There is little documented research examining disparities in cancer services between the Indigenous and non-Indigenous populations of Australia. Surgical procedures for cancer have received almost no attention, although differences have been seen between Indigenous patients and other patients in utilisation of hospital procedures, including those for all neoplasms combined.1,2 Inequalities in access to cardiovascular healthcare have also been reported.3 Furthermore, living in a rural area in Australia has been shown to affect cancer treatment patterns,4,5 and being treated in a rural hospital has been shown to worsen patient outcomes.4,5 The finding of a lower total procedure rate in the Indigenous population1,2 is consistent with these findings.
Our exploratory study aimed to examine possible disparities between the Indigenous and non-Indigenous populations of Western Australia (WA) in the uptake of cancer surgery for three common cancers (breast, prostate and lung), using administrative data collected routinely over 20 years.
The WA Record Linkage Project was used to extract all hospital morbidity, cancer registrations and death records for all residents of WA who:
had a mention in any record of cancer of the breast (codes, ICD-9 1746 or ICD-10 C507), prostate (ICD-9 185 or ICD-10 C61) or lung (ICD-9 162 or ICD-10 C33); or,
if there was no cancer registration, had a hospital record with the cancer identified together with an associated procedure.
Patients were included if they had an incident date for breast cancer between 1 January 1982 and 31 December 2000, or, for prostate or lung cancer, between 1 January 1982 and 31 December 2001. As breast cancer data were extracted earlier, the 2001 data were incomplete and not used.
The Record Linkage Project contains data for each patient for each hospital admission. The first record that mentioned the cancer of interest was labelled the index admission; any cancer or death record details were added to this record.
Patient age and marital status at the time of the index admission were used to adjust for confounding in the logistic regression models. Other variables were created for use in the regression model, including:
Indigenous status. Due to variability in the recording of this status, any mention in any hospital, cancer or death record was added to the index admission record.
Calendar period. For breast cancer, the date of diagnosis was categorised as 1982–1986, 1987–1991, 1992–1996 or 1997–2000; for lung cancer, the final category was 1997–2001. As diagnoses of prostate cancer increased greatly when testing for prostate-specific antigen (PSA) was added to the Medicare Benefits Schedule in 1993,8 date of diagnosis was categorised as pre-, peri- or post-PSA testing (1982–1992, 1993–1996 and 1997–2001, respectively).
Comorbidity. ICD codes in the hospital morbidity records for the index admission and admissions in the previous year (excluding the cancer of interest) were used to adjust for comorbidity using the Charlson Morbidity Index.9
Indices of disadvantage. The Index of Relative Socioeconomic Disadvantage (IRSD)10 and the Accessibility/Remoteness Index of Australia (ARIA)11 for the place of residence were added to the record based on the Australian Bureau of Statistics census collection districts (where unavailable, the postcode was used). The hospital of the index admission was categorised as public or private and as metropolitan or rural. The payment classification of the patient at the index admission was recoded as public or private.
Definitions of surgery. Lung cancer surgery was defined as one or more of pneumonectomy, lobectomy, segmentectomy, wedge resection or excision/resection of the bronchus or endotrachea. Prostate cancer surgery was defined as either radical or non-radical prostatectomy (including closed, transurethral, or open). For breast cancer, only women who underwent mastectomy or breast-conserving surgery were included, as the principal aim was to examine differences in patterns of surgical treatment rather than use of surgery per se. There were no Indigenous non-surgery breast cancer cases.
Univariate analysis was carried out, followed by crude and adjusted logistic regression analysis of the likelihood of receiving surgery for lung and prostate cancer, or breast-conserving surgery for breast cancer. The adjusted analyses used the demographic, comorbidity and disadvantage indices (Box 1). For age, the Box–Tidwell term (age × ln[age]) was used to provide a better fit of the model for adjustment purposes. The data were analysed using SPSS for Windows (Version 10.0.7.)12 and Stata 8.13
The study was approved by the Human Research Ethics Committee of the University of Western Australia.
The Indigenous population accounted for 2% of lung cancer cases. The Indigenous patients were younger and more likely to be female than the non-Indigenous patients (Box 1). Among the lung cancer patients who received surgical intervention, age and sex distribution were similar in the Indigenous and non-Indigenous groups. There was a tendency for Indigenous cases to not receive surgery, although this only reached significance with the longer time period (1982–2001) (Box 2).
Very few Indigenous men were recorded as having prostate cancer. The mean age of the Indigenous and non-Indigenous groups was similar. A much smaller proportion of Indigenous patients received radical or non-radical prostatectomy (Box 1). As only one Indigenous person received a radical prostatectomy, logistic regression was not performed. The likelihood of receiving non-radical prostatectomy was lower for Indigenous patients than for non-Indigenous patients in the demographically adjusted model but not in the fully adjusted model (Box 2).
