Healthcare is delivered using systems of interdependent processes of care. These systems are complex, variation in care is great, and errors are common.1 In other industries involving complex processes, analysis of service delivery systems has led to simplification of systems and the use of reminders and checklists, which have reduced variation in service delivery and error rates.2
Given the wide variety of medical conditions and individual patient characteristics and needs, it is unlikely that this approach can be applied to all medical care. However, a systems approach using relevant clinical pathways may be used selectively in managing patients with common medical conditions. Checklists and reminders within these pathways prompt the appropriate management at each stage of the patient’s condition.
Evidence-based guidelines are available to provide guidance for health professionals in the care of patients. These can be complex, and multiple guidelines often exist for the one clinical condition. Also, guidelines may not be readily available or easy to use in acute care situations. To overcome these difficulties, guidelines could be simplified and incorporated into everyday hospital practice by translating them into clinical pathways integrated into the patient’s medical record.
In this study, our aim was to determine whether using checklists and reminders in clinical pathways could increase compliance with evidence-based guidelines.
The hospital has a comprehensive clinical risk management program that has been developed over 14 years.3,4 The program uses medical record review and clinical incident reporting to detect adverse events. These adverse events are analysed and appropriate action is taken to prevent them recurring. The clinical pathway program described here was developed as a component of the hospital’s clinical risk management program.
A senior nurse with experience in intensive care and administration was appointed as clinical pathway coordinator. With clinical risk management well established at the hospital, champions of clinical and executive quality improvement were readily identified. They were asked to participate in developing and implementing pathways.
Clinical conditions suitable for pathway development were chosen according to the following criteria: the clinical risk management program had consistently detected adverse events in the treatment of the condition; the condition was treated frequently in the hospital; the consequences of treating the condition suboptimally were significant; and/or the average length of stay for patients treated for the condition was significantly greater than the Victorian state average.
For each clinical condition chosen, a multidisciplinary team of 12–18 members involved in care delivery (including nursing, medical, pharmacy and allied health staff) was selected to develop the pathway and oversee its implementation. Before the first meeting of each team, the clinical pathway coordinator collected information about similar pathways developed at other hospitals, information from journals and the Internet about what constituted best clinical practice, and the average length of stay in Victorian hospitals for the clinical area chosen.
At weekly team meetings, draft pathways were developed to meet local conditions and needs. The pathways contained information required for clinical decision-making (including management algorithms) and evidence-based guidelines (eg, criteria for eligibility for thrombolysis in acute myocardial infarction [AMI], and swallow assessment in stroke). Where possible and appropriate, such information was developed into checklists and reminders for the entire continuum of care, including emergency management, care for each day of the patient’s stay in hospital, and discharge planning. This information was designed to be easily completed by staff and incorporated into the patient’s admission medical record. Draft pathways were circulated for comment throughout the hospital, especially to medical staff, and some draft pathways were tested in trial runs to improve their design.
Extensive education of the staff using each pathway was undertaken before the pathway was formally launched. Further education sessions were then held to reinforce important areas of patient care.
After a clinical pathway was used, the patient’s medical record for that admission was audited manually, using the process measures chosen. Variations from the pathway guidelines were noted, and the information was given to the appropriate multidisciplinary team. Where improvement in the process measures had not occurred, the team conducted an analysis and took corrective action. Such action included altering pathways to make them clearer and easier to use, implementing further reminder systems, leaving messages in staff communication books, and the pathway coordinator attending ward meetings and holding further education sessions. Several cycles of measurement, analysis, action and further measurement were undertaken for each pathway as they were progressively modified.
The changes achieved in process measures were regularly communicated in graphical form to all hospital staff by means of a monthly newsletter and by reporting to clinical meetings of medical, nursing and allied health staff. The results were also reported to the hospital’s peak quality committee and board of management.
In this program, 29 pathways were developed. Two of the longer-established pathways at the hospital (ST-elevation AMI and stroke) are described in detail in this article.
Key process measures, known from large studies to have a considerable positive impact on patient outcome, were chosen for each pathway. Significant changes in patient outcome would have been hard to detect in the short term in our study, owing to small patient numbers.
The ST-elevation AMI clinical pathway was introduced on 1 October 2000, and the stroke clinical pathway on 1 June 2000. Our study included AMI patients admitted between 1 January and 31 December 1999 (pre-pathway) and between 1 October 2000 and 31 December 2002 (post-pathway), and stroke patients admitted between 31 July 1999 and 30 April 2000 (pre-pathway) and between 1 June 2000 and 31 December 2002 (post-pathway). We measured the degree of compliance with key process measures before and after the introduction of clinical pathways. We also assessed whether compliance was maintained over the 2 years following introduction of the pathway program.
