|
Research
Randomised controlled trial of general practice based asthma
clinics
Adrian R Heard, Ian J Richards, John H Alpers, Louis S Pilotto, Brian J
Smith and Julie A Black
MJA 1999; 171: 68-71
See also Gibson & Abdulwadud et al
Abstract -
Introduction -
Methods -
Results -
Discussion -
Acknowledgements -
References -
Authors' details
-
-
More articles on General practice and primary care
|
Abstract |
Objective: To compare the effects on asthma
morbidity of asthma clinics based in general practice with standard
general practice care.
Design and setting: A randomised controlled trial in
eight general practices. Patients, general practitioners and
outcomes assessors were not blinded to treatment allocation.
Participants: 195 patients with asthma aged 5-64 years; 191
completed the trial.
Intervention: Three asthma clinic sessions over six
months involving nurse counselling, education about asthma
management, spirometry and consultation with the general
practitioner.
Main outcome measures: Patients reporting days lost from
work or school, number of days lost, the presence of morning or
nocturnal asthma symptoms, use of an action plan, medication use,
current smoking, hospitalisation, and emergency visits.
Results: Asthma clinics were associated with a greater
reduction in nocturnal symptoms, an increase in the ownership of peak
flow meters and an increase in the number of patients commencing or
resuming smoking. Both control and intervention groups showed
similar improvement in days lost from work or school, the presence of
symptoms, use of an action plan and taking reliever medication.
Conclusion: Our study does not show that asthma clinics
are more effective than standard general practice care in reducing
asthma morbidity. It is uncertain how much of the improvement in
outcomes was due to the asthma clinic, the influence of the study
itself upon patients and practitioners, or other factors, such as the
tendency for a patient's asthma management to improve over time.
|
| | Introduction |
Asthma is the most common chronic disease in children and a leading
cause of morbidity in adults in Australia.1,2 Asthma clinics may be a way
of improving comanagement practices between health professionals
and people with asthma. They involve trained nurses conducting
asthma education, peak flow readings and spirometry with asthma
patients, combined with a brief general practitioner review.
Asthma clinics are an integral part of general practice in the United
Kingdom, but have yet to gain acceptance in Australia.3 One reason for
this might be that studies have not provided conclusive evidence that
these clinics reduce morbidity.4-9 This may be because
regular general practitioner review10 and/or asthma
education11 is the key element in
reducing asthma morbidity, and therefore only studies comparing
asthma clinics with patients receiving irregular reviews are likely
to show significant differences in outcomes.
In this study, we used a randomised controlled trial design to test
whether asthma clinics (intervention) were more effective in
reducing morbidity from asthma than standard medical treatment
(control). The clinics used the Patient Management System, a
recognised model for operating asthma clinics.12 |
| |
Methods |
| |
Ethical approval | |
Ethics approval for the study was obtained through the Royal
Australian College of General Practitioners' ethics committee at
the RACGP national office.
| |
Recruitment |
A previous major study of asthma self-management found a 50%
reduction in the number of people reporting at least one day lost from
work.6 We calculated that to detect
a similar reduction in a study with 80% power and a 95% confidence
interval a sample size of 170 was required.
Patients were recruited from eight general practices staffed by 42
general practitioners. Consent was sought from all people with
asthma aged 5-64 years attending these practices during three months
of 1997.
Subjects were individually randomised within practices into
intervention and control groups. This meant that each participating
general practitioner potentially saw both intervention and control
patients. A randomisation chart was set up for each participating
practice at Asthma South Australia, and general practitioners and
the asthma educators were informed of a subject's treatment
allocation before the baseline interview. Thus, patients, doctors
and outcome assessors were not blinded as to who had received the
intervention and who were controls.
| |
Intervention |
Each general practice operated one three-hour asthma clinic session
per week. The asthma educators in the trial were practising
registered nurses with extensive experience in respiratory care.
Their component of the clinic session involved education in asthma
management strategies, including a written asthma management plan,
spirometry and instruction on using peak flow meters, inhalers and an
asthma diary card. The session ended with a consultation by the
general practitioner. Each asthma clinic patient was asked to attend
three asthma clinic sessions within the six months of the study.
| |
Gathering outcomes data | |
We conducted a telephone interview using adapted questions from the
Southampton Morbidity Index13 and questions relating to
clinical practice14 at the beginning and end of
the study. Our outcome measures included number of patients
reporting days lost from work or school, number of days lost, use of an
action plan, medication use, current smoking, the level of morning or
nocturnal asthma symptoms, hospitalisation, emergency visits, and
number of home visits by the general practitioner.
| |
Data analysis |
All data were analysed on an intention-to-treat basis.
