Outdoor air pollution and children's respiratory symptoms in the steel cities of New South Wales
Peter R Lewis, Michael J Hensley, John Wlodarczyk, Ruth C Toneguzzi, Victoria J Westley-Wise, Trevor Dunn and Dennis Calvert
MJA 1998; 169: 459-463
For editorial comment, see Abramson & Beer
Abstract -
Introduction -
Methods -
Results -
Discussion -
Acknowledgements -
References -
Authors' details
-
-
More articles on Public and environmental health -
©MJA1998
Abstract
Objective: To investigate the relationship between outdoor air pollution and the respiratory health of children aged 8 to 10 years.Design: A cross-sectional survey (between October 1993 and December 1993) of children's health and home environment. Summary measures of particulate pollution (levels of particles with an aerodynamic diameter less than 10 µm [PM10] each 6th day) and SO2 (daily mean and maximum hourly values) were estimated for each area (using air quality monitoring station data from July 1993 to June 1994).
Setting and survey participants: Parents of 3023 primary school children (Years 3, 4 and 5) from industrial and non-industrial areas with air quality monitoring stations in the Hunter and Illawarra regions of New South Wales.
Main outcome measures: Reported occurrence of four or more chest colds, four or more attacks of wheezing, and night-time cough without a cold for more than two weeks, all within the previous 12 months.
Results: 77% response rate, ranging by area from 66% to 88%. The average annual outdoor air pollution for the nine areas was 18.6-43.7 µg/m3 for PM10 and 0.16-0.90 parts per hundred million for SO2. The proportion of children reported to have the main outcome symptoms were: chest colds, 3.0%-9.7%; night cough, 12.3%-30.5%; and wheeze, 3.4%-11.3%. There was no significant association with SO2, but a significant increase in the odds of symptoms per 10 µg/m3 increase in PM10 on chest colds (odds ratio [OR], 1.43; 95% confidence interval [CI], 1.12-1.82) and night-time cough (OR, 1.34; 95% CI, 1.19-1.53), but not wheeze. Passive smoking was significantly associated with chest colds but not with the other symptoms. Maternal allergy was associated with all three respiratory symptoms, most strongly with wheeze.
Conclusion: These results provide evidence of health effects at lower than expected levels of outdoor air pollution in the Australian setting. They also suggest differences in contributions of environmental and hereditary factors to cough and chest colds compared with wheeze.
Introduction
The effect of outdoor air pollution on the respiratory system has been investigated and reviewed often.1,2 Various health outcomes have been studied; for example, the relationship between exposure to elevated sulfur dioxide, total suspended particulates (TSP) and respiratory symptoms;3 the association between increased air pollution and hospital admissions for asthma;4,5 and studies of air pollution and mortality.6,7 These studies consistently report associations between air pollution and health outcomes, and illustrate the coherence of effects8 across the range of outcomes.There have been few studies of the relationship between air quality and health in Australia. Studies of asthma in school children living near power stations in the Hunter region of New South Wales had very low levels of exposure and lacked the power to detect small associations.9,10 Other studies in south-eastern Australia confirmed the high prevalence of asthma in Australia but had no exposure measures.11-13
The lower Hunter and Illawarra regions of New South Wales are on the coast, about 150 km north and 80 km south of Sydney, respectively. The main cities are Newcastle, in the Hunter region, and Wollongong, in the Illawarra region. The estimated resident populations in 1993 for Newcastle and Wollongong were 451 100 and 248 700, respectively.14 Both regions have fully integrated steelworks, combining coke ovens, blast furnaces, steel-making vessels and rolling mills, and the main pollutants are coke oven gases, blast furnace gases and particulates. In addition, lead smelting occurs in the Hunter region, and copper smelting in the Illawarra region.