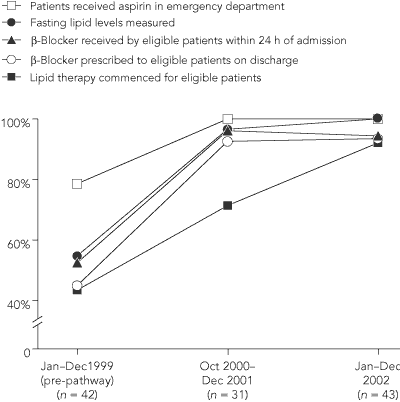
The key process measures selected for the ST-elevation AMI pathway were the proportions of (a) patients who received aspirin in the emergency department or before presentation; (b) eligible patients who received a β-blocker within 24 hours of admission; (c) patients whose fasting lipid levels were measured on the first day of admission; (d) eligible patients (ie, those with total cholesterol level > 4mmol/L) who commenced lipid-lowering therapy; and (e) eligible patients who were prescribed a β-blocker on discharge.
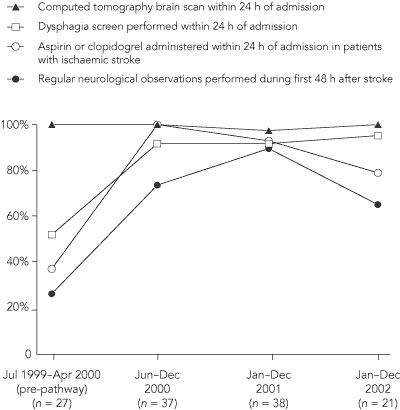
The key process measures selected for the stroke pathway were the proportions of (a) patients who had a computed tomography (CT) brain scan within 24 hours of admission; (b) patients who were screened for dysphagia within the first 24 hours of admission; (c) patients with ischaemic stroke who were given aspirin or clopidogrel within 24 hours of admission; and (d) patients who underwent regular neurological observation during the first 48 hours after the stroke.
Statistical analyses were performed using Stata software.5
Results of the key process measures before and after introduction of each clinical pathway are shown in Box 1.
Of 116 patients with ST-elevation AMI assessed in the study, 42 were admitted before the pathway was introduced (Jan–Dec 1999), 31 in the early post-pathway period (Oct 2000–Dec 2001), and 43 at 2-year follow-up (Jan–Dec 2002). The proportion of these patients who received the key interventions increased significantly after introduction of the pathway, and the increases were maintained over the following 2 years (Box 2).
Of 123 patients with stroke assessed in the study, 27 were admitted before the pathway was introduced (Jul 1999–Apr 2000), 37 in the early post-pathway period (Jun–Dec 2000), 38 at 1-year follow-up (Jan–Dec 2001) and 21 at 2-year follow-up (Jan–Dec 2002). Apart from the proportion of patients undergoing a CT brain scan within 24 hours of admission (which was already 100% before the pathway was introduced), the proportions of patients receiving all other key interventions increased in the first 6 months after the pathway was introduced and were maintained over the following 2 years (Box 3).
Our study demonstrates that adherence to processes that improve clinical outcomes for patients — and therefore quality of care — can be improved and sustained by the use of checklists and reminders in clinical pathways.
Factors that contributed to the success of the clinical pathway program in the hospital are summarised in Box 4. A strength of our study was that it measured not only the effect of implementing clinical pathways, but also the sustainability of adherence to the key processes over a 2-year period after implementation.
Weaknesses of our study were that it did not measure patient outcomes, adjust for the severity of patients’ conditions or include a control hospital. Thus, factors other than the introduction of clinical pathways may have influenced the use of some processes of care. Given the fairly small size of the hospital and the relatively low number of patients treated with particular medical conditions, it would have been difficult to undertake a randomised controlled trial. Furthermore, our results — based on a secondary referral hospital with a small and relatively stable clinical staff — may not be generalisable to a larger tertiary centre, where introducing clinical pathways would be logistically more complex.
Our results after the introduction of clinical pathways compare favourably with other multihospital observational studies in which pathways were not uniformly used. In a US study of patients with AMI,6 85% of eligible patients received aspirin and 69% β-blockers in the first 24 hours (compared with 100% and 95.1%, respectively, in our study). In an Australian study of stroke management in eight tertiary hospitals,7 57% of eligible patients received aspirin within 24 hours and 78% received antiplatelet therapy (compared with 92.2% receiving aspirin or clopidogrel during the first 24 hours in our study).
It has been noted before that sustaining change in clinical behaviour is difficult.8 In the stroke management component of our study, adherence to some key interventions was maintained for 18 months but then fell, albeit to a level still higher than before the pathway’s introduction. In our experience, maintaining improvements over time requires continuous vigilance by the pathway coordinator and reinforcement of the clinical importance of pathways for both nursing and medical staff.
