| Abstract |
Objectives: To compare rates of mortality from
coronary heart disease (CHD) between populations living within and
outside Australian capital city statistical divisions. Design and setting: Descriptive epidemiological study based on data for all residents of Australia aged 30-69 years who died between 1986 and 1996 in all States and Territories of Australia. Main outcome measures: Standardised mortality rates from all causes and coronary heart disease as coded by the Australian Bureau of Statistics, and estimated excess deaths in populations living outside capital city statistical divisions. Results: Between 1986 and 1996, mortality from CHD declined by 46% in men and 51% in women, and accounted for 61% of the decline in mortality from all causes in men and 48% in women. More deaths than expected from acute myocardial infarction resulted in mortality rates from CHD up to 30% higher in men and 21% higher in women living outside the capital city statistical divisions, and accounted for an overall estimated excess of 3835 deaths from CHD in men (32% of excess deaths from all causes), and 1385 deaths from CHD in women (27% of excess deaths from all causes) over the 11-year study period. Conclusions: Although there were impressive declines in coronary mortality in all Australian States and Territories from 1986 to 1996, populations living outside capital cities continue to have higher death rates from CHD. These differences in mortality rates indicate a need for further research into factors which may influence mortality rates for CHD in rural and remote areas, and immediate measures to ensure optimal treatment of coronary risk factors and acute coronary events in such populations. | |
| Coronary heart disease (CHD) remains the largest single cause of death in Australia.1 Although there has been a steady decline in the death rate associated with CHD over the past 30 years, rates of decline have not been equal throughout Australia.2,3 A study of coronary mortality in Tasmania showed higher rates of mortality outside the capital city region.4 We examined official data for Australian men and women aged 30-69 years between 1986 and 1996 for evidence of differences in rates of death from CHD between capital city and regional populations. | ||
| Methods |
The Australian Bureau of Statistics (ABS) collects and disseminates
social, demographic and economic statistics for 66 Statistical
Divisions based on an Australian Standard Geographical
Classification (ASGC).5 The boundaries of capital
city statistical divisions are determined by the anticipated
development of the city for a period of at least 20 years, and delimit an
area that is stable for general statistical purposes. Statistical
divisions outside a capital city are relatively homogeneous regions
characterised by identifiable social and economic links between the
inhabitants and between the economic units within the region, under
the unifying influence of one or more major towns or cities.
We obtained ABS estimates of the size of the Australian population aged 30-69 years, and its distribution between capital city and other statistical divisions for the years 1986 and 1996. We also obtained ABS data for mortality from all causes, and from CHD, acute myocardial infarction (AMI) and subacute and chronic myocardial ischaemia for men and women aged 30-69 years living within and outside capital city statistical divisions for each year from 1986 to 1996. We excluded deaths at 70 or more years because certification of the cause of death in older people may be unreliable.6 We defined mortality from CHD as deaths with an underlying cause classified under rubrics 410, 411, 413 and 414 of the International classification of diseases, ninth revision (ICD-9-CM),7 with mortality from AMI classified under ICD-9-CM rubric 410, and mortality from subacute and chronic myocardial ischaemia classified under rubrics 411, 413, 414. | |
| Statistical methods | ||
|
Annual age-standardised rates for mortality from all causes, CHD,
AMI and subacute and chronic myocardial ischaemia were calculated as
follows:
The number of deaths in each age group (30-39, 40-49,
50-59 and 60-69 years), coded to each cause of death category, were
summed. Age-specific rates were calculated and then standardised
with weightings obtained from Segi's "world population" (World
Health Organization standard population).8 The normal approximation
for the distribution was used to calculate 95% confidence intervals.
For each State and the Northern Territory, we calculated expected numbers of deaths in each age group for populations living outside capital city statistical divisions by applying age-specific mortality rates from populations living within the capital city statistical division. Differences between the actual (observed) number of deaths and the expected number of deaths were then summed across 10-year age strata to give total expected numbers of deaths. Excess deaths were calculated as the difference between the sum of the observed and the sum of the expected number of deaths for all States and the Northern Territory. The population of the Australian Capital Territory living outside the Canberra Statistical Division was less than 0.1% of the total population of the ACT and was not included in the calculation. | ||
| Results | ||
| Population size and distribution | ||
| Unpublished regional population data from the ABS estimated that, in 1986, there were 7 174 246 Australians aged 30-69 years, 64.4% of whom lived in capital city statistical divisions. The sex distribution in capital cities was 49.9% men and 50.1% women, compared with 51.0% men and 49.0% women outside capital cities. By 1996, the estimated population of Australians aged 30-69 years had increased to 8 793 107, 63.5% of whom lived in capital city statistical divisions. The sex distribution in capital cities was 49.8% men and 50.2% women, compared with 50.7% men and 49.3% women outside capital cities. | ||
| Trends in mortality rates among men | ||
|
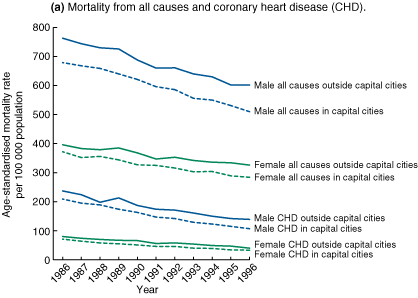
Between 1986 and 1996, mortality from all causes in all
30-69-year-old Australian men declined by 23%; this decline within
capital city statistical divisions was 25%, compared with 21% among
men living outside capital city statistical divisions (Box 1).
