Behaviour change involving the whole family is more likely to be successful.
The World Health Organization describes the “escalating global epidemic” of obesity as “one of today’s most blatantly visible — yet most neglected — public health problems”.1 Studies of obesity prevalence over time show an increase of 2.3–3.3-fold over about 25 years in the United States and 2.0–2.8-fold over 10 years in the United Kingdom.2
Current estimates in Australian children and young people indicate that 20%–25% are overweight or obese. The 1995 National Nutrition Survey found that 4.9% of boys and 5.4% of girls were obese, and two other studies in 1997 (the New South Wales Schools Fitness and Physical Activity Survey, and the Health of Young Victorians Study) gave similar results.3 There is also evidence that, between 1985 and 1995, the rates of overweight have doubled and those of obesity have trebled.4
An Australian expert working group has identified body mass index (BMI) as the most appropriate measure of excessive weight in children. BMI is calculated by dividing the weight (kg) by the height squared (m2).
Rapid changes in BMI occur in normal growth, and BMI varies with age and sex. It rises in the first year of life, then falls during preschool years, before rising again into adolescence. The point at which BMI starts to rise again (usually around 4–6 years of age) is termed “adiposity rebound”. Thus, calculated BMI values need to be compared with age and sex reference standards. For clinical use, the expert working group has recommended the BMI-for-age percentile charts developed in the United States by the National Center for Health Statistics in collaboration with the National Center for Chronic Disease Prevention and Health Promotion.5 These can be downloaded from the Centers for Disease Control and Prevention website (for boys 2–20 years: <www.cdc.gov/nchs/data/nhanes/growthcharts/set1/chart16.pdf> for girls 2–20 years <www.cdc.gov/nchs/data/nhanes/growthcharts/set1/chart16.pdf>). BMI greater than the 85th percentile suggests overweight, while BMI greater than the 95th percentile suggests obesity. These charts can be used in clinical practice to monitor progress.
Several studies have shown that there is a strong genetic basis to the development of obesity. Obesity appears to be a polygenic disorder, with many genes currently linked or associated with a predisposition to excess adiposity.6 At least five single-gene mutations causing human obesity that present in childhood have been identified. These are rare and all are associated with severe and very early onset obesity, and should prompt referral for further assessment.
Sedentary behaviour: Physical inactivity is a major element in the development of obesity in westernised societies — in children and adults alike. International studies have shown that television viewing is associated with an increased incidence of new cases of obesity, as well as with a decrease in success rates for obesity intervention.7 Television viewing exposes children to food marketing, increases opportunities for snacking on high-energy foods and drinks, decreases opportunities for physical activity, and reinforces sedentary behaviour. There are as yet no clear data linking viewing of interactive videos, or using computers or other electronic media, with the development of obesity, although they are likely to be associated.
Dietary intake: The increased prevalence of obesity in recent decades may have partly resulted from an increased consumption of high-fat foods or sweetened drinks, although the evidence for a clear effect of diet is not strong. In young children, parental influence on food selection is strong. In older children and adolescents peer influence is also important. Less desirable meal patterns, such as frequent snacking, also appear to be related to established obesity.
Other risk factors for obesity in childhood and adolescence include:
Early infant feeding: Breastfeeding is possibly protective for the development of obesity.8
Parental obesity, eating patterns, and attitudes: Parental obesity more than doubles the risk of adult obesity among both obese and non-obese children.9 Dietary disinhibition in the mothers of preschoolers is associated with subsequent excess weight gain in their daughters,10 and a 6-year outcome study of children showed that parental dietary disinhibition is associated with greater increases in body fatness.11 Parents who strongly encourage their children to eat have heavier children.12
Early adiposity rebound: Earlier adiposity rebound is associated with increased body fatness in adolescence.
Socioeconomic status: In some developed countries, poorer children or those who live in rural settings are more at risk of obesity, whereas in countries undergoing economic transition childhood obesity is associated with a more affluent lifestyle and with living in urban regions.
Ethnicity: Data from the United States show that there is an increased risk of obesity in Native Americans and Hispanic Americans compared with white Americans, although these differences may be largely related to differences in socioeconomic status.
