Falls are the leading cause of injury in Australian hospitals, with 38% of all hospital incidents related to falls.1 Patients are at increased risk of falling in the hospital setting because of increased incidence of confusion, confounding medical conditions, polypharmacy and environmental factors. A fall in hospital that results in serious injury is estimated to add at least $15 000 to a patient’s costs, as a result of increased length of stay and surgical costs. Besides the psychological and physical impact on the individual, it is estimated that the annual cost due to falls is over $500 million in Victoria and $2 billion nationally.2
A number of systematic reviews have shown that targeted multi-intervention approaches can reduce falls among older people in the community.3-5 In hospital settings, single interventions have not been proven successful in preventing or reducing falls, whereas multisystem or multistrategy approaches have shown to be more effective.6-11 Only recent studies, however, have had sufficient power to support this.12,13
A standardised definition for a “fall” was developed by the project team as follows:
An unintended change of position which results in the person coming inadvertently to the ground or other surface lower than the person had been previously. This includes impacting against an adjacent surface (eg, wall or furniture), slips, trips and lowering/assisting a patient who is in the act of falling.
Levels 1–4: minor injuries, including grazes and bruises;
Levels 5–6: significant injuries, including lacerations/skin tears requiring suturing/bandage/cold pack, or any injury requiring further investigation such as x-ray;
Level 7: injuries resulting in a fracture, head injury or increased length of stay;
Level 8: injuries resulting in permanent disability or contributing to death.
The Falls Prevention Project was a prospective, non-randomised quality improvement project that was phased in over 3 months from September 2001. We piloted and trialled various small projects on the different wards and in different groups of patients to find which approaches appeared to be helpful as well as acceptable to both patients and staff. The successful strategies (Box 1) were then systematically rolled out to the other wards.
Root-cause analyses of falls allowed us to identify systems and processes that contributed to falls on the wards and helped us set priority areas for focus. These analyses continued throughout the project for serious (Level 7 and 8) injuries. Of a number of published tools tested, we found the Falls Risk Assessment Scoring System (FRASS) tool gave the highest predictive value for falls in our patient population, together with good staff compliance in completing the tool.14 This tool allocated points for various risk factors such as confusion, multiple medications, history of falls, ambulation, need for assistance with toileting, and age. It was completed by nursing staff for all patients on admission, and was repeated after any fall. Given the large number of “at risk” patients identified by the FRASS tool, we further allocated some patients to a “super high-risk” category — based on a score higher than 15 out of 30 — to provide a priority focus for staff. Potential medical contributing factors (such as intercurrent illness, medications and postural hypotension) were taken into consideration and addressed.
There was little difference in patient demographics between the 12-month baseline period (2001) and the second full year of the project (2003), except for a slight reduction in length of stay by 2.5 days (Box 2). Root-cause analyses identified a number of key contributing factors, the major one being that 82% of falls were not observed. Over 60% occurred around the bed. Other contributing factors were ward equipment (eg, beds, chairs); medical factors (eg, hypotension, toileting issues, neurological and musculoskeletal impairment); intrinsic patient factors (eg, confusion, impulsiveness, language barrier, footwear); environmental factors (eg, lighting and floor surfaces); and staff attitude and knowledge (eg, resistance to changing work practices and to adopting additional documentation).
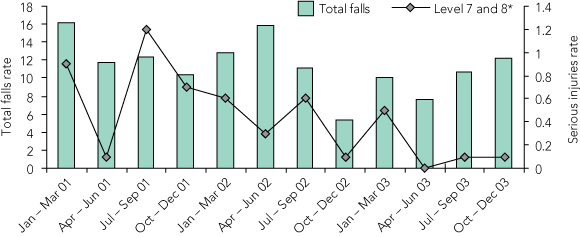
The total number of falls in each year of the project and the number involving serious injury, together with a quarterly breakdown, are shown in Box 3. Between 2001 and 2003, there was a 19% reduction in falls per 1000 OBDs (P = 0.001). Of greater importance was the 77% reduction in serious (Level 7 and 8) injuries per 1000 OBDs over the same period (P = 0.0004).
Given that so many falls were, and are, unwitnessed, the principal driver for our project was to try to increase surveillance, optimise the environment, and improve the management of this high-risk population by a multistrategy approach (Box 1).