Mortality from all causes in populations outside the capital cities
remained higher than in capital city populations, with the
difference increasing from 12% in 1986 to 18% in 1996.
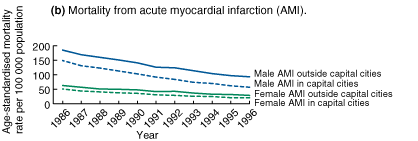
Between 1986 and 1996, mortality from CHD in Australian men aged 30-69 years declined by 46% and accounted for 61% of the decline in all-cause mortality. Mortality among men living within capital city statistical divisions declined by 49%, compared with 41% among men living outside capital city statistical divisions (Box 1). Mortality from CHD in populations outside the capital cities remained higher than in capital city populations, with the difference increasing from 13% in 1986 to 30% in 1996. Mortality from AMI among men living within capital city statistical divisions declined by 62%, compared with 50% among men living outside capital city statistical divisions (Box 1). Mortality from AMI in men living outside the capital cities remained higher than in capital city populations, with the difference increasing from 24% in 1986 to 63% in 1996. | ||
| Excess mortality outside capital city statistical divisions | ||
|
Box 2 shows that, among men, CHD accounts for 32% of the excess deaths
from all causes from 1986 to 1996 occurring outside the capital city
statistical divisions. Among those deaths coded as CHD, observed
deaths from AMI exceeded expected deaths by 5487. The number of excess
deaths from CHD is smaller than that from AMI, as there was a higher rate
of death from subacute and chronic myocardial ischaemia in capital
city populations.
Observed deaths from AMI among men aged 30-39 years living outside capital city statistical divisions exceeded expected deaths by 79%; corresponding figures for the remaining age groups were 72% (40-49 years), 51% (50-59 years), and 25% (60-69 years).
| ||
| Trends in mortality rates among women | ||
|
Between 1986 and 1996, mortality from all causes in all
30-69-year-old Australian women declined by 21%; this decline
within capital city statistical divisions was 24%, compared with 18%
among women living outside capital city statistical divisions (Box
1). Mortality from all causes in populations outside the capital
cities remained higher than in capital city populations, with the
difference increasing from 6% in 1986 to 15% in 1996.
Between 1986 and 1996, mortality from CHD in Australian women aged 30-69 years declined by 51% and accounted for 48% of the decline in all-cause mortality. Mortality among women living within capital city statistical divisions declined by 54%, compared with 50% among women living outside capital city statistical divisions (Box 1). Mortality from CHD in populations outside the capital cities remained higher than in capital city populations, with the difference increasing from 13% in 1986 to 21% in 1996. Mortality from AMI among women living within capital city statistical divisions declined by 59%, compared with 54% among women living outside capital city statistical divisions (Box 1). Mortality from AMI in women living outside the capital cities remained higher than in capital city populations, with the difference increasing from 24% in 1986 to 38% in 1996. | ||
| Excess mortality outside capital city statistical divisions | ||
|
Box 2 shows that, among women, CHD accounts for 27% of the excess
mortality from all causes occurring outside the capital city
statistical divisions. Observed deaths from AMI exceeded expected
deaths by 1479.
Observed deaths from AMI among women aged 30-39 years living outside capital city statistical divisions exceeded expected deaths by 108%; corresponding figures for the remaining age groups were 75% (40-49 years), 44% (50-59 years), and 20% (60-69 years). | ||
| Overall mortality | ||
| Box 3 shows that death rates from CHD outside capital cities are consistently higher than within capital cities in all Australian States and the Northern Territory, the only exception being mortality from CHD among women in the Northern Territory in 1986. | ||
| Discussion |
The contribution of reduced CHD mortality to the overall decline in
all-cause mortality in Australia from 1986 to 1996 was 61% for men and
48% for women. However, our findings show that CHD mortality rates
were higher outside capital cities, and that discrepancies
increased from 1986 to 1996 and were largest in younger age groups.