For analysis, we categorised morning and nocturnal symptoms as "at
least weekly" or "less frequently/never" to distinguish regular
from irregular symptoms and to maintain adequate numbers of
participants in each of the two categories. We analysed the number of
days lost from work with both linear and logistic regression. Linear
regression was conducted on the difference in the number of days lost
from work between baseline and six months, and was adjusted for
clustering by doctor. For logistic regression, also adjusted for
clustering by doctor, the variable was divided into two categories
(two or fewer days lost and three or more days lost), representing
better-controlled and less well controlled asthma, respectively.
The statistical analyses for all other study factors used logistic
regression, adjusted for baseline measurements and clustering by
treating doctor. We also conducted a longitudinal analysis using
χ2
tests to examine changes in the intervention and control groups over
the six months of the trial.
Odds ratios and 95% confidence intervals (95% CIs) were calculated
for all outcome measures. All tests were conducted using the Stata
statistical software package.15 |
| |
Results |
| |
Patients |
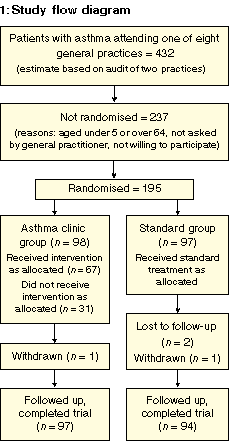
Over the three-month recruitment period, 195 people entered the
study, and 191 (97 in the clinic group and 94 controls) completed both
interviews (Box 1). The demographic profile of the control group
(mean age, 26.3 years, 95% CI, 22.3-30.2; proportion of males, 45%,
95% CI, 34%-55%) was similar to the intervention group (mean age, 27.5
years, 95% CI, 23.6-31.4; proportion of males, 42%, 95% CI 32%-52%).
Although there were no records of the number of eligible subjects
across all participating practices, an audit of all patients seeing
general practitioners at two of the eight practices showed a
participation rate of 45.1% of all asthmatics. The main reasons for
non-participation were either the general practitioner's failing
to ask the patient for consent or the patient's refusing consent. The
average age of non-participants (mean age, 20.8 years, 95% CI
17.1-24.5) was not significantly different from that of
participants (mean age, 21.4 years, 95% CI 17.1-25.7) in the two
audited practices. Of the 97 people in the clinic group, 67 completed
the three planned clinic sessions, 17 attended only one or two
sessions, and 13 failed to attend any sessions.
| |
Outcomes |
There was no difference between the clinic and control groups at
baseline for dichotomous study variables (Box 2), which provided
evidence for effective randomisation. There was a low incidence of
hospitalisation and emergency department attendance in both
groups. At six months, however, waking at night at least weekly due to
asthma and current smoking were significantly different between the
two groups, as was ownership of a peak flow meter (Box 3). There were no
differences reported at six months in patients' having discussed
trigger factors with their general practitioner or receiving an
action plan from their general practitioner.
Unlike the dichotomous outcome variables, the mean number of days
lost from work was significantly different between the treatment
groups at baseline, with a high level of variability in the control
data (intervention group mean, 2.62, 95% CI 1.84-3.40; control group
mean, 5.37; 95% CI 3.46-7.29). There was no difference in the number of
days lost from work at six months in the intervention group compared
with the control group (intervention group mean, 2.09, 95% CI
0.91-3.27; control group mean, 2.66; 95% CI 1.66-3.66). Linear
regression to compare the number of days lost at six months minus those
at baseline between intervention and control participants showed a
significant reduction in number of days lost in the control group
compared with the intervention group (P = 0.04). Logistic
regression comparing two or fewer days lost with three or more days
lost showed a non-significant trend towards fewer days lost from work
at six months in the intervention group (odds ratio, 0.50; 95% CI
0.24-1.03). Longitudinal analyses within the clinic and control
groups showed a trend towards decreasing morbidity over the
six-month period, with a 13% decrease in the number of people
reporting days lost from work, school or usual activities in both
groups (intervention group odds ratio, 0.57, 95% CI 0.31-1.06;
control group odds ratio, 0.57, 95% CI 0.31-1.06). Longitudinal
analyses also showed that the reported issuing of action plans
increased significantly in both groups (intervention group odds
ratio, 11.25, 95% CI 3.07-41.21; control group odds ratio, 3.94, 95%
CI 1.53-10.10). An increase in the discussion of trigger factors was
only significant for the control group (intervention group odds
ratio, 2.6, 95% CI 0.84-8.02; control group odds ratio, 3.72, 95% CI
1.36-10.21).
|
| |
Discussion |
Our study does not show that asthma clinics are more effective than
standard general practice care in reducing asthma morbidity. We
observed an improvement in most of the outcome measures in both the
intervention and control groups. Outcomes for patients who attended
an asthma clinic had few differences from those in the control group.