At Wimmera Base Hospital, all new resident medical officers now attend a tutorial early in their rotation about the importance of clinical pathways and their role in complying with them. This information is later reinforced if compliance begins to fall. Nursing staff, as a group, have greater long-term employment stability at the hospital and thus are the cornerstone of the clinical pathway program. They initiate pathways in the emergency department and prompt resident medical staff to follow the processes outlined in the pathways for each day of the patient’s admission.
We believe the methods used in our study provide a framework for developing and implementing clinical pathways that could be used by other hospitals, with modification to meet their local conditions and needs. Sufficient resources would be needed to address the factors that influence successful implementation of an intervention program. Some of these factors are difficult to quantify. The culture in a hospital is important, although difficult to change. As a starting point, hospitals should ensure that continual improvement in the quality of patient care is a major part of their strategic plan. We believe most hospitals will have some clinicians who are passionate about high-quality care and will be willing champions in driving clinical pathway programs.
Further research is required to determine the optimal clinical pathway format to maximise compliance by clinicians. The clinical pathways developed and used in our study could be computerised for use with Palm Pilot (hand-held computer) technology. Such an approach would be most suitable for hospitals in which there is already an electronic medical record system.
Pathways could also be expanded across the continuum of care and could include not only checklists and reminders for managing hospital inpatients, but also protocols for managing patients in primary care.
1 Results of key process measures before and after introduction of two clinical pathways at Wimmera Base Hospital, Victoria
|
Number (%) of patients whose treatment complied with key process measures |
|
|||||||||||||
Key process measures |
Before introducing clinical pathway* |
After introducing clinical pathway* |
Difference in proportions |
||||||||||||
ST-elevation acute myocardial infarction |
(n = 42) |
(n = 74) |
|
||||||||||||
Patients given aspirin in emergency department |
33/42 (78.6%) |
71/71† (100%) |
21.4% (7.3%–32.7%) |
||||||||||||
Eligible patients given β-blocker within 24 h of admission |
21/40 (52.5%) |
59/62 (95.2%) |
42.7% (26.3%–59.0%) |
||||||||||||
β-Blocker prescribed for eligible patients on discharge |
18/40 (45.0%) |
54/58 (93.1%) |
48.1% (31.4%–64.8%) |
||||||||||||
Fasting lipid levels measured |
23/42 (54.8%) |
67/68‡ (98.5%) |
43.7% (28.4%–59.1%) |
||||||||||||
Lipid therapy commenced for eligible patients |
10/23 (43.5%) |
50/59 (84.7%) |
41.2% (19.0%–63.5%) |
||||||||||||
Stroke |
(n = 27) |
(n = 96) |
|
||||||||||||
Computed tomography brain scan done within 24 hours of admission |
27/27 (100%) |
95/96 (99.0%) |
–1.0% (–4.7% to 10.0%) |
||||||||||||
Dysphagia screen performed within 24 h of admission |
14/27 (51.8%) |
86/93§ (92.5%) |
40.7% (21.0%–60.2%) |
||||||||||||
Patients with ischaemic stroke given aspirin or clopidogrel within 24 h of admission |
7/19 (36.8%) |
71/77 (92.2%) |
55.4% (32.9%–77.9%) |
||||||||||||
Regular neurological observations performed during first 48 h after stroke |
7/27 (25.9%) |
72/92¶ (78.3%) |
52.4% (33.8%–70.9%) |
||||||||||||
* The denominator for each category was the number of eligible patients. † One patient was allergic to aspirin; 1 died in the emergency department; 1 was already taking warfarin. ‡ Six patients died before Day 1, when the stroke clinical pathway indicated that fasting lipid levels were to be checked. § Three patients, on presentation, required intubation and ventilation. ¶ Four patients presented to hospital more than 48 h after having a stroke. |
|||||||||||||||
2 Proportion of patients with ST-elevation acute myocardial infarction who received key interventions before and after introduction of the clinical pathway (on 1 Oct 2000)
3 Proportion of patients with stroke who received key interventions before and after introducing the clinical pathway (on 1 Jun 2000)
4 Factors contributing to successful development and implementation of the clinical pathway program at Wimmera Base Hospital
Having an established clinical risk management culture in the hospital.
Having adequate funding to appoint a senior nurse to coordinate the program, to pay staff participating in teams for additional work, and to pay replacement staff to carry out normal duties.
Involving multidisciplinary teams in the development of clinical pathways, thus improving communication and teamwork between health professionals from different clinical disciplines and giving ownership of each pathway to all disciplines providing care.
