|
Research
An analysis of the causes of adverse events from the
Quality in
Australian Health Care Study
Ross McL Wilson, Bernadette T Harrison, Robert W Gibberd and John D
Hamilton
MJA 1999; 170: 411-415
For editorial comment, see Vincent
Abstract -
Introduction -
Methods -
Results -
Discussion -
Acknowledgements -
References -
Authors' details
-
-
More articles on Administration and health services
|
The Quality in Australian Health Care Study (QAHCS), published in the Journal in 1995,1 reported that 16.6% of hospital admissions were associated with an iatrogenic patient injury, termed an adverse event (AE) (see Box 1). This compares with the rate of 3.7% for AEs in the Harvard Medical Practice Study (HMPS),2 and a rate of 17% in a more recent study with an alternative observational method of determining AEs.3
Fifty per cent of the AEs in the QAHCS were judged to have a high preventability score (4 or more on a scale of 1-6 of increasing likelihood of preventability).1 The disability caused by these adverse events ranged from temporary disability (fully resolved in one month) in 46.6% of AEs, to death in 4.9% of AEs. Although recording AEs emphasises only the "complications" of rather than the benefits derived from healthcare, AEs are of great significance to individual patients as well as to the whole healthcare system. |
| |
Abstract |
Objective: To examine the causes of adverse events
(AEs) resulting from healthcare to assist in developing strategies
to minimise preventable patient injury.
Design: Descriptions of the 2353 AEs previously reported
by the Quality in Australian Health Care Study (QAHCS) were reviewed.
A qualitative approach was used to develop categories for human error
and for prevention strategies to minimise these errors. These
categories were then used to classify the AEs identified in the QAHCS,
and the results were analysed with previously reported
preventability and outcome data.
Results: 34.6% of the causes of AEs were categorised as
"a complication of, or the failure in, the technical performance
of an indicated procedure or operation", 15.8% as "the
failure to synthesise, decide and/or act on available
information", 11.8% as "the failure to request or arrange an
investigation, procedure or consultation", and 10.9% as "a
lack of care and attention or failure to attend the patient". AEs in
which the cause was cognitive failure were associated with higher
preventability scores than those involving technical performance.
The main prevention strategies identified were "new, better, or
better implemented policies or protocols" (23.7% of
strategies), "more or better formal quality monitoring or
assurance processes" (21.2%), "better education and
training" (19.2%), and "more consultation with other
specialists or peers" (10.2%).
Conclusion: The causes of AEs or errors leading to AEs can
be characterised, and human error is a prominent cause. Our study
emphasises the need for designing safer systems for care which
protect the patient from the inevitability of human error. These
systems should provide new policies and protocols and technological
support to aid the cognitive activities of clinicians.
|
| | Introduction |
An additional analysis of data from the Quality in Australian Health
Care Study (QAHCS)1 was undertaken in order to
understand more fully the causes of the adverse events (AEs)
identified and to assist in developing prevention strategies. Here,
we describe the error or errors in the delivery of healthcare which led
to the AEs. This contrasts with our previous report,1 which focused on
the patient characteristics associated with AEs and the nature and
consequences of the AEs.
|
| |
Methods |
The method of determining AEs in the QAHCS has been described
previously.1 The AEs were re-examined
with the specific goals of determining the causes for, or the
underlying errors leading to, each AE. In addition, strategies that
were judged to have the potential to prevent AEs were recorded.
To obtain this information the first and subsequent review forms (RF1
and RF2 forms1) collected during the QAHCS
were re-examined. The source material for these forms had been the
hospital medical records, but neither the hospitals nor the medical
records were revisited in this analysis.
Categories for the causes of the AEs were devised by an iterative
process during a three-day workshop. For this, we sought additional
expertise in clinical epidemiology and qualitative research
methods. Using these categories, the AEs recorded on the review forms
were assessed by three of the senior medical specialists who had
originally reviewed the medical records in the QAHCS.
All the material from each AE was reviewed by only one reviewer, as the
agreement between the medical reviewers in determining the presence
or absence of an AE during the QAHCS was 80% (kappa, 0.55). A proforma was
completed which asked the reviewer to identify the error and then
classify it by human cause and preventive strategy. All AEs were also
categorised into some of the processes of clinical care. Results for
the "delay", "treatment" and "investigation" categories are
presented. The categories were not mutually exclusive. These data
were then entered into a database, merged with the original data from
the QAHCS for each case and analysed. Two of the original total of 2353
AEs were missed in this review; thus, results are given for 2351 AEs.