The intervention group was less likely to be woken "at least weekly" at
night due to asthma. This may signal better home management of asthma
in the intervention group, an outcome that is anticipated by
guidelines16 but challenged in recent
studies.17 Ownership of peak flow
meters increased among the intervention group during the course of
the study, probably because the asthma educators promoted the use of
peak flow readings for asthma self-management.
More people in the intervention group either adopted or recommenced
smoking during the study. Smoking cessation advice was not included
as part of the study intervention. In intensive interventions such as
asthma clinics, smokers should be identified to ensure that smoking
cessation is achieved or maintained if possible.
In this study there were few reports of hospitalisations and
emergency department visits at baseline, reflecting our broad
inclusion criteria, which did not focus on severe asthmatics.
Outcomes which were infrequent in this study may be significant in
much larger studies.
In relation to days lost from work or school, the significant
difference between the intervention and control groups at baseline,
the high variability at baseline in the control group and the
different findings between the logistic and linear regressions at
six months do not allow an adequate understanding of the effect of the
intervention.
The lack of difference between groups in the proportion of
participants who had discussed trigger factors with their doctor and
who had received an asthma action plan raises one of the possible
explanations for the limited differences observed in this study.
Baseline levels of both these clinical practice indicators are
usually around 40%-60%,14 and were within that range
at baseline in our study. Yet the frequency of both indicators
increased substantially over the six months for both groups, which
might suggest that clinical practice for the control subjects was
contaminated as a result of general practitioners' seeing both
intervention and control subjects.
Other explanations may be:
- The asthma clinic in itself
makes no difference to the outcomes being measured, and that a simpler
intervention, such as regular general practitioner review, is the
critical factor. The results of a review of asthma education support
this.10 Whether the presence of an
asthma clinic in a general practice increases the rate of general
practitioner review is unknown.
- A possible Hawthorne effect.18 With general
practitioners and patients being unblinded to the study, it is
possible that both increased behaviours which led to better asthma
self-management outcomes.
- People with asthma tend to show improved outcomes over time. This
effect is likely to be enhanced after a visit to a general practitioner
where management decisions are made. The data showing that the number
of people reporting days lost from work or school decreased in both
intervention and control groups support this explanation.
- Baseline data may have been biased because subjects were randomised
into treatment groups before the baseline interview, and some
subjects may have been aware of their treatment status at the baseline
interview.
Whatever reasons led to the apparent improvement in outcomes, a
factor that may have contributed to the lack of difference between
intervention and control groups may be the poor compliance with the
intervention regimen. Nearly one-third of patients from the
intervention group did not comply with the required three clinic
visits, and 13% did not attend any visits.
The outcome of this study holds some lessons for future randomised
controlled trials in general practice. The major limitation of the
study was the randomisation by patient rather than practice, which
may lead to modification of general practitioner behaviour towards
the control group as well as the intervention group, thus increasing
the chance of contamination of controls and the Hawthorne effect.
The inability to blind general practitioners and patients to the
patient's treatment allocation also limited the study.
The participation rate of less than 50% is lower than the rate
considered desirable for randomised controlled trials, but
compares favourably with other community-based
studies.6,19
This study also demonstrates that, in general practice, larger,
longer-term or more targeted studies (such as to more severe
asthmatics) are required to show differences, especially for
variables such as hospitalisation for asthma, which have a
relatively low incidence among most general practice patients.
Conducting this study for a longer period would also have allowed it to
run over the full range of seasons, which is preferable for studies of
seasonal diseases such as asthma.
|
Acknowledgements | |
We would like to thank the two nurses who conducted the asthma clinics,
and Kieran McCaul from the Department of Human Services, South
Australia, for statistical advice on the final drafts of the article.
Thanks also go to the doctors and staff at the following participating
practices: Angaston Medical Centre, Brooker Clinic, Greenwith
Medical Centre, Golden Grove Medical Centre, Flinders Clinic,
Nuriootpa Medical Centre, North Plympton Medical Centre and Tanunda
Medical Centre. This study was made possible through a grant from the
Department of Human Services, Adelaide, South Australia.
|
| |
References |
- Abramson M, Kutin J, Czarny D, et al. The prevalence of asthma and
respiratory symptoms among young adults: Is it increasing in
Australia? J Asthma 1996; 33: 189-196.
-
Peat JK, Toelle BG, Gray EJ, et al. Prevalence and severity of
childhood asthma and allergic sensitisation in seven climatic
regions of New South Wales. Med J Aust 1995; 163: 22-26.
-
Barnes G, Partridge MR. Community asthma clinics: 1993 survey of
primary care by the National Asthma Task Force. Qual Health
Care 1994; 3: 133-136.
-
Jones KP, Mullee MA. Proactive, nurse-run asthma care in general
practice reduces asthma morbidity: scientific fact or medical
assumption? Br J Gen Pract 1995; 45: 497-499.
