Viral bronchiolitis is the commonest lower respiratory tract infection in children less than 12 months of age and is the most frequent cause of hospitalisation in infants under 6 months of age.1,2 It is caused by viral infections of the lower respiratory tract, principally by respiratory syncytial virus (RSV), which gives rise to widespread small-airway narrowing due to airway oedema, resulting in air trapping.1-4 It is a self-limiting condition, but may be life threatening in a few, especially those with pre-existing cardiac or respiratory conditions.1,3,4 Treatment, when needed, is supportive in order to maintain adequate hydration and oxygenation.1,3 Useful antiviral therapy is unavailable.3 It has been suggested that infants with mildly reduced lung function are predisposed to developing bronchiolitis rather than developing slightly reduced lung function because they have had bronchiolitis.5 Infants who go on to develop recurrent bouts of wheezing in early childhood following bronchiolitis may do so because their airways are of smaller calibre6 or have altered compliance,7 and these children do not necessarily develop asthma by school age.5,6
Bronchiolitis is a clinical diagnosis. Typically, infants present with breathing difficulty associated with coryza.4,8,9 Less commonly, young infants, especially those born prematurely, may present with apnoea before developing the characteristic cough, tachypnoea and use of the accessory muscles of respiration.1,3,4,8 Most cases occur between late autumn and early spring, coinciding with the peak prevalence of RSV within the community.1,8-10 The clinical features of bronchiolitis are shown in Box 1. The range of symptoms and signs at presentation is reflected in the case scenarios of mild bronchiolitis and moderately severe bronchiolitis (Box 2).
The differential diagnosis of viral bronchiolitis may include pulmonary aspiration, bacterial or viral pneumonia, cardiac failure, cystic fibrosis, sepsis (with apnoea), primary ciliary dyskinesia, airway malacia (tracheomalacia and/or bronchomalacia), inhaled foreign body in an older infant, and pneumothorax.8 Differentiating viral bronchiolitis from transient early wheezing is often a source of confusion, especially in older infants and toddlers.2,6,11,12 Infants with transient early wheezing usually do not have bronchiolitis, but rather have viral-induced wheezing.2,11,12 Predisposing factors for transient wheezing in young children include maternal smoking in pregnancy, postnatal exposure to tobacco smoke, and reduced lung function (reduced airway resistance or increased dynamic compliance) before the development of any lower respiratory tract infection.2,11,12
As the hallmark of bronchiolitis is crackles (crepitations) on chest auscultation,13 the recurrence of wheezing as the predominant feature, and factors such as the presence of eczema in an older infant and a history of atopy or asthma in one or both parents, suggest that the infant is less likely to have viral bronchiolitis.11-13
Assessment of severity begins with adequate history-taking. It is important to inquire about pre-existing conditions, including premature birth, chronic respiratory conditions (eg, cystic fibrosis), underlying neurological or neuromuscular conditions, cardiac conditions and immunodeficiency, infectious contacts, duration and rate of progression of symptoms, and how well the infant is feeding (how long it takes to complete a feed, and, if the infant is breastfeeding, enquire if the mother feels that the breast is being emptied). In addition, ask whether the nappies have been as wet as usual in the preceding 12 to 24 hours.1,4,8,12
The examination should include surveillance of the following factors.1,4,8,12,13
General appearance: Is the infant tachypnoeic (> 60 breaths per minute), flushed and warm to touch (significantly febrile if temperature > 38.5°C) and tachycardic for age (generally heart rate > 140 beats per minute)? Is the infant having periods of apnoea?
Hydration: Is the nappy wet? Are the mucous membranes moist? Is the infant able to suck at the breast or on a bottle?
Degree of respiratory difficulty: Is the infant using accessory muscles to breathe? Are there crackles or wheezes evident on chest auscultation?
Adequacy of oxygenation: In room air, is the infant pink or centrally cyanosed?
