|
Research
Health burden of hip and other fractures in Australia beyond 2000
Projections based on the Geelong Osteoporosis Study
Kerrie M Sanders, Geoffrey C Nicholson, Antony M Ugoni,
Julie A Pasco,
Ego Seeman, and Mark A Kotowicz
MJA 1999; 170: 467-470
For editorial comment, see Morris et al; see also Pocock et al.
Abstract -
Introduction -
Methods -
Results -
Discussion -
Acknowledgements -
References -
Author's Detials
-
-
More articles on Public and environmental health
|
| |
Abstract |
Objective: To calculate the expected increase in the
number of fractures in adults attributable to the predicted increase
in the number of elderly Australians.
Data sources: All fractures in adult residents (> 35
years) of the Barwon Statistical Division (total population, 218
000) were identified from radiological reports from February 1994 to
February 1996. The Australian Bureau of Statistics supplied
predictions of Australia's population (1996 to 2051).
Main outcome measure: The projected annual number of
fractures in Australian adults up to 2051 (based on stable rates of
fracture in each age group).
Results: The number of fractures per year is projected to
increase 25% from 1996 to 2006 (from 83 000 fractures to 104 000). Hip
fractures are projected to increase 36% (from 15 000 to 21 000) because
of a substantial rise in the number of elderly aged 85 years and over.
Hip fractures are expected to double by 2026 and increase fourfold by
2051.
Conclusions: In contrast to Europe and North America,
where numbers of hip fractures are expected to double by 2026 and then
stabilise, in Australia hip fractures will continue to place a
growing demand on healthcare resources for many decades. These
projections can be used for setting goals and evaluating the costs and
benefits of interventions in Australia.
|
| | Introduction |
Australia's population is ageing. Thus, diseases such as
osteoporosis are affecting a greater proportion of the population.
Cost-effective prevention and treatment of fractures will become
increasingly important, as the proportion of the "prime working"
population (aged 15 to 64 years) is expected to decrease by 7% between
1996 and 2051.1 Estimations of the annual
number of fractures will facilitate effective allocation of limited
healthcare resources.
Previously, fracture rates in Australia have been extrapolated from
rates in Dubbo and Busselton,2,3 populations that may not
be representative of the national population as they are both fairly
isolated towns with small numbers of men and women in the oldest age
groups. Lord et al investigated changes in hip fracture admissions in
New South Wales between 1979 and 1990 using International
Classification of Diseases hospital discharge codes.4 Although
frequently used for ascertaining hip fractures, the limitations of
this method are well documented.5,6
The Geelong Osteoporosis Study is a population-based study of age-,
sex- and site-specific fracture rate(s) within a well-defined
geographic region sufficiently large to establish reliable rates of
fracture. It is the largest Australian epidemiological study of
adult fractures, identifying 2184 fractures over two years in people
aged 35 years and over. Data from the 1996 national census confirm the
findings of an earlier study7 that the regional
population is typical of the nation in age distribution and
socioeconomic range.
The Australian Bureau of Statistics publishes projections of the
size, structure and distribution of Australia's population into the
next century.1 Assuming stable age- and
sex-specific rates of fracture, we have projected annual numbers of
fractures by anatomical site in adults over the next 50 years.
|
| |
Methods |
| |
Population |
The Barwon Statistical Division is a region of southern
Victoria7 defined by the Australian
Bureau of Statistics which includes urban, semi-urban and rural
residents and has a population of 218 000 (109 923 aged 35 years and
over).
| |
Fracture ascertainment | |
Using radiological reports from the two medical imaging practices in
the region, we identified all fractures in adults (aged 35 years and
over) residing within the Barwon Statistical Division over the
two-year ascertainment period (17 February 1994 to 16 February
1996). Fractures were identified by a weekly computerised keyword
search of all radiological reports. Although radiological services
are available at several sites throughout the region, these sites are
under the auspices of two medical imaging practices.
Only reports of definite fractures were included as "cases". Reports
referring to "likely" or "possible" fracture were not included
unless radiologically confirmed at a later date. Vertebral
fractures were included in the study on the basis of the radiological
report, provided there was no previous record of a fracture at that
level. The initial x-ray demonstrating each fracture was sought and
the date of fracture was the date of the radiological diagnosis.
