|
Research Australian general practitioners' views and use of colorectal cancer screening tests Michael J Sladden and Jeanette E Ward
MJA 1999; 170: 110-113
Abstract -
Introduction -
Method -
Results -
Discussion -
Acknowledgements -
References -
Author's details
- - More articles on Gastroenterology | |||
| Abstract |
Objectives: To determine general practitioners'
(GPs) current beliefs, knowledge and self-reported practices of
screening for colorectal cancer. Design and setting: Postal survey of national random sample of 1271 GPs in 1996. Outcome measures: GP views on effectiveness of faecal occult blood testing (FOBT) and flexible sigmoidoscopy in reducing premature death from colorectal cancer in "average-risk" patients (asymptomatic with no family history); views on frequency of tests and target group; use of these tests; and independent predictors of views and use. Results: Response rate was 67%. FOBT and flexible sigmoidoscopy were said to be effective as screening tests by 38% and 61% of GPs, respectively, but 30% and 25% were unsure. Independent predictors of belief in screening effectiveness were State of practice (for FOBT), male sex and awareness of Gut Foundation guidelines (for flexible sigmoidoscopy) and increasing age (for both). Most often chosen screening frequencies were every year for FOBT (29%), and five-yearly for flexible sigmoidoscopy (24%), although 19% and 26%, respectively, were unsure of the appropriate screening interval. Most often cited target group was people aged over 40 years with first-degree relatives with colorectal cancer: 63% of GPs would offer FOBT and 74%, flexible sigmoidoscopy. Fewer than 3% of GPs were likely to adopt an opportunistic approach to screening, yet 15% would be highly likely to recommend FOBT during a dedicated health check-up for a 58-year-old male patient, and 9% for a female patient. Conclusion: The absence to date of a coherent national policy on colorectal cancer screening is associated with wide variations in views and practice that are inconsistent with the available evidence. If GPs are to be involved in implementing population screening, national policy must be widely and effectively promulgated.
| ||
| Introduction |
The past decade has seen a saga of unfinished policy initiatives on
screening for colorectal cancer in Australia. As early as 1990,
screening by faecal occult blood test (FOBT) was being promoted for
people with "average risk" of colorectal cancer, in the absence of
convincing evidence or national policy.1 Since then, a range of bodies
have produced guidelines with quite different recommendations,
particularly for this "average risk" group.2-8 Examples are shown in Box
1.
More recent among these was the 1997 report of the Australian Health Technology Advisory Committee (AHTAC) Working Party on Colorectal Cancer Screening. This working party was formed after a 1994 call for a national symposium to develop "recommendations about early detection of colorectal cancer" as part of Australia's national health goals and targets,9 and a 1995 deputation to the Commonwealth from the Australian Cancer Network. The Network recommended pilot projects of screening and, if these were successful, implementation of national screening. AHTAC found that FOBT was effective in reducing mortality from colorectal cancer in the average-risk population (defined as the "well population aged over 50") and recommended studies to determine the effectiveness of different screening strategies, particularly how best to involve general practitioners (GPs). Meanwhile, in 1998, another set of draft guidelines, not yet nationally endorsed, was circulated by the Clinical Oncological Society of Australia and the Australian Cancer Network.8 Despite the unresolved status of national policy, research has continued to involve Australian GPs overtly or covertly in colorectal cancer screening.10-14 Most recently, a survey of Perth GPs reported high uptake of this screening.15 As no national studies have been conducted, we designed a postal survey to assess GPs' perceptions of the effectiveness of screening for colorectal cancer and self-reported levels of screening. | ||
Method | |||
| A covering letter, questionnaire and reply-paid envelope were mailed in May 1996 to a national random sample of 1271 GPs, as described elsewhere.16 Standardised response-aiding strategies were used to follow up non-respondents.16 | |||
| Questionnaire | |||
Questions on colorectal cancer screening were part of a larger
questionnaire on current status of cancer screening in general
practice. Respondents were asked to tick the response that matched
their views on:
| |||
| Data analysis |
Descriptive, cross-tabulation and logistic regression analyses
were performed with SPSS for Windows 7.17 Logistic regression
analyses were performed to determine independent predictors of
knowledge and practice outcomes. Fourteen potential predictors
were considered: GP's sex; age; State; full- or part-time practice;
practice type (solo or group); membership of a Division of General
Practice; Royal Australian College of General Practitioners
(RACGP) affiliation; membership of the Australian Medical
Association; personal history of cancer; family history of cancer;
awareness of RACGP guidelines; Australian Gastroenterology
Institute/Australian Cancer Society guidelines; and Gut
Foundation of Australia (GFA) guidelines; and practice location
(metropolitan or other18). All independent
variables were included in the full model. A further variable --
belief that FOBT/flexible sigmoidoscopy is an effective screening
test -- was included in the model to predict behaviour. A backwards
stepwise modelling strategy was used to identify significant
independent variables, whereby all dependent variables were
initially included and non-significant terms were progressively
eliminated. Significance was assessed using the Wald chi-squared statistic.