Unlike other studies, ours has shown not only a highly significant reduction in serious injuries but also that this could be sustained over an extended period. Vassallo et al reported a borderline reduction in falls, but no significant reduction in injuries, in a rehabilitation population.15 Their program was initiated up to 3 days after admission, and changes were based on weekly evaluation and case conference. In our project, assessment commenced on the day of admission (when the risk of falls is likely to be high), and changes were made prospectively, as and when necessary. We noted that it took more than 6 months to establish a culture of improved reporting, particularly of minor falls and repeat falls.
Healey et al, in a 12-month controlled study of elderly inpatients using a targeted risk factor approach, demonstrated a significant reduction in falls but not in fall-related injuries.13 Haines et al reported on an intensive multicomponent trial in a subacute hospital setting that achieved a 30% reduction in falls but no reduction in serious injuries;12 no long-term data were presented to show whether the changes could be sustained. Oliver et al, in a systematic review of hospital falls prevention programs, found that many involved only short-term follow-up6 (in contrast to our 2-year follow-up). One of the longest studies, by Barrett et al, reported an increased number of falls but a 25% reduction in injury over a 5-year period.11 As their data were not standardised for the number of OBDs, it is difficult to interpret this finding.
Using the first 12 months’ data as a historical control does introduce the potential bias of unforeseen confounders, including changes in casemix, staff and activity. However, most factors remained fairly constant over the 3-year period of the study. Admission criteria to CGMC did not change, although length of stay was reduced as a result of greater efforts to improve throughput of patients. Medical and nursing staffing profiles were unchanged and no additional staff were placed on the wards from the project team. Data were collected from the same wards, with similar patient profiles at the beginning and end of the study. Furthermore, our methodology overcame the bias introduced by studying multiple interventions within the same institution (the Hawthorne effect), which would likely have occurred in any randomised approach. Oliver, in a recent editorial, discussed the complexity of trial design in fall intervention studies.16
Our results confirm the belief of other investigators that a multisystem approach, rather than single interventions, is needed to achieve a significant reduction in falls and fall-related injury.6-13,17 Reducing falls is an imperative compounded by the rapid ageing of our population: between 2001 and 2051, there will be an anticipated five-fold increase in people aged over 85 years, the group at greatest risk of falling and sustaining serious injury in hospital. While our study did not attempt to measure the cost-effectiveness of interventions, the reduction in serious injuries from 27 to seven a year would have brought at least modest savings to the organisation, given the estimated cost of $15 000 per serious injury.
1 Strategies that have been trialled at Caulfield General Medical Centre to reduce falls
Review of toileting protocols and practices for patients at risk of falling
Fitted bed sheets
Review of use of non-slip bedside mats
Extended bedside call bells so patients do not fall reaching out
Non-slip chair mats
Electric low beds that go to within 12 cm of floor
Bed alarms that identify when patients have moved out of their bed
Bed poles to assist patients to transfer more independently
Family brochure informing them about falls and encouraging their involvement
Volunteer program
Early feeding of dependent patients
Engaging patients in more activities
Orange wrist band and chart above bed to identify patients at high risk of falling
Each ward appointed a “falls prevention” portfolio holder
Ward compliance audits
Staff orientation brochures/folders
Falls risk assessment tool and medical record alert sticker
Promotion of team ownership of the project and problem-solving of reasons for falls on respective wards
Protocols for after-fall reviews
Reporting of falls at multidisciplinary and quality improvement meetings and management forums
2 Demographics of patients admitted to Aged Care Services wards at Caulfield General Medical Centre in 2001 and 2003
Received 30 May 2005, accepted 18 January 2006
- David Fonda1,2
- Jennifer Cook1
- Vivienne Sandler1
- Michael Bailey2
- 1 Aged Care Services, Caulfield General Medical Centre, Melbourne, VIC.
- 2 Monash University, Melbourne, VIC.
We would like to thank the Victorian Department of Human Services (DHS) for project funding and Bayside Health and CGMC Falls Prevention Team for their dedicated work.
The DHS was not involved with study design, data collection, analysis, interpretation of results or preparation of our article for publication.
- 1. Joanna Briggs Institute. Falls in hospitals. Best Practice 1998; 2 (2).
- 2. Mathers C, Penm R. Health system costs of injury, poisoning and musculoskeletal disorders in Australia 1993–94. Canberra: Australian Institute of Health and Welfare, 1999. (AIHW Cat. No. HWE 12; Health and Welfare Expenditure Series No. 6.)