Among women with breast cancer there was no difference between Indigenous and non-Indigenous groups in the proportion who received breast-conserving surgery (Box 1). Likewise, the ages of the groups were similar. Logistic regression showed that Indigenous women had similar treatment patterns to non-Indigenous women (Box 2).
In general, the Indigenous population with lung or prostate cancer were less likely to receive a surgical procedure for their cancer than the non-Indigenous population. However, Indigenous women with breast cancer had a pattern of surgery similar to that of non-Indigenous women.
Age-standardised cancer incidence rates have tended to be lower in the Indigenous population than in the non-Indigenous population.14 In part, this may be attributable to known difficulties in identifying all Indigenous people in the hospital, cancer and death registries,15 which would result in the true effect of being Indigenous being underestimated. Furthermore, poor life expectancy for Indigenous people may mask cancers that are latent at the time of early death. The small numbers of diagnosed and identified cases limit the potential of the statistical analysis to illuminate treatment patterns and outcomes in the Indigenous population.
There is some evidence that Indigenous people with cancer in Australia generally have higher case fatality rates.16 This may be due to a higher relative incidence of cancers with high fatality, particularly lung cancer,14,17 later diagnosis or suboptimal treatment patterns. We found no difference in breast cancer treatment patterns, whereas there were differences in lung and prostate cancer treatment patterns.
Sociocultural and economic factors may influence treatment patterns and outcomes, as has been found with breast cancer.18 An Indigenous person may not have the financial resources, even with assistance programs, to travel for surgery and adjuvant treatment or to pay for medications;18 this may be compounded by a low rate of private health insurance.1 Cultural and religious barriers may also exist, such as sex of the healthcare provider,17 religious denomination of the hospital or a preference for traditional healing practices.19 There may also be concerns about how the immediate and extended family will cope with the illness and treatment,18 especially in areas lacking culturally sensitive aftercare services.19 Importantly, there may be concerns that treatment is ineffective and not worthwhile, especially for cancers with high case-fatality rates, such as lung cancer.
From a healthcare system perspective, plausible barriers exist at all stages of care.19 There are few Indigenous cancer specialists, and non-Indigenous specialists may have difficulty communicating effectively with patients and their families,1,20 potentially leading to paternalistic care3 and reduced compliance with treatment.2,20 Coordinated care between cancer centres, local hospitals and primary care services is essential, but service gaps are commonly reported.19 From a clinical perspective, the low rates of surgical intervention for lung cancer in this study may indicate that the cancers are more advanced and less amenable to treatment in the Indigenous population,21 or, alternatively, there may be comorbidity17 or other valid reasons why patients or surgeons have decided that surgical treatment is not the preferred option.20,22 Nevertheless, the potential for systematic unintentional treatment disparities remains.20,22
A number of policy options are available, but the primary concern must be to reduce social and health inequities for the Indigenous population.3,19 The results of this study suggest four possible policies. Firstly, research in the field to determine the reasons for treatment choice and to ensure that barriers to early treatment are minimised.17,20,22 A second policy step is to engage the Indigenous communities, and together find appropriate strategies.3 Thirdly, administrative datasets have proved useful in profiling morbidity and mortality patterns in the non-Indigenous population, but their use will remain limited in the Indigenous population unless sufficient cases are available for analysis. This could be achieved by better identification of the Indigenous population in the datasets and interstate cooperation to merge de-identified data. Finally, Indigenous issues must be embedded in cancer control strategy plans, and they must be implemented.
