sampling design in the NZQHS,28 the bivariate and multivariate analyses were weighted. Weighting made little difference to the estimates.
As previously reported, NZQHS investigators’ review of 6579 admissions identified 850 adverse events;16 210 of these were judged to be compensable under the statutory standard (Box 1). This corresponds to a rate of 3.2 compensable adverse events per 100 admissions under NZ’s no-fault standard, which is about three times greater than the frequency of compensable events previously detected in the US using the negligence standard (Box 2).
There were 14 matches between the NZQHS and claims populations. NZQHS reviewers had judged six of these to be compensable adverse events, which suggests that 2.9% (6/210) of compensable adverse events led to claims. In Box 2 the claiming rate among compensable adverse events in NZ is compared with corresponding rates from malpractice systems in New York and Utah/Colorado. Among the rest of the matches, five were judged by NZQHS reviewers to be adverse events that did not meet the compensation criteria, and three were judged not to be adverse events.
Box 3 gives baseline measures of patient characteristics from the NZQHS’s representative sample, and then compares characteristics of claimants and non-claimants who experienced adverse events. Compared with claimants, non-claimants were significantly older (mean age, 52 v 42 years; P < 0.001), more likely to be male (45% v 39%; P = 0.02), and more likely to be of Māori; or Pacific ethnicity (16% v 9% and 4% v 2%; P < 0.001). Non-claimants were also more likely to live in the most socioeconomically deprived areas (27% v 18%; P < 0.001). Claimants, on the other hand, were more likely to have sustained injuries that led to permanent disability, and a significantly larger proportion of their injuries were compensable (46% v 24%; P < 0.001).
These bivariate differences persisted in multivariate analyses of the claimants and non-claimants (Box 4). Claiming propensity decreased with deprivation: the odds of claiming among injured patients in the most deprived quintile were a third the odds of claiming among injured patients in the most privileged quintile (odds ratio [OR], 0.36; 95% CI, 0.23–0.57). Elderly patients were significantly under-represented among claimants (OR, 0.20; 95% CI, 0.14–0.29), as were patients of Māori; and Pacific ethnicity (OR for Māori;, 0.47; 95% CI, 0.32–0.69; OR for Pacific peoples, 0.26; 95% CI, 0.12–0.58). The model controlled for disability and eligibility for compensation, both of which were significant predictors of claiming (OR for permanent disability > 50% impairment, 5.2; 95% CI, 2.9–9.3; OR for compensable event, 2.8; 95% CI, 2.1–3.8).
Both the ACC and NZQHS data we used have some limitations. Ethnicity is missing for 119 patients (or 7.5% of the study sample), and misclassification is a well-recognised problem with data of this type.29 The NZ Index of Deprivation’s use of small area-based measures to assign socioeconomic characteristics at the individual level creates the potential for measurement error.26 The direction and magnitude of the impact of these data limitations on our findings are unknown, but we know of no reason why they would differ systematically between claimants and non-claimants, and thus affect the main results of our analyses.
The claiming rate we estimated is consistent with Davis and colleagues’ crude estimate (based on adverse event and claims data from one region of NZ) that compensable events outstrip claims in NZ by a factor of 30 to one.24 It is also consistent with the estimated claiming rate of 3.6% obtained by using all claims as the numerator and an extrapolation of compensable event rates to the national level as the denominator (749/21 000).
Our findings do not suggest that a considerably larger proportion of injured patients who are eligible for compensation will actually obtain it in a medicolegal environment like NZ’s, where negligence has been eliminated as the basis of determining eligibility for injury compensation. As in the US, patients who sustained injuries were much more likely to claim compensation than uninjured patients. But despite few apparent barriers to seeking compensation in NZ — for example, lawyers are not necessary and few claimants use them — the vast majority of eligible patients (97%) did not claim. The proportion that did claim was very close to the proportion estimated from tort systems in New York in the late 1980s2 and Utah and Colorado in the late 1990s.3
Our findings are also consistent with estimates from Denmark, another country with a comprehensive no-fault system. A recent review of 1573 patient records from a surgery department in Copenhagen found only two no-fault compensation claims among 209 potentially compensable events.30 The problem of chronic underclaiming appears to be quite insensitive to the structure of the compensation system.
