Non-metropolitan Australia is characterised by an enormous diversity of rural and remote communities.1 In meeting the diverse healthcare needs of these communities, the pivotal role of general practitioners should not be underestimated.2
Most rural GPs seek to provide a range of medical care that ensures residents of their communities have access to the services commonly available, and expected, in major urban centres.3 The wide range of activities undertaken by rural GPs requires very high skill levels, often with little local support, with the generalist rural doctor assuming full responsibility for the patients’ health outcomes.4 In addition to long working hours, constant on-call, lack of support and access to specialist services, and lack of locum relief,5 rural GPs are increasingly frustrated by remuneration that does not reward adequately for the time, skill and responsibility associated with meeting patient needs in small rural communities.6 This situation provides the “triggers” for experienced GPs to leave and discourages new graduates from entering rural practice.7
Little systematic empirical research exists on how the complexity of activities undertaken by rural doctors varies according to location. In this article, “complexity” refers to the ways in which patients with a variety of presenting problems are managed. Early research provided a descriptive comparison of the morbidity managed and the treatments provided in country and metropolitan practice, but that study had no necessary relationship between their delimitation of “country areas” and remoteness or rurality.8 Subsequently, the Bettering the Evaluation and Care of Health (BEACH) study identified significant differences between urban and rural practice.9
Our objective was to describe the relation between rurality and complexity of practice activities. This study forms part of a broader project to determine how aspects of rurality affect the content, complexity, and costs associated with delivering medical care, practice structures and organisational arrangements, as well as measures required to improve the viability of rural medical services.
To identify the extent to which the complexity of practice activities varied according to rurality, we used the seven-point Rural, Remote and Metropolitan Area (RRMA) classification, which is used extensively by governments for planning and resource allocation programs.10 The five non-metropolitan categories relevant to this study were:
RRMA 3: Large rural centre (population 25 000–99 999);
RRMA 4: Small rural centre (population 10 000–24 999);
RRMA 5: Other rural centre (population < 10 000);
RRMA 6: Remote centre (population > 5000);
RRMA 7: Other remote centre (population < 5000).
Practice complexity was measured using five sentinel questions (Box 1). A panel of experienced and representative rural and remote GPs used a Delphi process11,12 to devise the questions. Questions were framed at a face-to-face workshop of GPs from five states, and twice piloted with GPs (20 on each occasion) from all states and territories, including proceduralists and non-proceduralists, men and women, in solo and group practices across all RRMA groups. The questions were refined until they were shown to be valid and reliable indicators of practice complexity. The questions relate to whether GPs actually engage in the particular activity, and answers were self-reported by the GPs.
A survey of all non-metropolitan GPs in private practice was undertaken in July 2002, based on a Health Insurance Commission (HIC) file of all GPs who performed at least 375 non-referred services in January–March 2002 in rural and remote Australia. Approval for a mail survey of these 4406 GPs was gained from the Commonwealth Statistical Clearing House,13 and ethics approval was obtained from the Monash University Standing Committee on Ethics in Research Involving Humans.
A numbered questionnaire was mailed to each GP at his or her practice. Follow-up of GPs who had not replied within four weeks comprised a reminder letter and up to four telephone calls. A return address on the envelope allowed identification of undeliverable questionnaires.
Cross-tabulation analysis of the complexity items by RRMA was undertaken using SPSS.14 Confidence limits were calculated for the population proportions based on the hypergeometric probability distribution.15
The proportion of GPs reporting each activity was analysed using logistic regression.16 Responses to the discharge question were dichotomised as at least once a week compared with less than once a week. We tested whether the proportion varied between the five RRMA categories, and tested for a trend with population size within RRMAs 3 to 5 and between RRMAs 6 and 7. This analysis was repeated with covariate adjustment for age, time in current practice (a proxy for experience) and hospital Visiting Medical Officer (VMO) rights of the doctor for all GPs and for GPs who worked 35 or more hours a week.
Of the 4406 mailed questionnaires, 97 were returned because the doctor had left the practice, retired, taken extended leave or was otherwise ineligible to participate. The 1498 usable responses received by the cut-off date represented a 35% response rate for all the eligible GPs. Based on age, sex, RRMA and state, the respondents were representative of the survey population (Box 2).
