Various hospital and home-based interventions have been used to improve the quality and efficiency of the discharge process. These have focused on specific diagnostic groups, such as patients with heart failure,1 or those considered "at risk" of readmission.2-5 They have included various types of discharge planning1-6 and specific home-based interventions undertaken mostly by medical and nursing personnel.1-3,7-9 Results have varied, with some studies showing improved outcomes,1-3 others being inconclusive,7,9-11 and one reporting adverse outcomes.5 A review by Bours and colleagues on the effects of aftercare found that most studies did not report clear benefits.12
In Australia, studies have focused on post-discharge interventions administered by hospital-based staff. However, the Post-Acute Care (PAC) program in Victoria was developed as a different model, where PAC coordinators have a separate budget enabling them to purchase both therapeutic services (eg, physiotherapy) and supportive services (eg, personal care and Meals on Wheels) for patients in the immediate post-discharge period. The rationale is that patients are at most risk in this immediate period, particularly with the trend to decreasing length of hospital stay. The PAC program enables a coordinated approach to case management and provision of short-term community services. It is available for all patients aged 18 years and over who require community services.
We evaluated the benefits of the PAC program in patients aged 65 years and over through a randomised controlled trial. This age group was chosen because of its higher risk of readmission and adverse outcomes. To our knowledge, this is the first randomised controlled trial to evaluate a post-discharge service of this nature.
Four university-affiliated metropolitan general hospitals in Victoria participated in the evaluation. The study was performed between August 1998 and April 2000. Ethics committee approval was obtained from the local ethics committee in all four participating hospitals.
Participants were all patients aged 65 years and over who were discharged between August 1998 and October 1999 and met the eligibility criteria in Box 1.
Before randomisation, informed consent was obtained from patients, baseline demographic data were collected, and the Assessment of Quality of Life (AQoL) questionnaire was administered.13 This Australian questionnaire has five dimensions (Illness, Independent Living, Social Relationships, Physical Senses and Psychological Well-being). Patient carers were interviewed using the Caregiver Strain Index.14
Patients were randomly allocated to the intervention (PAC) or control group by computer-generated numbers. These were provided in sequentially numbered, sealed envelopes which were opened after baseline interviews.
Statistical analysis was performed using SPSS.15 Analysis was by modified intention to treat. The study aimed to recruit 720 patients aged 65 years or over. Allowing for an attrition rate of 20%, this would give about 600 patients available for analysis (α = 0.05 and β = 0.2), which would allow the study to detect a 15% difference in readmission rates.
Continuous variables were compared between groups using t tests. Although health services data were skewed, it was felt that, because of the nature and size of the study, parametric tests were sufficiently robust to allow comparison between groups. For categorical variables, Fisher's exact test or Pearson's χ2 test was used. To examine interaction between variables, stepwise multiple linear regression was used where the dependent variable was continuous. Log rank analysis was then used to compare differences between the intervention and control groups.
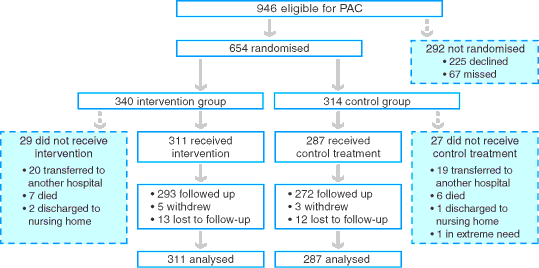
A total of 654 patients were recruited, and 598 were included in the analysis. Patient allocation is shown in Box 2. There were no significant differences between the groups in demographic characteristics, diagnostic categories, comorbidities, number of medications used, other baseline admission characteristics and length of hospital stay during the index admission (Box 3).
There was also no difference between the patient groups in mortality, both in terms of proportion of patients who died during the six months of follow-up (6% in both groups; χ2, P = 0.92) and time to death (log rank analysis, P = 0.84).
All patients completed the AQoL at baseline, and 540 completed it at one-month follow-up. At baseline, there was no difference in quality-of-life scores between the two groups, except in independent living, where the PAC group had a lower mean baseline score than the control group (0.4 v 0.45 on a scale of 0–1, with a higher score representing better quality of life; P = 0.02). However, the groups differed significantly in changes in scores between baseline and one-month follow-up (Box 4). The PAC group had significantly greater improvements in independent living (P = 0.002) and overall quality-of-life scores (P = 0.02).