Our analysis provides the frequency of occurrence of each of the
categories of causes of AEs, together with the proportion in each
category resulting in permanent disability (including death) and
the proportion with high preventability.
|
| |
Results |
Human error categories
Box 2 shows the frequency of occurrence of each of the human error
categories, and the proportion of the AEs in each category judged to
have permanent disability and high preventability. Of the 2351 AEs,
1922 (81.8%) were associated with one or more human error categories.
As the error categories were not mutually exclusive, the 1922 AEs were
associated with 2940 causes. "Complication of, or failure in, the
technical performance of an indicated procedure/operation"
was the most frequent cause of AEs; examples of this category are shown
in Box 3A.
Human errors associated with categories of failure of cognitive
function were the next most frequent cause of AEs (Box 2). These
included "Failure to synthesise, decide and/or act on available
information", "Failure to request or arrange
investigation, procedure or consultation", and
"Misapplication of, or failure to apply, a rule; or use of a bad or
inadequate rule".
The most frequent error category, "complication of, or failure
in, the technical performance of an indicated
procedure/operation", had a lower proportion of AEs with
permanent disability (14.2%). The next five most frequent human
error categories all had a high proportion of AEs with permanent
disability (25% or more) (Box 2). This pattern was also seen in the
proportions of AEs with death as the outcome: 2.2% in the first
category, and 8% or more in each of the next five categories.
Of the 1201 AEs having high preventability, 9 (0.7%) were not
associated with a human error category; for the remaining 1192 AEs,
2051 causes were identified (Box 2).
Delay categories
The importance of timeliness to the quality of healthcare led to
further analysis of all AEs to ascertain the nature and role of delay in
their causation (Box 4A).
Delays contributed to 20.0% of AEs: of these, delays in diagnosis
accounted for 56.8% and treatment delays for 40.6%. Diagnostic delay
was usually the failure to make, or attempt to make, a diagnosis of a
patient's condition rather than just providing symptomatic or even
no treatment. Treatment delay was when the diagnosis had been made but
there was a delay in initiating specific therapy. Examples of AEs in
the delay category are included in Box 3B.
The AEs with delay categories were judged to have very high
preventability (86%-90%) compared with the average (51.2%) for all
AEs (Box 4A).
Treatment categories
AEs categorised as caused by a treatment error were also analysed (Box
4B). In 19.6% of all AEs, treatment error contributed to the cause. The
majority of AEs in this group fell into the categories of "no or
inadequate treatment" (51.5%), or "wrong or inappropriate
treatment" (27.4%). As with AEs caused by delay, these AEs were
judged to have much higher preventability than the average for all
AEs. Examples of AEs involving treatment errors are shown in Box 3C.
Investigation categories
Analysis of the AEs caused by patient investigation issues is shown in
Box 4C, and examples are given in Box 3D. There was a problem with
clinical investigation in 10.7% of AEs. Paralleling the results in
the treatment category, most (78.6%) of these AEs were in this
category because an investigation was not done, rather than the
investigation being inappropriate (3.6%), or not acted upon
(15.5%). Consistent with other AEs that are attributed to cognitive
failure, there was a very high percentage of these AEs rated as high
preventability.
Strategies for preventing AEs
When describing AEs, preventability refers to the
identification of an avoidable error that led to the adverse event.
This is not to say that the error could be avoided on every occasion, and
that the adverse event would not occur. Rather, it implies that, with
the current state of knowledge and technology, it is possible to
identify and avoid that particular error, and hence reduce the
probability of an AE. The reviewers were making a judgement, having
identified the error, on the particular strategy for a change in the
healthcare system that could have prevented the AE. The outcomes of
these judgements are given in Box 5.