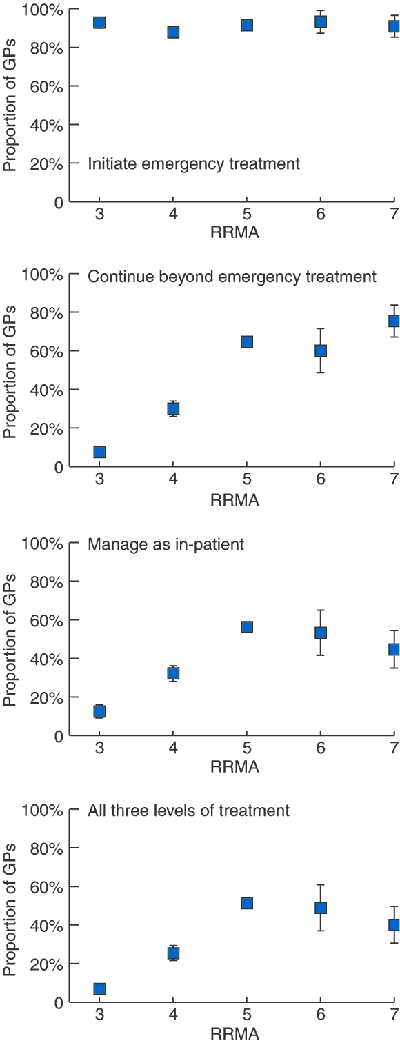
The findings for the measures of complexity, by RRMA category, are shown in Boxes 3, 4 and 5. In general, there was a trend for increasing complexity of service with increasing rurality or remoteness.
For each activity, except initiation of emergency treatment for myocardial infarction, the proportion varied widely and significantly between the RRMA categories (Boxes 3, 4 and 5). The logistic regression showed that most of the variation is accounted for as a trend for more complex activity with increasing rurality from RRMA 3 to RRMA 5. There are relatively few GPs in RRMAs 6 and 7, so even large differences within these RRMAs are not necessarily significant. Covariate adjustment for age, time in current practice and VMO rights did not materially alter these results, nor did restricting the data to GPs who work full-time.
In the case of treatment for myocardial infarction (Boxes 3 and 4), the difference by RRMA across the counts of the numbers of levels of care provided was significant. Almost all doctors across all rural areas initiate treatment, but those in regional centres (RRMA 3) are very unlikely to do much more than that. GPs in the most rural and remote communities (RRMAs 5–7) are the most likely to provide all three levels of care. In the most remote communities (RRMA 7), three-quarters of GPs reported administering streptokinase if indicated.
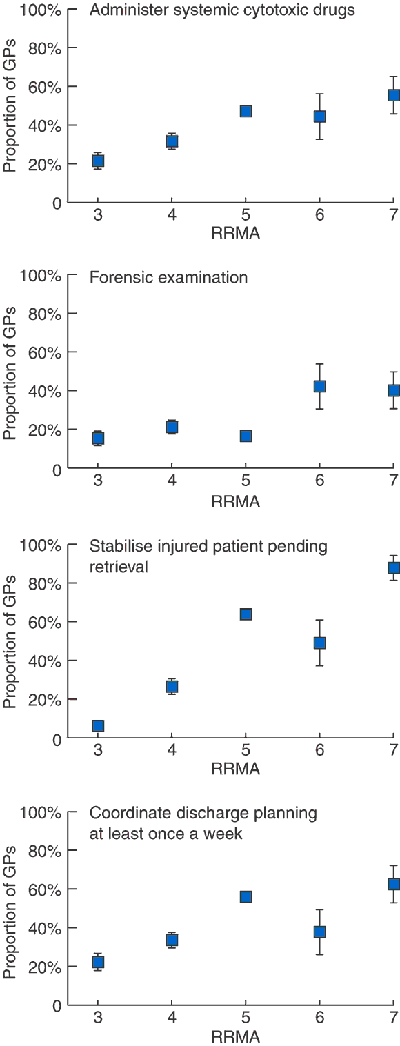
Differences in the proportion of GPs administering systemic cytotoxic drugs or performing a forensic examination on a sexual assault victim at the request of the police were significant (Boxes 3 and 5). GPs in RRMA 3 areas are the least likely to administer cytotoxic drugs, with GPs in RRMAs 5 and 7 providing higher rates of this service than those in RRMAs 3 and 4. Forensic examination on a sexual assault victim is twice as common for remote as rural GPs.
The rate of stabilisation of injured patients (Boxes 3 and 5) increases with increasing rurality. Few GPs in large regional centres (RRMA 3) stabilise patients, whereas almost all remote area (RRMA 7) GPs provide this service.
The proportion of GPs who frequently coordinate discharge planning varies by RRMA category (Boxes 3 and 5). The pattern showed similarity between RRMAs 3, 4 and 6 (where most GPs manage fewer than one patient per week) compared with GPs in RRMAs 5 and 7 (where most GPs were providing this service much more frequently).
