Where should the GP send this patient? The literature would strongly support transfer, without further delay, to a stroke unit, where he can be appropriately investigated (a computed tomography [CT] or magnetic resonance imaging [MRI] scan is essential) and treated. The positive value of stroke units was confirmed by the meta-analysis of the Stroke Unit Trialists Collaboration,1 reported as part of the Cochrane database. Comparing patients treated in a stroke unit with those treated in a general medical ward, after a median follow-up of one year, these researchers found that, with the former, there was a median reduction in the odds of mortality of 17%, a 31% lower odds of "death or dependency", and a 25% lower odds of "death and institutionalisation". Interestingly, more recent work suggests that the difference in mortality persists for 5 years,2 and even 10 years,3 after the acute event.
Unfortunately, despite the clear advantages of treatment in a dedicated stroke unit, we do not know which specific aspect makes the critical difference. In the meta-analysis, the definition of "dedicated stroke unit" was broad and included units that concentrated on acute management and generally discharged patients within 7 days (early rehabilitation being an important component of the care), units which accepted patients after about 7 days and whose main emphasis was rehabilitation, and combinations of the above. Rehabilitation was therefore one common component of all units, with key elements being a coordinated, multidisciplinary team with specific expertise in stroke, a physician with a special interest or dedication to stroke, agreed protocols for best practice and outcome audits, and educational programs for staff, patients and carers.4
It is strongly recommended that a rehabilitation assessment is undertaken within 24–48 hours of admission to a stroke unit.4 Early evaluation of swallowing and the establishment of safe feeding is critical, as aspiration (which is silent in up to 40% of patients) may lead to pneumonia and increased mortality.5,6 Secondary physical injury can be avoided by proper handling of flaccid or hypertonic limbs, and precautions to prevent falls are essential, particularly in patients with non-dominant-hemisphere strokes with associated neglect (loss of the ability to respond to objects or sensory stimuli located on the side of the body affected by the stroke).
About 20% of patients die in the first month after stroke, and more than half of the survivors will require specialist rehabilitation.7 Once the patient's condition stabilises medically, there is less need for the facilities of the acute hospital, and the focus of the rehabilitation program moves to improving function and independence, and preparing the stroke survivor and his or her carers for life after discharge in the context of their previous health, home and family situation, avocational and vocational needs.
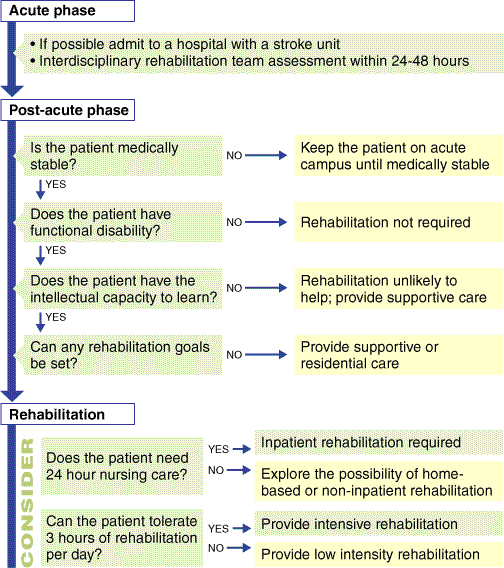
Rehabilitation is, however, an expensive and limited resource, and its success depends on careful selection of patients. There are thus vital questions to answer while the patient is in the acute ward (see 1). Firstly, is the patient medically stable and fit for a rehabilitation program, and is it possible to set realistic rehabilitation goals? If the answer to these is no, then it is better to look at other options for the patient. For example, medical instability is best managed by a longer stay in a medical ward, and, if the patient is assessed as unlikely to make any functional improvement, residential placement may be the best option. In the latter case, close liaison with the geriatric team is essential, particularly for older patients with severe dementia. Neither of these options, of course, excludes later rehabilitation (there is some evidence, for example, that rehabilitation may still be beneficial several years after a stroke8) and regular monitoring by the rehabilitation physician is often appropriate to select those patients who may require intermittent therapy to maintain or improve function.
Once the decision has been made to offer rehabilitation, the second question to be answered is where should it be provided? Options include specialist inpatient, outpatient or home-based services, and all of these can provide high quality rehabilitation programs. Important factors to take into account include the dependence of the patient (the need for 24-hour nursing care or supervision usually precludes home management), and how much support is available at home.