Underlying medical disorders: Secondary obesity may occur with medical conditions, including hypothyroidism, hypercortisolism, growth hormone deficiency and hypothalamic damage.
Prescription drugs: Some drugs may contribute to obesity. These include glucocorticoids, antipsychotic drugs (eg, risperidone) and some antiepileptic medications.
Childhood obesity is a chronic paediatric disease with possible immediate and long-term complications involving many body systems (Box 1). The National Health and Medical Research Council (NHMRC) Clinical practice guidelines for the management of overweight and obesity in children and adolescents13 provides a comprehensive review of the complications of childhood and adolescent obesity. We will briefly discuss insulin resistance and type 2 diabetes, and steatohepatitis.
Obesity in childhood and adolescence may be associated with insulin resistance. Without appropriate medical intervention, severe obesity and insulin resistance may progress to type 2 diabetes, which now accounts for up to 50% of newly diagnosed diabetes in some paediatric populations (eg, African Americans).14 Acanthosis nigricans is considered to be a marker of insulin resistance in children and adolescents (Box 2).
Non-alcoholic steatohepatitis (NASH) was first described in 1979 in adults. NASH also occurs in childhood, but is less well characterised. Liver biopsies from obese prepubertal children with NASH may show fatty change, inflammation and fibrosis, with progression to necrosis and cirrhosis.15 Most cases of paediatric NASH are described in older children and adolescents. Elevated serum transaminase levels should raise suspicion of NASH in an obese child or adolescent. If NASH is suspected, referral to a centre specialising in the management of childhood obesity is recommended.
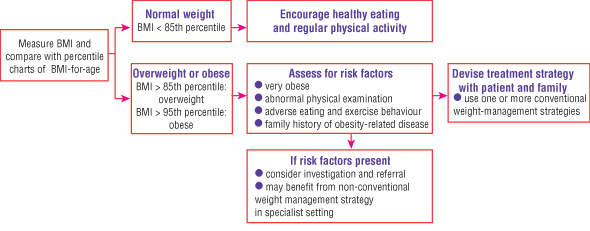
The decision to further investigate obesity should be based on a combination of adiposity (BMI percentile), presence of complications and other risk factors (including family history and lifestyle factors), and the family’s and young person’s willingness to undertake lifestyle change (Box 3 and Box 4).
Established obesity in children and adolescents has proven difficult to treat. A recent Cochrane review of the management of obesity in children and adolescents has shown that there are a limited number of randomised controlled trials.20 Common strategies in the treatment of paediatric obesity for which there is at least some evidence are given in Box 5.
Treatment programs for obesity should take into account the influence of the child’s family on food choices and level of physical activity. Studies on long-term maintenance of weight loss have shown the importance of altered food habits within the whole family, support for the child, and parental praise for changed eating behaviour and physical activity.21
Treatment of preadolescent obesity with parents as the exclusive agents of lifestyle change appears more effective than targeting the child alone.22 There has been some success with separate sessions for adolescents and parents and structured programs flexible enough to allow input from adolescents.23 There have even been short-term positive outcomes with a phone- and email-based program for adolescent weight management.24
There is some concern that rigid restriction or control of a child’s food intake may trigger disordered eating or, in the young child, reduction in linear height growth. Less prescriptive, lower-energy diets are now used, with an emphasis on all members of the family moving to healthier eating patterns.25 The aim is to provide a flexible program to help the family and the child to make sustainable changes in food choices and eating habits. In general, dietary interventions should emphasise energy reduction, lower-fat food choices, increased vegetable and fruit intake, healthier snacks and decreased portion sizes. Water should be used as the main beverage, and drinks with high sugar content, including soft drinks and fruit drinks, should be limited. The effect of these interventions should be a reduction in total energy intake by reducing the energy density of the diet. Changes in eating habits, shopping practices and types of food for the whole family will support a child’s ability to self-regulate his or her food intake.
