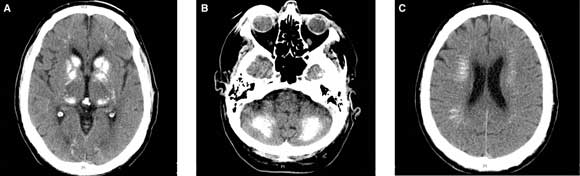
A 66-year-old man presented with a 12-month history of progressive gait disturbance with cerebellar ataxia and extrapyramidal features. Computed tomography of the head showed calcification of the basal ganglia and dentate nuclei of the cerebellum, and periventricular calcification (Box).
Biochemical testing showed serum level of calcium, 1.19 mmol/L (reference range [RR], 2.15–2.55 mmol/L); ionised calcium, 0.61 mmol/L (RR, 1.14–1.29 mmol/L); phosphate, 1.8 mmol/L (RR, 0.8–1.5 mmol/L); and parathyroid hormone, 0.9 pmol/L (RR, 1.5–8.0 pmol/L). The patient was diagnosed with hypocalcaemia caused by idiopathic hypoparathyroidism. He was treated with calcitriol (2 μg daily) and calcium carbonate (6.0 g daily). His gait showed some improvement, and serum calcium levels became normal over several weeks.
- Huong Van Nguyen1
- Seng Khee Gan2
- Royal Perth Hospital, Perth, WA.