Our results clearly show that the complexity of general practice activities differs widely with rurality. The more rural or remote the community, the more likely that the GP is regularly engaged in complex care, including critical emergency treatment using an expanded skill base. The higher rates of stabilisation of injured patients by remote and small-town rural doctors demonstrate their need for emergency medicine skills,17 and reflect the lack of treatment alternatives. The complex relation between discharge planning and remoteness reflects the influence of clinical, healthcare system and political factors. Clearly, GPs in the larger rural and remote centres have access to alternatives to providing patient discharge management themselves.
It is important to acknowledge the potential limitations of our study. Firstly, the survey response rate, although commensurate with those of similar studies, is disappointing given the effort made to maximise it.18-20 It is difficult to see how this could have been increased other than by legislation (as in the case of the Australian Bureau of Statistics surveys) or by remunerating respondents. Nevertheless, the differences between GPs in each RRMA region are large and unlikely to be merely the result of differential response rates.21
Secondly, many factors affect the nature and complexity of rural general practice. While the primary aim of this study was to establish evidence of any significant association with the concept of rurality, the influence of other confounding factors (such as the doctors’ age, experience or hospital access) was considered.
However, adjustment for the potentially confounding variables of age, time in current practice (a proxy for experience) and VMO rights did not materially affect the relations between rurality and the proportion of GPs undertaking each sentinel activity. These relations were also unchanged when only full-time GPs were included in the analysis. Further research is required to investigate the interplay of possible explanatory variables more fully.
These potential limitations notwithstanding, our findings have important implications for the GPs’ workload, responsibility, vocational satisfaction, the need for professional education and support, and, importantly, on the costs and remuneration of rural general practice (both economic and social). Programs and measures designed to support and remunerate GPs in non-metropolitan locations need to take account of the significant differences in practice activity, including the costs and types of professional support required. Particular consideration may be warranted in RRMA 5 communities given the high absolute number of doctors routinely engaged in complex work and the difficulty of recruiting GPs to these communities.
For rural consumers, the wide range of complex services that generalist rural doctors provide to their local communities ensures that patients have equitable access to medical services — services not otherwise available without travelling long distances to regional centres. The importance of local provision to patient care and health outcomes is recognised by the high value placed on the generalist rural doctor by rural Australians.22 Comprehensive local healthcare provided by the rural doctor affects the community’s wider social and economic fabric. Any loss of critical medical services will inevitably reduce the health status and life chances of rural and remote residents and the capacity to address their healthcare needs.
The effect of rurality on general practice activities (and hence on professional satisfaction, practice costs, and recruitment and retention) is a key concept warranting further research. In the absence of rigorous academic research into critical rural health issues in Australia, a good deal of accepted knowledge is derived from anecdotal and often unproven assumptions. This article provides the first comprehensive empirical Australian analysis of the relationship between rurality and the complexity of activities undertaken by rural doctors.
1: The sentinel questions developed for assessing complexity of practice
Please indicate which of the following you currently do in treating myocardial infarction — Initiate emergency treatment; Continue beyond emergency treatment, including the administration of streptokinase if indicated; Manage as an in-patient.
This question ascertained the level of discretionary emergency treatment provided by the GP.
Do you ever administer systemic cytotoxic drugs?
This question probed discretionary non-emergency treatment that provided a major benefit to the patient if available at the local level, and provided an indicator of both confidence and competence of the GP.
In the last three years, have you performed a forensic examination on a sexual assault victim at the request of the police?
This question provided some indication of the expanded skill base of the GP.
How often do you coordinate discharge management (discharge planning) of patients from hospital?
This question measured the involvement of the GP in the full cycle of patient care, ensuring continuity of care and not merely patient hand-over.
Are you routinely involved in the stabilisation of injured patients pending retrieval or evacuation?
This question indicated the skill base of the GP in emergency care.