As the region is well provided with medical facilities, few fractures
would not have been assessed or followed up by services within the
region. The standing orders for the ambulance service are to
transport patients from residences within the study region to The
Geelong Hospital. The study was well advertised and adults who may
have sustained fracture(s) while outside the region were asked to
contact study coordinators.
Non-residents and patients with pathological fractures
(metastatic cancer, Paget's disease and multiple myeloma) were
excluded. We have previously reported that the exclusion of high
trauma fractures may underestimate the prevalence of
bone-fragility fractures in the community,8 so we did not exclude
fractures on the basis of trauma classification.
The method of fracture ascertainment has been previously
described9 and validated, using hip
fracture as a model.10
The study was approved by The Geelong Hospital
Human Research and Ethics Advisory Committee.
| |
Projections |
We calculated the predicted number of fractures in each five-year age
group for men and women as:
|
Predicted number of fractures
= |
Number of fractures in the study region
Study region population
|
X Projected Australian population
X 0.5 (2 year ascertainment)
The study region population was determined from the 1996 Australian
Bureau of Statistics census. Annual population projections were
also provided by the Australian Bureau of Statistics.1 This method of
projection assumes that the fracture rate in each age group will
remain unchanged over time.
Confidence intervals around the projections were calculated by the
bootstrap method.11 |
| |
Results |
The number of fractures identified in the study population is shown in
Table 1.
| |
Projections for all fractures | |
During the ascertainment period, 2184 adults sustained fractures,
producing an age- and sex-adjusted incidence of 102 per 10 000
person-years.
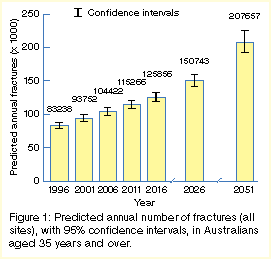
In 1996, we estimate that about 83 000 Australians aged 35 years and
over sustained fractures. We predict that by 2006 the total number of
fractures per year will increase by 25%, to 104 000 (Figure 1).
| |
Projections for hip fractures | |
Over the two-year ascertainment period, 428 people sustained hip
fractures, producing an age- and sex-adjusted incidence in people
aged 35 years and over of 17.2. The number of hip fractures in Australian
women is projected to increase from 11 300 per year in 1996 to 44 700 in
2051. In men, the number is projected to rise from 4 000 to 15 300. Figure 2 shows the projection for all people
aged 35 years or over.
The number of Australians sustaining hip fractures each year is
projected to increase by 15% every five years until 2036, then by about
10% every five years until 2051. A fourfold increase in hip fractures
is expected by 2051, when about 23% of Australia's projected
population will be aged 65 years and over (compared with 12% in 1996)
and over 8% of the population will be aged 85 years and over (compared
with 2% in 1996).
Hip fractures are likely to increase more than fractures at other
sites because the greatest population growth is expected in the
oldest age groups, where the hip is the most common site of
fracture.9 | |
Projections for fractures at sites other than the hip | |
During the ascertainment period, 1756 adults aged 35 years and over
sustained fractures at sites other than the hip, producing an age- and
sex-adjusted incidence of 77 per 10 000 person-years.
We estimate that in 1996 about 68 000 Australians aged 35 years and over
sustained fractures at sites other than the hip, and that the number of
non-hip fractures is likely to increase by 9% every five years until
2036, and then by 4% every five years until 2051 (to 147 645 non-hip
fractures per year).
Projections for vertebral, Colles, humeral and pelvic fractures
(the most common sites of fracture after the hip) are shown in Figure 3. Fractures at these sites are likely
to increase more than fractures at other sites where fracture rates do
not increase substantially with age.9 Population projections
suggest that vertebral, humeral and pelvic fractures will increase
by 12% every five years to 2036, then by 6% every five years to 2051.
Colles fracture rates increase with age in women, but not in
men,8
and the overall number of adults sustaining a Colles fracture will
increase by 10% every five years until 2036, then by 5% every five years
until 2051.
Fractures other than hip, vertebral, Colles, humeral and pelvic
fractures are predicted to increase at about half the rate predicted
for these sites (6% every five years until 2036, then 3% every five
years until 2051).
| |
Projection of fracture numbers by age group | |
The number of fractures in adults aged 35 to 59 years is not predicted to
change substantially over the projection period, as only a small
population increase in this age group is anticipated. By contrast,
among those aged 60 years and over, the number of fractures is
predicted to increase by at least 10% every five years, and by almost
20% every five years among those aged 85 years and over (Table 2).
