One of the prizes of our affluence is that more Australians than ever before will survive until old age. Average life expectancy in Australia is now 77 years for men and 83 years for women.1 Increasing longevity is an indicator of social and economic progress, and, in the opinion of some experts, brings a more balanced age structure to the population.2 However, in policy debates in Australia, and in particular in debates about health financing, this success has been greeted only with dire predictions of skyrocketing costs.3-5
This is strange, because most experts think that healthcare systems have little to fear from population ageing;6,7 numerous studies have shown that the effects of population ageing will be small and manageable.8-14 What then is the evidence about the effect of population ageing on healthcare costs and why has pessimism about population ageing become embedded in the conventional wisdom of health policy?
It is true that older people use more healthcare than younger people and that the proportion of older people in the population is increasing. However, it is possible that aggregate health costs are determined by factors that are independent of the age structure of the population, and that the age structure merely defines the distribution of predetermined expenditures.8 International comparisons support this hypothesis.
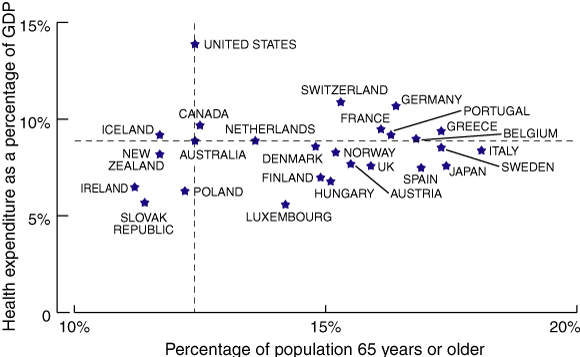
More specifically, across the countries belonging to the Organisation for Economic Co-operation and Development (OECD), ageing of the population is not related to health expenditure as a proportion of GDP (Pearson’s correlation coefficient, 0.11; 95% CI, − 0.29 to 0.48; P = 0.59). The Box shows health expenditure by proportion of population aged 65 years or older in 26 OECD countries. All the countries in the lower right-hand quadrant have populations with a greater proportion of older people than in Australia, but they spend less on health as a percentage of GDP. Most have similar, if not better, health outcomes, as measured by life expectancy. For example, in the year 2000, 17.3% of the Swedish population were aged 65 years or older, but that country spent only 8.6% of its GDP on health. This is less than the 9.3% spent by Australia in 2001–02, when only 12.7% of the population was 65 years or older. The proportion of the Australian population aged 65 years or older will not exceed 17% until the year 2020.
Regardless of the current experience of these “older population” OECD countries, projections of future health expenditure usually assume that population ageing and aggregate costs are closely related. Even using this (possibly incorrect) assumption, projections from models, both for Australia and for other established market economies, consistently show that any increase in expenditure due to population ageing is likely to be small and manageable.
Richardson and Robertson published projections for Australia for 1995–2051.8 They concluded that the effect of future ageing on health expenditure in Australia would be so small that, in the absence of other factors, the size of the health sector would diminish relative to gross domestic product (GDP). Cooper and Hagan, in a 1999 report for the Australian Government Department of Health and Aged Care, reached a similar conclusion:
“. . . projected annual rates of increase [due to ageing] are below the average annual rates of GDP recorded in Australia over lengthy periods, so that health care should not—by virtue of progressive ageing of the population alone—increase as a proportion of national expenditures over the longer term”.9
Badham also found that ageing will have only a small effect on health expenditure.10
Standard methods were used in each of these three recent projections: current expenditures, stratified by age and sex, were multiplied by official projected populations from the Australian Bureau of Statistics and summed to obtain future total expenditure. The Badham analysis also examined the effect of extrapolating per-capita expenditure trends forward in time. This had the effect of reducing the influence of ageing on future expenditure.10
The Richardson–Robertson and Badham forecasts were based on age- and sex-specific expenditures for hospital, ambulatory, pharmaceutical, nursing home, and allied health services, as well as capital costs. The Cooper–Hagan forecasts were based on current age- and sex-specific expenditures for the Medicare Benefits Schedule, Pharmaceutical Benefits Scheme and hospital costs.
All three analyses made an adjustment for future gains in life expectancy, sometimes known as Fuch’s effect.15 Proponents of this adjustment argue that such a correction is needed, because the relationship between ageing and healthcare costs is confounded by time to death. That is, even allowing for increasing trends in the elderly population’s use of medications and elective surgery (eg, hip replacement, cataract surgery, angioplasty), an important proportion of healthcare costs are incurred in the last couple of years of life by the process of dying. (The percentage could be as high as 40%.16) Projecting age-specific expenditure rates forward in time and applying them to population projections can be misleading, because the costs of dying are projected onto an age group that is too young. This can be avoided by estimating expenditure not from the number of years since birth (ie, age), but from the number of years to expected death.
