Access block (the prolonged wait for an inpatient hospital bed after emergency department treatment) is regarded as one of the major issues currently facing emergency medicine in Australasia.1-3 It has been linked with increased emergency department (ED) waiting time for medical care4 and leads to ED overcrowding.1,5-7 This overcrowding is recognised as a reason for decreased efficiency and quality of care,3-7 and has been linked to adverse events.1,8 However, few published studies1 have examined the relationship between access block, type of service and patient characteristics in EDs in New South Wales.
We elected to explore different definitions of access block (Box 1) and to identify whether the associations between selected characteristics of patients subject to access block remain for each definition.1,2,9,10
Our study used the NSW Emergency Department Data Collection (NSW EDDC),11 from 1 January 1999 to 31 December 2001. The data collection compiles de-identified Emergency Department Information System (EDIS) data from 55 emergency departments that report performance to NSW Health. The participating hospitals comprise 12 Principal Referral (A1), two Paediatric (A2), four Ungrouped Acute (A3), 14 Major Metropolitan (B1), nine Major Non-metropolitan (B2) and 14 District Hospitals (C1 and C2).12 Reliability of EDIS data was examined in terms of missing data rates. The major strength of EDIS data is the accuracy of time-related information, such as time of presentation, triage time, time seen by doctor, departure ready time and discharge time. Some of the limitations of the data include a poor level of confidence in the reliability of diagnostic data, complexity of patient conditions (as ED patients may present with more than one medical problem) and limited space to enter diagnostic information. State-wide bed occupancy rates for all hospitals were not available.
For each patient, four calculations of access block were made, according to the definitions in Box 1. Statistical analyses were used to explore the relationship between hospital type, triage category, departure status, arrival time, age and sex, and the four definitions of access block. Tests of significance (χ2) were used to examine group differences and whether the explanatory variables had an independent effect on access block.
Adjusted analyses were used to explore the independent contribution of each explanatory variable on access block, adjusting for triage category (an indicator of urgency), type of hospital, year of presentation and other variables. Multiple logistic regression was used to identify the independent effect of each of the explanatory variables on the dependent variable.13 To test the main hypothesis of the study, four forced-entry multiple logistic regression models were used (one for each of the definitions of access block). The odds ratios, adjusted for the effects of other variables, with their 95% confidence intervals, are shown to express the likelihood of access block for each explanatory variable. Confounding variables were explored and adjusted for in the multiple logistic regression analyses.
NSW Health gave approval to release the data to the research team, and South Western Sydney Area Health Service Human Research Ethics Committee granted approval for the project.
During 1999–2001, 4 356 323 presentations were recorded in NSW hospital EDs and, of these, 1 046 831 patients (24%) were admitted to a ward or inpatient unit, critical care unit or transferred to other hospitals. Regardless of the definition, access block has increased each year (Box 2).
Principal referral hospitals presented a higher rate of access block for all definitions compared with other types of hospitals (Box 3). The rate was higher for females than for males, for all definitions. Irrespective of definition, the rate of access block increased with age, and the relative difference between young and older patients was large.
The results from logistic regression analyses controlling for four definitions of access block confirmed that, after adjusting for triage category, year of presentation, type of hospital and mode of arrival, sociodemographic characteristics of the patients such as age and sex have significant association with access block in EDs (Box 3).
During the 3-year period, and irrespective of definition, between 2% and 5% of patients had to wait 12–16 hours, and between 2.8% and 5% had to wait more than 16 hours in the ED (Box 4).
Our most important finding is that access block, regardless of definition, is increasing after adjusting for known confounders. Depending on definition, the rate of access block in the past 3 years ranged between 15% and 30%.
Irrespective of definition, rates of access block varied significantly (P < 0.001) by type of hospital, patients’ mode of arrival, time of arrival, triage category, age and sex. The Australian Council on Healthcare Standards and Australasian College for Emergency Medicine (ACHS–ACEM) definition and the NSW Health definition 1 provide estimates that are similar to each other. The difference between these definitions is the waiting time before treatment (Box 1). Rates of access block according to the NSW Health definition 2 and the time delay definition differ by about 40%, but the only difference between these definitions is that the allowable delay after assessment and treatment is halved to 2 hours in the time delay definition.
The NSW Health definitions 1 and 2 represent a systems perspective, but exclude waiting times for treatment for ED patients. They provide the lowest estimate of the magnitude of the problem (Box 2). The ACHS–ACEM definition represents the perspective of the key professional body: the Australasian College for Emergency Medicine. This estimate is between the NSW Health definition 2 and the time delay definition, which represents the highest rate of access block of all definitions.