Caregiver burden was assessed at baseline and one-month follow-up for 263 patients (140 PAC and 123 control). There was no significant difference in scores for the Caregiver Strain Index between PAC and control patients (mean score, 3 for both groups, on a scale of 0–10).
In the six-month follow-up period, there were no significant differences between the PAC and control groups in unplanned readmissions to the index hospital or emergency department presentations (Box 5). However, hospital bed-day use was significantly lower in the PAC group than in the control group (mean, 3.0 days v 5.2 days; P = 0.01; mean difference, 2.2 days; 95% CI, 0.5–3.9).
Using multiple linear regression analysis, with hospital bed-day use as the dependent variable, the strongest predictor of this use was unplanned admissions in the 12 months before recruitment, followed by length of stay during the index admission. The PAC intervention was significantly negatively correlated with hospital use in the six-month follow-up period (P = 0.009).
Nursing and personal care services made up a significantly greater proportion of the community services used in the six months post-discharge by PAC participants than by control participants. In contrast, Meals on Wheels services made up a greater proportion of services used by control participants (Box 5).
There were no significant differences between groups in costs of community services used in the 12 months before the index admission and the six months after discharge (Box 6). However, hospital utilisation costs in the six months after discharge were significantly lower in the PAC group than in the control group (mean difference, $1770; 95% CI, $237–$3304). Total costs, including costs of the intervention ($292.40 per PAC client), hospitalisation and use of community services over the six months of follow-up, were also significantly lower in the PAC group (mean difference, $1545; 95% CI, $11–$3078).
This study provides evidence that coordinating the provision of short-term community services and providing follow-up through the PAC program can be a beneficial component of discharge planning. The PAC program led to greater improvement in overall quality of life at one month after discharge and a reduction in hospital bed-day utilisation in the six months after discharge, with an apparent reduction in healthcare costs.
The model of care was important in generating these outcomes. PAC coordinators are trained to identify and target community services to meet patient needs, have a good working knowledge of local community services and can obtain services at short notice. The capacity to purchase services with a dedicated budget adds flexibility. The ability of the PAC intervention to reduce hospital stay among readmitted patients may relate to the fact that community service structures are already in place among these patients, allowing faster discharge planning. The failure of PAC to reduce mortality or readmissions is not surprising given the generic nature of the intervention and the absence of any medical intervention.
Although patients were aware of their study status, the research staff who administered questionnaires and assessed outcomes were blinded to it. This study design is therefore not significantly different from that of other health service studies on older patients.1-3
A further study limitation relates to the cost analysis, which used averages for costs of community services and hospital bed-day utilisation. Although a more accurate estimate of costs would have been to follow up each individual and cost each component of their admission and community service utilisation, the logistical and budgetary requirements of doing so would have been beyond the scope of this study. The social work intervention in the control group was also not costed, thus underestimating the cost benefit of the PAC intervention. Taking into account this limitation, the PAC intervention apparently reduced costs by reducing hospital bed-days, despite increasing nursing and personal care services. We conclude that coordination and purchase of community services by trained staff confers additional benefits on older patients in the transition from hospital to home.
1: Eligibility criteria for the Post-Acute Care (PAC) study
Inclusion criteria were:
Patients were in an acute ward for over 48 hours and were discharged home;
Patients were expected to live at least one month post-discharge; and
Patients and carers were able to give informed consent.
Exclusion criteria included:
Patients admitted from or discharged to a nursing home or hostel;
Patients discharged from an emergency department; and
Obstetric or psychiatric patients.
Patients were eligible for study enrolment if they met the following risk criteria:
The patient was likely to have mobility or self-care management problems OR met two or more of the following:
– The patient lived alone;
– The patient had responsibilities for caring for others at home; or
– The patient used community services before hospital admission;
AND
The patient required community services on discharge.