One hope for efforts to promote disclosure of medical injuries is that greater transparency may attenuate this identification problem. In theory, the blame-free atmosphere of a no-fault environment is better placed to realise this goal. In practice, NZ’s continued use of medical error as one of the bases of eligibility for compensation has meant its scheme has retained some of the fault and blame elements that characterise tort systems. These vestiges have almost certainly inhibited disclosure.31 The recent changes to the scheme, replacing “medical mishap” and “medical error” with “treatment injury” are explicitly designed to eliminate fault-finding from the compensation inquiry, promote disclosure, and reinforce the system’s no-fault mission.23
Second, injured patients and their families have many interests besides money,32,33 though it is essentially the only remedy available in a tort system. The NZ system offers monetary compensation for economic losses, and offers alternative processes for responding to patients’ other needs. Patients who seek an apology, an explanation, or system change to protect others from similar harm can have those interests met by using free, independent advocacy services or filing a complaint with the national Health and Disability Commissioner.34
Non-economic damages are not compensated. Older patients and people representing children may be discouraged from claiming because significant earnings-related compensation is not available to them.24 A disproportionate degree of underclaiming among those groups is consistent with the results of our comparisons of non-claimants with claimants.
Our findings related to social deprivation are consistent with previous research.3,4,35,36 Burstin and colleagues found that poor, elderly and uninsured patients in New York were significantly less likely to sue for malpractice, even after controlling for the presence of medical injury.4 Similarly, Studdert and colleagues’ analysis of adverse events and lawsuits in Utah and Colorado found that sociodemographic risk factors for being members of the “worthy but uncompensated” group included being poor, uninsured, a Medicare or Medicaid beneficiary, and 75 years of age or older.3
Māori; have special status in NZ, as the indigenous people and partners to the Treaty of Waitangi. Like many indigenous populations who have been colonised, they are disadvantaged across a spectrum of indicators including education, health, and justice — even after adjusting for socioeconomic status.29 In our study, patients of Māori; and Pacific ethnicity were significantly less likely to claim after injuries. Further research is required to investigate the cause of these disparities. However, more widespread adoption of culturally safe practices, including the use of appropriate language, respect for custom, the use of culturally validated outcome measures, and the employment of Māori; and Pacific staff37 may help to overcome these disparities.
How the country’s recent shift towards a more permissive compensation standard will affect the low claiming rates and the disparities we observed is unclear. Patients’ general awareness of opportunities for compensation may increase, as may transparency about medical injuries among clinicians, with overtones of error and fault removed from the compensation determination. All else being equal, both of these changes would tend to boost claiming rates among eligible patients. However, the shift to a treatment injury standard also enlarges the pool of eligible patients, perhaps threefold.24 The relative size of these changes, combined with others we have not considered, will determine the ultimate impact of the new compensation standard on claiming rates.
2 Frequency of compensable events and claims after adverse events in New Zealand, and in New York and Utah/Colorado, USA
Probability of a claim following a compensable adverse event |
|||||||||||||||
3 Characteristics of patients in New Zealand Quality in Healthcare Study (NZQHS), injured non-claimants in NZQHS, and claimants with the Accident Compensation Corporation (ACC)
* P values were calculated for the difference between claimants and non-claimants using t tests and χ2 tests as appropriate. Calculations were weighted to account for NZQHS sampling methodology.
† Percentages were calculated using the available data as denominators. Ethnicity data were missing for 19 non-claimants (2.3%) and 100 claimants (13.5%); deprivation scores were missing for 7 non-claimants (0.8%) and 88 claimants (11.9%); disability severity was missing for 40 non-claimants (4.8%) and 165 claimants (22.3%).
- Marie M Bismark1,3
- Troyen A Brennan1
- Peter B Davis2
- David M Studdert1
- 1 Department of Health Policy and Management, Harvard School of Public Health, Boston, Mass, United States.
- 2 Department of Sociology, University of Auckland, Auckland, New Zealand.
- 3 Health Law, Buddle Findlay, Wellington, New Zealand.