It is likely that the differences we found in CHD mortality are real, as they are matched by parallel trends in all-cause mortality rates, and at least two studies have confirmed the validity of deaths coded by the ABS to CHD.9,10 While a study based on 1979 data questioned the validity of subcategories of CHD such as rubric 410 (AMI),11 we found consistently higher death rates from AMI in populations outside capital cities in all Australian States and the Northern Territory (data not shown), despite variations in medical certification requirements between States. The apparent higher rates of mortality in capital city populations from subacute and chronic CHD may be the result of a coding anomaly or of deaths occurring in large population centres after patients were moved there for the management of their subacute or chronic CHD. Our study was limited to documenting the difference in CHD mortality between capital cities and other areas. Clearly, an understanding of the factors associated with higher CHD mortality outside capital cities has implications for prevention and improved treatment of CHD. This would require detailed examination of population characteristics to determine which populations outside capital cities, including subpopulations such as Indigenous people, are most at risk of higher mortality. It is also necessary to consider factors such as differences in socioeconomic status, in risk factors for CHD, and in access to medical care. Previous reports showed that the decline in mortality from CHD in NSW was slower in lower income populations, many of which were in rural or regional areas.12,13 Also, sudden cardiac death in Tasmanian men was found to occur twice as frequently in unemployed men compared with employed men.14 While the association between populations with lower socioeconomic status and higher risk for CHD is recognised, the actual factors that influence this association have not been well delineated. Risk factors for CHD clearly have an influence on mortality. Much of the decline in mortality from CHD in Finland from 1972 to 1992 can be explained by changes in the three main coronary risk factors: serum cholesterol level, blood pressure and smoking.15 In Australia, the National Heart Foundation (NHF) Risk Factor Prevalence Surveys found significant declines between 1980 and 1989 in the prevalence of hypertension and cigarette smoking, but no overall favourable trend in lipid levels.16 However, these surveys are limited to capital cities, and it is not known whether regional areas of Australia have seen the same trends in risk factor prevalence. In 1992, a major risk factor prevalence survey based on the 1989 NHF Risk Factor Prevalence Survey was undertaken in two rural regions of Tasmania. The prevalence of major coronary risk factors was consistent with the high rate of mortality from CHD among men in North-West Tasmania, but did not explain variation in rates of mortality in women across the three regions of Tasmania.17 Differences in mortality from CHD may be the result of differential incidences of CHD or differences in case-fatality rates. A detailed study of sudden cardiac death among previously asymptomatic men found that the higher rate of deaths in the two rural regions of Tasmania occurred mostly among men for whom symptomatic CHD could have been diagnosed, implying a higher case-fatality rate for CHD.14 This finding was supported by higher rates of coronary deaths occurring after hospitalisation in the two rural regions of Tasmania from 1986 to 1989,4 and in Newcastle in 1984.18 A higher case-fatality rate may result from differences in risk of death from factors such as previous infarction, delays in reaching medical care, or differences in medical care.19 While the relative geographic isolation of most populations outside the capital cities may be expected to result in delays in reaching secondary and tertiary medical centres, the findings of the MONICA study did not support changes in time to medical care (including ambulance staff) having a significant effect on deaths before hospitalisation in major population centres.18 A significant decline in case fatality after hospitalisation did, however, make an important contribution to the overall decline in coronary deaths in the MONICA centres of Auckland (New Zealand), Newcastle (Australia) and Perth (Australia) from 1984 to1993. Medical management of acute coronary events has changed substantially over the past 20 years. The use of aspirin, thrombolytic therapy and coronary angioplasty as first-line treatments for AMI has resulted in reductions in mortality of up to 43%.20,21 The use of thrombolytic therapy in the MONICA centres increased from being rare in the early 1980s, to being used in approximately 50% of hospitalised patients with non-fatal definite myocardial infarction or coronary death by the early 1990s.22,23 The benefits of such treatments are dependent on them being given soon after the event,24 and it is not clear whether populations living at any distance from secondary or tertiary medical centres experience delays in access to new treatment methods for symptomatic CHD. In southern Tasmania between 1992 and 1996, 849 doses of streptokinase and tissue plasminogen activator were administered for AMI. No thrombolytic therapy was administered outside the capital city of Hobart (Royal Hobart Hospital Pharmacy Supplies Report), despite 15% of the population of the Southern Region living outside the capital city and having mortality rates approximately 40% higher than the capital city population. In conclusion, although there have been impressive declines in mortality from CHD in all Australian States and Territories over the past 30 years, the 35% of the Australian population living outside the capital cities continue to have higher coronary mortality. Our results indicate the need for increased research into factors which may influence mortality rates for CHD in rural and remote areas. | |
Acknowledgements | ||
| This study was supported by funding from Roche Products Pty Ltd and the Tasmanian branch of the AMA, and by assistance in-kind from the Hobart City Council and Australian Hospital Care Ltd. We are grateful to Chris Sweeney from the Australian Bureau of Statistics and to the Pharmacy Department of the Royal Hobart Hospital. | ||
| References |
(Received 23 Sep 1999, accepted 31 Jan 2000) | |
Authors' details | ||
|
The Hobart Private Hospital, Hobart, TAS.