Evidence-based practice tips
Parents influence food choices and other eating behaviours in their children. Disordered eating in a parent may be associated with excess body weight in the child (III-3).10,11
The prevalence of type 2 diabetes is increasing in children and adolescents, particularly in certain ethnic groups. This increase appears associated with high levels of obesity in these populations (III-2).14
There is short-term evidence that reducing sedentary behaviours in obese children is as effective for weight management as increased activity (III-3).27
There is some limited evidence that a weight management program for children and adolescents can be delivered in a variety of settings and achieve similar outcomes. The majority of such programs use a group format (III-3).2
Levels of evidence (I–IV) are derived from the National Health and Medical Research Council’s system for assessing evidence.35
Enhanced physical activity (both planned and incidental/lifestyle) is an important component of weight management programs for obese children, although, as with dietary intake, there is no evidence as to the most effective physical activity prescription. In a study of the long-term effectiveness of physical activity interventions, the lifestyle exercise group maintained better weight than the programmed exercise group.26 There is some evidence that a reduction in sedentary behaviour is an effective component of a weight management program for obese children.27
Behaviour modification is a component of most weight management programs. A variety of different behaviour modification strategies have been used in obesity treatment studies (Box 5).28
Several types of interventions have been used to treat childhood obesity: individual counselling sessions, group programs, and sessions given by different types of healthcare professionals.2 Interventions have been conducted in different settings, including primary care, community health centres, tertiary institutions and holiday camps. There is some evidence for the effectiveness of group programs, holiday camps and email- and phone-based behavioural interventions.24
In general, very low calorie diets, whether they involve normal food items or non-food substitutes, produce rapid weight loss in adolescents. This may be of benefit when there is significant medical comorbidity, but should be conducted in a specialised centre.13 Very low calorie diets are never indicated for children.
Sibutramine (Reductil, Abbott): Berkowitz et al29 performed a randomised controlled trial of sibutramine in 82 adolescents with BMI 32–44. The addition of sibutramine to a comprehensive behavioural program induced significantly more weight loss than the behavioural program and placebo; however, 23/82 required a lower dose and 10/82 ceased treatment because of hypertension.
Orlistat (Xenical, Roche): Short-term studies of orlistat in obese adolescents showed good tolerability and weight loss.30
The NHMRC guidelines13 suggest that use of both sibutramine and orlistat in obese adolescents with complications should take place only in a specialist centre, and only when there is a reasonable expectation of benefit over risk.
Metformin: Two recent, small controlled trials of the use of metformin in adolescents with hyperinsulinaemia and obesity but no diabetes found that the metformin group had a reduction in hyperinsulinaemia and a modest weight loss compared with the non-metformin group.31,32
The NHMRC guidelines13 state that metformin has a potential role in therapy in these adolescents, and that metformin therapy should be considered in obese adolescents with significant hyperinsulinaemia and a family history of diabetes.
A recently published Cochrane review of interventions for preventing obesity in children concluded that there are “limited high quality data on the effectiveness of prevention programs”.33 However, the published studies do highlight the potential of combining a reduction in sedentary behaviour and an increase in physical activity, as well as the utility of a school-based setting.
The randomised-controlled-trial approach may be inappropriate for large-scale or comprehensive obesity-prevention studies. New approaches to assessing the effectiveness of “real world” obesity-prevention interventions are being developed. Several community-based interventions aimed at preventing obesity and incorporating such approaches are currently under way in a number of countries, including Australia and New Zealand.
Swinburn et al34 introduced the concept of the obesogenicity of modern environments, with the influences promoting the development of obesity operating on micro- and macroenvironmental levels, and having physical, economic, political and sociocultural aspects. Elements in the microenvironment that influence physical activity and food intake include settings where people live, work and study; community facilities (shopping malls, clubs, churches); food retailers and outlets (supermarkets, canteens, lunch bars, restaurants); recreational facilities (parks, pools, gyms); type of neighbourhood (street safety, cycle paths, footpaths); and access to local primary healthcare.
At the macroenvironmental level (ie, beyond the sphere of influence of individuals) factors affecting dietary intake and physical activity include food production, importation, marketing and distribution; urban and rural development (town planning); transport systems (public transport); and health systems. Assessing the environment of a given community using this framework indicates the opportunities for preventive strategies. As yet, there are few successful examples of multifaceted, large-scale interventions to guide obesity-prevention programs. Such interventions need to be supported by adequate resourcing and significant community ownership.