Principal referral (A1) hospitals showed a higher rate of access block for all definitions. Hospital type B1 has the second highest estimate. It is important to emphasise that A2 hospitals (paediatric) reveal rates about half the size of those in the A1 hospitals. Thus, children are much less likely to be subjected to access block when they require admission to an A2 hospital facility. The differences in the hospital profiles for A1 and A2 hospitals are important. A1 hospitals have more than 25 000 acute weighted separations annually, whereas A2 hospitals have between 10 000 and 25 000. Only A1 hospitals and their EDs provide tertiary specialist referral services. Thus, both the number of separations and a tertiary referral responsibility appear to contribute to a higher rate of access block in A1 hospitals.12
Patients who were brought to EDs by any kind of ambulance had higher rates of access block.4,15 This may be associated with complexity of illness, as patients in triage categories 2 and 3 had a higher rate of access block than others. Many patients in triage categories 2 and 3 may have unresolved diagnoses such as possible coronary syndromes.
Access block was highest for admission to non-critical care wards or inpatient units. This is likely to reflect the fact that there are more admissions to such facilities than to specialised facilities such as critical care units and theatres.
Delay in transfer to the destination ward adversely affects patient outcome, especially for seriously ill people.16,17 Although access block for patients admitted to critical care areas is lower, it remains a source of concern, as failure to manage these patients in an ideal environment results in higher mortality rates and poorer outcomes.16,17 Richardson found that patients who experienced access block had a mean inpatient (after ED) length of stay 0.8 days longer than those who had no access block.1 Liew et al18 also found that excess ED length of stay is associated with excess inpatient length of stay. It is notable that, although comprehensive records are kept on triage category and time to stabilisation in all patients attending the ED,11 there are no similar NSW Health guidelines for time to departure after departure-ready status has been determined.
Cameron et al have suggested that the traditional model of hospital beds is not sustainable into the future.4 These authors and others15 have also indicated an association between access block and ambulance diversion. Our study is consistent with those findings.
Although our findings refer to NSW only, they are similar to results reported in other states.1,8,19 To our knowledge, no attempt has been made to amalgamate ED data across Australia, but EDIS is used elsewhere in Australia, so these findings could be validated in other states.
Our findings are relevant for clinicians and policy makers because they can be used for identifying targets and for guiding policy debate and further research. Overall, our study seems to support the ACHS–ACEM definition as being sensitive to changes and in the mid-range of the definitions we studied. We recommend that clinicians and health service managers become familiar with all definitions, to establish what aspect of the system each one is measuring and to determine which definition is the most appropriate for health system surveillance and patient outcome. From the scientific point of view, our findings show there is no significant additional information to be gained with the use of several definitions; therefore, we recommend that stakeholders start the process of adopting one standard definition to be used across all Australian states and territories.
In summary, our findings confirm what has been reported previously by individual hospitals across the country. Access block continues to increase in prevalence across NSW. To date, initiatives to reduce access block have failed. Thirty to forty per cent of adults admitted to principal referral or major metropolitan hospitals experience unacceptable delays getting to destination wards. These delays are likely to be associated with poorer clinical outcomes and increased length of stay after the ED phase of care, and impair the ability of EDs to deliver high standard emergency care. A fundamental rethink by clinicians and health service administrators is required, so that leaving admitted patients waiting for beds within EDs, or managing any patients in ED corridors (humorously described as “the science of corridology”20), becomes completely unacceptable.
1: Definitions of access block
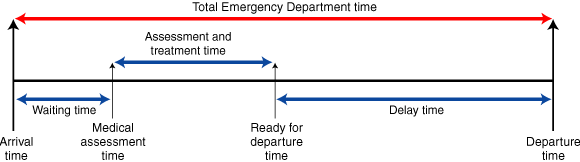
ACHS–ACEM definition: Total time in the emergency department (from arrival time to departure time) exceeding 8 hours.2
NSW Health definition 1: Active treatment and delay time (from medical assessment time to departure time) exceeding 8 hours.9
NSW Health definition 2: Delay time (from ready for departure time to departure time) exceeding 4 hours.9
Time delay definition: Delay time exceeding 2 hours.
ACHS–ACEM = Australian Council on Healthcare Standards and Australasian College for Emergency Medicine.