The Hunter Illawarra Study of Airways and Air Pollution (HISAAP) arose out of longstanding community concerns about the health effects of air pollution near heavy industry in Newcastle and Wollongong. The generalisability of overseas studies to Australia was not known, because of differences in climate, geography, population and pollution sources. Public health workers need local data to initiate action on air quality at the community level and to formulate air quality guidelines.
This study, the first part of HISAAP, investigated the association between outdoor air quality, as particulates and sulfur dioxide, and respiratory symptoms among primary school children.
Methods
The study was a cross-sectional survey to measure the prevalence of respiratory and atopic symptoms among primary school children and relate these to measures of ambient air quality.
Study areas
To make best use of resources, study areas were selected on the basis of existing or proposed air quality monitoring stations. In the lower Hunter region, the study areas close to industrial sources of air pollution were North Lake Macquarie, Mayfield and Stockton, and distant areas were Beresfield and Wallsend (Figure 1a). In the Illawarra region, we estimated that there would be an increasing gradient of exposure to air pollution, from Wollongong, to Albion Park, Kembla Grange and Port Kembla (Figure 1b).
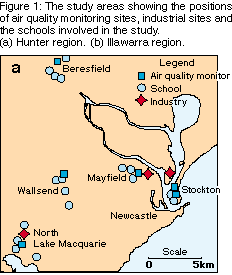
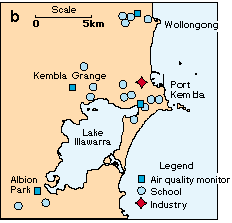
Wallsend, Beresfield, Wollongong and Albion Park were expected to have background levels of air pollution. We were able to compare these multiple control areas with those areas close to point sources of air pollution.
Sampling strategy
All primary schools within a three-kilometre radius of the air quality monitoring sites were approached to be involved in the study. The sampling frame included all children in Years 3 and 4, aged 8 to 10 years, whose parents or guardians approved their child's participation. In areas that had small numbers of children, children in Year 5 were included. We aimed to enrol about 300 children in each of the nine areas.
Questionnaire
Our questionnaire incorporated features used by previous investigators in the Hunter region and NSW,9,11,12 the International Study of Asthma and Allergies in Childhood,15 the American Thoracic Society questionnaire16 and the Six Cities study.17 It addressed demographic data and parental education; child's health (cough, chest colds, wheeze) and atopic symptoms (hayfever, eczema); child's use of respiratory medications; family's symptoms; and home environmental factors (indoor smoking, heating, cooking, carpets, cats). The questionnaire was piloted in both regions.18The primary health outcomes were night-time cough, chest colds and frequent wheeze. They were the responses to the following questions:
- In the last 12 months has your child had a
dry cough at night, apart from a cough with a cold or chest infection? If
yes, has this cough lasted for more than 2 weeks?
- In the last 12 months how many chest colds did your child have? . . . 4 or
more chest colds.
- How many attacks of wheezing has your child had in the last 12 months? . . . 4 or more attacks.
Exposure to indoor tobacco smoke was assessed by asking whether the respondent, other adult or any other person smoked cigarettes inside the home.
The survey was conducted from October 1993 to December 1993. Children received consent forms and questionnaires at school. Parents completed the questionnaires, and children returned them to their teachers. If a questionnaire was not returned after two weeks, a copy was posted to the parents for completion and return by reply-paid post.
Exposure measurement
The lower Hunter and Illawarra Air Pollution Monitoring Networks19 consist of sites operated by the Environment Protection Authority (EPA) and industry self-monitoring sites audited by the EPA. Particulate and sulfur dioxide measures were collected for all study areas, from January 1993 to December 1994. As air pollution data were incomplete for some sites in 1993, the goal was to have representative data for 12 consecutive months close to the reference period of the questionnaire (the 1993 calendar year). The most complete data were found to be from July 1993 to June 1994. Sensitivity analyses using data from adjacent 12-month periods showed very little effect on the results.Particulate pollution as PM10 (particles with an aerodynamic diameter less than 10 µm) was measured for 24 hours every sixth day using high volume air samplers with a size-selective inlet, and these measures were averaged over the 12 months. North Lake Macquarie, Mayfield and Stockton measured only TSP, so local data in which both TSP and PM10 were measured for shorter periods20,21 were used to derive a conversion factor to PM10. In North Lake Macquarie, PM10 was estimated to be 60% of TSP, close to the value used by others.22 In Mayfield and Stockton, PM10 was estimated to be 45% of TSP.