Peter T Sexton, PhD, FAFPHM, Director of Medical Services; Tiina-Liisa H Sexton, BCom, CA, Research Assistant. Reprints: Dr P T Sexton, The Hobart Private Hospital, Cnr Argyle and Collins Streets, Hobart, TAS 7000. | ||
| 2: Estimated excess deaths from all causes, CHD and AMI among men and women living outside capital city statistical divisions from 1986 to 1996 | |||||
| Age group (years) | |||||
| 30-39 | 40-49 | 50-59 | 60-69 | Total | |
| Men | |||||
| Mortality from all causes | |||||
| Observed deaths | 8599 | 12698 | 26227 | 60856 | 108380 |
| Expected deaths | 7363 | 10718 | 21619 | 56725 | 96425 |
| Excess deaths | 1236 | 1980 | 4608 | 4131 | 11955 |
| Mortality from CHD (ICD-9-CM 410, 411, 413, 414) | |||||
| Observed deaths | 682 | 2703 | 7239 | 18241 | 28865 |
| Expected deaths | 493 | 2099 | 5902 | 16536 | 25030 |
| Excess deaths | 189 | 604 | 1337 | 1705 | 3835 |
| Mortality from AMI (ICD-9-CM 410) | |||||
| Observed deaths | 470 | 1972 | 5334 | 13287 | 21063 |
| Expected deaths | 263 | 1144 | 3541 | 10628 | 15576 |
| Excess deaths | 207 | 828 | 1793 | 2659 | 5487 |
| Women | |||||
| Mortality from all causes | |||||
| Observed deaths | 3887 | 7021 | 13863 | 31467 | 56238 |
| Expected deaths | 3202 | 5998 | 11972 | 29918 | 51090 |
| Excess deaths | 685 | 1023 | 1891 | 1549 | 5148 |
| Mortality from CHD (ICD-9-CM 410, 411, 413, 414) | |||||
| Observed deaths | 143 | 537 | 1878 | 6937 | 9495 |
| Expected deaths | 91 | 381 | 1503 | 6135 | 8110 |
| Excess deaths | 52 | 156 | 375 | 802 | 1385 |
| Mortality from AMI (ICD-9-CM 410) | |||||
| Observed deaths | 102 | 391 | 1400 | 5073 | 6966 |
| Expected deaths | 49 | 223 | 972 | 4243 | 5487 |
| Excess deaths | 53 | 168 | 428 | 830 | 1479 |
| CHD=coronary heart disease. AMI=acute myocardial infarction | |||||
| 3: Mortality within and outside capital city statistical divisions by Australian States and Territories | ||||||
| Men | ||||||
| Age-standardised mortality rate per 100000 (95% CI) | % change | Estimated excess | ||||
| 1986 | 1996 | per year | deaths from CHD | |||
| All causes | CHD | All causes | CHD | from CHD | 1986-1996 | |
| New South Wales | ||||||
| Capital | 722 (702-741) | 223 (212-234) | 511 (496-527) | 106 (99-113) | -4.8 | |
| Balance | 761 (736-786) | 232 (218-246) | 601 (581-622) | 143 (133-153) | -3.5 | 1506 |
| Victoria | ||||||
| Capital | 658 (638-678) | 199 (188-210) | 487 (470-503) | 97 (90-105) | -4.7 | |
| Balance | 755 (722-789) | 242 (223-261) | 583 (556-611) | 131 (118-144) | -4.2 | 1015 |
| Queensland | ||||||
| Capital | 691 (657-724) | 226 (207-245) | 549 (523-575) | 122 (109-134) | -4.2 | |
| Balance | 754 (723-785) | 227 (210-245) | 585 (562-609) | 136 (125-147) | -3.6 | 444 |
| South Australia | ||||||
| Capital | 653 (619-687) | 213 (194-232) | 528 (499-557) | 125 (110-139) | -3.8 | |
| Balance | 707 (650-764) | 234 (201-267) | 633 (583-683) | 160 (135-186) | -2.9 | 291 |
| Western Australia | ||||||