The wish of the patient and family must also always be respected; patients who live in extended families often prefer to be in the home environment, particularly (in the Australian context) if they speak limited English.
Several randomised controlled trials have been published in the past five years comparing home-based rehabilitation programs with rehabilitation in hospital, and these have been the subject of a systematic review9 that showed no statistically significant difference between the two approaches, either in terms of patient and carer outcomes or resource utilisation.
Nevertheless, some of the individual studies reviewed by the Cochrane Collaboration did show change: three studies suggested higher levels of patient satisfaction, and specifically reported that patients felt more involved in planning their rehabilitation programs if they were treated at home.10-12 In addition, one study13 reported the important finding that carers at home developed more "stress" at 6 months, but this was detected only by one of the three tools used (the 36-item Short-form Health Status survey [SF-36]), and the difference was not present at the 12-month follow up.14
Of concern in this regard is a recent British study15 that found a higher mortality rate at 3, 6 and 12 months in patients receiving home-based rehabilitation than in those admitted to a stroke unit. However, patients in that study were transferred to home care shortly after admission to the acute hospital, whereas most Australian units provide inpatient and home-based rehabilitation sequentially. Another important aspect of that study was the definite difference in functional outcome found between the stroke unit, general ward and home therapy groups, with the greatest improvement occurring in patients treated in the stroke unit. Moreover, the groups also differed markedly in the median amount of therapy received during similar lengths of stay (eg, a total of 21.5 hours of physiotherapy in the stroke unit versus only 7.3 hours at home). Perhaps it is the amount of therapy that makes the difference, not where it is delivered?
Attempts to compare community-based (non-inpatient) programs with inpatient programs have been beset by wide variation in program definition, and the poor performance of standard outcome measures in this context.16 Any rehabilitation professional knows from experience that many carefully selected patients do well as outpatients.
Many issues need to be addressed in rehabilitation programs, whatever the environment. Rehabilitation will only be successful if the team, patient and carers cooperate to set interdisciplinary goals. Regular team and family meetings are thus mandatory. Cohesion is often aided by the appointment of a "key person", one member of the team who liaises with the family; this is also often less intimidating to family members.
Individual team members then bring their specific expertise to the rehabilitation goals.
■ A rehabilitation physician usually leads the team and works closely with the nurses to deal with comorbidities, such as hypertension and diabetes, and to treat or prevent secondary complications, such as pressure areas and seizures (about 5% of patients will have a seizure in the first year after stroke). A further important complication is post-stroke depression, with a high incidence of more than 60% noted by Robinson et al17 nearly two decades ago. More recently, depression has been shown to affect the functional outcome of a stroke, perhaps providing a reason for more aggressive treatment of depression after a stroke.18 Anxiety may be even more common, but prescribing anxiolytics and hypnotics is rarely of benefit to these patients, even if they have a poor sleep pattern. The rehabilitation specialist also has an important role in the pharmacological treatment of spasticity, using drugs such as baclofen or dantrolene, or through nerve blocks, motor point injections or botulinum toxin injections. Various pain syndromes (which may include musculoskeletal trauma or complex regional pain syndrome) are common after stroke and require careful medical assessment and medical assessment and management.
Most of the evidence in favour of rehabilitation in the post-acute phase is based, as in the acute phase, on evaluation of a multidisciplinary program as a whole, or a particular discipline (eg, speech or occupational therapy) as an entity, rather than on the individual components or the philosophy of rehabilitation. For example, the Cochrane Collaboration19 is currently reviewing the large body of research comparing specific physiotherapy techniques (eg, the neurophysiological paradigms of Bobath and Brunnstrom and the "motor relearning" approach). Preliminary reports suggest that none is clearly superior for lower-limb function, but in many instances high-quality research is just not available. Lack of an evidence base should not stop us persevering with a technique that apparently helps while we await conclusive evidence.