We thank Jean-Marie Berthelot and Roy Lay-Yee for their expert statistical assistance. Elana Curtis offered valuable comments. Funding for this study was provided by the Commonwealth Fund, an independent non-profit organisation based in New York City. Our work was independent of the funders.
None identified.
- 1. Danzon P. Medical malpractice theory, evidence and public policy. Cambridge, Mass: Harvard University Press, 1985.
- 2. Localio AR, Lawthers AG, Brennan TA, et al. Relation between malpractice claims and adverse events due to negligence. Results of the Harvard Medical Practice Study III. N Engl J Med 1991; 325: 245-251.
- 3. Studdert DM, Thomas EJ, Burstin HR, et al. Negligent care and malpractice claiming behaviour in Utah and Colorado. Med Care 2000; 38: 250-260.
- 4. Burstin HR, Johnson WG, Lipsitz SR, Brennan TA. Do the poor sue more? A case-control study of malpractice claims and socioeconomic status. JAMA 1993; 270: 1697-1701.
- 5. Weiler PC. Medical malpractice on trial. Cambridge, Mass: Harvard University Press, 1991.
- 6. Bovbjerg RR, Sloan FA. No-fault for medical injury: theory and evidence. Univ Cincinnati Law Rev 1998; 67: 53-123.
- 7. Weiler PC. The case for no-fault liability. MD Law Rev 1993; 52: 908.
- 8. Luntz H. Reform of the law of negligence: wrong questions — wrong answers. Univ N S W Law J 2002; 25: 836-841.
- 9. Sappideen C. No fault compensation for medical misadventure — Australian expression of interest. J Contemp Health Law Policy 1993; 9: 311-322.
- 10. Studdert DM, Brennan TA. No-fault compensation for medical injuries: the prospect for error prevention. JAMA 2001; 286: 217-223.
- 11. Corrigan JM, Greiner A, Erickson SM, editors. Fostering rapid advances in health care. Learning from system demonstrations. Washington, DC: Board on Health Care Services; Institute of Medicine, National Academies of Sciences, 2002.
- 12. British Medical Association. Report of the working party on no fault compensation. London: BMA, 1991.
- 13. New Zealand Legislation. Injury Prevention, Rehabilitation and Compensation Act, 2001.
- 14. Tito F. Compensation and professional indemnity in health care — final report. Review of professional indemnity arrangements for healthcare professionals. Canberra: AGPS, 1996.
- 15. Commonwealth of Australia. Review of the Law of Negligence. Final report. 2002. http://revofneg.treasury.gov.au/content/Report2/PDF/Law_Neg_Final.pdf (accessed Jan 2006).
- 16. Davis P, Lay-Yee R, Briant R, et al. Adverse events in New Zealand public hospitals. I: occurrence and impact. N Z Med J 2002; 115 (1167): U271. http://www.nzma.org.nz/journal/115-1167/271/ (accessed Jul 2006).
- 17. Brennan TA, Leape LL, Laird NM, et al. Incidence of adverse events and negligence in hospitalised patients. Results of the Harvard Medical Practice Study 1. N Engl J Med 1991; 324: 370-376.
- 18. Thomas EJ, Studdert DM, Burstin HR, et al. Incidence and types of adverse events and negligent care in Utah and Colorado. Med Care 2000; 38: 261-271.
- 19. Wilson R, Runciman W, Gibberd R, et al. The Quality in Australian Health Care study. Med J Aust 1995; 163: 458-471. <eMJA pdf>
- 20. New Zealand Legislation. Accident Rehabilitation and Compensation Insurance Act, 1992.
- 21. New Zealand Legislation. Injury Prevention, Rehabilitation, and Compensation Amendment Act (No. 2), 2005.
- 22. Bismark MM, Paterson RJ. No-fault compensation in New Zealand: harmonizing injury compensation, provider accountability, and patient safety. Health Aff (Millwood) 2006; 25: 278-283.
- 23. Braddell R. No-fault medical misadventure law ends finger-pointing [letter]. N Z Med J 2005; 118: U1516. http://www.nzma.org.nz/journal/118-1216/1516/ (accessed Jul 2006).