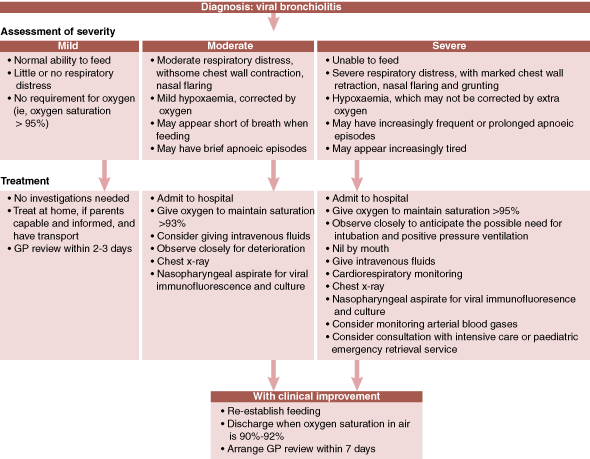
The severity of bronchiolitis can be assessed as mild, moderate or severe (Box 3).1,3,8 Risk factors have been established for more severe bronchiolitis, and thus an increased likelihood of hospital admission (Box 4).14-16 The presence of one or more of these risk factors indicates the need for review within 24 hours by the general practitioner, or referral to an emergency department with paediatric expertise.
For children with mild bronchiolitis, no investigations are indicated, as they will not influence management [E3] (see Box 5 for key to evidence ratings).3,8 For moderate to severe bronchiolitis, the following investigations may be considered in a child in the emergency department [E3, E4].
Oximetry;
Nasopharyngeal aspirate for RSV and viral culture;
Chest radiograph: if moderate (or more) respiratory difficulty, or if diagnostic uncertainty (eg, localised signs on chest auscultation or cardiac murmur with signs of congestive cardiac failure);
Full blood count: if localised radiological changes are present together with neutrophilia on the blood count, then consider a diagnosis of bacterial pneumonia;
Electrolyte, urea and creatinine levels, especially if the child needs intravenous fluids;
Blood culture: if temperature > 38.5°C; and
Blood gas levels: oximetry will guide adequacy of oxygenation, although the likelihood of CO2 retention is low for a child who requires an inspired oxygen concentration (Fio2) < 40%.18
Mild bronchiolitis requires explanation and reassurance, but no specific pharmacological or other therapy [E4] (Box 3).3,4 Bronchodilators and, to a lesser extent, systemic corticosteroids are frequently prescribed in general practice. However, randomised clinical trials of bronchodilators in viral bronchiolitis, whether in the outpatient setting or in hospitalised patients, have shown no clear or sustained benefits [E1].3,4,19 Much of the confusion over bronchodilators and corticosteroids in bronchiolitis relates to the fact that bronchiolitis, transient early wheezing and asthma can produce similar clinical features, especially in children aged over 9 to 12 months.8,11
Conversely, older infants with wheeze (who indeed may have asthma as well as or instead of a viral lower respiratory tract infection) and atopy may have a higher likelihood of responding to bronchodilators or a short course of oral corticosteroids [E4].11,12,20 If bronchodilators are considered, it is important to assess clinical response to a single trial dose before commencing potentially unnecessary treatment [E4]. Bronchodilators are most appropriately administered through a metered-dose inhaler and small-volume spacer or nebuliser rather than as an oral suspension.20
There is no role for nebulised corticosteroids in bronchiolitis [E2].21 Oral corticosteroids, if prescribed, should be limited to a 3-day course of prednisolone at a single daily dose of 1 mg/kg in those in whom a clinical diagnosis of asthma is made [E4].20 The difficulty remains in ascertaining what is asthma among a heterogeneous group of conditions associated with wheeze in early childhood.2,6,11 Reflecting this difficulty, one randomised controlled trial suggested that children aged 1 to 5 years with viral wheeze do not benefit from oral corticosteroids [E2].22
In the management of moderate to severe viral bronchiolitis in infants, “first principles” and common sense support the following recommendations [E4] (Box 3).1,3,4,8,23 Supplemental oxygen is the single most useful therapy, usually delivered via nasal prongs — care with feeding and minimal interference is required, and intravenous fluids are likely to be needed. Careful observation is necessary with high-risk and more unwell infants to facilitate timely introduction of ventilatory support in the few infants who will need it. Increasingly, this involves using mask or nasopharyngeal continuous positive airway pressure ventilation, which often obviates the need for endotracheal ventilation.