- 3. Gillespie LD, Gillespie WJ, Robertson MC, et al. Interventions for preventing falls in elderly people. Cochrane Database Syst Rev 2003; (4): CD000340.
- 4. American Geriatrics Society, British Geriatrics Society and American Academy of Orthopaedic Surgeons Panel on Falls Prevention. Guideline for the prevention of falls in older persons. J Am Geriatr Soc 2001; 49: 664-672.
- 5. Chang J, Morton S, Rubenstein L, et al. Interventions for the prevention of falls in older adults: systematic review and meta-analysis of randomised clinical trials. BMJ 2004; 328: 680-683.
- 6. Oliver D, Hopper A, Seed P. Do hospital fall prevention programs work? A systematic review. J Am Geriatr Soc 2000; 48: 1679-1689.
- 7. Hayes N. Prevention of falls among older patients in the hospital environment. Br J Nurs 2004; 13: 896-901.
- 8. National Ageing Research Institute. An analysis of research on preventing falls injury in older people: acute care settings. Report to the Commonwealth Department of Health and Aged Care Injury Prevention Section. Melbourne: NARI, 2000.
- 9. Evans D, Hodgkinson B, Lambert L, et al. Falls in acute hospitals — a systematic review. Adelaide: Joanna Briggs Institute, 1998.
- 10. Guelich M. Prevention of falls in the elderly: a literature review. Top Geriatr Rehabil 1999; 15: 15-25.
- 11. Barrett J, Bradshaw M, Hutchinson K, et al. Reduction of falls-related injuries using a hospital inpatient falls prevention program. J Am Geriatr Soc 2004; 52: 1969-1970.
- 12. Haines T, Bennell K, Osborne R, Hill K. Effectiveness of targeted falls prevention programme in subacute hospital setting: randomised controlled trial. BMJ 2004, 328: 676-679.
- 13. Healey F, Monro A, Cockram A, et al. Using targeted risk factor reduction to prevent falls in older in-patients: a randomised controlled trial. Age Ageing 2004; 33: 390-395.
- 14. MacAvoy S, Skinner T, Hines M. Clinical methods. Fall risk assessment tool. Appl Nurs Res 1996; 9: 213-218.
- 15. Vassallo M, Vignaraja R, Sharma J, et al. The effect of changing practice on fall prevention in a rehabilitative hospital: the Hospital Injury Prevention Study. J Am Geriatr Soc 2004; 52: 335-339.
- 16. Oliver D. Prevention of falls in hospital inpatients. Agendas for research and practice [editorial]. Age Ageing 2004; 33: 328-330.
- 17. Mitchell A, Jones N. Striving to prevent falls in an acute care setting — action to enhance quality. J Clin Nurs 1996; 5: 213-220.





Abstract
Objective: To determine whether the rate of falls and associated serious injuries in a hospital aged care setting can be reduced using a multistrategy prevention approach.
Design, setting and participants: Three-year quality improvement project comparing data at baseline (2001) and at 2-year follow-up (2003) after interventions to reduce falls. All patients admitted to the Aged Care Services wards at Caulfield General Medical Centre, Melbourne, between January 2001 and December 2003 were included.
Interventions: Multistrategy approach phased in over 3 months from September 2001 and involving data gathering, risk screening with appropriate interventions, work practice changes, environmental and equipment changes, and staff education.
Main outcome measures: Total number of falls; number of falls resulting in serious injuries (fractures, head injuries, death); staff compliance with the risk assessment.
Results: Over a 2-year period, there was a 19% reduction in the number of falls per 1000 occupied bed-days (OBDs) (12.5 v 10.1; P = 0.001) and a 77% reduction in the number of falls resulting in serious injuries per 1000 OBDs (0.73 v 0.17; P < 0.001). Staff compliance with completing the falls risk assessment tool increased from 42% to 70%, and 60% of staff indicated they had changed their work practices to prevent falls.
Conclusion: A multistrategy falls prevention program in an aged care hospital setting produced a significant reduction in the number of falls and a marked reduction in serious fall-related injuries. Incorporating a falls prevention program into all levels of an organisation, as part of daily care, is crucial to the success and sustainability of falls prevention.