Healthcare call centres are attracting considerable interest as a means of meeting growing consumer demand for advice.1-4 Australian parents often seek telephone advice on healthcare concerns relating to their children.5-9 One such service, Kidsnet, was established in May 1997 at the Children’s Hospital at Westmead (CHW) to meet the growing demand for telephone advice.
Historically, triage nurses have answered calls for advice. Kidsnet provides a separate pool of experienced paediatric nurses, supported by medical staff of the Emergency Department (ED), to answer calls from parents in an office in the ED. The staff use accredited protocols and reference material endorsed by a management committee.
Kidsnet has a single line with the capacity to support multiple staff using automatic call distribution. Because of funding constraints, the service provides a single operator between the hours of 0930 and 1630 and between 1830 and 0100, 7 days a week.
Advice is restricted to guidance on when best to seek care. Follow-up calls are made selectively to maintain a relationship with a caller, alleviate concerns or provide further information.
From the inception of the service on 1 May 1997 to 30 June 2002, information about the caller and child was collected on all calls to Kidsnet by means of a locally developed database. Contact details were only recorded if provided by the caller. Between 1 January 1998 and 28 February 2002, as part of a quality assurance program, nursing staff telephoned callers randomly and delivered a structured questionnaire, usually 48 hours after the initial call. Questions related to the initial call, satisfaction level, helpfulness of the information given and the action taken after the call. No specific selection criteria were applied, other than ensuring that cases were selected at different times and on all days of the week.
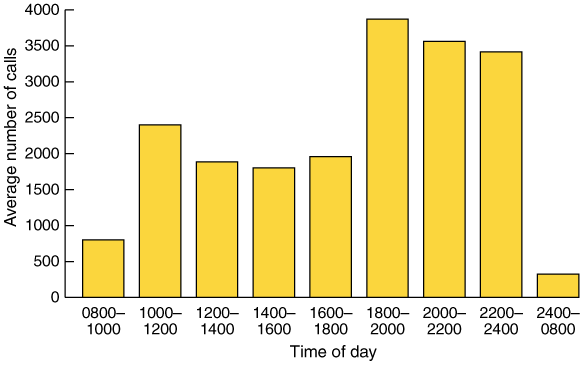
The annual number of calls to Kidsnet increased steadily from 18 327 in 1997/98 to 22 844 in 2001/02, and 28.6% of calls were from those who had used the service at least once before. An average of 1669 calls were received per month. Call numbers peaked in winter and spring. An average of 60 calls were received per day, with a greater demand for service from the evening through to midnight (Box 1). The call rate was higher on weekends (average, 63 calls/day) than on weekdays (average, 52 calls/day).
The average call duration was slightly longer in the first year of operation (10.38 minutes), but then remained fairly consistent at about 9.5 minutes per call.
Most callers (99%) were from New South Wales, with 89% of those living in metropolitan Sydney. Mothers were the predominant callers (85.1%), followed by fathers (11.3%). Most calls (83.5%) were for children aged under 5 years. In over a third of calls (38.5%) the child had not previously been seen by a healthcare professional for the current illness, while 36.7% had been seen by their general practitioner, 6% had attended an ED, and 1.3% had been seen by a clinic sister.
The most common conditions for which advice was sought are shown in Box 2. Most callers (46.6%) were advised to have their child reviewed within 24 hours, 25.7% were advised on home management and 19.7% were advised to seek immediate care. Only 1.5% were transferred to another agency, such as mothercraft or adolescent counselling services, for advice or management.
Kidsnet was established to meet local demand and relieve pressure on the ED and, in particular, on triage, which was taking most calls. Although the service is only provided for limited hours, the demand for Kidsnet continues.
Use of Kidsnet has been similar to that reported for other services.4,6 There was increased demand during outbreaks of measles in 1997 and meningococcal disease in 2002, highlighting the important role of call centres in such circumstances.
Although Kidsnet was established primarily to meet local needs, it has always been used by the wider community, especially out of hours when other services may not be accessible. Parents, and in particular, mothers, of young children tend to seek advice about what to do more commonly than do parents with older children.
The reasons for which parents seek advice reflect common day-to-day problems, and appear consistent with the types of paediatric problems reported by other telephone services.6,9 Giving relatively high levels of home care advice was our experience and has been reported by others.7,8 The number of parents advised to seek immediate care for their child was significantly lower for Kidsnet than that reported by others.6 These differences may be explained by the high level of paediatric expertise of Kidsnet staff.