The approach to feeding is based upon assessment of the degree of tachypnoea, likelihood of fatigue and risk of pulmonary aspiration. Oral feeding, if tolerated well, should be continued in infants with no more than moderate respiratory difficulty (respiratory rate < 80 breaths per minute, some chest-wall retraction, and maintaining an Spo2 > 93% in supplemental oxygen) [E4]. Intravenous fluids should be administered when there is moderate to severe or severe respiratory difficulty (marked chest wall retraction, nasal flaring, expiratory grunting), marked tachypnoea (> 80 breaths per minute), apnoeic episodes, or visible tiring during feeds [E4]. Intravenous fluids may be required in about half the patients admitted to hospital with “uncomplicated bronchiolitis” (ie, no previous admissions with bronchiolitis, no predisposing conditions) [E3].23 There is considerable variation in the intravenous hydration strategies recommended for infants with bronchiolitis between institutions [E4]. None of these are supported by RCT evidence. A balance must be sought between increased fluid requirements because of fever, insensible losses with tachypnoea and an elevated metabolic rate with the risks of overhydration and reduced lung compliance. Regular review of hydration status is important. Nasogastric tube feeding is generally reserved for the recovery phase [E4].
There are no RCTs of nursing management strategies [E4].2 Good bedside nursing care involves the recognition of deterioration that will necessitate treatment. Factors to monitor include signs of increasing difficulty with feeding and associated risks of pulmonary aspiration, fatigue, work of breathing, and apnoeic episodes. Additionally, maintaining continuity of oxygen therapy, oxygen saturation (Spo2) and heart rate monitoring, minimising the impact of procedures (eg, cannulation), as well as giving support and education to the parents, are important. Whenever possible, nurses caring for infants with moderate to severe bronchiolitis should have paediatric training [E4].
Physiotherapy is not recommended in bronchiolitis, although there are no RCTs addressing this intervention [E4].
Most infants can be discharged in less than 3 days, depending on their ability to sustain adequate levels of hydration and oxygenation (Spo2 > 90%–92%) and the ability of the parents to attend to the needs of the recovering infant [E3].23 All children admitted to hospital should be reviewed by their general practitioner within 7 days. If persisting cough, tachypnoea or wheeze develops, then review by a paediatrician or respiratory paediatrician is appropriate.
There is no direct evidence from RCTs that cohort segregation, handwashing, and use of gowns, masks, gloves and goggles, in combination or individually, reduces the nosocomial transmission of bronchiolitis in hospitalised infants [E2].2,19 Three observational studies have found a lower incidence of RSV transmission in hospital after the introduction separately of cohort segregation, handwashing, gowns and masks, and goggles, 24-26 but a fourth failed to find a benefit of gowns and masks [E3].27 Combinations of these strategies in one RCT found no advantage of gowns and masks over handwashing with gowns and masks, but did not report the transmission rates of RSV in the children [E2].28 Consequently, the most important point to emphasise to parents and staff is that frequent adequate hand washing by nursing and medical staff, other staff and parents will minimise the risk of cross-infection [E4]. In practice, we recommend not nursing infants with bronchiolitis (RSV positive, or awaiting RSV test results) in rooms with high-risk infants (unless the latter are also RSV positive) [E4].