Undertaking a literature search to determine best clinical practice for each medical condition and adapting the evidence for local conditions before incorporating it into the clinical pathway.
Detailing the processes of care in each pathway in the form of checklists and reminders.
Involving key medical staff early in the pathway development process and inviting all medical staff to comment on individual pathways before their implementation.
Incorporating clinical pathways into the patient medical record and ensuring they are completed by all clinical staff providing care.
Enlisting the help of clinical and executive champions to guide the pathway program through the hospital’s clinical and administrative systems.
Gaining the support of board of management champions to promote the program to the hospital’s quality committee and at board level.
Providing regular feedback of program results to all clinical staff, major clinical groups and appropriate hospital committees.
- Alan M Wolff1
- Sally A Taylor2
- Janette F McCabe3
- Clinical Risk Management Unit, Wimmera Health Care Group, Horsham, VIC.
We wish to thank the staff and board of management of the Wimmera Health Care Group for their continued support and participation in the program. We also thank Professor Edward Janus, Visiting Physician, and Mr Ian Campbell, Visiting Surgeon, for their valued participation in developing and promoting clinical pathways and in reviewing our manuscript.
Our study was supported by the Victorian Managed Insurance Authority and the Victorian Department of Human Services through their Designing Care initiative. These funding sources had no role in the study design, data collection, analysis and interpretation, or in writing this article.
- 1. Nolan TW. Understanding medical systems. Ann Intern Med 1998; 128: 293-298.
- 2. Leape LL. Error in medicine. JAMA 1994; 272: 1851-1857.
- 3. Wolff AM, Bourke J. Reducing medical errors: a practical guide. Med J Aust 2000; 173: 247-251.
- 4. Wolff AM, Bourke J, Campbell IA, Leembruggen DW. Detecting and reducing hospital adverse events: outcomes of the Wimmera clinical risk management program. Med J Aust 2001; 174: 621-625. <MJA full text>
- 5. Stata statistical software, version 7.0. College Station, Tex: Stata Corporation, 2001.
- 6. Jencks SF, Huff ED, Cuerdon T. Change in the quality of care delivered to Medicare beneficiaries, 1998–1999 to 2000–2001. JAMA 2003; 289: 305-312.
- 7. Duffy BK, Phillips PA, Davis SM, et al. Evidence-based care and outcomes of acute stroke managed in hospital specialty units. Med J Aust 2003; 178: 318-323. <MJA full text>
- 8. Tobin SN, Campbell DA, Boyce NW. Durability of response to a targeted intervention to modify clinician transfusion practices in a major teaching hospital. Med J Aust 2001; 174: 445-448.





Abstract
Objectives: To determine whether the quality of hospital inpatient care can be improved by using checklists and reminders in clinical pathways.
Design: Comparison of key indicators before and after the introduction of clinical pathways incorporating daily checklists and reminders of best practice integrated into patient medical records.
Setting and participants: The study, at Wimmera Base Hospital in Horsham, Victoria, included patients admitted between 1 January 1999 and 31 December 2002 with ST-elevation acute myocardial infarction (AMI) and patients admitted between 31 July 1999 and 31 December 2002 with stroke.
Main outcome measures: Compliance with key process measures determined as best practice for each clinical pathway.
Results: 116 patients with AMI and 123 patients with stroke were included in the study.
ST-elevation AMI. After introducing the clinical pathway program, percentage-point increases for treatment compliance were 21.4% (95% CI, 7.3%–32.7%) for patients receiving aspirin in the emergency department; 42.7% (95% CI, 26.3%–59.0%) for eligible patients receiving β-blockers within 24 h of admission; 48.1% (95% CI, 31.4%–64.8%) for eligible patients being prescribed β-blockers on discharge; 43.7% (95% CI, 28.4%–59.1%) for patients having fasting lipid levels measured; and 41.2% (95% CI, 19.0%–63.5%) for eligible patients having lipid therapy.
Stroke. After introducing the clinical pathway program, percentage-point increases for treatment compliance were 40.7% (95% CI, 21.0%–60.2%) for dysphagia screening within 24 h of admission; 55.4% (95% CI, 32.9%–77.9%) for patients with ischaemic stroke receiving aspirin or clopidogrel within 24 h of admission; and 52.4% (95% CI, 33.8%–70.9%) for patients having regular neurological observations during the first 48 h after a stroke. There was a fall of 1.0 percentage point (ie, a difference of –1% [95% CI, –4.7% to 10.0%]) in the proportion of patients having a computed tomography brain scan within 24 h of admission.
Conclusion: Significant improvements in the quality of patient care can be achieved by incorporating checklists and reminders into clinical pathways.