2: Rate of access block by definition and year of presentation
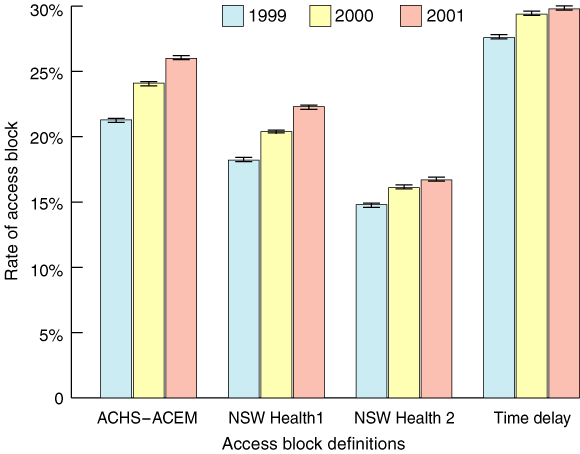
ACHS–ACEM = Australian Council on Healthcare Standards and Australasian College for Emergency Medicine.
3: Rates of access block in New South Wales hospital emergency departments, 1999–2001, according to patient and hospital characteristics
|
ACHS–ACEM definition |
NSW Health definition 1 |
NSW Health definition 2 |
Time delay definition |
|||||||
|
Rate |
OR |
Rate |
OR |
Rate |
OR |
Rate |
OR |
|||
Year of presentation |
|||||||||||
1999 |
21.3% |
1.00 |
18.2% |
1.00 |
14.8% |
1.00 |
27.6% |
1.00 |
|||
2000 |
24.1% |
1.21 |
20.4% |
1.18 |
16.1% |
1.12 |
29.4% |
1.11 |
|||
2001 |
26.0% |
1.39 |
22.3% |
1.35 |
16.7% |
1.19 |
29.8% |
1.14 |
|||
Type of hospital* |
|||||||||||
A1 Principal referral |
33.9% |
1.00 |
28.5% |
1.00 |
23.1% |
1.00 |
40.8% |
1.00 |
|||
A2 Paediatric |
16.4% |
0.38 |
14.0% |
0.41 |
6.7% |
0.83 |
12.1% |
0.44 |
|||
A3 Ungrouped Acute |
17.8% |
0.36 |
15.7% |
0.39 |
14.2% |
0.49 |
28.7% |
0.53 |
|||
B1 Major Metropolitan |
26.6% |
0.73 |
23.4% |
0.80 |
18.4% |
0.79 |
32.3% |
0.72 |
|||
B2 Major Non-metropolitan |
7.6% |
0.16 |
6.3% |
0.17 |
2.9% |
0.11 |
8.6% |
0.14 |
|||
C1 District 1 |
9.4% |
0.19 |
8.4% |
0.22 |
6.7% |
0.24 |
13.7% |
0.23 |
|||
C2 District 2 |
3.8% |
0.08 |
2.6% |
0.07 |
2.6% |
0.10 |
13.2% |
0.24 |
|||
Mode of arrival |
|||||||||||
Ambulance (any type) |
28.2% |
1.00 |
24.9% |
1.00 |
19.3% |
1.00 |
33.1% |
1.00 |
|||
Public or private transport |
20.3% |
0.90 |
16.7% |
0.87 |
13.2% |
0.95 |
25.8% |
0.98 |
|||
Other |
11.6% |
0.43 |
10.4% |
0.45 |
7.2% |
0.52 |
14.7% |
0.54 |
|||
Time of arrival |
|||||||||||
08:00–16:00 |
20.0% |
1.00 |
15.8% |
1.00 |
14.0% |
1.00 |
29.0% |
1.00 |
|||
16:00–23:59 |
23.4% |
1.40 |
21.2% |
1.66 |
16.2% |
1.33 |
26.9% |
0.96 |
|||
00:00–07:59 |
38.1% |
2.95 |
33.2% |
3.00 |
21.3% |
1.72 |
34.9% |
1.34 |
|||
Triage category† |
|||||||||||
1: Immediately life-threatening |
13.7% |
1.00 |
13.7% |
1.00 |
14.3% |
1.00 |
28.3% |
1.00 |
|||
2: Imminently life-threatening |
22.5% |
1.94 |
21.6% |
1.84 |
19.2% |
1.41 |
33.0% |
1.27 |
|||
3: Potentially life-threatening |
24.8% |
2.33 |
21.7% |
1.91 |
16.8% |
1.19 |
30.4% |
1.11 |
|||
4: Potentially serious |
24.9% |
2.44 |
19.5% |
1.70 |
14.1% |
0.96 |
26.5% |
0.91 |
|||
5: Less urgent |
14.6% |
1.53 |
10.9% |
1.05 |
8.4% |
0.68 |
17.5% |
0.64 |
|||
Departure status |
|||||||||||
Admitted to ward and inpatient unit |
24.9% |
1.68 |
21.1% |
1.73 |
16.5% |
1.54 |
29.9% |
1.40 |
|||
Admitted and died in ED |
12.6% |
0.70 |
12.0% |
1.04 |
11.1% |
1.03 |
25.8% |
1.11 |
|||
Admitted to critical care unit |
17.8% |
1.12 |
16.0% |
1.19 |
14.1% |
1.28 |