2: Representativeness of survey respondent group
|
Respondents |
Population* |
|||||||||
|
Number (%) |
Number (%) |
|||||||||
Rural, Remote, Metropolitan Area |
|||||||||||
RRMA 3 |
265 |
(17.7%) |
1042 |
(23.6%) |
|||||||
RRMA 4 |
370 |
(24.7%) |
1176 |
(26.7%) |
|||||||
RRMA 5 |
753 |
(50.3%) |
1875 |
(42.6%) |
|||||||
RRMA 6 |
45 |
(3.0%) |
135 |
(3.1%) |
|||||||
RRMA 7 |
65 |
(4.3%) |
178 |
(4.0%) |
|||||||
Total |
1498 |
(100.0%) |
4406 |
(100.0%) |
|||||||
State |
|||||||||||
NSW |
458 |
(30.6%) |
1243 |
(28.2%) |
|||||||
NT |
14 |
(0.9%) |
43 |
(1.0%) |
|||||||
QLD |
336 |
(22.4%) |
1189 |
(27.0%) |
|||||||
SA |
157 |
(10.5%) |
357 |
(8.1%) |
|||||||
TAS |
71 |
(4.7%) |
234 |
(5.3%) |
|||||||
VIC |
337 |
(22.5%) |
971 |
(22.0%) |
|||||||
WA |
125 |
(8.3%) |
369 |
(8.4%) |
|||||||
Total |
1498 |
(100.0%) |
4406 |
(100.0%) |
|||||||
Age group |
|||||||||||
25-34 |
198 |
(13.4%) |
551 |
(13.0%) |
|||||||
35-44 |
490 |
(33.2%) |
1287 |
(30.3%) |
|||||||
45-54 |
502 |
(34.0%) |
1484 |
(34.9%) |
|||||||
55-64 |
213 |
(14.4%) |
667 |
(15.7%) |
|||||||
65+ |
72 |
(4.9%) |
260 |
(6.1%) |
|||||||
Total |
1475† |
(100.0%) |
4249‡ |
(100.0%) |
|||||||
Sex |
|||||||||||
Female |
395 |
(26.6%) |
1121 |
(25.5%) |
|||||||
Male |
1092 |
(73.4%) |
3282 |
(74.5% |
|||||||
Total |
1498 |
(100.0%) |
4403‡ |
(100.0%) |
|||||||
* All GPs in practice in RRMAs 3–7 who performed at least 375 non-referred services during January–March 2002. † Twenty-three respondents (1.5% of total response) did not provide their age. ‡ Age was not available for 157 GPs (3.6% of total population) and sex not recorded for three GPs (<0.1% of total population). |
|||||||||||
3: Proportion (95% CI) of GPs who carry out sentinel activities, by RRMA and level of treatment
Rural Category |
Myocardial infarction |
Administer systemic cytotoxic drugs |
Perform forensic examination on a sexual assault victim at request of police |
Stabilise injured patients pending retrieval or evacuation |
Coordinate discharge planning at least once a week |
||||||
Initiate emergency treatment |
Administer streptokinase if indicated |
Manage as
|
Provide all
|
||||||||
RRMA 3 |
92.8%
|
7.5%
|
12.5%
|
6.8%
|
21.5%*
|
15.3%†
|
6.1%*
|
22.2%*
|
|||
RRMA 4 |
88.1%
|
30.0%
|
32.2%
|
25.4%
|
31.6%‡
|
21.2%‡
|
26.4%‡
|
33.7%§
|
|||
RRMA 5 |
91.4%
|
64.7%
|
56.2%
|
51.3%
|
47.1%*
|
16.5%‡
|
63.8%*
|
55.9%¶
|
|||
RRMA 6 |
93.3%
|
60.0%
|
53.3%
|
48.9%
|
44.4%
|
42.2%
|
48.9%
|
37.8%
|
|||
RRMA 7 |
90.8%
|
75.4%
|
44.6%
|
40.0%
|
55.4%
|
40.0%
|
87.7%
|
62.5%**
|
|||
* Four responses missing. † Three responses missing. ‡ Six responses missing. § Eight responses missing. ¶ Eleven responses missing. ** One response missing. |
|||||||||||
- John S Humphreys1
- Judith A Jones2
- Michael P Jones3
- David Mildenhall4
- Paul R Mara5
- Bruce Chater6
- David R Rosenthal7
- Nola M Maxfield8
- Michael A Adena9
- 1 School of Rural Health, Monash University, North Bendigo, VIC.
- 2 Jones & Just, Mt Kuringai, NSW.
- 3 University of Western Australia, Albany, WA.
- 4 Health Connections, Gundagai, NSW.
- 5 Theodore, QLD.
- 6 Parallel Rural Community Curriculum, Renmark, SA.
- 7 Wonthaggi Medical Group, Wonthaggi, VIC.
- 8 Covance Pty Ltd, Ainslie, ACT.
This research was funded through the Commonwealth Department of Health and Ageing General Practice Branch, under the auspices of the Rural Doctors Association of Australia in association with Monash University School of Rural Health, Bendigo. Particular thanks go to Gordon Calcino, Naarilla Hirsch, Angela Mikalauskas and Caroline Fredericks for their assistance in expediting access to HIC data; to Fiona Blackshaw and Sybille McKeown from the Statistical Clearing House, Anna Boots from the Rural Doctors Association of Australia, and Vanessa Prince and Marg Bibic from Monash University.