1 Complications of obesity in children and adolescents
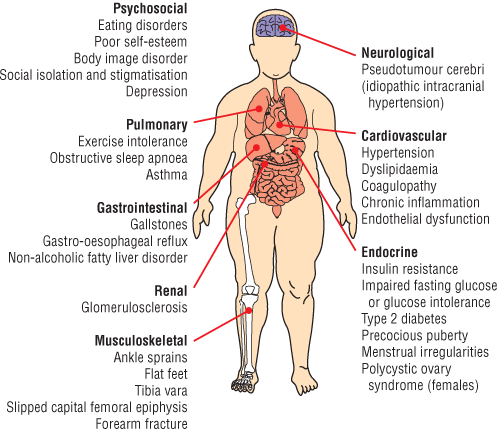
Adapted from reference 2 (Lancet 2002; 360: 475), with permission from Elsevier.
2 Acanthosis nigricans
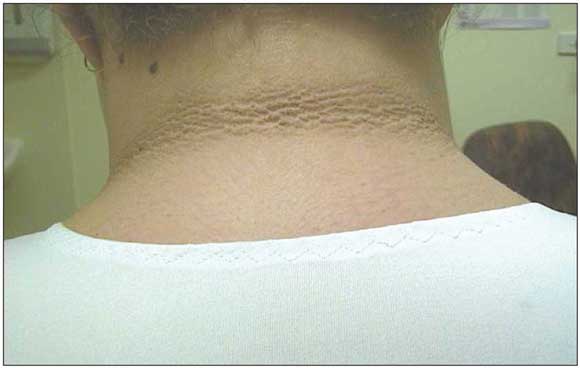
Acanthosis nigricans — a thickened, pigmented skin lesion in flexures and on the dorsum of hands — is associated with insulin resistance.
3 Assessment of the obese child or adolescent
History |
|||||||||||||||
General history
Weight history
Complication history
Asthma |
Family’s weight and metabolic history
Lifestyle history
|
||||||||||||||
Examination |
|||||||||||||||
|
Physical examination findings requiring further assessment:†
|
||||||||||||||
* Waist circumference can be used as a proxy for abdominal obesity, with its increased risk of metabolic complications. There are no specific cut-off points for waist circumference for age to categorise abdominal obesity in children and adolescents. However, if the waist circumference of a child or adolescent falls above the acceptable waist circumference cut-off points for adults19 (increased risk: men > 94 cm, women > 80 cm), then the child can be readily classified as having abdominal obesity. This imperfect, but practical, approach will, of course, lead to an underestimation of abdominal obesity in paediatric patients. Waist circumference may be most useful in clinical assessment of individual patients when measured serially and used to monitor change over time. †For most overweight children, investigations are not necessary. However, if a child or adolescent is very obese, has a family history of metabolic disease, or a history and examination suggesting the presence of complications of obesity, then a fasting lipid profile, fasting levels of insulin and glucose, and liver function tests (to assess the presence of non-alcoholic steatohepatitis) should be considered. Endocrinological tests are not required, unless there is other evidence of endocrine disease or short stature. Consider referral for review at a specialist centre. |
|||||||||||||||
5 Conventional management of childhood obesity
Family involvement
Behaviour change needs to involve the whole family, and provide support for the child
Developmentally appropriate approach
Preadolescent children: Focus on parents as the agents of change
Adolescents: Parents and adolescents attend separate sessions
Dietary change
Avoid severe food restriction
Reduce energy intake
Reduce portion size
Select foods with lower fat content and low glycaemic index
Increase vegetable and fruit intake
Reduce high-sugar foods and drinks
Use water as the main beverage
Increased physical activity
Incidental activity
Lifestyle activity
Exercise programs
Active transport (walking, cycling)
Decreased sedentary behaviour
Reduce time spent watching television, playing computer games, using other electronic media
Encourage alternatives to motorised transport
Behaviour modification
Build confidence
Assess readiness for change
Change habits associated with eating and physical activity
Set realistic goals for lifestyle change
- Jennifer A Batch1
- Louise A Baur2
- 1 Department of Endocrinology and Diabetes, Royal Children’s Hospital, Brisbane, QLD.