26.8% |
1.18 |
|||
Admitted via operating theatres |
13.1% |
1.00 |
11.2% |
1.00 |
10.4% |
1.00 |
21.9% |
1.00 |
|||
Admitted or transferred to another hospital |
20.7% |
1.70 |
18.3% |
1.81 |
12.1% |
1.17 |
22.1% |
1.07 |
|||
Age group (years) |
|||||||||||
0–19 |
9.6% |
0.31 |
7.4% |
0.28 |
5.5% |
0.36 |
15.4% |
0.56 |
|||
20–39 |
22.3% |
1.00 |
18.7% |
1.00 |
13.4% |
1.00 |
25.7% |
1.00 |
|||
40–59 |
25.8% |
1.29 |
22.3% |
1.31 |
17.5% |
1.39 |
31.2% |
1.33 |
|||
60–79 |
28.9% |
1.49 |
25.0% |
1.50 |
20.2% |
1.66 |
34.7% |
1.54 |
|||
≥ 80 |
32.9% |
1.67 |
28.5% |
1.67 |
22.8% |
1.87 |
37.6% |
1.69 |
|||
Sex |
|||||||||||
Male |
22.6% |
1.00 |
19.5% |
1.00 |
15.5% |
1.00 |
28.4% |
1.00 |
|||
Female |
25.1% |
1.07 |
21.3% |
1.05 |
16.3% |
1.01 |
29.6% |
1.01 |
|||
ACHS–ACEM = Australian Council on Healthcare Standards and Australasian College for Emergency Medicine. OR = odds ratio. * This classification is based on Hospital Classification and Peer Groups developed by NSW Health in 1995–1996 and revised in 1996–1997 to report emergency department performance.12 † National Triage Scale.14 |
|||||||||||
4: Proportion of patients subject to access block by time period
Access block time* (hours) |
Access block definition |
||||||||||
ACHS–ACEM |
NSW Health 1 |
NSW Health 2 |
Time delay |
||||||||
< 2 |
— |
— |
— |
— |
|||||||
2 to < 4 |
— |
— |
— |
13.1% |
|||||||
4 to < 6 |
— |
— |
5.3% |
5.3% |
|||||||
6 to < 8 |
— |
— |
2.6% |
2.6% |
|||||||
8 to < 10 |
8.1% |
6.5% |
1.6% |
1.6% |
|||||||
10 to < 12 |
4.6% |
3.7% |
1.3% |
1.3% |
|||||||
12 to < 14 |
2.8% |
2.5% |
1.2% |
1.2% |
|||||||
14 to < 16 |
2.2% |
2.0% |
1.1% |
1.1% |
|||||||
16 to < 18 |
1.9% |
1.7% |
1.0% |
1.0% |
|||||||
18 to < 20 |
1.6% |
1.5% |
0.8% |
0.8% |
|||||||
≥ 20 |
2.6% |
2.3% |
1.0% |
1.0% |
|||||||
Total |
23.8% |
20.2% |
15.9% |
29.0% |
|||||||
ACHS–ACEM = Australian Council on Healthcare Standards and Australasian College for Emergency Medicine. * Starting time depends on definition; see Box 1. Dash = Patient departed emergency department within time specified in the definition. |
|||||||||||
- Roberto Forero1
- Lis Young2
- Hai N Phung3
- Kenneth M Hillman4
- Mohammed Mohsin5
- Adrian E Bauman6
- Sue Ieraci7
- Sally M McCarthy8
- C David Hugelmeyer9
- 1 Simpson Centre for Health Services Research, Liverpool Health Service, Liverpool, NSW.
- 2 South West Sydney Area Health Service, Liverpool, NSW.
The study was funded by Priority Driven Research Program-Australian Health Ministers Advisory Committee. Grant No. AHMAC-PDR 2001/03. We thank Sandra Farrugia, Nancy Santiano, ED Project Steering Committee members, Simpson Centre and Epidemiology Unit staff for their support during the project.