Sulfur dioxide measurements were obtained hourly using pulsed fluorescent spectrophotometry. Twelve-month averages of the daily maximum values and of the daily mean values were calculated.
There were no major trends in air pollution during this time. Seasonal changes did not affect the relative ranking of the areas in terms of air pollution.
Analysis
We used SAS software for the analysis.23 Descriptive statistics were produced for participation rates, health measures and environmental measures for each of the nine study areas.Logistic regression analysis using generalised estimating equations (GEEs) was used to model the reported symptom (outcome variable) on the following explanatory variables: PM10 and sulfur dioxide measures, unflued gas heating, adults smoking inside the home, indoor cats, age, sex, and maternal allergy.24 The level of clustering for this analysis was the school (ie, clusters of children within schools), with 35 schools in the study. Although schools were also clustered within study areas, area was not chosen as the clustering level because of the allocation of exposure measure by area.
Ethical approval
The study received ethical approval from the NSW Education Department, the Regional Catholic Education Office, and the Ethics Committees of the Hunter Area Health Service, the University of Newcastle, the Illawarra Area Health Service, and the University of Wollongong.
Results
Subjects
Questionnaires were given to 3023 primary school children -- 1554 children (from 18 schools) in the Hunter region, and 1469 (from 17 schools) in the Illawarra region. In the Hunter region, 1284 (82%) questionnaires were returned, and in the Illawarra region 1056 (72%) were returned. There were no significant differences in age and sex profiles across the study areas (Table 1).
Respiratory symptoms
About a quarter of the children were reported to have had at least one of the primary respiratory symptoms in the preceding 12 months (Table 2). While some areas with high proportions of children with symptoms were close to industry (Mayfield and Stockton with children having chest colds), this was not a consistent pattern (Beresfield and children with night cough). The proportion of children who had ever been diagnosed with asthma ranged from 17.4% to 38.4%.
Home environment and outdoor air pollution
Depending on the study area, a third to half of the children lived in homes where one or more adults smoked cigarettes in the home (Table 3). The proportion of children in homes with gas heating that did not have a flue to the outside varied greatly between the areas.The levels of particulate pollution in Mayfield and Stockton approached the US EPA standard for PM10 of 50 µg/m3 (annual mean) (Table 3) and the Australian standard, at that time set for TSP at 90 µg/m3 (annual mean). The annual mean sulfur dioxide levels (daily means) were below the Australian standard of 2 parts per hundred million (annual mean).19 Within study areas, particulate levels were not necessarily high in high sulfur dioxide areas, and vice-versa.
Scatter plots of primary health outcomes by air quality measures suggested some positive associations between PM10 and both night cough and chest colds (Figure 2).
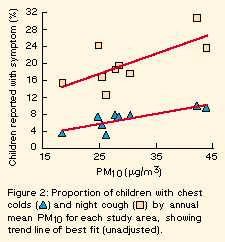
Generalised estimating equation analysis
For each 10 µg/m3 increase in annual mean PM10, children were 43% more likely to be reported as having four or more chest colds (odds ratio [OR], 1.43; 95% confidence interval [CI], 1.12-1.82). The approximate difference in particulate pollution between the area with the highest PM10 level and the area with the lowest was 25 µg/m3, and children were 144% more likely to be reported to have frequent chest colds per 25 µg/m3 increase in annual mean PM10 (OR, 2.44; 95% CI, 1.33-4.49).There was a consistent significant association between particulate pollution and symptoms of night cough and chest colds (Table 4). No association was found between sulfur dioxide and the three respiratory symptoms. An adult smoking in the home was associated with chest colds, and unflued gas heating was associated with frequent wheeze. Boys were more likely to experience frequent wheeze, and there was a significant association between increasing age and likelihood of frequent wheeze. Maternal allergy was consistently associated with an increased risk for all health outcomes, but strongest for wheeze.