-
Lahdensuo A, Haahtela T, Herrala J, et al. Randomised comparison of
guided self-management and traditional treatment of asthma over one
year. BMJ 1996; 312: 748-752.
-
Mayo PH, Richman J, Harris HW. Results of a program to reduce
admissions for adult asthma. Ann Intern Med 1990; 112:
864-871.
-
Martys C. Asthma care in Darley Dale: general practitioner audit.
BMJ 1992; 304: 758-760.
-
Evans D, Mellins R, Lobach K, et al. Improving care for minority
children with asthma: Professional education in public health
clinics. Paediatrics 1997; 99: 157-164.
-
Charlton I, Charlton G, Broomfield J, et al. Audit of the effect of a
nurse run asthma clinic on workload and patient morbidity in a general
practice. Br J Gen Pract 1991; 41: 227-231.
-
Gibson P, Coughlan J, Abramson M, et al. The effects of
self-management education and regular practitioner review in
adults with asthma. (Cochrane Review). In: The Cochrane Library,
Issue 2. Oxford: Update Software; 1998.
-
Bauman A. Effects of asthma patient education upon psychological
and behavioural outcomes. Int Rev Health Psych 1993; 2:
199-212.
-
Charlton I, Antoniou AG, Atkinson J, et al. Asthma at the
interface: bridging the gap between general practice and a district
general hospital. Arch Dis Child 1994; 70: 313-318.
-
Jones K, Charlton I, Middleton M, et al. Targeting asthma care in
general practice using a morbidity index. BMJ 1992; 304:
1353-1356.
-
Beilby J, Wakefield M, Ruffin R. Reported use of asthma management
plans in South Australia. Med J Aust 1997; 166: 298-301.
-
StataCorp. Stata Statistical Software: Release 5.0. [computer
program]. College Station, Texas: Stata Corporation, 1997.
-
The Thoracic Society of Australia and New Zealand. Peak flow meter
use in asthma management. Med J Aust 1996; 164: 727-730.
-
Garrett J, Fenwick J, Taylor G, et al. Peak expiratory flow meters
(PEFMs): who uses them and how does education affect the pattern of
utilisation? Aust N Z J Med 1994; 24: 521-528.
-
Rice B. The Hawthorne effect: persistence of a flawed theory.
Psychol Today 1982; 16: 71-74.
-
Garrett J, Fenwick J, Taylor G, et al. Prospective controlled
evaluation of the effect of a community based asthma education centre
in a multiracial working class neighbourhood. Thorax 1994;
49: 976-983.
(Received 4 May 1998, accepted 31 May 1999)
|
| | Authors' details |
SA HealthPlus, Department of Human Services, Adelaide, SA.
Adrian R Heard, BSocAdmin, MPH, Senior Project Officer.
Centre for Health Care Evaluation, Bedford Park, SA.
Ian J Richards, BApplSc, MPH, Project Officer.
Flinders Medical Centre, Bedford Park, SA.
John H Alpers, MD, FRACP, Director, Respiratory Unit.
North Western Adelaide Health Service, Woodville South, SA.
Louis S Pilotto, FAFPHM, PhD, Senior Consultant.
Brian J Smith, FRACP, PhD, Senior Lecturer, Department of
Medicine.
Asthma SA, Royston Park, SA.
Julie A Black, BNG, Chief Executive Officer.
Reprints will not be available from the authors.
Correspondence: Mr A
R Heard, SA HealthPlus, PO Box 65, Rundle Mall, SA 5000.
Email: Adrian.HeardaATdhs.sa.gov.au
|
| |  | | Back to text | | 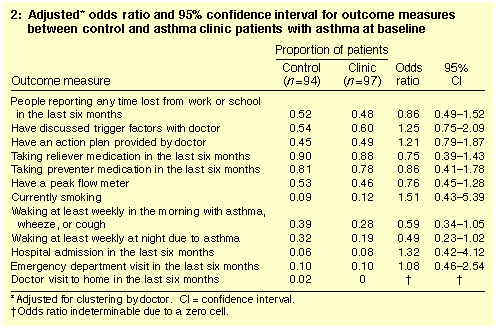 | | Back to text | | 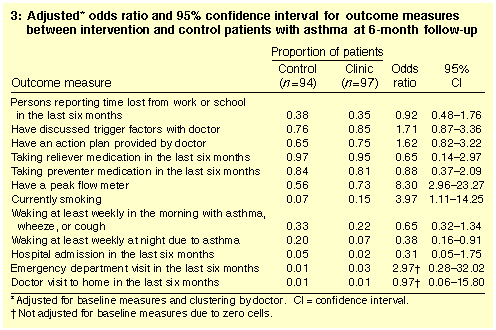 | | Back to text |
|