None identified
- 1. Richardson DB. The access-block effect: relationship between delay to reaching an inpatient bed and inpatient length of stay. Med J Aust 2002; 177: 492-495. <MJA full text>
- 2. Australasian College for Emergency Medicine. Policy document — standard terminology. Emerg Med (Fremantle) 2002; 14: 337-340.
- 3. Baggoley C. President’s message. Emerg Med (Fremantle) 1998; 10: 269-271.
- 4. Cameron P, Scown P, Campbell D. Managing access block. Aust Health Rev 2002; 25: 59-68.
- 5. Derlet RW, Richards JR. Overcrowding in the nation’s emergency departments: complex causes and disturbing effects. Ann Emerg Med 2000; 35: 63-68.
- 6. Schafermeyer RW, Asplin BR. Hospital and emergency department crowding in the United States. Emerg Med (Fremantle) 2003; 15: 22-27.
- 7. Schneider S, Zwemer F, Doniger A, et al. Rochester New York: a decade of emergency department overcrowding. Acad Emerg Med 2001; 8: 1044-1050.
- 8. Richardson DB. Association of access block with decreased ED performance. Acad Emerg Med 2001; 8: 575-576.
- 9. NSW Health. Emergency department performance. Patients admitted to hospital from emergency departments. Available at: www.asnsw.health.nsw.gov.au/hospitalinfo/measures/data/Curr_ED_Qual_CM_Area_access.html (accessed Nov 2003).
- 10. Cameron PA, Campbell DA. Access block: problems and progress. Med J Aust 2003; 178: 99-100. <MJA full text>
- 11. NSW Emergency Department Data Collection (HOIST) [database]. Centre for Epidemiology and Research, NSW Health. Available, for authorised staff members only, at: www.health.nsw.gov.au (accessed Mar 2002).
- 12. NSW Health. NSW Public Hospital Comparison data book 1996/1997. Sydney: 1998. Electronic version. Available at: www.health.nsw.gov.au/iasd/iad/yb9697/hddb.pdf (accessed Nov 2003).
- 13. Hosmer DW, Lemeshow S. Applied logistic regression. New York: John Wiley & Sons, 1989.
- 14. Australasian College for Emergency Medicine. Guidelines for implementation of the Australasian Triage Scale in emergency departments. Available at: www.acem.org.au/open/documents/triageguide.htm (accessed Nov 2003).
- 15. Cobelas C, Cooper C, Ell M, et al. Quality management and the Emergency Services Enhancement Program. J Qual Clin Pract 2001; 21: 80-85.
- 16. Rivers E, Nguyen B, Havstea S, et al. Early goal-directed therapy. N Engl J Med 2001; 345: 1368-1377.
- 17. Rapoport J, Teres D, Lemeshow S, Harris D. Timing of intensive care unit admission in relation to ICU outcome. Crit Care Med 1990; 18: 1231-1235.
- 18. Liew D, Liew D, Kennedy MO. Emergency department length of stay independently predicts excess inpatient length of stay. Med J Aust 2003; 179: 524-526. <MJA full text>
- 19. Richardson DB, Ruffin RE, Hooper JK, et al. Responses to access block in Australia. Med J Aust 2003; 178: 103-111. <MJA full text>
- 20. Freeman J. The emerging subspecialty of hallway medicine. Can J Emerg Med 2003; 5: 283-285.





Abstract
Objectives: To estimate the magnitude of access block and its trend over time in New South Wales hospitals, using different definitions of access block, and to explore its association with clinical and non-clinical factors.
Design and setting: An epidemiological study using the Emergency Department Information System datasets (1 January 1999 to 31 December 2001) from a sample of 55 NSW hospitals.
Main outcome measures: Prevalence of access block measured by four different definitions; strength of association between access block, type of hospital, year of presentation, mode and time of arrival, triage category (an indicator of urgency), age and sex.
Results: Rates of access block (for all four definitions) increased between 1999 and 2001 by 1%–2% per year. There were increases across all regions of NSW, but urban regions in particular. Patients presenting to Principal Referral hospitals and those who arrived at night were more likely to experience access block. After adjusting for triage category and year of presentation, the mode of arrival, time of arrival, type of hospital, age and sex were significantly associated with access block.
Conclusions: Access block continues to increase across NSW, whatever the definition used. We recommend that hospitals in NSW and Australia move to the use of one standard definition of access block, as our study suggests there is no significant additional information emerging from the use of multiple definitions.