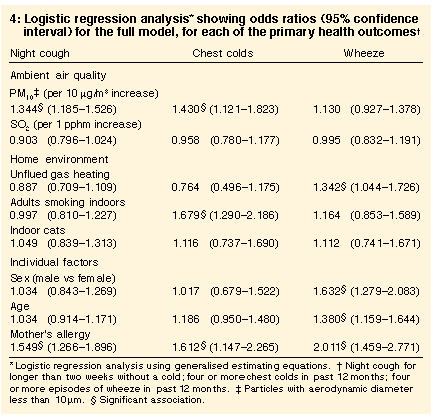
To estimate the possible impact of the two areas with the largest particulate pollution (Mayfield and Stockton, in the Hunter region), the GEE analysis was repeated excluding those areas. There was little change in the coefficients for most variables, including maternal allergy, for each outcome. However, the odds ratio for chest colds per 10 µg/m3 increase in annual mean PM10 increased substantially -- with Mayfield and Stockton excluded, the odds ratio was 2.05 (95% CI, 1.46-2.87), compared with 1.43 for the full dataset.
Discussion
This cross-sectional study of primary school children has shown an important association between relatively low levels of particulate air pollution and respiratory symptoms. The importance is reflected in the finding that the odds ratios for particulates were of the same order as for exposure to indoor tobacco smoke. We found an association with maternal allergy across all three symptom outcomes, but strongest for wheeze.The prevalence estimates of respiratory symptoms are similar to those found in other Australian and New Zealand studies.11-13,25 The association between air pollution and respiratory symptoms in children is also consistent with similar cross-sectional studies from other countries. An Italian study found that children living in polluted areas experienced more cough, rhinitis, pneumonia and early respiratory infections than control subjects,26 but that study did not measure actual air pollution exposure. A British study found that children were more likely to miss school because of respiratory symptoms of cough and wheeze if their school was exposed to a higher coal dust burden (OR, 1.55; 95% CI, 1.17-2.06).27 Our results are directly comparable with those of the Six Cities and 24 Communities studies in North America;17,28,29 effects of particulate pollution on respiratory symptoms and effects of indoor smoking were of the same order in those studies and ours.
Two results of particular note are the relationship between frequent wheeze and age, and the effect of removing from the analysis the areas with the highest particulate pollution. The increase in wheeze with age is quite large (OR, 1.38 per year). Stratified analysis revealed similar coefficients for younger and older age groups, suggesting that a sampling bias may explain the strength of the relationship. The substantial increase in the odds ratio of particulate pollution and chest colds after removal of the areas with highest PM10 suggests that the dose-response curve for particulate pollution and chest colds is curvilinear and much steeper at lower pollution levels.
Potential limitations of our study include possible reporting bias by residents of industrial areas and the variability in the measurement methods for particulate air pollution. It is not possible to estimate the level of possible reporting bias, but its effect may be reduced by selection bias in that families with children with lung disease may not come to, or may leave, polluted areas. The difference in measurement of particulates was unavoidable. A subsequent diary study obtained comparisons of TSP and PM10 which provided evidence on which to convert the measures for local conditions.20,21
Particularly striking are the results which show differences in the determinants of wheeze compared with coughs and colds. While maternal allergy played a part in all, passive smoking was restricted to colds, and particulates to coughs and colds. This suggests differences in underlying pathology which deserve further exploration.
