But what is happening, and, more importantly, why?
The clinical disciplines emerged in the late 17th and 18th centuries as discrete crafts, often in direct competition with each other — even as late as 1880, doctors regarded nurses as a threat to their professional sovereignty.1 Consequently, to ease potential conflict, roles and accountabilities were precisely defined. This unambiguous scope of practice was mostly effective at the time. It enabled different disciplines to get along and perform as a team in specific situations, and it promoted some — if begrudging — measure of interdisciplinary respect. Acute care teams were able to undertake ward rounds, conduct operations, and care for patients successfully in hospitals. What has gone wrong since then?
The ageing of the population, with increased comorbidity and the burgeoning increase in chronic disease, underscores the crisis. Diabetes will be the second most common condition affecting males by 2016.2 We are ill-prepared for the onslaught of increasing clinical care needed by patients with chronic degenerative diseases and other demands.
Simultaneously, the supply side is declining for a variety of reasons: insufficient health students to keep pace with population growth; feminisation of the workforce; increasing medical technology sometimes, perversely, requiring more personnel; retirement patterns;3 and the changing aspirations of “Generation Y”, which admires commitment to balancing lifestyle and family over duty to one’s profession.
Although the clinical landscape is changing rapidly, the primary structure of the health workforce remains the same, despite entreaty from many to rethink the traditional barriers between professions and consider developing new professions.4 There is some blurring at the margins of medical and nursing roles, but disciplinary “silos” remain entrenched, each profession defending its walls against what is seen as loss of disciplinary sovereignty. This has been a feature of the health system from early on (for example, in 1871, doctors of the failing Sydney Hospital charged the newly established nursing profession in Australia with incompetence, blaming them for the crisis; the nurses were exonerated by a New South Wales Government inquiry).5 Unease between the health professions is not yet completely resolved, and this territorialism threatens teamwork.
The contribution of older and newer disciplines is not at issue. Indeed, there is a generally favourable verdict.6 Yet, to the average patient, some of the professional fragmentation is arcane and subtle far beyond intuition. Few lay people can easily explain the difference in contributions between chiropractor and osteopath, or physiotherapist and occupational therapist. Rather, multidisciplinary teamwork is more important than ever, and no one clinical discipline, let alone one clinician, can ever over a short time hope to look after all the complexities of a single patient’s needs, except for a very narrow range of problems.
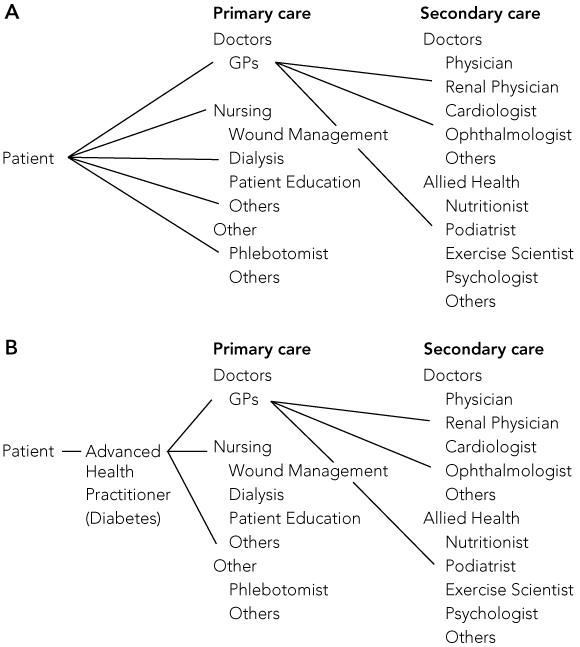
Pity the person with diabetes, who confronts a logistical hurdle in setting out to access each professional necessary for his or her health care (Box): multiple appointments, travel, time and organisation. Health managers, too, face serious challenges in providing the necessary fragments in one time and place, avoiding missing any fragments and ensuring adequate interprofessional communication.