3: Demographic and baseline medical characteristics of 598 patients
|
PAC group (n = 311) |
Control group (n = 287) |
|||||||||
Mean age (years) (95% CI) |
76.5 (75.7–77.2) |
76.8 (76.0–77.5) |
|||||||||
Male sex |
124 (40%) |
123 (43%) |
|||||||||
Born overseas |
174 (56%) |
126 (44%) |
|||||||||
Private insurance |
50 (16%) |
46 (16%) |
|||||||||
Main income from government pension |
215 (69%) |
189 (66%) |
|||||||||
Highest education |
|
|
|||||||||
Diploma/certificate |
218 (70%) |
192 (67%) |
|||||||||
University |
72 (23%) |
75 (26%) |
|||||||||
Index admission |
|
|
|||||||||
Unplanned |
208 (67%) |
198 (69%) |
|||||||||
Mean days of stay (95% CI) |
10.0 (8.8–11.1) |
10.4 (9.5–11.4) |
|||||||||
Diagnostic group |
|
|
|||||||||
Medical |
155 (50%) |
154 (54%) |
|||||||||
Surgical |
156 (50%) |
133 (46%) |
|||||||||
Complications |
99 (32%) |
95 (33%) |
|||||||||
Mean number of comorbidities (95% CI) |
2.3 (2.1–2.4) |
2.3 (2.1–2.5) |
|||||||||
Mean number of medications (95% CI) |
|
||||||||||
On admission |
4.8 (4.5–5.2) |
4.7 (4.3–5.1) |
|||||||||
At discharge |
6.2 (5.8–6.6) |
6.3 (5.9–6.7) |
|||||||||
PAC = Post-acute care. |
|||||||||||
4: Change in scores on the Assessment of Quality of Life questionnaire* between baseline and one-month follow-up
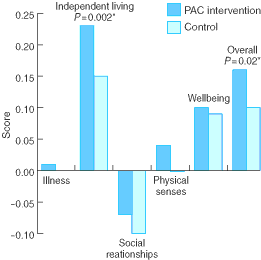
* Range of scores for each dimension and for overall score was 0–1, with higher scores representing better quality of life.
5: Use of hospital and community services
|
12 months before admission |
6 months after discharge |
|||||||||
Service |
PAC group (n = 311) |
Control group (n = 287) |
P |
PAC group (n = 311) |
Control group (n = 287) |
P |
|||||
Hospital |
|
|
|
|
|
|
|||||
Unplanned admissions (mean, 95% CI) |
0.5 (0.3–0.6) |
0.4 (0.3–0.5) |
0.61 |
0.4 (0.3–0.5) |
0.5 (0.4–0.6) |
0.19 |
|||||
Emergency visits (mean, 95% CI) |
0.1 (0.0–0.1) |
0.1 (0.0–0.1) |
0.11 |
0.1 (0.0–0.1) |
0.1 (0.0–0.1) |
0.95 |
|||||
Patients with unplanned admissions |
80 (26%) |
74 (26%) |
0.39 |
75 (25%) |
79 (28%) |
0.25 |
|||||
Patients with emergency visits |
19 (6%) |
11 (4%) |
0.18 |
20 (6%) |
18 (6%) |
0.99 |
|||||
Hospital days used (mean, 95% CI) |
NA |
NA |
NA |
3.0 (2.1–3.9) |
5.2 (3.8–6.7) |
0.01* |
|||||
|
|
|
|
|
|||||||
Meals on Wheels |
1626 (37%) |
2038 (43%) |
< 0.001* |
1030 (18%) |
1831 (33%) |
< 0.001* |
|||||
Nursing |
1277 (29%) |
1511 (32%) |
0.001* |
3300 (58%) |
2882 (52%) |
< 0.001* |
|||||
Home care |
794 (18%) |
538 (11%) |
< 0.001* |
623 (11%) |
605 (12%) |
0.73 |
|||||
Personal care |
505 (11%) |
546 (11%) |
0.84 |
540 (10%) |
136 (3%) |
< 0.001* |
|||||
Other |
219 (5%) |
95 (2%) |
|
172 (3%) |
55 (1%) |
|
|||||
PAC = Post-acute care. * Difference is significant (P < 0.05) by comparison of means (continuous variables) or χ2 test with proportions. |
|||||||||||
6: Costs of hospital and community services
|
Total cost ($) |
Average cost per patient ($) |
|||||||||
|
PAC (n = 311) |
Control (n = 287) |
PAC (n = 311) |
Control (n = 287) |
Mean difference (95% CI) |
P * |
|||||
Community service use |
|
|
|
|
|
|
|||||
Previous 12 months |
216 456 |
341 314 |
697 |
1 189 |
(− 148 to 1133) |
0.13 |
|||||
6 months post-discharge |
142 749 |
150 962 |
459 |
526 |
(− 135 to 269) |
0.52 |
|||||
Hospital utilisation (in the 6 months post-discharge) |
2 609 290 |
2 916 207 |
8 390 |
10 161 |
1770 |
0.02 |
|||||
Total (in the 6 months post-discharge) |
2 843 162 |
3 067 169 |
9 142 |
10 687 |
1545 |
0.048 |
|||||
PAC = Post-acute care. * P for difference in average cost between PAC and control group. |
|||||||||||
Received 16 September 2002, accepted 8 January 2003
- Wen K Lim1
- Sue F Lambert2
- Len C Gray3
- 1 Centre for Applied Gerontology, Bundoora Extended Care, Bundoora, VIC.