| ||
| Results | We received 855 usable questionnaires from 1271 eligible GPs (67% response rate). The response rate for women (75%) was significantly higher than that for men (63%) (chi-squared = 15.4, 1 df, P < 0.001), but did not vary with age, vocational registration status, RACGP affiliation, or practice size and location. | ||
| GP views about screening | |||
|
GP views about the effectiveness of screening for colorectal cancer
in preventing premature deaths are shown in Box 2. More GPs believed
flexible sigmoidoscopy to be effective (61%) than believed FOBT to be
effective (38%), but there was substantial uncertainty about both
screening tests, with 25% and 30% of GPs unsure. Independent
predictors of believing either test to be effective are summarised in Figure 1. For FOBT, these comprised
increasing GP age and State of practice (specifically, South
Australia). For flexible sigmoidoscopy, they comprised increasing
GP age, male sex, and awareness of the Gut Foundation guidelines
(which favour screening).
GPs' views on appropriate screening frequencies and target groups are shown in Box 2. Most often chosen frequencies were every year for FOBT (29%), and five-yearly for flexible sigmoidoscopy (24%). However, 19% and 26%, respectively, were unsure of the appropriate screening interval. The most often cited target group was people aged over 40 years with first-degree relatives with colorectal cancer: 63% of GPs would offer FOBT and 74%, flexible sigmoidoscopy. | |||
| Self-reported practice | |||
|
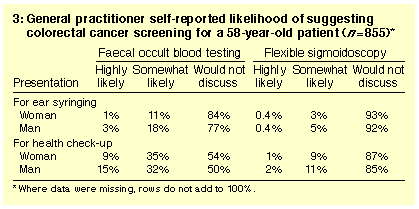
Likelihood of suggesting colorectal cancer screening is shown in Box 3. Fewer than 3% of GPs were "highly likely" to adopt an opportunistic
approach to colorectal cancer screening for a 58-year-old patient
(by either test) or to recommend flexible sigmoidoscopy screening
during a dedicated health check-up. More would be "highly likely" to
recommend FOBT during a dedicated health check -- 15% if the patient
was a man and 9% if a woman. This sex difference was significant
(McNemar's chi-squared = 43.7, 1 df,
P < 0.0001). Independent predictors of being "highly
likely" to include FOBT in a health check-up are shown in Figure 2. They comprised increasing GP age,
State of practice, and belief in the effectiveness of the tests.
Usefulness ratings of guidelines available at the time of the survey are shown in Box 4. While RACGP, AGI/ACS and GFA guidelines were rated as "very" or "somewhat" useful by 33%, 50% and 45% of respondents, respectively, they were unable to be recalled by 52%, 35% and 41%.
| |||
| Discussion |
Our study suggests considerable confusion about colorectal cancer
screening at the "front line" of general practice. About a third of
respondents believed that FOBT was an effective screening test in
average-risk individuals, while two-thirds believed this of
flexible sigmoidoscopy. These beliefs are inconsistent with the
evidence available at the time of our study: level II (randomised
controlled trial) evidence19 that FOBT reduced
colorectal cancer mortality, but only level III (case-control
study) evidence20 supporting flexible
sigmoidoscopy. A wide range of responses were given about
appropriate screening frequency. This is not surprising, as the
three guidelines available at the time offered different and
contradictory advice, and none met the criteria for being
systematically evidence-based. Further confusion is likely if yet
more guidelines8 are published that
contradict the evidence-based AHTAC guidelines.7 Far fewer GPs reported using the screening tests than reported they were effective; most respondents did not use the tests. This discordance was greater for sigmoidoscopy than for FOBT. Again, it is likely that the lack of clarity and the variation between guidelines, as well as availability of conflicting information and educational material, have caused uncertainty among GPs, with concomitant inconsistency in their behaviour. Perhaps FOBT is used more often than sigmoidoscopy because it is easier to arrange. Increasing GP age and physician belief in screening effectiveness independently predicted self-reported provision of screening. South Australian GPs were more likely to advocate screening, perhaps because of research studies and community-based initiatives in that State.10 GPs also favoured screening men rather than women for colorectal cancer. Sex bias not been reported previously