Pharmacological therapies are widely used despite a lack of efficacy. This is true of corticosteroids, adrenaline and bronchodilators, for which there is sufficient information available to assess their role [E1, E2].2,3,19,29-34
In viral bronchiolitis, bronchodilators do not improve oxygen saturation, or affect rate or duration of hospitalisation [E1]. A Cochrane review showed only a clinically non-relevant, modest short-term improvement in clinical scores.19 Ipratropium bromide has not been shown to be useful in bronchiolitis29-31 [E2] and this was supported by a Cochrane review [E1].19
Multiple studies have failed to demonstrate efficacy of corticosteroids in viral bronchiolitis. A meta-analysis of corticosteroids in bronchiolitis failed to show sufficient benefit to change current accepted practice (ie, that corticosteroids should not be routine therapy in viral bronchiolitis) [E1].33 However, a more recent study demonstrated a modest benefit with high-dose oral dexamethasone in children aged 2 to 24 months with mild to moderate bronchiolitis treated as outpatients [E2].34 This study should not alter practice until substantiation can be provided in the largest and most important population (infants 0–6 months) with viral bronchiolitis, along with demonstration that any benefits are clinically significant and that safety is established.
Adrenaline is not widely used in Australia for treating bronchiolitis.35 A recently published Australian RCT demonstrated a lack of efficacy of nebulised adrenaline in infants aged 0 to 12 months with viral bronchiolitis [E2].36
The use of ribavirin, a guanosine analogue with broad-spectrum antiviral activity (particularly against RSV), is not supported by evidence of significant benefit [E1].3,4,37 Moreover, it is accompanied by major practical problems in administration, occupational health and safety concerns, and high cost [E4].3,4,37-39
Five small, low-powered RCTs found no evidence of benefit of intravenous immunoglobulins compared with albumin solution (four studies) or with normal saline (one study) in children admitted to hospital with bronchiolitis [E2].3
Antibiotics are commonly prescribed in bronchiolitis, although they have no action against viruses. One small RCT failed to demonstrate any benefit in hospitalised infants with bronchiolitis [E2].40 The only role for antibiotics is in complicated bronchiolitis where a secondary bacterial infection, such as with streptococcus or staphylococcus, is suspected. This is rare, but not easily excluded in a sick infant with fever, toxicity and significant opacities on the chest radiograph [E4]. Unfortunately, antibiotics are most frequently prescribed in children with mild bronchiolitis with minimal chest radiographic changes, such as partial right upper lobe collapse, which are commonplace in uncomplicated RSV bronchiolitis.1,3,40
Palivizumab is a human recombinant monoclonal antibody directed against a surface glycoprotein of RSV. It is administered as a monthly injection (up to 6 months) over the “RSV season”.3 Although it does reduce hospitalisation and admission rates to ICU in high risk groups (eg, former preterm infants, especially those with chronic neonatal lung disease), it did not reduce the incidence of mechanical ventilation [E2].41 Consequently, its efficacy and cost-effectiveness has been challenged.3,42
This is an antibody preparation derived from the sera of adult humans.43 Delivered as a monthly intravenous infusion, it reduced hospitalisation rates and had similar results to palivizumab, but had the disadvantages of being given intravenously, being expensive, and being considerably less potent than palivizumab in an animal model.44,45
Viral bronchiolitis in infancy is a common condition that can usually be managed at home with simple measures. A minority of infants with underlying conditions are at risk of developing more severe illness. Such infants can usually be identified with adequate history-taking. The presence of crepitations on chest auscultation and hypoxaemia at presentation are the best clinical predictors of the need for hospitalisation.
1: Clinical features of bronchiolitis
Nasal obstruction ± rhinorrhoea and an irritating cough are noticed first.
After 1–3 days there follows increasing tachypnoea and respiratory distress. The chest is often overexpanded.
Auscultatory signs are very variable: fine inspiratory crackles are often heard early, becoming coarser during recovery; expiratory wheeze is often present, initially high-pitched, with prolonged expiration.
Respiratory distress may be mild, moderate or severe.
Fever of 38.5°C or greater is seen in about 50% of infants with bronchiolitis.
Apnoea may be the presenting feature, especially in very young, premature or low-birthweight infants. It often disappears, to be replaced by severe respiratory distress.
