A 20-year old woman presented with a history of frequent epistaxis (from 10 years of age) and bleeding from the tongue (from 8 years of age). She also reported breathlessness on exertion, along with cyanosis and bulbous deformity of the fingers since 4 years of age. There was no history of bleeding from any other site or of a similar illness in the family.
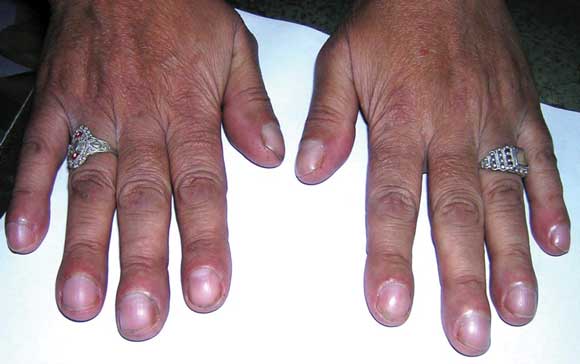
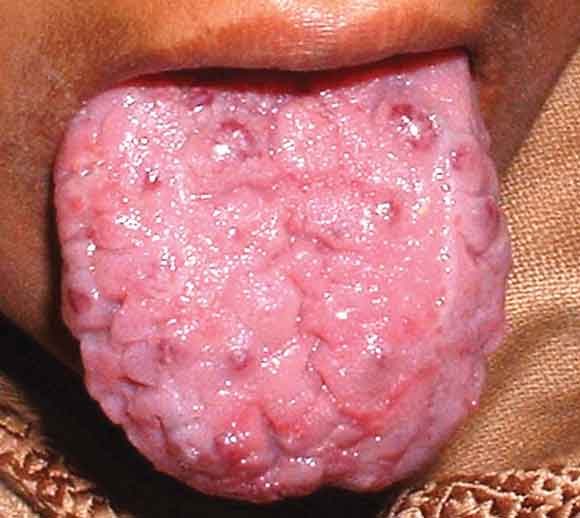
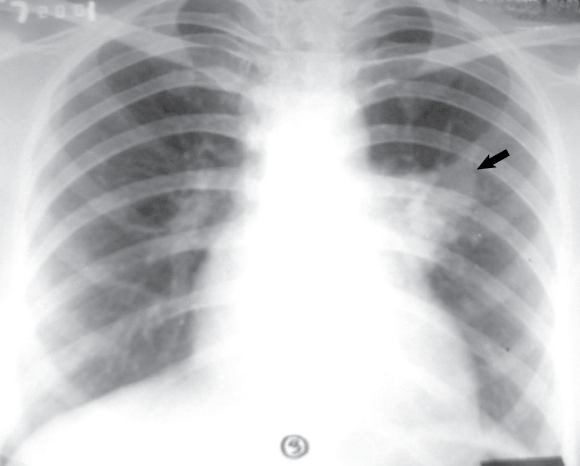
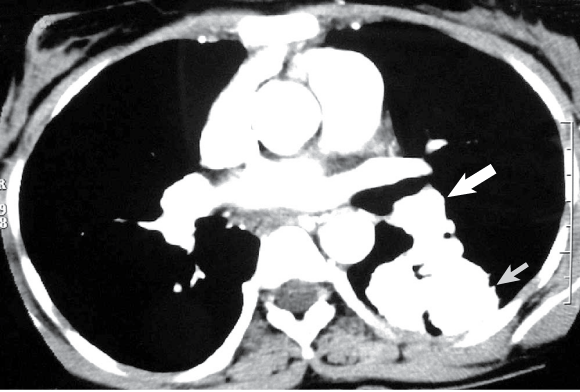
On examination, the patient had cyanosis and clubbing (Box 1), and a lumpy tongue (Box 2) suggestive of tongue telangiectasia. A chest x-ray showed left mid-zone opacity (Box 3), which was confirmed to be a pulmonary arteriovenous malformation (AVM) on spiral computed tomographic angiography (Box 4). Transcutaneous embolotherapy produced a marked improvement in her symptoms. The patient is currently asymptomatic and undergoing regular follow-up.
The patient has hereditary haemorrhagic telangiectasia (Osler–Weber–Rendu disease), an autosomal dominant disorder related to mutations on chromosomes 9 and 12. Clinical diagnosis is based on the findings of epistaxis, telangiectasia, visceral AVMs and family history. Fulfilling three of these criteria indicates a definite diagnosis; two, a possible case. In our patient, the presence of three of the four manifestations confirmed the diagnosis.
Pulmonary AVMs are found in 14%–30% of patients with this disease.1 A family history of the disease may not be present in all cases, owing to de-novo germline mutations. As these occur more frequently in later cell divisions during gametogenesis, siblings are rarely affected.
- Ritesh Agarwal1
- Ashutosh N Aggarwal2
- Dheeraj Gupta3
- Department of Pulmonary Medicine, Postgraduate Institute of Medical Education and Research, Chandigarh, India.
- 1. Fuchizaki U, Miyamori H, Kitagawa S, et al. Hereditary haemorrhagic telangiectasia (Rendu-Osler-Weber disease). Lancet 2003; 362: 1490-1494.