Improvements in function after stroke are the result of a number of processes, including recovery of parts of the ischaemic penumbra (the potentially viable zone surrounding areas of cerebral infarction), resolution of cerebral oedema, neuroplasticity (parts of the brain on the same or opposite side may take on the functions of the damaged area), and the patient learning to compensate by using the unaffected parts of the body. Recovery is affected by the size of the stroke, and by any pre-existing comorbidities or dementia, and is likely to be maximal within the first three months. Determining the prognosis is always difficult, but is usually possible by six months after the stroke, and often much earlier. The Oxfordshire Classification of Stroke is a clinically based classification which can assist in prognostication for survival and dependence, but it is important not to provide a too-confident prediction.20
The challenge for the future is to develop new approaches that will enhance stroke outcome. Management of comorbidities may be an important aspect of this. Depression has been discussed above, but another topical condition is sleep apnoea, which affects more than 60% of stroke survivors,21 and is associated with increased mortality22 and worse functional outcome at 3 and 12 months.23
Specific rehabilitation approaches are increasingly being subjected to scientific scrutiny, and studies now attest to the value of biofeedback,24 and newer techniques such as treadmill training with bodyweight support,25 and the use of robotics.26 One approach that has had extensive publicity is intensive therapy (six hours per day) on the paralysed arm, with splinting of the unaffected arm.27 Time will show whether all or none of the above techniques are of practical and lasting importance.
More randomised controlled trials comparing rehabilitation approaches are thus urgently required. Only through high quality research can we hope to successfully apply rehabilitation principles to improve the outcome of patients affected by this common and severely disabling condition.
Evidence-based recommendations
Acute care – Rehabilitation priorities and principles should be integrated into the acute care of patients (E1).1
Home v hospital – There is no evidence that rehabilitation at home leads to better patient or carer outcomes than hospital-based stroke rehabilitation, or consumes fewer resources (E1).9
Assessment – It is strongly recommended that a rehabilitation assessment is undertaken within 24–48 hours of admission to hospital (E1).4
Reassessment – There is evidence that rehabilitation may still be beneficial several years after a stroke; therefore, regular reassessment, even of patients in nursing homes with stroke, is often appropriate (E4).8
- Michael R P Pollack1
- Peter B Disler2
- 1 Rehabilitation Medicine Unit, John Hunter Hospital, New Lambton, NSW.
- 2 Rehabilitation Programme and Victorian Rehabilitation Research Institute, Melbourne Health, and University of Melbourne, Parkville, VIC.
- 1. Stroke Unit Trialists' Collaboration. Collaborative systematic review of the randomised trials of organised inpatient (stroke unit) care after stroke. BMJ 1997; 314: 1151-1159.
- 2. Jorgensen HS, Kammersgaard LP, Nakayama H. Treatment and rehabilitation on a stroke unit improves 5-year survival. A community-based study. Stroke 1999; 30: 930-933.
- 3. Indredavik B, Bakke F, Slordahl SA, et al. Stroke unit treatment: 10 year follow-up. Stroke 1999; 30: 1524-1527.
- 4. Royal College of Physicians of the United Kingdom: Intercollegiate Working Party for Stroke. National Clinical Guidelines for Stroke (2000). London: Royal College of Physicians, 2000.
- 5. Horner J, Massey EW, Riski J, et al. Aspiration following stroke: clinical correlates and outcome. Neurology 1988; 38: 1359-1362.
- 6. Post-Stroke Rehabilitation: Clinical Practice Guideline. No. 16. Rockville, MD: US Department of Health and Human Services, 1995: (ACHPR Publication No. 95-0662).
- 7. Warlow CP, Dennis MS, van Gijn J, et al, editors. Stroke; a practical guide to management. 2nd edition. Malden, Mass: Blackwell Science, 2001: 420.
- 8. Wade DT, Collen FM, Robb GF, Warlow CP. Physiotherapy intervention late after stroke and mobility. BMJ 1992; 304: 609-613.
- 9. Early Supported Discharge Trialists. Services for reducing duration of hospital care for acute stroke patients [systematic review]. Cochrane Stroke Group. Cochrane Database Syst Rev Issue 3, 2002: CD000443.
- 10. Mayo N, Wood-Dauphinee S, Cote R, et al. There's no place like home. An evaluation of early supported discharge for stroke. Stroke 2000; 31: 1016-1023.
- 11. Widen Holmqvist L, von Koch L, Kostulas V, et al. A randomised controlled trial of rehabilitation at home after stroke in southwest Stockholm. Stroke 1998; 29: 591-597.