Nineteen (1.6%) of the 1201 high preventability AEs did not have a
prevention strategy category. Of the 2613 prevention strategies
identified in the 1182 AEs with high preventability, 24.7% (646) were
for "better education and training", 20.9% (545) were for
"new or better implemented policies or protocols" and 18.6%
(486) were for "more or better formal quality monitoring or
assurance processes".
|
| |
Discussion |
AEs are important to patients, healthcare providers and to the
custodians and funders of health services. One estimate of the
national cost to the Australian healthcare system of just the
additional hospital bed-days (as a result of the AEs identified in
19921) is in excess of $800 million
dollars per year.4 This estimate ignores any
subsequent hospital admissions and out-of-hospital healthcare
expenses, loss of productivity of the patients involved, and long
term community costs of permanent disability from AEs. It also
ignores the benefits received from healthcare.
Providing insights into how AEs occur can help in developing
prevention strategies to reduce the frequency and severity of
patient injuries during healthcare. Our review and analysis of the AE
data from the QAHCS have shown that the causes of AEs or errors leading
to AEs can be characterised, and that human error is a prominent cause.
It is important to recognise that human error is inevitable for even
the best-trained and best-qualified healthcare providers. Weed has
recently pointed out that the unaided human mind is incapable of
performing consistently at the necessary level to provide optimal
healthcare.5 However, other
studies6 have noted that the label
"human error" is prejudicial and non-specific; it may retard rather
than advance our understanding of how complex systems fail. It is
postulated that within complex systems error is a symptom of
organisational problems, and this is likely to apply to healthcare.
Therefore, we need a healthcare-system response to error that moves
the system towards being as "failsafe" as possible rather than one
that blames the clinician who may have erred. Examples from the more
frequently studied area of adverse drug events7 would be
decision-support technology for antibiotic
prescribing,8 with its demonstrated
benefits, and electronic prescribing to reduce prescribing and
transcription errors in hospital.9
Our analysis identified broad functional categories that are linked
to the processes that make up the system of healthcare delivery and
hence cut across specialties, diagnosis-related groups (DRGs) and
particular patient groups. The sample size is large enough to provide
useful information even when several AEs could not be classified into
the categories chosen, or insufficient information was available to
indicate cause. On the other hand, several factors bias the
information available for assessing AEs because of an emphasis on
procedures and short term outcomes and possible under-reporting of
the contribution of the supporting systems to the cause of the AEs.
Firstly, because the original data source was the hospital medical
record, the information available about AEs is biased towards the
patient involved and away from other potentially important
contextual events at the time. Further, the medical record often
focuses more on the actions of clinicians involved in direct or
procedural patient intervention, and less on the actions of other
staff or systems with a more supportive role. These and other factors
will lead to an emphasis on procedures and short term outcomes, and a
possible under-reporting of the contribution of supporting systems
in causing AEs. Finally, information about subsequent or prior
hospitalisations is usually only available if the patient attended
the same hospital on all occasions.
Having acknowledged these potential limitations, cognitive
failure (Box 2) appears to have a role in 57% of all the causes of AEs, and
most of the AEs involved were judged to be of high preventability and to
have caused significant disability. These AEs were largely
associated with errors of omission rather than commission. Does this
represent a minimum "obligatory" error rate resulting from a
combination of human error and our healthcare system, and hence which
cannot be improved? Our data are not able to answer this question
unequivocally, but we believe they show sufficient opportunities
for moving the system towards a failsafe mode to suggest that the
answer is no. Until recently there has been an under-recognition of
the role and responsibilities of the healthcare system and its
custodians in providing a "safe environment" using
systems-improvement tools.10
One response to these data should be to look at the factors in
healthcare delivery that may interfere with the cognitive or
technical performance of healthcare providers. Insufficient use of
information technology to assemble the necessary information at the
time of decision-making may increase error. Another important
factor is fatigue, which has already been shown to increase error in
doctors.11 Sleep deprivation may
have a much more significant role in human error in healthcare than the
current work-load patterns pay heed to, but more research is needed.
Other factors that may be important include the level of supervision
provided to junior staff, and the pervasive effect of the culture of
medical practice, which can unhelpfully portray error as individual
failure or deviation from perfection.12 Our study method does not
provide direct information about the role of these factors.
The high proportion of causes of AEs involving cognitive failure must
represent a manifestation of human error occurring in a system that is
not patient protective, if one accepts that these practitioners are
appropriately trained and competent by international standards.