1 Demographic characteristics of cancer patients in Western Australia, 1982–2001, and proportions who underwent surgery
|
Non-Indigenous |
Indigenous |
P |
||||||||||||
Lung cancer |
|
|
|
||||||||||||
Total with lung cancer (% of all cases) |
13103 (98.0%) |
274 (2.0%) |
|
||||||||||||
Age in years (mean [SD]) |
67.4 (11.1) |
61.7 (12.5) |
< 0.01 |
||||||||||||
Number who were male (%) |
9222 (70.4%) |
159 (58.0%) |
< 0.01 |
||||||||||||
Received lung cancer surgery (%) |
1693 (12.9%) |
26 (9.5%) |
0.08 |
||||||||||||
Age in years (mean [SD]) |
64.0 (10.5) |
61.8 (11.7) |
0.29 |
||||||||||||
Number who were male (%) |
1160 (68.5%) |
15 (57.7%) |
0.24 |
||||||||||||
Prostate cancer |
|
|
|
||||||||||||
Men with prostate cancer (% of all cases) |
14123 (99.5%) |
64 (0.5%) |
|
||||||||||||
Age in years (mean [SD]) |
72.0 (9.3) |
72.4 (11.5) |
0.79 |
||||||||||||
Received radical prostatectomy (%) |
1787 (12.7%) |
1 (1.5%) |
0.01 |
||||||||||||
Age in years (mean [SD]) |
61.7 (6.5) |
* |
|
||||||||||||
Received non-radical prostatectomy (%) |
5770 (40.8%) |
24 (35.3%) |
0.002 |
||||||||||||
Age in years (mean [SD]) |
73.8 (8.3) |
71.4 (13.2) |
0.15 |
||||||||||||
Breast cancer |
|
|
|
||||||||||||
Women who had breast cancer surgery (%) |
11055 (98.6%) |
151 (1.4%) |
|
||||||||||||
Age in years (mean [SD]) |
58.5 (14.0) |
57.5 (13.6) |
0.37 |
||||||||||||
Received breast-conserving surgery rather than mastectomy (%) |
5243 (47.6%) |
71 (47.0%) |
0.98 |
||||||||||||
Age in years (mean [SD]) |
57.6 (14.0) |
57.6 (13.1) |
0.97 |
||||||||||||
* As only one Indigenous man underwent radical prostatectomy, his age is omitted to prevent identification. |
|||||||||||||||
2 Odds ratio of receiving cancer surgery for Indigenous people versus non-Indigenous people in Western Australia
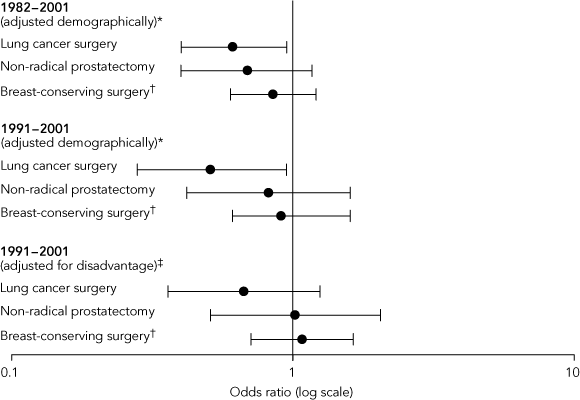
* Odds ratios for 1982–2001 and 1991–2001 (first analysis) were adjusted demographically for patient age, Box–Tidwell transformation of age, calendar period, Charlson index and marital status. The lung cancer analyses were also adjusted for sex and histological type. † For the breast cancer analyses, the periods examined were 1982–2000 and 1991–2000, respectively, rather than 1982–2001 and 1991–2001.
‡ Odds ratios for 1991–2001 (second analysis) were adjusted demographically as above and also for disadvantage using patient Index of Relative Socioeconomic Disadvantage (IRSD),10 Accessibility Remoteness Index of Australia (ARIA),11 hospital status (public or private) and location (metropolitan or rural), and patient insurance status (public or private).
Received 19 February 2004, accepted 3 June 2004
- Sonja E Hall1
- Caroline E Bulsara2
- Max K Bulsara3
- Delia Hendrie4
- C D'Arcy J Holman5
- Timothy G Leahy6
- Margaret R Culbong7
- 1 School of Population Health, University of Western Australia, Crawley, WA.
- 2 Western Australian Aboriginal Community Controlled Health Organisation, Perth, WA.
- 3 Geraldton Regional Aboriginal Medical Service, Geraldton, WA.
We thank the Western Australian Data Linkage Project for providing data and advice. S E H was funded by a National Health and Medical Research Council postgraduate research scholarship.
None identified.
- 1. Cunningham J. Diagnostic and therapeutic procedures among Australian hospital patients identified as Indigenous. Med J Aust 2002; 176: 58-62. <MJA full text>
- 2. Cunningham J, Beneforti M. Hospital statistics, Aboriginal and Torres Strait Islander Australians, 1997–1998. Canberra: Australian Bureau of Statistics, 2000. (Catalogue No. 4711.0.)
- 3. Couzos S, Murray R, for the Kimberley Aboriginal Medical Services’ Council. Aboriginal primary health care: an evidence-based approach Melbourne: Oxford University Press, 2003.
- 4. Craft PS, Primrose JG, Lindner JA, McManus PR. Surgical management of breast cancer in Australian women in 1993: analysis of Medicare statistics. Med J Aust 1997; 166: 626-630. <MJA full text>
- 5. Kricker A, Haskill J, Armstrong B. Breast conservation, mastectomy and axillary surgery in New South Wales women in 1992 and 1995. Br J Cancer 2001; 85: 668-673.