2: Scenarios of bronchiolitis
Four-month-old infant with mild bronchiolitis
“Jane”, a 4-month-old, previously well infant, presents to the general practitioner with 2 days of nasal congestion, feeding more slowly than usual but maintaining a normal urine output. She is afebrile, alert, interactive and not dehydrated, with bilateral crackles on chest auscultation. There is no chest-wall recession, a mildly elevated respiratory rate of 52 breaths per minute and she is pink in room air.
Jane has mild bronchiolitis and needs no pharmacological therapy.
Management: Jane’s parents are given an explanation of bronchiolitis and an information sheet about what to expect over the coming days.
It is important that they understand this information, and that they have a telephone and a car or access to transport.
Jane needs to be reviewed in 2–3 days.
Two-month-old infant with moderately severe bronchiolitis
“Henry” is a 2-month-old boy who presents with nasal congestion and poor feeding for 2 days. His mother comments that he has not had a wet nappy for at least 8 hours. Henry was born at term and has been thriving. His older brother has had a cold over the last week. On examination Henry is tachypnoeic (respiratory rate of 68 breaths per minute), tachycardic (152 beats per minute) and mildly febrile (38.6°C). Although he appears pink in room air, his breathing is laboured, with considerable use of accessory muscles of respiration, and he has crackles in both lung fields audible on chest auscultation.
Henry has moderately severe bronchiolitis complicated by dehydration and a likely need for supplemental oxygen.
You inform the parents that he will need admission to hospital.
4: Factors increasing the likelihood of hospital admission3,4,13-16
History of significant apnoea before assessment
Known structural cardiac anomaly, especially large left-to-right shunt (eg, ventricular septal defect)
Known pre-existing lung disease (eg, cystic fibrosis)
Chronological age less than 6 weeks
Significant prematurity (< 32 weeks) and/or chronic neonatal lung disease
Severe degree of respiratory distress or apnoea
Significant dehydration
Hypoxaemia (Spo2 < 93%)
Re-presentation to the emergency department within 24 hours
Uncertain diagnosis.
5: Level-of-evidence ratings17
This article uses evidence ratings simplified from the National Health and Medical Research Council’s level-of-evidence ratings
E1: Systematic review or meta-analysis of all relevant randomised controlled trials (RCTs)
E2: Well-designed RCTs
E3: Well-designed cohort or case–control studies
E4: Consensus opinion of the authors.
- 1. Wohl ME, Chernick V. State of the art: bronchiolitis. Am Rev Respir Dis 1978; 118: 759-781.
- 2. Martinez FD. Respiratory syncytial virus bronchiolitis and the pathogenesis of childhood asthma. Pediatr Infect Dis J 2003; 22 (2 Suppl): S76-S82.
- 3. Lozano JM, Wang E. Bronchiolitis. Clin Evid 2002; 8: 291-303.
- 4. Black CP. Systematic review of the biology and medical management of respiratory syncytial virus infection. Respir Care 2003; 48: 209-233.
- 5. Turner SW, Young S, Landau LI, et al. Reduced lung function both before bronchiolitis and at 11 years. Arch Dis Child 2002; 87: 417-420.
- 6. Martinez FD, Wright AL, Tuassig LM, et al. Asthma and wheezing in the first six years of life. The Group Health Medical Associates. N Engl J Med 1995; 332: 133-138.
- 7. Frey U, Makkonen K, Wellman T, et al. Alterations in airway wall properties in infants with a history of wheezing disorders. Am J Respir Crit Care Med 2000; 161: 1825-1829.
- 8. Phelan P, Olinsky A, Robertson C. Clinical patterns of acute respiratory infections. Oxford: Blackwell Science, 1994: 52-93.
- 9. Roe M, O’Donnell DR, Tasker RC. Respiratory viruses in the intensive care unit. Paediatr Respir Rev 2003; 4: 166-171.