Conventional conservative managements have all failed.7 A new approach is indicated, pragmatic in application and systemic in reach.
The current approach is simply to demand more: more doctors, more nurses, and more allied health workers. By itself, this strategy cannot succeed.8 In the short term, we cannot train enough doctors, particularly general practitioners, let alone nurses.9 The geometrically expanding health needs of our growing and ageing community are outstripping the arithmetically increasing production of health professionals.
We need fundamental workforce innovation, changes to scope of practice, and job redesign (all properly evaluated).10 Role substitution is one approach that has been implemented, usually involving nurses replacing doctors after extra training. Examples include caring for patients with heart failure in the home (where nurses obtain better results, interestingly).11 Nurses are also specially trained for new technology roles, such as managing complex operating theatre equipment, and providing the special skills of intensive care. But requiring a complete nursing education as a prerequisite seems hopelessly inefficient if the basic skills are under-used in the new role. Moreover, 78% of the nation’s nursing workforce will need to be replaced between 2003 and 2012, and there is a projected shortfall of about 6100 nurses annually.12 Nursing as a career seems to have difficulties in recruitment, presumably an image problem, that dwarf any other health profession’s workforce problems.13 Recruiting from the nursing pool will only shift the problem there, creating more problems than it solves.
We propose a new workforce rather like physician assistants of the United States.14 Our current educational machinery increasingly deepens specialisation, preparing clinicians for functions “just in case” (an emphasis on specialised functions ready to hand), rather than “just in time” (accessing such functions as needed).15 In other words, clinical work demands easy patient access to a wide range of clinical skills, yet our workforce becomes increasingly fragmented. Most clinical work for patients with multiple comorbidities increasingly requires knowledge and skills that are “mile wide” and “inch deep”.
If this sounds like science fiction, look at the experiments at the University of Southampton Hospital Trust, in the United Kingdom, where an “educational escalator” (a series of common educational modules provided by both health and educational sectors) now exists. With some modification, this could enable health workers to move either vertically or laterally into other health professions. Further, a patchwork of modules could be grouped together in different ways to form several complete sets of different professional skills,16 some common to many roles, some to all. The matrix enables health professionals to move across the tapestry in any direction needed by the health service, and preferred by the individual, dependent upon aspiration and ability. This contrasts with the current system, which looks more like Snakes and Ladders (without the ladders): to move into a new traditional discipline (say, to move from physiotherapy to occupational therapy, or even medicine) means abandoning almost everything so far achieved (prior learning being almost never recognised) to start from a bottom square again.
All this raises the question of what traditional disciplines we need to retain. Do we need doctors with all their specialist divisions? The answer depends on what society wants. If it is one individual responsible for the delivery of care at separate points of the care continuum, then one person has to assume that responsibility. In the current system, that is ultimately a doctor. Certainly that responsibility is sometimes delegated to another (for example, a nurse or allied health professional, or in our new model, a new health professional: Box), and with that delegation (assuming it is done properly) goes also responsibility. But the person making the delegation is ultimately a doctor.
This solution creates a new environment in which people can enter medicine by a route different to the current one (rather like officer selection for the military, which allows “elevation through the ranks”). Everyone then would have a common entrance into health. Progress would be by merit and ability. People could advance their careers or retreat them as suits their career, personal aspirations and abilities. They would have a better understanding of each others’ roles, reducing the perception of arrogance levelled at doctors.17
This would also be a good time to correct that absurd inversion of health learning: the primacy of basic science as a necessary “foundation” for clinicians, existing in slightly different forms for every health care worker. It is rather like teaching a child the principles of the gyro, the atomic structure of metal, and Boyle’s Law for pressure of gases as prerequisites for learning to ride a bicycle. Basic science learning is necessary, of course, but surely at the end stage? Far more necessary is the acquisition of basic management-of-people skills, communication skills, and the ability to comfort, which all health workers need, and which (consistently) society says is missing.17 The consequence is that all health workers should be grounded in this common core as the basic foundation, and this might include everyone in the health care sector — management, administration, reception and patient services staff. As people progress in their learning, so they drill down deeper into the basic sciences.