- 6. National Coding Centre. The Australian version of the international classification of diseases, 9th revision, clinical modification (ICD-9-CM). Sydney: National Coding Centre, 1995.
- 7. National Coding Centre. The international statistical classification of diseases and related health problems, 10th revision, Australian modification (ICD-10-AM). Sydney: National Centre for Classification in Health, University of Sydney, 2000.
- 8. Threlfall TJ, English DR, Rouse IL. Prostate cancer in Western Australia: trends in incidence and mortality from 1985 to 1996. Med J Aust 1998; 169: 21-24. <MJA full text>
- 9. Romano P, Roos L, Jollis J. Adapting a clinical comorbidity index for use with ICD-9-CM administrative data: differing perspectives. J Clin Epidemiol 1993; 46: 1075-1079.
- 10. Australian Bureau of Statistics. 1996 Census of population and housing. Socioeconomic indexes for areas. Canberra: ABS, 1998. (Catalogue No. 2039.0.)
- 11. Department of Health and Aged Care. Accessibility/remoteness index of Australia (ARIA). Canberra: Commonwealth Department of Health and Aged Care, 1999. (Occasional papers Series No. 6.)
- 12. SPSS for Windows [computer software]. Release 10.0.7. US: Microsoft Corporation, 2000.
- 13. StataCorp Stata Statistical Software: Release 8.0 [computer software]. College Station, Tex: Stata Corporation, 2003.
- 14. Threlfall TJ, Thompson J. Cancer incidence and mortality in Western Australia, 1999 and 2000; Statistical series number 65. Perth: Department of Health, 2002.
- 15. Young M. Assessing the quality of identification of Aboriginal and Torres Strait Islander people in Western Australia hospital data, 2000. Health Information Centre Occasional Paper 13. Perth: Health Department of Western Australia, 2001.
- 16. Australian Bureau of Statistics. Causes of death 2002. Canberra: ABS, 2003. (Catalogue No. 3303.0.)
- 17. Coory M, Thompson A, Ganguly I. Cancer among people living in rural and remote Indigenous communities in Queensland. Med J Aust 2000; 173: 301-304.
- 18. McMichael C, Kirk M, Manderson L, et al. Indigenous women’s perceptions of breast cancer diagnosis and treatment in Queensland. ANZ J Public Health 2000; 24: 515-519.
- 19. National Aboriginal and Torres Strait Islander Health Council. National Strategic Framework for Aboriginal and Torres Strait Islander Health: framework for action by Governments; prepared for the Australian Health Ministers Conference. Canberra: National Aboriginal and Torres Strait Islander Health Council, 2003.
- 20. Fisher DA, Weeramanthri TS. Hospital care for Aboriginals and Torres Strait Islanders: appropriateness and decision making [letter]. Med J Aust 2002; 176: 49-51. <MJA full text>
- 21. South Australian Health Commission. Epidemiology of cancer in South Australia. Adelaide: South Australian Health Commission, 1997.
- 22. Cunningham J. Diagnostic and therapeutic procedures among Australian hospital patients identified as Indigenous [letter]. Med J Aust 2002; 176: 504. <MJA full text>





Abstract
Objective: To examine whether hospital patients with cancer who were identified as Indigenous were as likely to receive surgery for the cancer as non-Indigenous patients.
Design, setting and patients: Epidemiological survey of all Western Australian (WA) patients who had a cancer registration in the state-based WA Record Linkage Project that mentioned cancer of the breast (1982–2000) or cancer of the lung or prostate (1982–2001).
Main outcome measures: The likelihoods of receiving breast-conserving surgery or mastectomy for breast cancer, lung surgery for lung cancer, or radical or non-radical prostatectomy for prostate cancer were compared between the Indigenous and non-Indigenous populations using adjusted logistic regression analyses.
Results: Indigenous people were less likely to receive surgery for their lung cancer (odds ratio [OR], 0.64; 95% CI, 0.41–0.98). Indigenous men were as likely as non-Indigenous men to receive non-radical prostatectomy (OR, 0.69; 95% CI, 0.40–1.17); only one Indigenous man out of 64 received radical prostatectomy. Indigenous women were as likely as non-Indigenous women to undergo breast-conserving surgery (OR, 0.86; 95% CI, 0.60–1.21).
Conclusions: These results indicate a different pattern of surgical care for Indigenous patients in relation to lung and prostate, but not breast, cancer. Reasons for these disparities, such as treatment choice and barriers to care, require further investigation.