- 24. Davis PB, Lay-Yee R, Fitzjohn J, et al. Compensation for medical injury in New Zealand: does “no-fault” increase the level of claims making and reduce social and clinical selectivity? J Health Polit Policy Law 2002; 27: 833-854.
- 25. Salmond C, Crampton P, Sutton F. NZDep 96 Index of Deprivation. Research Report No. 8. Wellington: Health Services Research Centre, 1998.
- 26. Salmond C, Crampton P. NZDep2001 Index of Deprivation. Wellington: Department of Public Health. Wellington School of Medicine and Health Services, 2002. http://www.moh.govt.nz/PHI/Publications (accessed Jul 3006).
- 27. Blakely T, Pearce N. Socio-economic position is more than just NZDep. N Z Med J 2002; 115: 109-111.
- 28. Davis PB, Lay-Yee R, Briant R, et al. Adverse events in New Zealand public hospitals: principal findings from a national survey. Wellington: Ministry of Health, 2001.
- 29. Robson B, Reid P. Ethnicity matters: Maori perspectives. Wellington: Statistics New Zealand, 2001.
- 30. Christoffersen JK, Holm-Nielsen A. [The pattern of treatment injuries and near misses in a surgery department. A review of a 1-year material] [Danish]. Ugeskr Laeger 2004; 166: 1760-1763.
- 31. Fitzjohn J, Studdert DM. A compensation perspective on error prevention: is the ACC medical misadventure scheme compensating the right sort of injury? N Z Med J 2001; 114: 432-434.
- 32. Hickson GB, Clayton EW, Githens PB, Sloan FA. Factors that prompted families to file medical malpractice claims following perinatal injuries. JAMA 1992; 267: 1359-1363.
- 33. Vincent C, Young M, Phillips A. Why do people sue doctors? A study of patients and relatives taking legal action. Lancet 1994; 343: 1609-1613.
- 34. Paterson R. The patients’ complaints system in New Zealand. Health Aff (Millwood) 2002; 21: 70-79.
- 35. May ML, Stengel DB. Who sues their doctors? How patients handle medical grievances. Law Soc Rev 1990; 24: 105-120.
- 36. Sager M, Voeks S, Drinka P, et al. Do the elderly sue physicians? Arch Intern Med 1990; 150: 1091-1093.
- 37. Durie M. Providing health services to indigenous peoples. BMJ 2003; 327: 408-409.





Abstract
Objectives: (i) To determine the proportion of patients in New Zealand who claim compensation from the national no-fault compensation program after experiencing a compensable injury; and (ii) to identify characteristics of injured patients who are least likely to claim despite having sustained a compensable injury.
Design: We estimated the percentage of eligible patients who claim no-fault compensation by linking a national claims database (Accident Compensation Corporation) to records reviewed in the New Zealand Quality of Healthcare Study (NZQHS). Bivariate and multivariate analyses were used to investigate socioeconomic and sociodemographic differences between claimants and injured non-claimants.
Participants and setting: Patients who experienced an adverse event associated with care in NZ public hospitals in 1998 and claimed compensation with the ACC, the national no-fault insurer (n = 741). Patients identified by the NZQHS as having sustained an adverse event associated with hospital care in the same year who did not file a compensation claim (n = 839).
Main outcome measures: Adverse events, compensable adverse events, and compensation claims.
Results: Among patients judged by NZQHS reviewers to be eligible for compensation, 2.9% (6/210) claimed. Odds of claiming after an adverse event were significantly lower for patients who were elderly (odds ratio [OR], 0.20; 95% CI, 0.14–0.28), from the most deprived areas (OR, 0.36; 95% CI, 0.23–0.57), or of Māori; or Pacific ethnicity (OR, 0.47; 95% CI, 0.32–0.69 and OR, 0.26, 95% CI, 0.11–0.58).
Conclusions: Despite few apparent institutional or economic barriers, the proportion of injured patients in NZ who seek compensation after sustaining a compensable injury is very low. Hence, substantial underclaiming occurs in both negligence and no-fault systems. The disproportionately low propensity of elderly, poor and minority patients to seek compensation also appears to be pervasive.