The other recent Australian expenditure forecast was published by the federal government in its Intergenerational Report.11 That forecast did not use an adjustment for life expectancy and was based only on direct federal government expenditure (ie, it excluded inter alia state government expenditure on public hospitals). Nevertheless, the findings were consistent with the other forecasts; namely, the Report found that only 10% of growth in federal government health spending over the last decade was attributable to population ageing (see Table 7 on page 36 of the Report).11 (The main drivers for the remaining 90% were pharmaceuticals and diagnostic tests.) Projecting this trend forward in time, on page 38 the Report concluded that “ageing of the population will have only a small effect on spending”.11 (In spite of this finding, the Overview on page 1 of the Report linked fiscal sustainability with widespread participation in private health insurance, justified by a vague reference to population ageing.11)
Recent reports from other developed countries have also found that ageing will have only a small and manageable effect on future healthcare expenditure. For example, a report from the Canadian Institute for Health Information concluded:
“. . . expenditure increases resulting from ageing by themselves will be relatively stable and modest . . . and will require little, if any, increase in the share of national resources devoted to health care”.12
Reports from the United States and the United Kingdom have reached similar conclusions.13,14
Even these small, modelled increases might be overestimates, because the period between illness and death may become shorter — resulting in a compression of morbidity — and this could conceivably lead to a decrease in healthcare costs. Data from several developed countries during the 1980s and 1990s have shown increases in the period of disability-free life. For example, in the United States, the proportion of the elderly who were disabled decreased from 26.2% in 1982 to 19.7% in 1999.17 Similarly, the proportion of people in the UK who require help with activities of daily living halved between 1976 and 1991.18 The available data in Australia show a slight increase in disability among the elderly of 0.2% per annum,19 but most commentators think that this is due to better reporting rather than to a real increase.20 In other words, it seems unlikely that the decreases in disability observed in other countries have not also occurred in Australia.
Further, trends in smoking, an important risk factor for several chronic diseases, are enough, on their own, to cast doubt on expenditure forecasts based on current morbidity levels. The youngest of the generation of men for whom the prevalence of smoking was 70% are now older than 65 years. In the medium term, our health system will be dealing with a population of whom fewer than 30% smoked, and this is very likely to translate into substantial healthcare savings.21 If we could reduce the prevalence of smoking to even lower levels, then the long-term trends in expenditure would be even more favourable.22
The evidence above is consistent with a forecast put forward by Fries in 1980.23 He postulated that people would remain healthy for an increasing proportion of their lives, and therefore would need less healthcare at each age. At the end, all systems would fail at once, bringing on a short period of acute illness ending in “natural death”. Under this optimistic scenario, “heroic” medical interventions to stave off death in relatively young older people (say, younger than 80 years) would be required less often. Most people would survive until old age, at which time the process of dying would be relatively inexpensive.
No one can predict the future, but if the available evidence supports Fries’ optimistic scenario, why are we being bombarded with the pessimistic and unlikely scenario of an ever-older and ever-sicker population that will bankrupt our economy?
The pessimistic scenario is popular in policy debates for three reasons:
It fits with current and popular ideological positions that favour growth in the private sector. The argument is that relentless demographic trends in ageing make publicly financed systems unsustainable. The obvious answer is more private healthcare, which can be portrayed not as a policy choice, but inevitable. Such reasoning hinders debate about the best mix of public and private sector activity to optimise health status across the population within a given level of expenditure.
It provides a justification for keeping a tight rein on public-sector health expenditure. If the cost of future health services is to be driven relentlessly upward by the increasing demands of an ageing population, then governments had better act responsibly and put the brakes on public-sector spending.
It provides a justification for past expenditure trends. The needs emerge from the population, and providers of care just do their best to meet them with the resources available. Such reasoning might distract from accountability and evaluation. For example, pharmaceutical costs continue to be a major driver of increasing healthcare costs in Australia11 and it would be easy to attribute this to an ageing population. However, as Hill and her coauthors have pointed out, an important factor is the preference of general practitioners for prescribing newer and more expensive (but not necessarily more effective) drugs.24 Such inappropriate prescribing results in increased costs with reduced benefit. We can avoid the difficult task of fixing this problem if we attribute the increasing costs to an ageing population.
