Demographic shifts over the next 20 years will produce fundamental change in Australia’s society and economy. The ageing of the “baby boomer” generation and population growth will place an unprecedented demand on health services, which will need to be met by the resources of a shrinking pool of employed younger people.1,2 The health care workforce will also be caught in the grip of this changing demographic landscape. It is widely anticipated that retirement among ageing clinicians will result in workforce shortages within the next 5 years.3-6
Grouped data on the demographic characteristics (age, sex, hours worked and region) for GPs (including trainees), specialists and registered nurses were obtained from the ABS Census of Population and Housing for the years 1986, 1991, 1996 and 2001. All health professions are generally combined in a single category, so separation of health professions was specially requested. As individuals cannot be followed from one census to the next, age groups were followed as cohorts (there is little movement in age groups approaching retirement, as they are largely unaffected by migration [Department of Immigration, Multicultural and Indigenous Affairs, Research and Statistics Section, Immigration data extract, 1 February 2005, personal communication]).
Cohort age boundaries vary a little in the literature. We applied more common boundaries which aligned with the 5-year age groups of the data (Box 1). The data were then used to calculate attrition rates as GPs, specialists and nurses left the workforce (because of factors including retirement, ill health and death).
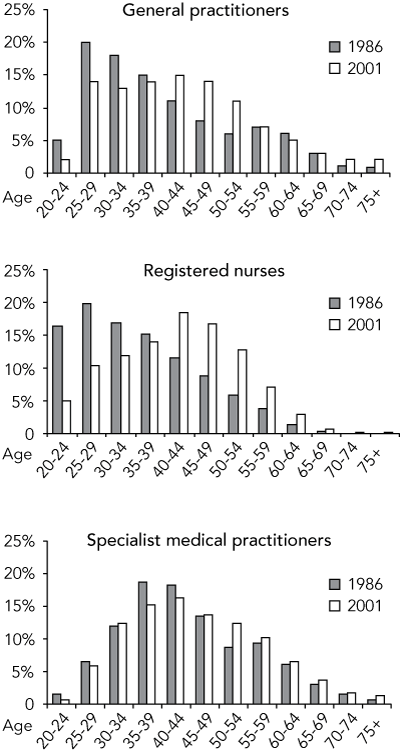
Between 1986 and 2001 there was an increase in the total numbers of GPs, nurses and specialists (Box 1) and a significant difference in their age distribution (P < 0.001) (Box 2).
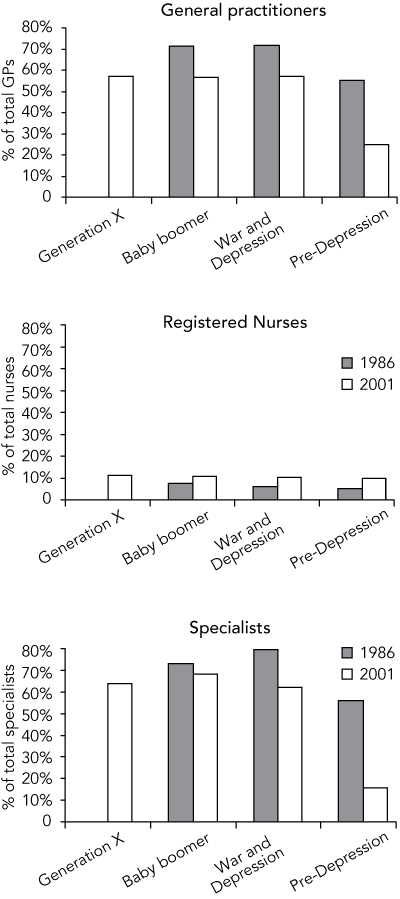
Between 1986 and 2001, the proportion of GPs aged over 40 years rose from 42% to 58% (Box 2). Over the same period, the proportion of baby boomers in the GP workforce fell from 58% to 55% (Box 1).
A similar, but more marked, pattern was seen for registered nurses. Over the period 1986 to 2001, the proportion of working nurses aged over 40 years doubled from about 30% to 60%, while baby boomers still made up over 60% of the nursing workforce in 2001. Few registered nurses remain in the workforce after the age of 60 years — less than 5% (Box 2).