- 10. Martin AJ, Gardner PS, McQuillin J. Epidemiology of respiratory viral infection among paediatric inpatients over a six year period in north-east England. Lancet 1978; 2: 1035-1038.
- 11. Martinez FD. What have we learned from the Tucson Children’s Respiratory Study? Paediatr Respir Rev 2002; 3: 193-197.
- 12. Cover RA, Spahn JD. Treating the wheezing infant. Pediatr Clin North Am 2003; 50: 631-654.
- 13. Mulholland EK, Olinsky A, Shann FA. Clinical findings and severity of acute bronchiolitis. Lancet 1990; 335: 1259-1261.
- 14. Navas L, Wang E, de Carvalho V, Robinson J. Improved outcome of respiratory syncytial virus infections in a high risk hospitalized population of Canadian children. J Pediatr 1992; 121: 348-354.
- 15. Wang EEL, Law BJ, Stephens D. Pediatric Investigators Collaborative Network on Infections in Canada (PICNIC) study of morbidity and risk factors with RSV disease. J Pediatr 1995; 126: 212-219.
- 16. Arnold SR, Wang EE, Law BJ, et al. Variable morbidity of respiratory syncytial virus infection in patients with underlying lung disease: a review of the PICNIC RSV database. Pediatric Investigators Collaborative Network on Infections in Canada. Pediatr Infect Dis J 1999; 18: 866-869.
- 17. National Health and Medical Research Council. How to use evidence: assessment and application of scientific evidence. Canberra: NHMRC, 2000. Available at: www.health.gov.au/nhmrc/publications/pdf/cp69.pdf (accessed Jan 2004).
- 18. Reynolds EOR. The effect of breathing 40 per cent oxygen on the arterial blood gas tensions of babies with bronchiolitis. J Pediatr 1963; 63: 1135-1139.
- 19. Kellner JD, Ohlsson A, Gadomski AM, Wang EE. Bronchodilators for bronchiolitis (Cochrane Review). In: The Cochrane Library, Issue 4, 2003. Chichester UK: John Wiley & Sons Ltd.
- 20. Covar RA, Spahn JD. Treating the wheezing infant. Pediatr Clin North Am 2003; 50: 631-654.
- 21. Richter H, Seddon P. Early nebulized budesonide in the treatment of bronchiolitis and the prevention of post-bronchiolitic wheezing. J Pediatr 1998; 132: 849-853.
- 22. Oommen A, Lambert PC, Grigg J. Efficacy of a short course of patient-initiated oral prednisolone for viral wheeze in children aged 1–5 years: randomised controlled trial. Lancet 2003; 362: 1433-1438.
- 23. Kini NM, Robbins JM, Kirschbaum MS, et al. Inpatient care for uncomplicated bronchiolitis. Arch Pediatr Adolesc Med 2001; 155: 1323-1327.
- 24. Krasinski K, LaCouture R, Holzman R, et al. Screening for respiratory syncytial virus and assignment to a cohort to reduce nosocomial transmission. J Pediatr 1990; 116: 894-898.
- 25. Isaacs D, Hickson H, O’Callaghan C, et al. Handwashing and cohorting in prevention of hospital acquired infections with respiratory syncytial virus. Arch Dis Child 1991; 66: 227-231.
- 26. Gala CL, Hall CB, Schnabel KC, et al. The use of eye goggles to control nosocomial respiratory syncytial virus infection. JAMA 1986; 256: 2706-2708.
- 27. Hall CB, Douglas RG. Nosocomial respiratory syncytial virus infections: should gowns and masks be used? Am J Dis Child 1981; 135: 512-515.
- 28. Murphy D, Todd JK, Chao RK, et al. The use of gowns and mask to contain respiratory illness in pediatric hospital personnel. J Pediatr 1981; 99: 746-750.
- 29. Henry RL, Milner AD, Stokes GM. Ineffectiveness of ipratropium bromide in acute bronchiolitis. Arch Dis Child 1983; 58: 925-926.