Figure 4 shows the projected distribution of
hip fractures across age groups for selected years from 1996 to 2051.
|
| |
Discussion |
The ageing of the Australian population is increasing the demand for
health resources. Health expenditure per person aged 65 years and
over is nearly four times higher than for younger individuals ($4900 v
$1300).12 It is likely that hip fracture, which becomes increasingly common
with advancing age, contributes significantly to this higher
expenditure. Almost all people with a fractured hip are
hospitalised, with an average length of stay of 13 days.13 Studies in
other white populations suggest that 50% of patients who survive hip
fracture are discharged to nursing homes, and 25% remain
institutionalised one year later.14,15 Comparable
Australian data are not available, although the increased mortality
after hip fracture has been confirmed.16 We estimate that hip
fractures accounted for 0.9% of total government health services
expenditure for 1995/96.12 Based on the number of
Australian salary earners in 1998 (Australian Bureau of Statistics)
and an average cost of $16 000 per hip fracture,17 treatment alone costs
salary earners an average of $28 per year. In current dollar terms,
this may escalate to $120 per salary earner per year by 2051 if the
projected increase is realised.
The number of adults sustaining a hip fracture is likely to more than
double from 15 000 in 1996 to 34 000 in 2026, then almost double again by
2051. Fractures at other sites are expected to increase by 70% from
1996 to 2026, then by a further 26% to 2051. These rates of increase are
far above the expected growth in total healthcare costs due to the
ageing of the Australian population, which is estimated to be 4% every
five years for the next 30 to 40 years.18
For the number of hip fractures to remain stable, their incidence (per
10 000 population per year) would need to decline from 17.2 in
19969
to 15.6 in 2001, 14.3 in 2006 and 11.3 in 2026. In the United States, an
18% reduction in hip fracture rates between 1988 to 2000 has been
targeted by public health strategists.19 Current therapies (such
as hormone replacement therapy and bisphosphonates) may reduce
fracture rates by 50%, but their cost-effectiveness remains
controversial.20,21
In most white populations the number of hip fractures is predicted to
double between 1990 and 2025, and then plateau as the growth in the aged
population ceases.22 However, in contrast with
Europe and North America, the aged population and the number of hip
fractures in Australia and New Zealand are likely to continue to
increase from 2025 to 2050.22
Current trends suggest that almost three times as many women as men
will sustain a hip fracture (Table 1).
Largely for this reason, efforts to prevent hip fracture have focused
on osteoporosis in women. However, mortality and rate of
institutionalisation after hip fracture is higher in
men,23 and increasing hip
fracture rates among men, but not women, have been
reported.24,25
The projected increased longevity in men
suggests that osteoporosis will affect a growing number of
Australian men, yet there are no data concerning efficacy of any drug
treatment to prevent hip or vertebral fractures in men.26
Our projected number of vertebral fractures is likely to be an
underestimate because our ascertainment relied on clinical
indications for medical imaging. Between 50% and 75% of vertebral
fractures do not come to medical attention.27,28 However, our data are
likely to include some previously undiagnosed vertebral fractures
that occurred before the ascertainment period. Nevertheless, the
predicted number of vertebral fractures represents the number
likely to come to medical attention each year. Excluding vertebral
fractures does not alter the projected rate increase of all
fractures.
The validity of these projections is dependent upon reliable and
stable incidence rates and accurate population projections. The
major strength of our study was the comprehensive ascertainment of
all fractures among adult residents of a defined region
representative of Australia.9 A decline in hip fracture
rates has recently been reported,19 but other studies have
pointed to stable age-specific rates in women and younger men and
increasing rates in older men.24,25,29,30
These projections highlight the need to decrease fracture rates
among the elderly and can be used for setting goals and evaluating the
costs and benefits of interventions in Australia.
|
Acknowledgements | |
This study was supported by the Victorian Health Promotion
Foundation. We acknowledge the invaluable contributions of the
radiologists (D Barry, JM Cameron, PJ Carman, WP Holloway, V Mercuri,
PM Motterdam and DB Robertson) and staff at the Geelong Radiological
Clinic, as well as the radiologists (NJ Ferris, DO Lun, CB Styles) and
staff of the Medical Imaging Department at the Geelong and Colac
hospitals. We also wish to thank Biljana Skoric and Soheila Panahi.
|
| |
References |
- McLennan W. Projections of the populations of Australia, States
and Territories, 1995-2051. Canberra: Australian Bureau of
Statistics, 1996: 128. (Catalogue no. 3222.0.)