- 2 The Children’s Hospital at Westmead and Discipline of Paediatrics and Child Health, University of Sydney, Sydney, NSW.
- 1. World Health Organization. Nutrition. Controlling the global obesity epidemic. Available at: www.who.int/nut/obs.htm (accessed Nov 2004).
- 2. Ebbeling CB, Pawlak DB, Ludwig DS. Childhood obesity: public health crisis, common sense cure. Lancet 2002; 360: 473-482.
- 3. Booth ML, Wake M, Armstrong T, et al. The epidemiology of overweight and obesity among Australian children and adolescents 1995-7. Aust N Z J Public Health 2001; 25: 162-169.
- 4. Magarey AM, Daniels LA, Boulton TJ. Prevalence of overweight and obesity in Australian children and adolescents: reassessments of 1985 and 1995 data against new standard international definitions. Med J Aust 2001; 174: 561-564. <MJA full text>
- 5. CDC 2002. Growth charts: United States. Advance data number 314. 4 December Revised. Atlanta, Ga: Centers for Disease Control and Prevention.
- 6. Chagnon YC, Rankinen T, Snyder EE, et al. The human obesity gene map: the 2002 update. Obes Res 2003; 11: 313-367.
- 7. Robinson TN. Television viewing and childhood obesity. Pediatr Clin North Am 2001; 48: 1017-1025.
- 8. Butte NF. The role of breast feeding in obesity. Pediatr Clin North Am 2001; 48: 189-198.
- 9. Whitaker RC, Wright JA, Pepe MS, et al. Predicting obesity in young adulthood from childhood and parental obesity. N Engl J Med 1997; 337: 869-873.
- 10. Cutting TM, Fisher JO, Grimm-Thomas K, et al. Like mother, like daughter: familial patterns of overweight are mediated by mother’s dietary disinhibition. Am J Clin Nutr 1999; 69: 608-613.
- 11. Hood MY, Moore LL, Sundarajan-Ramamutri A, et al. Parental attitudes and the development of obesity in children: the Framingham Children’s study. Int J Obes 2000; 24: 1319-1325.
- 12. Klesges RC, Caotes TJ, Brown G, et al. Parental influences on children’s eating behaviours and relative weight. J Appl Behav Analysis 1983; 16: 371-378.
- 13. National Health and Medical Research Council. Clinical practice guidelines for the management of overweight and obesity in children and adolescents. Canberra: NHMRC, 2003. Available at: www.health.gov.au/internet/wcms/publishing.nsf/Content/obesityguidelines-guidelines-children.htm/$FILE/children.pdf (accessed Nov 2004).
- 14. Goran MI, Ball GD, Cruz ML. Obesity and risk of type 2 diabetes and cardiovascular disease in children and adolescents. J Clin Endocrinol Metab 2003; 88: 1417-1427.
- 15. Manton ND, Lipsett J, Moore DJ, et al. Non-alcoholic steatohepatitis in children and adolescents. Med J Aust 2000; 173: 476-479. <MJA full text>
- 16. Marshall WA, Tanner JM. Variations in pattern of pubertal changes in girls. Arch Dis Child 1969; 44: 291-303.
- 17. Marshall WA, Tanner JM. Variations in the pattern of pubertal changes in boys. Arch Dis Child 1970; 45: 13-23.
- 18. Update on the 1987 Task Force Report on high blood pressure in children and adolescents: a working group report from the National High Blood Pressure Working Group on hypertension control in children and adolescents. Pediatrics 1996; 98: 649-658.
- 19. Han TS, Leer EM, Seidell JA, et al. Waist circumference action levels in the identification of cardiovascular risk factors: prevalence study in a random sample. BMJ 1995; 311: 1401-1405.
- 20. Summerbell C, Kelly S, Waters L, et al. Interventions for treating obesity in childhood (Cochrane review). The Cochrane Library, Issue 3, 2003. Oxford: Oxford Update Software.
- 21. Epstein LH, Myers MD, Raynor HA, Saelens BE. Treatment of paediatric obesity. Pediatrics 1998; 101 (3 Pt 2): 554-570.