- 2 Department of Medicine, Princess Alexandra Hospital, Woolloongabba, QLD.
The study was funded by the Victorian Department of Human Services. W K L was funded by the National Health and Medical Research Council.
None identified.
- 1. Rich MW, Beckham V, Wittenberg C, et al. A multidisciplinary intervention to prevent the readmission of elderly patients with congestive heart failure. N Engl J Med 1995; 333: 1190-1195.
- 2. Stewart S, Pearson S, Luke C, et al. Effects of home based intervention on unplanned readmissions and out-of-hospital deaths. J Am Geriatr Soc 1998; 46: 174-180.
- 3. Naylor MD, Brooten D, Campbell R, et al. Comprehensive discharge planning and home follow-up of hospitalized elders: a randomized clinical trial. JAMA 1999; 281: 613-620.
- 4. Naylor M, Brooten D, Jones R, et al. Comprehensive discharge planning for the hospitalized elderly: a randomized clinical trial. Ann Intern Med 1994; 120: 999-1006.
- 5. Weinberger M, Oddone EZ, Henderson WG. Does increased access to primary care reduce hospital readmissions? N Engl J Med 1996; 334: 1441-1447.
- 6. Evans RL, Hendricks RD. Evaluating hospital discharge planning: a randomized clinical trial. Med Care 1993; 31: 358-370.
- 7. Siu AL, Kravitz RL, Keeler E, et al. Postdischarge geriatric assessment of hospitalized frail elderly patients. Arch Intern Med 1996; 156: 76-81.
- 8. Townsend J, Piper M, Frank AO, et al. Reduction in hospital readmission stay of elderly patients by a community based hospital discharge scheme: a randomised controlled trial. BMJ 1988; 297: 544-547.
- 9. Hansen FR, Spedtsberg K, Schroll M. Geriatric follow-up by home visits after discharge from hospital: a randomized controlled trial. Age Ageing 1992; 21: 445-450.
- 10. Smith DM, Weinberger M, Katz BP, et al. Postdischarge care and readmissions. Med Care 1988; 26: 699-708.
- 11. Fitzgerald JF, Smith DM, Martin DK, et al. A case manager intervention to reduce readmissions. Arch Intern Med 1994; 154: 1721-1729.
- 12. Bours GJ, Ketelaars CA, Corry AJ, et al. The effects of aftercare on chronic patients and frail elderly patients when discharged from hospital: a systematic review. J Adv Nursing 1998; 27: 1076-1086.
- 13. Hawthorne G, Richardson J, Osborne R. The Assessment of Quality of Life (AQoL) instrument, a psychometric measure of health-related quality of life. Qual Life Res 1999; 8: 209-224.
- 14. Robinson BC. Validation of a caregiver strain index. J Gerontol 1983; 38: 344-348.
- 15. SPSS software, version 9.0 for Windows. Chicago, Ill: SPSS Inc, 1999.





Abstract
Objective: To evaluate the benefits of coordinating community services through the Post-Acute Care (PAC) program in older patients after discharge from hospital.
Design: Prospective multicentre, randomised controlled trial with six months of follow-up with blinded outcome measurement.
Setting: Four university-affiliated metropolitan general hospitals in Victoria.
Participants: All patients aged 65 years and over who were discharged between August 1998 and October 1999 and required community services after discharge.
Interventions: Participants were randomly allocated to receive services of a Post-Acute Care (PAC) coordinator (intervention) versus usual discharge planning (control).
Main outcome measures: Comparison of quality of life and carer stress at one-month post-discharge, mortality, hospital readmissions, use of community services and community and hospital costs over the six months post-discharge.
Results: 654 patients were randomised, and 598 were included in the analysis (311 in the PAC group and 287 in the control group). There was no difference in mortality between the groups (both 6%), but significantly greater overall quality-of-life scores at one-month follow-up in the PAC group. There was no difference in unplanned readmissions, but PAC patients used significantly fewer hospital bed-days in the six months after discharge (mean, 3.0 days; 95% CI, 2.1–3.9) than control patients (5.2 days; 95% CI, 3.8–6.7). Total costs (including hospitalisation, community services and the intervention) were lower in the PAC than the control group (mean difference, $1545; 95% CI, $11–$3078).
Conclusions: The PAC program is beneficial in the transition from hospital to the community in older patients.