The age structure of the medical specialist population did not change as substantially over the study period. Between 1986 and 2001, the proportion of specialists aged over 40 years rose from about 60% to about 65%. In 2001, baby boomers formed about 60% of the specialist population (Box 1).
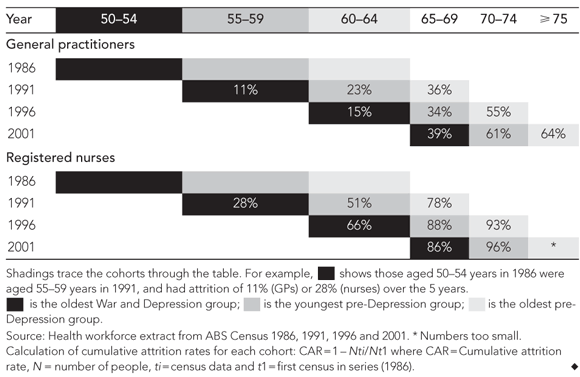
With the rapid ageing of the medical workforce, patterns of attrition become critical to the workforce age structure. The cumulative attrition rate of the “pre-Depression” and “War (World War II) and Depression” cohorts from 1986 to 2001 were examined. Most notable was the earlier retirement of nurses compared with GPs (P < 0.001) (Box 3).
Over the study period, census data also showed a decline in the proportion of GPs reporting working 41 or more hours per week (P < 0.001) (Box 4). Although this partly reflects feminisation of the workforce (Box 5), men have also reduced their working hours. About 80% of male baby boomers were working more than 41 hours per week in 1986, but only 64% of the younger male cohort “generation X” worked more than 41 hours in 2001.
Only about 10% of nurses reported working 41 or more hours per week. However, there has been a slight but significant increase in the proportion of nurses working long hours (P < 0.001) (Box 4).
The ageing of the medical workforce provides a direct benefit to the Australian community through the accumulated experience of senior health professionals. However, it also creates some very significant workforce planning issues. For example, if the baby boomer cohort of nurses leaves the workforce at the same rate as previous generations, all but a handful will have retired within the next 15 years. This reflects a loss of more than half the current workforce. As the oldest baby boomers turn 59 this year, we are on the cusp of this rapid attrition from the nursing workforce. The decline in nursing undergraduate commencements over the 10 years to 2003 will only exacerbate the emerging shortage.6
Baby boomers also represent just over half the GP workforce, although they may move more slowly from the workforce as they tend to retire later.7 However, by 2001, those remaining in the workforce typically worked fewer hours.3-6 In part, the ageing of the GP workforce reflects an increasing proportion of medical graduates choosing to enter specialty disciplines.5 This will also be influenced by the longer training period now undertaken by GPs, although, in our analyses, trainee GPs are grouped in the same category as fully qualified GPs.
Baby boomers also make up about half of the specialist population. One reason specialists have a higher average age is the length of training required. Nonetheless, there is a need to examine potential shortages in individual specialties, as ageing is not homogeneous (for example, the average age of emergency medicine specialists in 2002 was 41 years, compared with 54 years for general surgery3).
Although the census data do not directly answer this question, the wider literature on retirement provides some useful indicators. Three of the most significant factors are the available income replacement rate (from superannuation, pension and private investments), flexibility of working arrangements, and health status.8-10
Most nurses are employed within the hospital system and have access to employer superannuation, although women with children may have a lower accumulated balance because of broken employment patterns. Also, female nurses are eligible for the aged pension at a younger age than men.10,11 Although nurses on average earn less than GPs, this is consistent with earlier retirement, as they require less income to generate the same proportion of their pre-retirement earnings.
Hospital-based nurses approaching retirement are less likely to have the same flexibility of working hours as the self-employed and may choose to retire rather than continue shift work. The literature points to physically demanding and stressful work and health problems as determinants of early retirement, with back injuries being one of the most important.8,9,12
Finally, most nurses are female and women tend to leave the workforce earlier.13 Wives are on average younger than husbands, and may shorten their working life to align their retirement with that of their spouse.14 However, although women are observed to retire earlier in general retirement studies, we found no difference in the rate of attrition of male and female nurses in this study.