- 30. Seidenberg J, Masters B, Hudson A, et al. Effect of ipratropium bromide on respiratory mechanics in infants with acute bronchiolitis. Aust Paediatr J 1987; 23: 169-172.
- 31. Wang EEL, Milner R, Allen U, Maj H. Bronchodilators for treatment of mild bronchiolitis: a factorial randomised trial. Arch Dis Child 1992; 67: 289-293.
- 32. Everard ML, Kurian M. Anti-cholinergic therapy for treatment of wheeze in children under the age of two years. In: The Cochrane Library, Issue 4, 1998. Oxford: Update Software.
- 33. Garrison MM, Christiakis DA, Harvey E, et al. Systemic corticosteroids in infant bronchiolitis: a meta-analysis. Pediatrics 2000; 105: E44.
- 34. Schula S, Coates AL, Binnie R, et al. Efficacy of oral dexamethasone in outpatients with acute bronchiolitis. J Pediatr 2002; 140: 27-32.
- 35. Barben JU, Robertson CF, Robinson PJ. Implementation of evidence based management of acute bronchiolitis. J Pediatr Child Health 2000; 36: 491-497.
- 36. Wainwright CE, Altamirano L, Cheney M, et al. A multicenter, randomized, double-blind, controlled trial of nebulized epinephrine in infants with acute bronchiolitis. N Engl J Med 2003; 349: 27-35.
- 37. Randolph AG, Wang EEL. Ribavirin for respiratory syncytial virus infection of the lower respiratory tract. In: The Cochrane Library, Issue 4, 2003. Chichester, UK: John Wiley & Sons Ltd.
- 38. Decker JA, Seitz TA, Shults RA, et al. Occupational exposures to aerosolized pharmaceuticals and control strategies. Scand J Work Environ Health 1992; 18: 100-102.
- 39. Wheeler JG, Wofford J, Turner RB. Historical cohort evaluation of ribavirin efficacy in respiratory syncytial virus infection. Pediatr Infect Dis J 1993; 12: 209-213.
- 40. Friis B, Andersen P, Brenoe E, et al. Antibiotic treatment of pneumonia and bronchiolitis. A prospective randomised study. Arch Dis Child 1984; 59: 1038-1045.
- 41. Palivizumab, a humanized respiratory syncytial virus monoclonal antibody, reduces hospitalization from respiratory syncytial virus infection in high-risk infants. The IMpact RSV study group. Pediatrics 1998; 102: 531-537.
- 42. Numa A. Outcome of respiratory syncytial virus infection and a cost–benefit analysis of prophylaxis. J Paediatr Child Health 2000; 36: 422-427.
- 43. Reduction of respiratory syncytial virus hospitalization among premature infants and infants with bronchopulmonary dysplasia using respiratory syncytial virus immune globulin prophylaxis. The PREVENT study group. Pediatrics 1997; 99: 93-99.
- 44. Johnson S, Oliver C, Prince GA, et al. Development of a humanized monoclonal antibody (MEDI-493) with potent in vitro and in vivo activity against respiratory syncytial virus. J Infect Dis 1997; 176: 1215-1224.
- 45. Wang EEL, Tang NK. Immunoglobulin for preventing respiratory syncytial virus infection. In: The Cochrane Library, Issue 4, 2003. Chichester, UK. John Wiley & Sons Ltd.





Abstract
Viral bronchiolitis is the commonest cause of hospital admission in young infants.
Respiratory syncytial virus is responsible for most cases of bronchiolitis.
Secondary bacterial infection is rare and antibiotics are seldom necessary.
Most children with bronchiolitis develop only mild illness and can be managed at home.
Infants born prematurely, those with pre-existing cardiac or respiratory disease, and infants in the first three months of life are more likely to need hospital admission.
On current evidence, nebulised adrenaline, inhaled and systemic corticosteroids, and inhaled bronchodilators do not have a role in the routine management of infants with bronchiolitis.