-
Jones G, Nguyen T, Sambrook PN, Kelly PJ, Gilbert C, Eisman JA.
Symptomatic fracture incidence in elderly men and women: The Dubbo
osteoporosis study (DOES). Osteoporos Int 1994; 4: 277-282.
-
Prince RL, Knuiman MW, Gulland L. Fracture prevalence in an
Australian population. Aust J Public Health 1993; 17:
124-128.
-
Lord SR. Hip fractures: changing patterns in hospital bed use in NSW
between 1979 and 1990. Aust N Z Surg 1993; 63: 352-355.
-
Bacon W, Maggi S, Looker A, et al. International comparison of hip
fracture rates in 1988-89. Osteoporos Int 1996; 6: 69-75.
-
Maggi S, Kelsey JL, Litvak J, Heyse SP. Incidence of hip fractures in
the elderly: a cross national analysis. Osteoporos Int 1991;
1: 232-241.
-
Ross KN. The development of the 1984 "Indicator of Disadvantage"
and its application to resource allocation decisions for the
"Disadvantaged Schools Program" in Australia. Geelong: School of
Education, Deakin University, 1984.
-
Sanders K, Pasco J, Ugoni A, et al. The exclusion of high trauma
fractures may underestimate the prevalence of bone fragility
fractures in the community: The Geelong Osteoporosis Study. J
Bone Mineral Res 1998; 13: 1337-1342.
-
Sanders K, Seeman E, Ugoni A, et al. The age- and gender-specific
rate of fractures in Australia: a population based study.
Osteoporos Int 1999. In press.
-
Pasco JA, Henry MJ, Gaudry TM, et al. Identification of incident
fractures: Geelong Osteoporosis Study. Aust N Z J Med 1999;
29: 203-206.
-
Efron B, Tibshirani R. The introduction to the bootstrap. New
York: Chapman & Hall, 1993.
-
Australia's health 1998: the sixth biennial health report of the
Australian Institute of Health and Welfare. Canberra: AGPS, 1998.
-
Abraham B, d'Espaignet E, Stevenson C. Australian health trends
1995. Canberra: Australian Institute of Health and Welfare, 1995.
-
Orwoll ES. The special problem of hip fracture. In: Favus MJ,
editor. Primer on the metabolic bone diseases and disorders of
mineral metabolism. 3rd ed. Philadelphia: Lippincott-Raven, 1996:
272-282.
-
Keene G, Parker M, Pryor G. Mortality and morbidity after hip
fractures. BMJ 1993; 307: 1248-1250.
-
Center J, Nguyen TV, Schneider D, et al. Mortality after all major
types of osteoporotic fracture in men and women: an observational
study. Lancet 1999; 353: 878-882.
-
Randell A, Sambrook P, Nguyen T, et al. Direct clinical and welfare
costs of osteoporotic fractures in elderly men and women.
Osteoporos Int 1995; 5: 427-432.
-
Gray R. Insurance: the long term funding of aged care. National
Healthcare 1998; 8(4): 32-33.
-
Melton L, Atkinson EJ, Madhok R. Downturn in hip fracture
incidence. Public Health Rep 1996; 111 (March/April):
146-150.
-
Black DM, Cummings SR, Karpf DB, et al. Randomised trial of effect
of alendronate on risk of fracture in women with existing vertebral
fractures. Fracture Intervention Trial Research Group.
Lancet 1996; 348: 1535-1541.
-
Jonsson B, Christiansen C, Johnell O, Hedbrandt J.
Cost-effectiveness of fracture prevention in established
osteoporosis. Osteoporos Int 1995; 5: 136-142.
-
Cooper C, Campion G, Melton LJ III. Hip fractures in the elderly: A
world-wide projection. Osteoporos Int 1992; 2: 285-289.
-
Sernbo I, Johnell O. Consequences of a hip fracture: A prospective
study over 1 year. Osteoporos Int 1993; 3: 148-153.
-
Melton LJI, O'Fallon WM, Riggs BL. Secular trends in the incidence
of hip fractures. Calcif Tissue Int 1987; 41: 57-64.