Although only a small sample of consumers were surveyed, they reported that the service is highly valued and the advice given perceived to be accurate. This is consistent with reports of other services, which highlighted that both the advice given by call centres and compliance with advice was good and consumer satisfaction high.4,7-10
The findings of the consumer survey suggest that, were Kidsnet not available, many calls would devolve back onto the ED. Our experience with Kidsnet would suggest that call centres could contribute to better redistribution of calls and decrease the call load on triage services. However, other studies suggest that call centres increased ED attendances.11
The demand for telephone advice generally, and from EDs in particular, is significant.1,3,4,7-9 The experience at CHW has been that the demand for Kidsnet has continued to increase. The service is highly valued, and the advice given perceived to be accurate. The high rate of recurrent use of Kidsnet supports the usefulness of the service to parents.
2: The 10 most common conditions discussed in calls
Top 10 disease categories |
Average number |
% Of total calls |
|||||||||
Gastrointestinal |
3 661 |
32% |
|||||||||
Fever |
3 541 |
31% |
|||||||||
Respiratory |
1 361 |
12% |
|||||||||
Lumps and bumps |
784 |
7% |
|||||||||
General non-specific problem |
569 |
5% |
|||||||||
Injury |
462 |
4% |
|||||||||
Ears, nose and throat |
393 |
3% |
|||||||||
Poisons |
184 |
2% |
|||||||||
Specific condition |
179 |
2% |
|||||||||
Infectious diseases |
155 |
1% |
|||||||||
Total |
11 289 |
100% |
|||||||||
- Ralph M Hanson1
- Bronwyn J Exley2
- Paul Ngo3
- Maureen P Fitzpatrick4
- Elizabeth L Petering5
- Sara J Matthews6
- Diana Lechner7
- Celeste J Daniels8
- The Children’s Hospital at Westmead, Westmead, NSW.
We thank Professor Kim Oates and Ms Janet Wood for their editorial comments.
None identified.
- 1. Oberklaid F, Bell J, Duke V. Paediatric telephone consultation — a neglected area of health service delivery. Aust Paediatr J 1984; 20: 113-114.
- 2. Oberklaid F. Paediatric telephone advice. A major gap in quality service delivery. J Paediatr Child Health 2002; 38: 6-7.
- 3. Fatovich DM, Jacobs IJ, McCance JP, et al. Emergency department telephone advice. Med J Aust 1998; 169: 143-146. <MJA full text>
- 4. Fatovich DM, Jacobs IJ. Emergency department telephone advice. A survey of Australian emergency departments. Emerg Med 1998; 10: 117-121.
- 5. Oberklaid F. Twenty-four hour access to health information and advice. Med J Aust 1998; 169: 125-126. <MJA full text>
- 6. Turner VF, Bentley PJ, Hodgson SA, et al. Telephone triage in Western Australia. Med J Aust 2002; 176: 100-103. <eMJA full text>
- 7. Poole SR, Schmitt BD, Carruth T, et al. After-hours telephone coverage: the application of an area-wide telephone triage and advice system for paediatric practices. Pediatrics 1993; 92: 670-679.
- 8. Dale J, Crouch R, Patel A, Williams S. Patients telephoning A&E for advice: a comparison of expectations and outcomes. J Accid Emerg Med 1997; 14: 21-23.
- 9. Crouch R, Patel A, Dale J. Paediatric calls to an inner city Accident and Emergency Department: service demand and advice given. Accid Emerg Nursing 1996; 4: 170-174.
- 10. Kempe A, Luberti AA, Hertz AR, et al. Delivery of pediatric after-hours care by call centers: a multicenter study of parental perceptions and compliance. Pediatrics 2001; 108: e111.
- 11. Richardson DB. Impact of a telephone call centre on emergency department workload. Emerg Med 2002; 14: 116.





Abstract
Kidsnet was established in 1997 at the Children’s Hospital at Westmead as a paediatric telephone triage service.
The demand for Kidsnet increased from 18 327 in 1997/98 to 22 844 in 2001/02, with an average of 1669 callers per month.
Most callers were able to proceed to seeking care at a more appropriate time and were satisfied with the service provided.
The service is highly valued and the advice given perceived to be accurate.
Kidsnet has shown that it can play a key role in providing safe advice to families.