Our data lead us to question the current air quality standards, which are based on the premise that levels at or below recommended ambient levels are not likely to produce a clinically important effect. In particular, recommended levels do not consider increased individual sensitivity caused by a disease such as asthma.
While this study cannot infer causation, it adds to other local and overseas work that increasingly indicates the role of air pollution in respiratory health -- alone and synergistically with other aeroallergens.30 This information contributes to the review of Australian air quality guidelines, and to the broader societal debate about lifestyle, transport and energy consumption. Individuals, communities, industry and organisations need to reassess their environmental performance not only for the environment, but also for health.
Acknowledgements
Our thanks to members of the following organisations which supported the study: Newcastle Environmental Toxicology Research Unit (especially Randall Robertson and Julie Holt), University of Newcastle, Hunter Public Health Unit, Hunter Area Pathology Service, Newcastle City Council, Lake Macquarie Council, Illawarra Public Health Unit, University of Wollongong, NSW Health Department, NSW Environment Protection Authority, Australian Nuclear Science and Technology Organisation, BHP (Newcastle and Port Kembla), Incitec, Pasminco Metals Sulphide, Southern Copper. We are grateful to the schools, parents, and children who participated in this study. HISAAP was partly funded by the NSW Health Department as part of its Health and Air Research Program. Dr P Lewis received an NHMRC Public Health Fellowship for two years.References
- Committee on the Medical Effects of Air Pollution. Asthma and outdoor air pollution. London: HMSO, 1995.
- Committee of the Environmental and Occupational Health Assembly of the American Thoracic Society. Health effects of outdoor air pollution. Am J Respir Crit Care Med 1996; 153: 3-50.
- Lunn FE, Knowelden J, Handyside AJ. Patterns of respiratory illness in Sheffield infant schoolchildren. Br J Prev Soc Med 1967; 21: 7-16.
- Pope CA III. Respiratory admissions associated with PM10 pollution in Utah, Salt Lake and Cache Valleys. Arch Environ Health 1991; 46: 90-97.
- Bates DV, Baker-Anderson M, Sizto R. Asthma attack periodicity: a study of hospital emergency visits in Vancouver. Environ Res 1990; 51: 51-70.
- Anderson HR, Ponce de Leon A, Bland JM, et al. Air pollution and daily mortality in London: 1987-92. BMJ 1996; 312: 665-669.
- Dockery DW, Pope CA III, Xu X, et al. An association between air pollution and mortality in six US cities. N Engl J Med 1993; 329: 1753-1759.
- Bates DV. Health indices of the adverse effects of air pollution: the question of coherence. Environ Res 1992; 59: 336-349.
- Henry RL, Abramson R, Adler JA, et al. Asthma in the vicinity of power stations: I. A prevalence study. Pediatr Pulmonol 1991; 11: 127-133.
- Henry RL, Bridgman HA, Wlodarczyk J, et al. Asthma in the vicinity of power stations: II. Outdoor air quality and symptoms. Pediatr Pulmonol 1991; 11: 134-140.
- Bauman A, Mitchell CA, Henry RL, et al. Asthma morbidity in Australia: an epidemiological study. Med J Aust 1992; 156: 827-831.
- Peat JK, Toelle BG, Gray EJ, et al. Prevalence and severity of childhood asthma and allergic sensitisation in seven climatic regions of New South Wales. Med J Aust 1995; 163: 22-26.
- Robertson CF, Bishop J, Dalton M, et al. Prevalence of asthma in regional Victorian schoolchildren. Med J Aust 1992; 156: 831-833.
- Australian Bureau of Statistics. Regional population growth 1991 and 1996. Canberra: ABS, 1997. (Catalogue No. 3218.0.)
- Asher M, Keil U, Anderson H. International study of asthma and allergies in childhood (ISAAC): rationale and methods. Eur Respir J 1995; 8: 483-491.
- Ferris BG. Epidemiology standardisation project. Part II. Am Rev Respir Dis 1978; 118: 1-53.