- Christopher B Del Mar1
- Naomi Dwyer2
- Bond University, Gold Coast, QLD.
None identified.
- 1. Black N. Rise and demise of the hospital: a reappraisal of nursing. BMJ 2005; 331: 1394-1396.
- 2. Cameron AJ, Welborn TA, Zimmet PZ, et al. Overweight and obesity in Australia: the 1999–2000 Australian Diabetes, Obesity and Lifestyle Study (AusDiab). Med J Aust 2003; 178: 427-432. <MJA full text>
- 3. Schofield DJ, Beard JR. Baby boomer doctors and nurses: demographic change and transitions to retirement. Med J Aust 2005; 183: 80-83. <MJA full text>
- 4. Queensland Health. Smart state: health 2020. A vision for the future. Summary discussion paper. Brisbane: Queensland Health, 2002. Available at: http://www.health.qld.gov.au/health2020/ (accessed May 2006).
- 5. Barrett NR. The contribution of Australians to medical knowledge. Med Hist 1967; 11: 321-333.
- 6. Australian Institute of Health and Welfare. Australia’s health 2004. Canberra: AIHW, 2004. (AIHW Catalogue No. AUS44.) Available at: http://www.aihw.gov.au/publications/index.cfm/title/10014 (accessed May 2006).
- 7. Duckett SJ. Interventions to facilitate health workforce restructure. Aust New Zealand Health Policy 2005; 2: 14.
- 8. Forster P (Chair). Queensland health systems review. Final report. Brisbane: Queensland Health, 2005. Available at: http://www.health.qld.gov.au/health_sys_review/final/default.asp (accessed May 2006).
- 9. Joyce CM, McNeil JJ, Stoelwinder JU. More doctors, but not enough: Australian medical workforce supply 2001–2012. Med J Aust 2006; 184: 441-446. <MJA full text>
- 10. Australian Government Productivity Commission. Australia’s health workforce. Position paper. Melbourne: Productivity Commission, 2005.
- 11. Stewart S, Marley JE, Horowitz JD. Effects of a multidisciplinary, home-based intervention on unplanned readmissions and survival among patients with chronic congestive heart failure: a randomised controlled study. Lancet 1999; 354: 1077-1083.
- 12. Australian Health Workforce Advisory Committee. The Australian nursing workforce — an overview of workforce planning 2001–2004. AHWAC report 2004.2. Sydney: AHWAC, 2004. Available at: http://www.health.nsw.gov.au/amwac/reports.html (accessed May 2006).
- 13. Buerhaus PI, Staiger DO, Auerbach DI. Implications of an aging registered nurse workforce. JAMA 2000; 283: 2948-2954.
- 14. Physician assistant and nurse practitioner workforce trends. Am Fam Physician 2005; 72: 1176.
- 15. Duckett S. Health workforce design for the 21st century. Aust Health Rev 2005; 29: 201-210.
- 16. Humphris D, Hean S. Educating the future workforce: building the evidence about interprofessional learning. J Health Serv Res Policy 2004; 9 (Suppl 1): 24-27.
- 17. National Health and Medical Research Council. Communicating with patients: advice for medical practitioners. Canberra: NHMRC, 2004. Available at: http://www.nhmrc.gov.au/publications/synopses/e58syn.htm (accessed May 2006).





Abstract
The health workforce crisis needs radical treatment; simply educating more health workers will be insufficient, and role substitution among existing health workers is untenable.
We propose a new class of health worker who would take on single disease or single procedure responsibilities, working mostly to protocols; and be embedded within current structures.
We also propose modular health education which has fewer entry points into the health system, allows transfer between different disciplines, and is based on modules that can be accumulated to allow progress through the system to gain more clinical responsibility.