-
Bacon W. Secular trends in hip fracture occurrence and survival:
Age and sex differences. J Aging Health 1996; 8: 538-553.
-
Seeman E. Osteoporosis: trials and tribulations. Am J Med
1997; 103 (2A): 74S-87S.
-
Kanis JA, McCloskey EV. Epidemiology of vertebral osteoporosis.
Bone 1992; 13 Suppl 2: S1-S10.
-
Cooper C, Atkinson EJ, O'Fallon M, Melton L. Incidence of
clinically diagnosed vertebral fractures: a population-based
study in Rochester, Minnesota, 1985-1989. J Bone Min Res
1992; 7: 221-227.
-
Falch JA, Kaastad TS, Bohler G, et al. Secular increase and
geograpical differences in hip fracture incidence in Norway.
Bone 1993; 14: 643-645.
-
Agnusdei D, Camporeale A, Gerardi D, et al. Trends in the incidence
of hip fracture in Siena, Italy, from 1980 to 1991. Bone 1993;
14: S31-S34.
(Received 13 Nov 1998, accepted 13 Apr 1999)
|
| | Author's Detials |
University of Melbourne Department of Medicine, Barwon Health-The Geelong Hospital, Geelong, VIC
Kerrie M Sanders, MNutrition, PhD, Research Fellow;
Geoffrey C Nicholson, PhD, FRACP, Professor of Medicine;
Julie A Pasco, PhD, Study Coordinator;
Mark A Kotowicz,
FRACP, Senior Lecturer in Medicine.
Department of General Practice and Public Health, The University of
Melbourne, Melbourne, VIC.
Antony M Ugoni, BSc(Hons), Lecturer in Biostatistics.
Austin and Repatriation Medical Centre, Melbourne, VIC.
Ego Seeman, MD, FRACP, Associate Professor of Medicine, The
University of Melbourne.
Reprints will not be available from the authors.
Correspondence: Dr M
A Kotowicz, University Department of Medicine, Barwon
Health-Geelong Hospital, PO Box 281, Geelong, VIC 3220.
Email: m.kotowiczATmedicine.unimelb.edu.au
| |
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au>".
<URL: http://www.mja.com.au/>
|
| |  | | Back to text | | 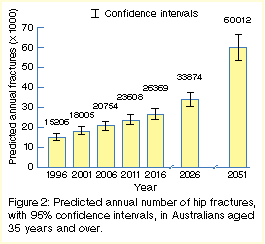 | | Back to text | | 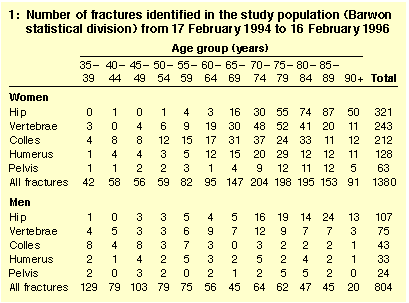 | | Back to text | | 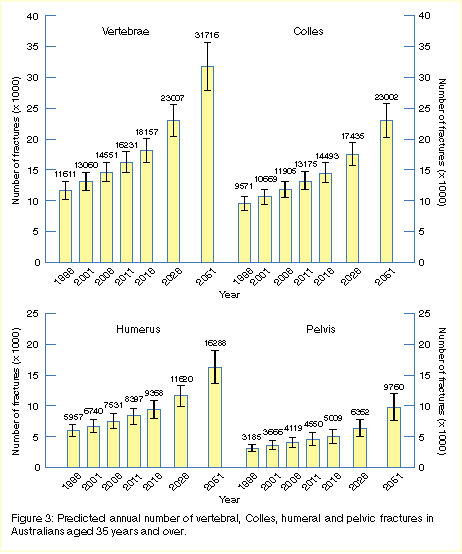 | | Back to text | | 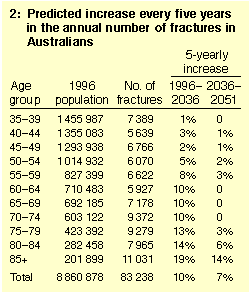 | | Back to text | | 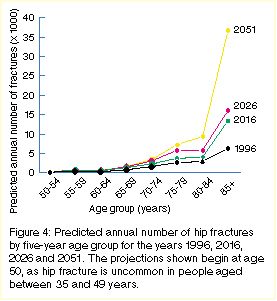 | | Back to text |
|