None identified.
- 1. National Rural Health Policy Forum. Healthy horizons 1999–2003. Canberra: Department of Health and Aged Care, 1998.
- 2. General practice in Australia 2000. Canberra: Department of Health and Aged Care, 2000.
- 3. Wilkinson W, Gibbs D, Aloizos J. The review of the impact of Part IV of the Trade Practices Act 1974 on the recruitment and retention of medical practitioners in rural and regional Australia. Canberra: Department of Health and Ageing, 2002.
- 4. Strasser R. Rural general practice: is it a distinct discipline? Aust Fam Physician 1995; 24: 870-876.
- 5. Humphreys JS, Jones M, Jones J, Mara P. Workforce retention in rural and remote Australia: determining the factors that influence length of practice. Med J Aust 2002; 176: 472-476. <MJA full text>
- 6. Relative value study overview. Canberra: Department of Health and Aged Care, 2001. Available at: www.health.gov.au/rvs/overview.htm (accessed Mar 2002).
- 7. Humphreys JS, Jones J, Jones M, et al. A critical review of rural medical workforce retention in Australia. Aust Health Rev 2001; 24: 91-102.
- 8. Britt H, Miles DA, Bridges-Webb C, et al. A comparison of country and metropolitan general practice. Med J Aust 1993; 159 (9 Suppl): S9-S64.
- 9. Britt H, Miller GC, Valenti L. It’s different in the bush. A comparison of general practice activity in metropolitan and rural areas of Australia 1998–2000. Canberra: Australian Institute of Health and Welfare, 2001. (AIHW Catalogue No. GEP 6.)
- 10. Department of Primary Industries and Department of Human Services and Health. Rural, remote and metropolitan areas classification. Canberra: AGPS, 1994.
- 11. Adler M, Ziglio E. Gazing into the oracle: the Delphi method and its application to social policy and public health. London: Jessica Kingsley Publishers, 1996.
- 12. Schopper D, Ammon C, Ronch A, Rougemont A. When providers and community leaders define health priorities: the results of a Delphi survey in the canton of Geneva. Soc Sci Med 2000; 51: 335-342.
- 13. Colledge M, Starick R. Australian Commonwealth government statistical clearing house: vehicle for reducing response load and improving survey quality. Int Stat Rev 2000; 48: 221-231.
- 14. SPSS for Windows [computer program]. Version 11.0. Chicago, Ill: SPSS Inc, 1996.
- 15. Berry K, Mielke P. Exact confidence limits for population proportions based on the negative hypergeometric probability distribution. Percept Mot Skills 1996; 83: 1216-1218.
- 16. Altman DG. Practical statistics for medical research. London: Chapman & Hall, 1991.
- 17. Hungerford P. Rural emergency medicine: the final frontier. Emerg Med (Fremantle) 1998; 10: 208-209.
- 18. Kellerman SE, Herold J. Physician response to surveys: a review of the literature. Am J Prev Med 2001; 20: 61-67.
- 19. McDonald P. Response rates in general practice studies [letter]. Br J Gen Pract 1993; 43: 484.
- 20. McAvoy BR, Kaners EFS. General practice postal surveys: a questionnaire too far? BMJ 1996; 313: 732-733.
- 21. Cummings SM, Savitz LA, Konrad TR. Reported response rates to mailed physician questionnaires. Health Serv Res 2001; 35: 1347-1355.
- 22. Humphreys JS, Weinand HW. Health care preferences in a country town. Med J Aust 1991; 154: 733-737.





Abstract
Objectives: To examine the complexity of activities undertaken in general practice in relation to degree of rurality of the practice.
Design and setting: National mail questionnaire survey across non-metropolitan Australia in July 2002.
Participants: 1498 respondents out of 4406 GPs providing at least 375 Medicare-rebatable consultations in rural and remote locations during January–March 2002 (response rate, 35%).
Main outcome measures: Responses to five sentinel measures of practice complexity.
Results: In general, the proportion of GPs providing complex services increases with increasing rurality or remoteness. Isolated rural and remote GPs manage myocardial infarctions to a higher level than GPs in larger rural and regional centres, are more likely to administer cytotoxic drugs, perform forensic examinations, stabilise injured patients pending retrieval, and coordinate discharge planning more often.
Conclusions: The more rural or remote the area, the more likely a GP is to be regularly engaged in complex care. These findings have implications for the workload, responsibility, vocational satisfaction, need for professional education and support, and costs and remuneration of practice.