- Ware JH, Dockery DW, Spiro A III, et al. Passive smoking, gas cooking and respiratory health of children living in six cities. Am Rev Respir Dis 1984; 129: 366-374.
- Lewis PR, Toneguzzi R, Long K, et al. The Hunter Illawarra study of airways and air pollution: refining the process. NSW Public Health Bulletin 1995; 6: 110-112.
- State Pollution Control Commission. Quarterly air quality monitoring report No 4, 1990. Sydney: SPCC, 1992.
- Lewis P, Holt J, Fryer J. Daily particulate monitoring in the Speers Point/Boolaroo area -- Lake Macquarie Research Grant 94-9. Newcastle: University of Newcastle, Newcastle Environmental Toxicology Research Unit, 1997.
- Environment Section, BHP. Mayfield quality control: measures of particulate pollution. BHP, 1995.
- Dockery DW, Pope CA III. Acute respiratory effects of particulate air pollution. Annu Rev Public Health 1994; 15: 107-132.
- SAS for Windows [computer program]. Version 6.03. Cary, North Carolina: SAS Institute, 1988.
- Karim MR. PC version of GEE1 [computer program]. Baltimore: Department of Biostatistics, The Johns Hopkins University, 1989.
- Moyes CD, Waldon J, Ramadas D, et al. Respiratory symptoms and environmental factors in schoolchildren in the Bay of Plenty. N Z Med J 1995; 108: 358-361.
- Corbo GM, Forastiere F, Dell'Orco V, et al. Effects of environment on atopic status and respiratory disorders in children. J Allergy Clin Immunol 1993; 92: 616-623.
- Brabin B, Smith M, Milligan P, et al. Respiratory morbidity in Merseyside schoolchildren exposed to coal dust and air pollution. Arch Dis Child 1994; 70: 305-312.
- Cunningham J, O'Connor GT, Dockery DW, Speizer FE. Environmental tobacco smoke, wheezing and asthma in children in 24 communities. Am J Respir Crit Care Med 1996; 153: 218-224.
- Dockery DW, Speizer FE, Stram DO, et al. Effects of inhalable particles on respiratory health of children. Am Rev Respir Dis 1989; 139: 587-594.
- Devalia JL, Rusznak C, Herdman MJ, et al. Effect of nitrogen dioxide and sulphur dioxide on airway response of mild asthmatic patients to allergen inhalation. Lancet 1994; 344: 1668-1671.
(Received 29 Oct 1997, accepted 21 Jul, 1998)
Authors' details
Newcastle Environmental Toxicology Research Unit, University of Newcastle, Newcastle, NSW.Peter R Lewis, MPH, FAFPHM, Public Health Research Fellow;
Michael J Hensley, MB BS, PhD, Director and Professor of Medicine;
John Wlodarczyk, BEc, PhD, Statistician;
Ruth C Toneguzzi, RN, DipClinEpi, Clinical Nurse Specialist.
Illawarra Public Health Unit, Wollongong, NSW.
Victoria Westley-Wise, MPH, FAFPHM, Director;
Trevor
Dunn, GdDipSc(Nursing), MPH(Occ Health), Project Manager.
University of Wollongong, Wollongong, NSW.
Dennis Calvert, MD, FRACP, Professor in Medicine and Public
Health.
Reprints will not be available from the authors.
Correspondence: Dr P
R Lewis, Newcastle Environmental Toxicology Research Unit,
Division of Medicine, John Hunter Hospital, Locked Bag 1, Hunter
Regional Mail Centre, NSW 2310.
E-mail: plewiATdoh.health.nsw.gov.au
-
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au>".
<URL: http://www.mja.com.au/>
Received 25 May 2026, accepted 25 May 2026
- Peter R Lewis
- Michael J Hensley
- John Wlodarczyk
- Ruth C Toneguzzi
- Victoria J Westley-Wise
- Trevor Dunn
- Dennis Calvert