In policy making, politics matter and evidence is often only welcomed in so far as it legitimises decisions taken (policy-based evidence).25 In Australia, population ageing has been used to justify current and popular ideological positions that favour the private health sector and seek to contain public-sector activity. It has also distracted attention from the need to evaluate current patterns of care. As a consequence, pessimism about population ageing has stifled constructive debate and limited the number of policy options considered.
The available evidence indicates that population ageing will only have a limited effect on healthcare costs, and there is no evidence that population ageing will cause chaos for our health system. Policy making in Australia would be improved if this was more widely acknowledged.
- 1. Australian Bureau of Statistics. Deaths, 2002. Canberra: ABS, 2003. (Catalogue No. 3302.0.)
- 2. Ebrahim S. Ageing, health, and society. Int J Epidemiol 2002; 31: 715-718.
- 3. Pearson C. Operation will be a success. The Weekend Australian 2003; May 10–11: 18.
- 4. Mitchell H. Andrew Olle Media Lecture 2003. Available at: www.abc.net.au/sydney/stories/s974184.htm (accessed Dec 2003).
- 5. Murphy C. Why the government has to care. The Financial Review 2004; 21 Feb: 22.
- 6. Duckett SJ. Rational care before rationed care. Intern Med J 2002; 32: 533-534.
- 7. Frankel S, Ebrahim S, Davey Smith G. The limits to the demand for health care. BMJ 2000; 321: 40-45.
- 8. Richardson J, Roberston I. Ageing and the cost of health services. Working Paper 90. Melbourne: Centre for Health Program Evaluation, 1999.
- 9. Cooper C, Hagan P. The ageing Australian population and future health costs: 1996–2051. Department of Health and Aged Care. Occasional Papers: New Series No. 7. Canberra: AGPS, 1999.
- 10. Badham J. Future financial impact of the current health financing system. Aust Health Rev 1998; 214: 96-110.
- 11. Commonwealth of Australia. Intergenerational Report, 2002–03. Budget Paper No. 5. Canberra, Canprint, 2002: 36, 38, 1. Available at: www.budget.gov.au/2002-03/bp5/html/01_BP5Prelim.html (accessed Apr 2004).
- 12. Canadian Institute for Health Information. National health expenditure trends. Ottawa, CIHI, 2000.
- 13. National Academy on an Aging Society. Demography is not destiny. Washington, DC: National Academy on an Aging Society, 1999.
- 14. Mullan P. The imaginary time bomb. Why an ageing population is not a social problem. London: I B Tauris & Co, 2000.
- 15. Fuchs V. Though much is taken—reflections on ageing, health and medical care. Milbank Mem Fund Q 1984; 62: 143-155.
- 16. Van Weel C, Michels J. Dying, not old age, to blame for costs of health care. Lancet 1997; 350: 1159-1160.
- 17. Manton KG, Gu X. Changes in the prevalence of chronic disability in the United States black and nonblack population above age 65 from 1982 to 1999. Proc Natl Acad Sci U S A 2001; 98: 6354-6359.
- 18. Grundy E. The health and health care of older adults in England and Wales, 1841-1994. In: Charlton J, Murphy M, editor. The health of adult Britain 1841–1994. London, Stationery Office, 1997.
- 19. Australian Institute of Health and Welfare. Disability and ageing: Australian population patterns and implications. Canberra, AIHW, 2000. (AIHW Catalogue No. DIS 19.)
- 20. Mathers C. Trends in health expectancies in Australia 1981–1993. J Aust Popul Assoc 1996; 13: 1-15.
- 21. Australian Government Department of Health and Ageing. Returns on investment in public health, Canberra: DHAC, 2003.
- 22. Girgis ST, Ward JE. A financial case to enable state health jurisdictions to invest in tobacco control. Med J Aust 2003; 179: 539-524. <MJA full text>
- 23. Fries JF. Aging, natural death and the compression of morbidity. N Engl J Med 1980; 303: 130-135.
- 24. Hill SR, Henry DD, Smith AJ. Rising prescription drug costs: whose responsibility? Med J Aust 1997; 167: 6-7.
- 25. Klein R. From evidence-based medicine to evidence-based policy? J Health Serv Res Policy 2000; 5: 65-66.





Abstract
There have been dire predictions that population ageing will result in skyrocketing health costs. However, numerous studies have shown that the effect of population ageing on health expenditure is likely to be small and manageable.
Pessimism about population ageing is popular in policy debates because it fits with ideological positions that favour growth in the private sector and seek to contain health expenditure in the public sector. It might also distract attention from the need to evaluate the appropriateness and effectiveness of current patterns of care.
Pessimistic scenarios have stifled debate and limited the number of policy options considered. Policy making in Australia would be improved if we took a more realistic view of the effect of population ageing on health expenditure.