| Capital | 638 (603-673) | 183 (164-202) | 498 (471-525) | 102 (89-114) | -4.0 | |
| Balance | 779 (716-841) | 249 (214-285) | 594 (546-642) | 121 (100-143) | -4.7 | 203 |
| Tasmania | ||||||
| Capital | 605 (526-684) | 141 (103-179) | 595 (520-669) | 102 (71-133) | -2.5 | |
| Balance | 758 (685-831) | 276 (232-320) | 619 (558-680) | 144 (115-174) | -4.3 | 243 |
| Northern Territory | ||||||
| Capital | 640 (463-817) | 115 (46-185) | 716 (569-863) | 97 (36-158) | -1.4 | |
| Balance | 1443 (1206-1679) | 233 (138-329) | 1030 (862-1199) | 132 (73-191) | -3.9 | 133 |
| Australian Capital Territory | ||||||
| 598 (521-675) | 205 (159-251) | 428 (372-484) | 111 (82-140) | -4.2 | ||
| All of Australia | ||||||
| Capital | 679 (668-690) | 209 (203-215) | 510 (501-519) | 107 (103-111) | -4.4 | |
| Balance | 763 (747-778) | 237 (228-245) | 602 (590-614) | 139 (133-145) | -3.8 | 3835 |
| Women | ||||||
| Age-standardised mortality rate per 100000 (95% CI) | % change | Estimated excess | ||||
| 1986 | 1996 | per year | deaths from CHD | |||
| All causes | CHD | All causes | CHD | from CHD | 1986-1996 | |
| New South Wales | ||||||
| Capital | 391 (377-405) | 82 (76-88) | 284 (273-296) | 32 (28-36) | -5.5 | |
| Balance | 420 (401-439) | 89 (80-97) | 335 (319-350) | 45 (39-51) | -4.5 | 564 |
| Victoria | ||||||
| Capital | 360 (346-375) | 65 (59-72) | 274 (262-286) | 31 (27-35) | -4.8 | |
| Balance | 361 (338-384) | 68 (58-77) | 307 (287-327) | 35 (28-41) | -4.4 | 277 |
| Queensland | ||||||
| Capital | 371 (347-395) | 67 (57-78) | 308 (288-328) | 39 (32-46) | -3.8 | |
| Balance | 378 (355-400) | 75 (65-85) | 299 (282-316) | 36 (30-42) | -4.7 | 171 |
| South Australia | ||||||
| Capital | 347 (323-371) | 69 (58-79) | 285 (264-306) | 31 (24-38) | -5.0 | |
| Balance | 291 (317-400) | 83 (64-103) | 339 (301-377) | 39 (26-52) | -4.8 | 143 |
| Western Australia | ||||||
| Capital | 349 (324-374) | 59 (49-70) | 275 (255-295) | 37 (30-45) | -3.4 | |
| Balance | 386 (339-433) | 78 (296-372) | 334 (57-99) | 36 (24-49) | -4.9 | 105 |
| Tasmania | ||||||
| Capital | 424 (360-488) | 68 (42-93) | 365 (308-422) | 49 (28-70) | 22.5 | |
| Balance | 421 (367-475) | 87 (62-111) | 385 (336-434) | 54 (36-72) | -3.4 | 62 |
| Northern Territory | ||||||
| Capital | 434 (271-597) | 46 (-10-103) | 392 (261-523) | 41 (-3-86) | -1.0 | |
| Balance | 911 (702-1120) | 37 (-6-81) | 762 (593-932) | 88 (28-148) | +12.5 | 63 |
| Australian Capital Territory | ||||||
| 380 (319-440) | 56 (32-80) | 267 (223-311) | 41 (23-59) | -2.4 | ||
| All of Australia | ||||||
| Capital | 372 (363-380) | 71 (68-75) | 284 (278-291) | 33 (31-36) | -4.9 | |
| Balance | 396 (384-407) | 80 (75-85) | 326 (317-335) | 40 (37-44) | 24.5 | 1385 |
| CHD=coronary heart disease. Capital=within capital city statistical divisions. Balance=outside capital city statistical divisions. | ||||||
Received 9 June 2026, accepted 9 June 2026
- Peter T Sexton
- Tiina-Liisa H Sexton
- The Hobart Private Hospital, Cnr Argyle and Collins Streets, Hobart, TAS 7000