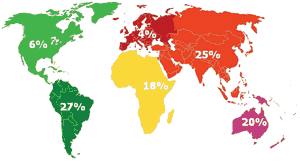
Medical education in Maastricht is practice-oriented. The Faculty of Medicine (Box 1) provides training in all fields of medicine, as well as the initial phase of training for medical research. Maastricht University supports an international orientation, and medical students are encouraged to spend at least one term of their medical course abroad. Most students choose an elective in PHC, and in this quest are encouraged and supervised by the PHC working group of the Department of General Practice at Maastricht Medical School. This group aims to introduce students to patient care, research and education in PHC settings outside the Netherlands. From an active participation in PHC and doing small-scale research, students learn how to deal with limited resources and how to assess socioeconomic and cultural relationships with, and determinants of, health. The philosophy of the group is described in Box 2. During the past 10 years, collaboration with elective sites on all continents has been established (Box 3). One in five students seeking to pursue a PHC elective does so in Australia. All sites within one country or part of a continent are typically coordinated and supervised by one member of the PHC working group, which is responsible for about 30% of all electives abroad by Maastricht medical students.
In the past 5 years, 42 senior medical students (10 men, 32 women) have pursued a PHC elective in Australia. Doctors and coordinators in Broken Hill, Collarenebri, Menindee and Wilcannia in New South Wales; Cherbourg, Gympie, Murgon, Mount Isa and Theodore in Queensland; Carnarvon, Katanning and Kununurra in Western Australia; Mannum in South Australia (Box 4), and Melbourne in Victoria agreed to supervise students during this time. In most cases, initial contacts led to further student placements.
Rural areas are different from metropolitan areas, sociologically, culturally, spiritually, and, not surprisingly, in terms of general practice activity. But there are additional explicit reasons why students are motivated to pursue an elective in rural Australia:
A medical elective in Australia offers the student an English-speaking environment. Dutch students are at ease with medical English, as parts of the Maastricht curriculum are in English and most medical literature is in English.
Medical studies in the Netherlands and Australia have similarities that make it easier to fit in when starting an elective. The two countries are well known for their innovative approach to medical education. For example, Maastricht University and the University of Newcastle (NSW) were among the first medical faculties to develop and adapt the system of problem-based learning, pioneered at McMaster University in Canada.
The students and their supervisors know what to expect, as final-year Dutch medical students have the same level of clinical knowledge and training as their Australian counterparts. On the other hand, the geographic environment may be quite different. With a population density of 423 people per square kilometre, the Netherlands ranks among the most densely populated countries in the world. In contrast, Australia has 2.4 people per square kilometre. As nearly every Dutch citizen lives within 20 km of the nearest city with extensive medical facilities, rural areas in that sense are absent.
Working in a rural setting has several distinct advantages for doctors-to-be. First, they learn how to cope in a situation with limited resources. Australian rural clinics are relatively well equipped, but simple referral is often not possible because of remoteness. Secondly, although students gain experience in all the different specialties during their 2-year rotations in the Netherlands, including their regular 10-week rotation in general practice, the overseas elective is the only remaining opportunity to practise medicine in a broad sense. These facts motivate students to take up an elective in rural Australia. Thirdly, in rural health, general practitioners are often also doctors at the local hospital, and the more remote the area, the more likely a GP is to be regularly engaged in complex and procedural care. In the Dutch health care system, there is a distinct separation between care provided by GPs and hospital care. Thus, general practice in rural Australia offers a wider scale of medical exposure. As a result, students can enhance their practical skills, like suturing (Box 5), taking blood samples, and applying plaster bandages, under the supervision of GPs. This hands-on approach is highly appreciated by students.
Good rural placements for Australian students are scarce, and naturally we do not want to interfere with these arrangements. By sending only a very limited number of students (maximum of 10 nationwide) per year, we avoid competing for placements with Australian medical schools. The University of Sydney Department of Rural Health in Broken Hill has been an excellent partner. Despite increasing numbers of Australian students, they have been able to continue offering some placements to international students. Even so, our students have often worked together with their Australian colleagues, which was welcomed from both sides (Box 6).
- Jochen Cals1
- Peter Joyner2
- Robert J Tuffley3
- Geert-Jan Dinant1
- 1 Department of General Practice, Maastricht University, Maastricht, The Netherlands.
- 2 Mannum Medical Centre, Mannum, SA.
- 3 The Gympie Clinic, Gympie, QLD.
The authors and the PHC working group would like to thank all Australian clinics, doctors, health workers and nurses who have contributed to the excellent learning and personal experiences of our students. Furthermore, we are very grateful for the cooperation of Marion Aarts and Astrid Peters of the Office of International Relations of Maastricht University.
None identified.







Abstract
The Primary Health Care (PHC) working group of the Department of General Practice of Maastricht University in the Netherlands was founded in 1998 specifically to introduce students to patient care, research and education in primary health care settings outside the Netherlands.
Rural health care in Australia is appealing to international medical students because of its unique setting.
In the past 5 years, 42 medical students from Maastricht University have pursued a medical elective in rural Australia, supervised by the PHC working group.
Doctors and coordinators in primary care clinics across Australia have welcomed and supervised students from Maastricht and exposed them to the reality of rural health care.
Future collaboration with other Australian primary care clinics is welcomed.