Our study provides clear guidance on methods for improvement, with
"new, better, or better implemented policies or protocols"
accounting for 24% of prevention strategies identified for the
AEs, "quality monitoring and assurance processes"
accounting for 21%, and "better education and
training" for a further 19%.
In summary, improvement is needed in the agreed processes of care,
supported by information systems that allow general dissemination
of current knowledge of diseases or treatments, and information on
outcomes of care for each patient, through appropriate quality
processes. Simple examples are the availability of practice
guidelines and protocols at the point-of-care, and the use of
automated reminders for patients and practitioners when a
particular test or follow-up is required. In addition, having
adequate patient "outcome" information in a form that can be
benchmarked is a powerful tool in identifying unacceptable
variation.
|
Acknowledgements | |
We acknowledge the contributions of Professor B Armstrong,
Professor W R Runciman, Professor R Holland, Dr T Robertson and Dr A
Hobbes.
|
| |
References |
- Wilson RMcL, Runciman WB, Gibberd RW, et al. The Quality in
Australian Health Care Study. Med J Aust 1995; 163: 458-471. <eMJA pdf>
-
Brennan TA, Leape LL, Laird N, et al. Incidence of adverse events and
negligence in hospitalised patients: results of the Harvard Medical
Practice Study I. N Engl J Med 1991; 324: 377-384.
-
Andrews LB, Stocking C, Krizek T, et al. An alternative strategy for
studying adverse events in medical care. Lancet 1997; 349:
309-313.
-
The Final Report of the Taskforce on Quality in Australian Health
Care. Appendix 7. Canberra: AGPS, June 1996.
<http://www.health.gov.au/pubs/hlthcare/toc.htm>
-
Weed LL. New connections between medical knowledge and patient
care. BMJ 1997; 315: 231-235.
-
Cook RI, Woods DD. Operating at the sharp end: the complexity of
human error. Human performance in anaesthesia: a corpus of cases.
Report to the Anaesthesia Patient Safety Foundation, 1991.
Columbus, Ohio: The Ohio State University: 255-307.
-
Classen DC, Pestonick SL, Evans RS, et al. Adverse drug events in
hospitalised patients: excess length of stay, extra costs and
attributable mortality. JAMA 1997; 227: 301-306.
-
Evans RS, Pestonick SL, Classen DC, et al. A computer-assisted
management program for antibiotics and other anti-infective
agents. N Engl J Med 1997; 338: 231-238.
-
Bates DW, Boyle DL, Vander Vliet MB, et al. Relationship between
medication errors and adverse drug events. J Gen Intern Med
1995; 10: 199-205.
-
Leape LL. A systems analysis approach to medical error. J Eval
Clin Pract 1997; 3: 213-222.
-
Nocera A, Khursandi DS. Doctors' working hours: can the
profession afford to let the courts decide what is reasonable. Med
J Aust 1998; 168: 616-618.
-
Leape LL. Error in medicine. JAMA 1994; 272: 1851-1857.
(Received 4 May 1998, accepted 20 Jan 1999)
|
| | Authors' details |
Royal North Shore Hospital, Sydney, NSW 2065.
Ross McL Wilson, MB BS, FRACP, Senior Specialist in Intensive
Care; Director of QARNS (Quality Assurance Royal North Shore);
Bernadette T Harrison, RN RM, Manager QARNS.
University of Newcastle, Newcastle, NSW 2308.
Robert W Gibberd, PhD, Associate Professor, Department of
Statistics; and Director of Health Services Research Group.
John D Hamilton, MB BS, FRCP, Professor of Medicine, Faculty
of Medicine and Health Sciences.
Reprints: Dr R McL Wilson, Director of QARNS, Royal North
Shore Hospital, Pacific Highway, St Leonards, NSW 2065.
Email: rwilsonATdoh.health.nsw.gov.au
| |
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au>".
<URL: http://www.mja.com.au/>
|
| | | 1: Terms and definitions
Adverse event (AE): An AE was defined as an injury or complication which resulted in disability or prolongation of hospital stay and was caused by the healthcare received rather than by the disease from which the patient suffered. The AE either occurred during the hospital admission, or during an earlier contact with healthcare services, and was responsible for all or part of the hospital admission.
Error: An act of commission or omission that caused, or contributed to the cause of, the unintended injury.