GPs are more likely to be male, have higher earnings and be self-employed. Higher earnings on the job and number of years of education decrease the probability of job exit.12 Job satisfaction is also important in reducing doctors’ intentions to retire.15
GPs, usually self-employed and without compulsory superannuation, may not have developed an awareness of the need for retirement savings until later in life. People under 45 are less likely to save for retirement, and even in the top income quintile (top 20%), a third do not save.16 In retirement, they are unlikely to qualify for more than a small part-rate aged pension, and not until aged 65 if they are male.11 Therefore, for GPs without significant income producing assets, the fall in income from their pre-retirement earnings (the substitution effect) can be significant and provides an incentive to continue to work.8,17 In addition, they do not face a mandatory retirement age and are able to continue to work flexibly at reduced hours, thus increasing the likelihood of working longer.9
What effect do the retirement patterns of doctors and nurses have on the wider economy? The health workforce was about 450 000 in 2001, comprising 6% of the total workforce, with more than half being doctors and nurses.18,19 With such large numbers, and higher than average incomes, the retirement patterns of the medical and nursing workforce will noticeably affect the future labour market and taxation revenue.
GPs already have retirement patterns that conform to the Treasury ideal — gradual retirement and working beyond traditional retirement age as a solution to an emerging labour force shortage and to fund the future health costs of an ageing population.20,21 However, there are more than 200 000 nurses in a profession from which early retirement is typical. It is important to increase labour force participation of older nurses and, in particular, we need to examine how nurses could be encouraged to stay in the workforce longer. Addressing workplace safety and health issues, or increasing the flexibility of shift work, may be as important to workforce longevity as economic incentives. For example, the creation of less physically demanding jobs, such as practice nursing in a general practice clinic, may provide positions which are attractive to nurses considering retirement.
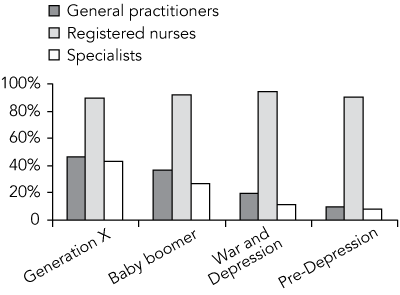
1 Definition and size of cohorts
Number of general practitioners (% of total GP workforce) |
Number of nurses (% of total nursing workforce) |
Number of specialists (% of total specialist workforce) |
|||||||||||||
Received 12 April 2005, accepted 30 May 2005
- Deborah J Schofield1
- John R Beard2
- Northern Rivers University Department of Rural Health, University of Sydney, Lismore, NSW.
We thank Arul Earnest for assistance with statistical analysis and Dr Sue Page and Dr Megan Passey for helpful comments based on their own experience as medical practitioners.
None identified.
- 1. Budget Paper 5: Intergenerational Report 2002–03. Canberra: Commonwealth of Australia, 2002. Available at: http://www.budget.gov.au/2002-03/bp5/html/index.html (accessed Jun 2005).
- 2. Economic implications of an ageing Australia. Research report. Canberra: Productivity Commission, 2005. Available at: http://www.pc.gov.au/study/ageing/finalreport/index.html (accessed Jun 2005).
- 3. Medical labour force 2002. National Health Labour Force Series No. 30. Canberra: AIHW, 2004. (AIHW Catalogue No. HWL 30.) Available at: http://www.aihw.gov.au/publications/index.cfm/title/10071 (accessed Jun 2005).
- 4. Australian Institute of Health and Welfare. Nursing labour force 2001. National Health Labour Force Series No. 26. Canberra: AIHW, 2003. (AIHW Catalogue No. HWL 26.) Available at: http://www.aihw.gov.au/publications/index.cfm/title/8782 (accessed Jun 2005).
- 5. Australian Medical Workforce Advisory Committee. Annual Report 2003–04. AMWAC Report 2004.5. Sydney: AMWAC, 2004. Available at: http://www.health.nsw.gov.au/amwac/reports.html (accessed Jun 2005).
- 6. Australian Health Workforce Advisory Committee. Annual Report 2003–04. AHWAC Report 2004.3. Sydney: AHWAC, 2004. Available at: http://www.health.nsw.gov.au/amwac/reports.html (accessed Jun 2005).