- 12. Rodgers H, Soutter J, Kaiser W, et al. Early supported hospital discharge following acute stroke: pilot study results. Clin Rehabil 1997; 11: 280-287.
- 13. Anderson C, Rubenach S, Mhurchu CN, et al. Hospital or home for stroke rehabilitation? Results of a randomized controlled trial. I: Health outcomes at 6 months. Stroke 2000; 31: 1024-1031.
- 14. Hackett M, Vandal A, Anderson C, Rubenach S. Long-term outcome in stroke patients and caregivers following accelerated hospital discharge and home-based rehabilitation [letter]. Stroke 2002; 33: 643-645.
- 15. Kalra L, Evans A, Perez I, et al. Alternative strategies for stroke care: a prospective randomised controlled trial. Lancet 2000; 356: 894-899.
- 16. Dekker R, Drost EA, Groothoff JW, et al. Effects of day-hospital rehabilitation in stroke patients: a review of randomised controlled trials. Scand J Rehab Med 1998; 30: 87-94.
- 17. Robinson RG, Lipsey JR, Price TR. Depression: an often overlooked sequel of stroke. Geriatric Medicine Today 1984; 3: 35-45.
- 18. Van de Weg FB, Kuik DJ, Lankhorst GJ. Post-stroke depression and functional outcome: a cohort study investigating the influence of depression on functional recovery after stroke. Clin Rehabil 1999; 13: 268-272.
- 19. Pollock A, Langhorne P, Baer G, Pomeroy V. Physiotherapy for the recovery of postural control and lower limb function following stroke. (Protocol for a Cochrane Review). In: The Cochrane Library, Issue 2, 2002. Oxford: Update Software.
- 20. Bamford J, Sandercock PAG, Dennis MS, et al. Classification and natural history of clinically identifiable subtypes of cerebral infarction. Lancet 1991; 337: 1521-1526.
- 21. Bassetti C, Aldrich MS. Sleep apnea in acute cerebrovascular diseases: final report on 128 patients. Sleep 1999; 22: 217-223.
- 22. Dyken ME, Somers PD, Yamada T, et al. Investigating the relationship between stroke and obstructive sleep apnea. Stroke 1996; 27: 401-407.
- 23. Good DC, Henkle JQ, Gelber D, et al. Sleep-disordered breathing and poor functional outcome after stroke. Stroke 1996; 27: 252-259.
- 24. Walker C, Brouwer BJ, Culham EG. Use of visual feedback in retraining balance following acute stroke. Phys Therapy 2000; 80: 886-895.
- 25. Danielsson A, Sunnerhagen KS. Oxygen consumption during treadmill walking with and without body weight support in patients with hemiparesis after stroke and in healthy subjects. Arch Phys Med Rehabil 2000; 81: 953-957.
- 26. Volpe B, Krebs H, Edelstein O, Diels C. A novel approach to stroke rehabilitation: robot aided sensorimotor stimulation. Neurology 2000; 54: 1938-1944.
- 27. Kunkel A, Kopp B, Muller G, et al. Constraint-induced movement therapy for motor recovery in chronic stroke patients. Arch Phys Med Rehabil 1999; 80: 624-628.






Abstract
Stroke is the third highest cause of death and the leading cause of chronic disability in adults in Australia.
Studies show clear advantages of treatment of patients in the acute phase of stroke in a dedicated stroke unit.
Rehabilitation after stroke is a continuum, starting within days of stroke onset and ending only when it no longer produces any positive effect. More than half the 75% of patients who survive the first month after a stroke will require specialised rehabilitation.
Effective rehabilitation relies on a coordinated, multidisciplinary team approach. Regular team meetings, as well as meetings with the patient, his or her family and carers, are essential.
Improvements in function after stroke are the result of recovery within the ischaemic penumbra, resolution of cerebral oedema, neuroplasticity, and compensatory strategies learnt by the patient.
Evidence supporting rehabilitation programs is based on evaluation of the multidisciplinary approach, or on the effect of a particular discipline (eg, speech therapy), rather than on individual components of treatment.
When the patient is discharged from a formal rehabilitation program, the general practitioner's role becomes paramount. GPs can help patients deal with the consequences of stroke, such as depression, and any comorbidities. GPs may also provide counselling on issues ranging from interpersonal and sexual relationships, through ability to drive again, and vocational and recreational activities.