- for errors of commission this will usually be the immediate morbid consequences of the error
- for errors of omission this will usually be the continuation of, and consequences of, an existing morbid state that could have been cut short, or had a better outcome, if the error had not occurred.
Prevention strategy: Changes in the system in which an error occurred that may- reduce the probability of the error occurring
- increase the probability that the error would be remedied before an unintentional injury occurred
Preventability: Preventability of an AE was assessed by the detection of "an error in management due to the failure to follow accepted practice at an individual or system level"; accepted practice was taken to be "the current level of expected performance for the average practitioner or system that manages the condition in question".
|
|
| | Back to text | | 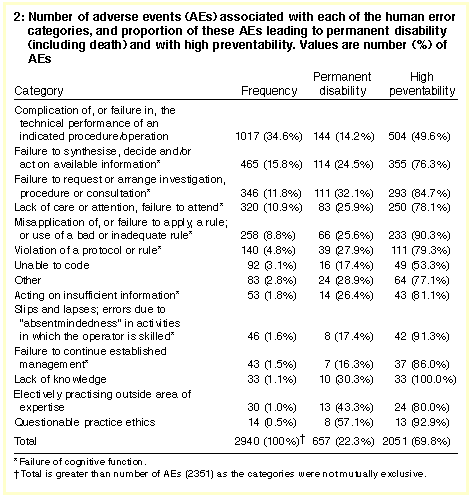 | | Back to text | |
|
3. Examples of categories of causes of adverse events and preventability scores | A. Human error categories
Example 1: A 50-year-old man sustained a bowel perforation from colonoscopy for investigation of abdominal pain. Laparotomy required.
Category: "Technical performance".
Preventability score: 3.
Example 2: A 71-year-old man required six operations for femoral hernia repair.
Category: "Technical performance".
Preventability score: 2.
Example 3: A 32-year-old woman had persisting severe back pain after two laminectomies, three myelograms, one decompression/fusion, and three thecal/epidural injections over 18 months. In pelvic traction at the time of review.
Category: "Technical performance".
Preventability score: 4.
Example 4: A failed attempt at percutaneous endoscopic gastrostomy on a 32-year-old woman was followed by an open procedure. The patient died 9 days later. Autopsy revealed acute peritonitis, subphrenic abscess and bilateral pneumonia. There did not appear to have been an antemortem diagnosis of intra-abdominal sepsis, or any specific treatment for it.
Category: "Technical performance".
Preventability score: 6.
B. Delay in diagnosis and/or treatment categories
Example 1: Diagnosis of cancer of the colon was delayed until the patient, a 62-year-old woman, presented with a ruptured caecum and peritonitis from an obstructing tumour. In hospital 3 months earlier with a history suggestive of cancer of the colon and iron-deficiency anaemia, but no investigation performed.
Categories: Diagnosis delay, violation of protocol or rule; failure to synthesise, decide or act on available information; lack of care/attention.
Preventability score: 5.5.
Example 2: A 28-year-old man with abdominal pain was treated with cholecystectomy. Gallbladder was macroscopically and histologically normal. Small bowel lymphoma was eventually diagnosed and treated, with resolution of the presenting symptoms.
Categories: Diagnosis delay; failure to synthesise, decide or act on available information; failure to request or arrange an investigation, procedure or consultation.
Preventability score: 5.
C. Treatment categories
Example 1: A 52-year-old man with known asthma was prescribed a beta-blocker for hypertension. This resulted in acute respiratory failure leading to artifical ventilation and tracheostomy.
Categories: Wrong or inappropriate treatment; misapplication of or failure to apply a rule; failure to synthesise, decide or act on information.
Preventability score: 6.
Example 2: A 54-year-old man developed gastrointestinal bleeding (haemoglobin level, 45 g/L) while receiving non-steroidal anti-inflammatory drugs and steroids for rheumatoid arthritis. This required hospital admission and blood transfusion, at which time the correct diagnosis of osteoarthritis was made.
Categories: Wrong or inappropriate treatment; acting on insufficient information; failure to request or arrange an investigation, procedure or consultation.
Preventability score: 5.5.
Example 3: Hospitalisation and surgical intervention
for septic arthritis that followed steroid injection into a joint.