- 22. Golan M, Fainaru M, Weizman A. Role of behaviour modification in the treatment of childhood obesity with the parents as the exclusive agents of change. Int J Obes Rel Metab Disord 1998; 22: 1217-1224.
- 23. Brownell KD, Kelman JH, Stunkard AJ. Treatment of obese children with and without their mothers: changes in weight and blood pressure. Pediatrics 1983; 71: 515-523.
- 24. Saelens BE, Sallis JF, Wiffley DE. Behavioural weight control for overweight adolescents initiated in primary care. Obes Res 2002; 10: 20-32.
- 25. Epstein LH, Gordy CC, Raynor HA, et al. Increasing fruit and vegetable intake and decreasing fat and sugar intake in families at risk of childhood obesity. Obes Res 2001; 9: 171-178.
- 26. Epstein LH, Wing RR, Koeske R, et al. A comparison of lifestyle change and programmed aerobic exercise on weight and fitness changes in obese children. Behav Ther 1982; 13: 651-665.
- 27. Reilly JJ, McDowell ZC. Physical activity interventions in the prevention and treatment of paediatric obesity: systematic review and critical appraisal. Proc Nutr Soc 2003; 62: 611-619.
- 28. Floodmark C-E, Lissau I. Psychotherapy. In: Burniat W, et al, editor. Child and adolescent obesity: causes and consequences, prevention and management. Cambridge: Cambridge University Press, 2002: 327-344.
- 29. Berkowitz RJ, Wadden TA, Tershakovec AM, et al. Behavioural therapy and sibutramine for the treatment of adolescent obesity. JAMA 2003; 289: 1805-1812.
- 30. McDuffie JR, Calis KA, Uwaifo GI, et al. Three month tolerability of orlistat in adolescents with obesity related co-morbid conditions. Obes Res 2002; 10: 642-650.
- 31. Freemark M, Bursey D. The effects of metformin on body mass index and glucose tolerance in obese adolescents with fasting hyperinsulinaemia and family history of type 2 diabetes. Pediatrics 2001; 107: E55.
- 32. Kay JP, Alemzadeh R, Langley G, et al. Beneficial effect of metformin in normoglycaemic morbidly obese adolescents. Metabolism 2001; 50: 1457-1461.
- 33. Campbell K, Waters E, O’Meara S, et al. Interventions for preventing obesity in children (Cochrane review). The Cochrane Library, 2002, Issue 2. Oxford: Oxford Update Software.
- 34. Swinburn B, Egger G, Fezeela R. Dissecting obesogenic environments: the development and application of a framework for identifying and prioritising environmental interventions for obesity. Prev Med 1999; 29: 563-570.
- 35. National Health and Medical Research Council. How to use the evidence: assessment and application of scientific evidence. Handbook series on preparing clinical practice guidelines. Table 1.3: Designation of levels of evidence. Canberra: NHMRC, February 2000: 8. Available at: www.health.gov.au/nhmrc/publications/pdf/cp69.pdf (accessed Sep 2004).







Abstract
Obesity in children and adolescents has reached alarming levels — 20%–25% of children and adolescents are overweight or obese, and 4.9% of boys and 5.4% of girls are obese.
Rates of obesity have increased significantly in Australia from 1985 to 1995, with the prevalence of overweight doubling and obesity trebling.
Body mass index (related to reference standards for age and sex) is recommended as a practical measure of overweight and obesity in children, and is used in monitoring individual progress in clinical practice.
Obesity in childhood and adolescence may be associated with a range of medical and psychological complications, and can predispose individuals to serious health problems in adult life, including type 2 diabetes, hypertension, dyslipidaemia and non-alcoholic steatohepatitis.
Obesity interventions for which there is some evidence include family support, a developmentally appropriate approach, long-term behaviour modification, dietary change, and increased physical activity and decreased sedentary behaviour.
Prevention of obesity in children and adolescents requires a range of strategies involving changes in both the microenvironment (eg, housing, neighbourhoods, recreational opportunities) and the macroenvironment (eg, food marketing, transport systems, urban planning).