- 7. Davidson J, Lambert T, Goldacre M. Career paths and destination 18 years on among doctors who qualified in the United Kingdom in 1977: postal questionnaire survey. BMJ 1998; 317: 1425-1428.
- 8. Dwyer DS, Mitchell OS. Health problems as determinants of retirement: are self-rated measures endogenous? J Health Econ 1999; 18: 173-193.
- 9. Hurd M, McGarry K. The relationship between job characteristics and retirement. Working paper 4558. Cambridge, Mass: National Bureau of Economic Research, 1993.
- 10. Centrelink. Income test for pensions. Available at: http://www.centrelink.gov.au (accessed Mar 2005).
- 11. Centrelink: Pensions, payments, allowances and tests. In: About seniors [website]. Available at: http://www.aboutseniors.com.au/centrelink.html (accessed Mar 2005).
- 12. Meghir C, Whitehouse E. Labour market transition and retirement of men in the UK. J Econom 1997; 79: 327-354.
- 13. Australian Bureau of Statistics. Retirement and retirement intentions. Canberra: ABS, 1997. (ABS Catalogue No. 6238.0.)
- 14. Butler M, Huguen O, Teppa F. What triggers early retirement? Results from Swiss pension funds. CEPR Discussion paper 4394. London: Centre for Economic and Policy Research, 2004.
- 15. Sibbald B, Bojke C, Gravelle H. National survey of job satisfaction and retirement intentions among general practitioners in England. BMJ 2003; 326: 22.
- 16. Kelly S, Toohey M. Who are Australia’s best savers? The second report on savings prepared for the Financial Planning Association of Australia. Canberra: National Centre for Social and Economic Modelling, 2002. Available at: http://www.fpa.asn.au/FPA/Research.asp (accessed Jun 2005).
- 17. Mitchell OS, Fields GS. The economics of retirement behaviour. J Labour Stud 1984; 2: 84-105.
- 18. Australian Bureau of Statistics. 2001 Census classification counts: occupation, Australia. Available at: http://www.abs.gov.au (accessed Mar 2005).
- 19. Australian Institute of Health and Welfare. Health and community services labour force 2001. National Health Labour Force Series No. 27. Canberra: AIHW, 2003. (AIHW Catalogue No. HWL 27; ABS Catalogue No. 8936.0.) Available at: http://www.aihw.gov.au/publications/index.cfm/title/9328 (accessed Jun 2005).
- 20. Gruen D, Garbutt M. The output implications of higher labour force participation. Treasury Working Paper 2003-02. Canberra: Treasury, 2003. Available at: http://www.treasury.gov.au/contentitem.asp?NavId=049&ContentID=702 (accessed Jun 2005).
- 21. Gruen D, Garbutt M. The long term fiscal implications of raising Australian labour force participation or productivity growth. Treasury Working Paper 2004-01. Canberra: Treasury, 2004. Available at: http://www.treasury.gov.au/contentitem.asp?NavId=049&ContentID=820 (accessed Jun 2005).





Abstract
Objectives: To examine the effect of demographic change on employment patterns for general practitioners, medical specialists and nurses since 1986, and to compare their patterns of retirement.
Design and setting: Secondary analysis of previously unpublished Australian Bureau of Statistics Census data for the years 1986, 1991, 1996 and 2001.
Main outcome measures: Age distribution of GPs, specialists and nursing workforce; attrition rates as GPs, specialists and nurses left the workforce; and hours worked according to age group.
Results: The age profile of the GP, specialist and nursing workforce has aged since 1986 (P < 0.001), with the “baby boomer” generation making up more than half the workforce in 2001. A large proportion of GPs continued to work beyond the traditional retirement age of 65 years, with nurses retiring at a younger age than doctors (P < 0.001). All GP cohorts worked fewer hours in 2001 than they did in 1986 (P < 0.001), with “generation X” GPs working fewer hours than the baby boomers did at the same age (P < 0.001).
Conclusions: Attrition of baby boomer clinicians will place unprecedented pressure on the medical workforce, and policy makers face a critical challenge to ensure workforce needs are met over the next 20 years. Policies and incentives to encourage ongoing employment among older clinicians, albeit at reduced hours, are crucial if the Australian health workforce is to be adequate to meet the growing community demand of the 21st century.