Categories: Unclassified treatment; technical; lack of care/attention.
Preventability score: 4.5.
D. Investigation categories
Example 1: A 75-year-old woman died from acute renal failure after developing gentamicin toxicity. Gentamicin was used to treat an infected pleural effusion, and drug levels were not measured.
Categories: Investigation not performed; failure to request or arrange an investigation, procedure or consultation; lack of care/attention.
Preventability score: 5.
Example 2: A 58-year-old woman had recurrent hospital admissions for chest pain and impaired cardiac function without specific investigation, and hence a reduction in treatment options.
Categories: Investigation; violation of protocol or rule; failure to synthesise, decide and/or act on available information.
Preventability score: 5.
|
|
| | Back to text | | |
4: Contribution of delay, treatment and investigation categories to adverse events (AEs). Values are number (%) of AEs | | | Permanent | High | | A. Delay category | Frequency | disability | preventability |
| | Diagnostic delay | 267 (56.8%) | 93 (34.8%) | 231 (86.5%) | | Treatment delay | 191 (40.6%) | 53 (27.7%) | 172 (90.1%) | | Administrative | | delay | 12 (2.6%) | 3 (25.0%) | 11 (91.7%) | | Total | 470 (100%) | 149 (31.7%) | 414 (87.9%) | | | | B. Treatment category |
| | No or inadequate | | treatment | 237 (51.5%) | 72 (30.4%) | 176 (74.3%) | | Wrong/inappropriate | | treatment | 126 (27.4%) | 35 (27.8%) | 96 (76.2%) | | No or inadequate | | prophylaxis | 41 (8.9%) | 9 (22.0%) | 34 (82.9%) | | Treatment | | unclassified | 36 (7.8%) | 7 (19.4%) | 28 (77.8%) | | Missed treatment | 20 (4.4%) | 4 (20.0%) | 16 (80.0%) | | Total | 460 (100%) | 127 (27.6%) | 350 (76.1%) | | | | C. Investigation category |
| | Investigation | | not performed | 198 (78.6%) | 81 (40.9%) | 171 (86.4%) | | Investigation | | not acted on | 39 (15.5%) | 13 (33.3%) | 36 (92.3%) | | Investigation | | inappropriate | 9 (3.6%) | 2 (22.2%) | 9 (100.0%) | | Investigation | | unclassified | 6 (2.4%) | 2 (33.3%) | 5 (83.3%) | | Total | 252 (100%) | 98 (38.9%) | 221 (87.7%) |
|
| | Back to text | | |
5: Frequency of occurrence of categories of prevention strategies and the proportion of adverse events (AEs) judged as causing permanent disability or having high preventability. Values are number (%) of AEs | | | Permanent | High | | Category | Frequency | disability | preventability |
| | New, better, or better implemented | | policies or protocols | 884 (23.7%) | 206 (23.3%) | 545 (61.7%) | | More or better formal quality monitoring | | or assurance processes | 790 (21.2%) | 186 (23.5%) | 486 (61.5%) | | Better education and training | 715 (19.2%) | 160 (22.4%) | 646 (90.3%) | | Consultation with other specialists | | or peers | 391 (10.5%) | 133 (34.0%) | 294 (75.2%) | | Don't know | 341 (9.2%) | 51 (15.0%) | 186 (54.5%) | | Better access to, or transfer of, information | 135 (3.6%) | 40 (29.6%) | 100 (74.1%) | | Discharge procedures and protocols | 122 (3.3%) | 27 (22.1%) | 100 (82.0%) | | Other | 89 (2.4%) | 22 (24.7%) | 46 (51.7%) | | Changes in organisation management | 88 (2.4%) | 22 (25.0%) | 75 (85.2%) | | Changes in organisation culture | 77 (2.1%) | 26 (33.8%) | 66 (85.7%) | | More or better personnel | 72 (1.9%) | 29 (40.3%) | 53 (73.6%) | | More or better equipment or other | | physical resources | 22 (0.6%) | 8 (36.4%) | 16 (72.7%) | | Total | 3726 (100%)* | 910 (24.4%) | 2613 (70.1%) |
| |
* Total is greater than the number of AEs (2351) as the categories were not mutually exclusive. |
|
| | Back to text |
|