in colorectal cancer screening, and may reflect the higher incidence of colorectal cancer among men.21 Alternatively, perhaps GPs place a lower priority on colorectal cancer screening in women, for whom cervical and breast cancer screening are widely performed, but a higher priority in men, for whom there is, as yet, no "male cancer" screening of proven benefit. National levels of self-reported use of screening tests were less than previously reported,15,22,23 although the higher levels in South Australia were consistent with earlier data.10 GPs' wider endorsement of screening for "above-average-risk" individuals with first-degree relatives with colorectal cancer (63%-74%) was similar to the levels found in recent studies (80%-94% GP support),10,15 but considerably higher than in a similar 1982 study (23% GP support).22 Screening of relatives is apparently becoming more acceptable. Usefulness and recall of guidelines was low, similar to other recent findings.15 Our results suggest an urgent need for a national colorectal cancer screening policy. As GPs remain the most respected source of health information,24 it is vital they have access to timely and accurate information. The AHTAC report, released in 1998, was necessary but insufficient. If GPs are to be involved in implementation of colorectal cancer population screening (which, by definition, will target average-risk individuals), strategies are needed to inform them of the importance of screening and to facilitate appropriate changes in behaviour. When there has been a concerted effort to communicate agreed policy to Australian GPs (eg, about mammographic screening), uniformity of GP views has been achieved.25 However, when evidence is lacking (eg, for clinical breast examination),25 or State-based initiatives are patchy,26 it appears that GPs differ considerably in their views of screening effectiveness and self-reported behaviour. Our study concentrated on screening average-risk individuals, for which previous guidelines have been confusing, non-evidence based and at variance with each other. Most guidelines distinguish between screening for average-risk and above-average-risk individuals, generally recommending colonoscopic screening for above-average-risk groups (eg, those with familial adenomatous polyposis and hereditary non-polyposis colorectal cancer). Clearly, strategies for effective evidence-based screening of above-average-risk groups must also be promoted. Thus, our results reveal our failings to date as an organised healthcare system to provide GPs with timely, consistent and evidence-based health policy, as they and their patients deserve. Our study provides a baseline against which the effectiveness of future dissemination of colorectal cancer screening policy may be measured. | ||
| Acknowledgements |
A Commonwealth General Practice Evaluation Program seeding
grant funded this study. We thank the GPs who participated in our
research with no financial incentive, Phoebe Holt for contributing
to questionnaire design, and Tracey Bruce for diligent survey
administration. The study was approved by the Ethics Committee of the
Royal Prince Alfred Hospital, Sydney, NSW.
| ||
| References |
(Received 25 Jun, accepted 28 Oct, 1998)
| ||
| Author's details |
Division of Community and Rural Health, University of Tasmania, Hobart, TAS. Michael J Sladden,FRACGP, MAppEpid, Honorary Senior Lecturer.
Needs Assessment and Health Outcomes Unit, Central Sydney Area
Health Service, Sydney, NSW.
Reprints will not be available from the authors.
| ||
|
| |||
| Figure 1 : Independent predictors of general practitioners (GPs) reporting that faecal occult blood testing or flexible sigmoidoscopy is effective in reducing premature deaths from colorectal cancer. | |||
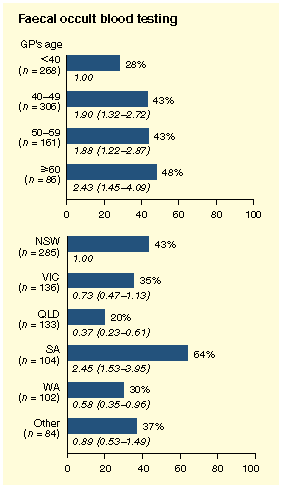 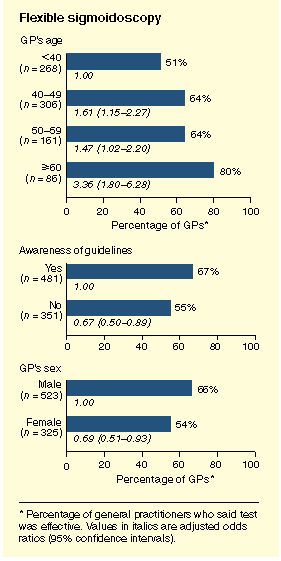 | |||
| Back to text
| |||
| Figure 2 : Independent predictors of general practioners (GPs) reporting they would be "highly likely" to discuss faecal occult blood testing during a deicated health check-up with a 58-year-old patient. (Adjusted odds ratios with 95% confidence intervals are available from the authors.) | |||
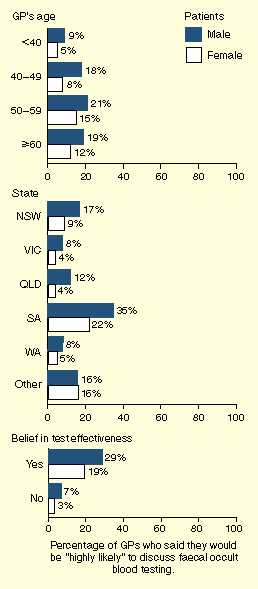 | |||
| Back to text
| |||
| |||
 | |||
| Back to text
| |||
 | |||
| Back to text
| |||
 | |||
| Back to text | |||
Received 25 May 2026, accepted 25 May 2026
- Michael J Sladden
- Jeanette E Ward




