- The costs of subacute care (palliative care, rehabilitation
medicine, psychogeriatrics, and geriatric evaluation and
management) and non-acute care (nursing home, convalescent and
planned respite care) are not adequately described by existing
casemix classifications.
- The predominant treatment goals in subacute care are enhancement of
quality of life and/or improvement in functional status and, in
non-acute care, maintenance of current health and functional
status.
- A national classification system for this area has now been
developed -- the Australian National Sub-Acute and Non-Acute
Patient Classification System (AN-SNAP).
- The AN-SNAP system, based on analysis of over 30 000 episodes of care,
defines four case types of subacute care (palliative care,
rehabilitation, psychogeriatric care, and geriatric evaluation
and management) and one case type of non-acute care (maintenance
care), and classifies both overnight and ambulatory care.
- The AN-SNAP system reflects the goal of management -- a change in
functional status or improvement in quality of life -- rather than the
patient's diagnosis. It will complement the existing AN-DRG
classification.
Introduction The Australian healthcare system is about to implement a new casemix classification system for subacute and non-acute care, the costs of which are not adequately described by traditional diagnostic tools. Subacute care comprises palliative care, rehabilitation medicine, psychogeriatrics, and geriatric evaluation and management. Non-acute care includes nursing home, convalescent and planned respite care. The new casemix classification system, which includes hospital as well as community care, reflects the goal of management -- a change in functional status or improvement in quality of life -- rather than the underlying patient diagnosis.
Background Subacute casemix has been evolving for 15 years. In 1983, when the United States Health Care Financing Administration decided that payments for hospital care would be on a prospective payment system, based on acute-care diagnosis-related groups (DRGs), rehabilitation, psychiatric, children's and long-term facilities were specifically excluded. It was recognised that these forms of care, although not acute, were still complex and expensive and required long hospital stays.
In 1987, a US Department of Health and Social Services report reiterated that their current DRG system did not adequately take into account the special circumstances of patients requiring long hospital stays.1 Studies in the United States over the following few years not only confirmed that DRGs did not adequately describe costs in one of these areas of care (rehabilitation medicine),2 but that as a consequence quality of care had deteriorated, as measured by changed length of hospital stay, increased readmission rates and a rising number of nursing home admissions.3-5
As casemix development progressed in Australia, Australian studies6-12 also expressed the need for a different approach for costing of rehabilitation,6,8-10,12 geriatric evaluation and management,6,9,12 palliative care7,9,11,12 and psychogeriatrics.6,12
The term subacute care was coined in 199213 to describe "care which is provided for a person who requires health services but whose principal medical diagnosis (modified for factors such as age and procedures) is not adequate in explaining the need for, or the cost of, the services that s/he receives".
Goals of subacute and non-acute care In subacute care the predominant goal is enhancement of a patient's quality of life and/or improvement in his or her functional status. In non-acute care the predominant goal is maintenance of a patient's current health and functional status. Because of this difference in goals, it was expected that factors other than diagnosis were more likely to explain the costs of these forms of care.
Rehabilitation: Factors contributing to the success of rehabilitation programs have included patient characteristics such as functional status on admission, age, disease site, time from referral to beginning of program, comorbidities such as cognitive function and depression, and availability of resources.14-16 The factor which appears in US and Australian studies to predict cost most accurately in these areas of care is a patient's functional status on admission.12,15-17
Palliative care: Australian clinicians were instrumental in developing a casemix classification system with a primary approach from a clinical perspective. The development involved broad consultation and collaboration. The palliative care classification identified stage of illness or palliative care phase (eg, stable, deteriorating, terminal), symptom severity and acuity level (or nursing dependency) as the major factors explaining costs for this form of care.7
Psychogeriatrics and other aged care: The goals of admission in aged care are improving health status, modifying symptoms and enhancing function, living conditions, behaviour and quality of life.12
Subacute and non-acute care classifications Several classification systems for subacute and non-acute episodes of care have been developed, including the Resource Utilisation Groups and the California Long Term Care System.18 The Resident Classification Index19 is an Australian classification system used in nursing homes to classify non-acute episodes of care. In the United States the FIM-FRG system (Functional Independence Measure- Function Related Groups)17 for rehabilitation medicine is the most developed.
Studies in Australia have continued to demonstrate that the best predictor of cost for subacute care is the goal of care. The most recent studies are the 1995 Victorian Rehabilitation Casemix Report10 and the 1996 NSW Sub-Acute Casemix Area Network Project.12
AN-SNAP study The Australian National Sub-Acute and Non-Acute Patient Casemix Study20 was conducted in 1996 in 99 hospital and community health sites in all Australian States and Territories and in five sites in New Zealand. Over 30 000 episodes of care were analysed, including overnight, same day, outpatient and community episodes of care.
The study established that there are five case types of subacute and non-acute care. Subacute care includes palliative care, rehabilitation, psychogeriatric care, and geriatric evaluation and management; and the final case type -- maintenance care -- is defined as non-acute care. Each of the five case types is defined according to the characteristics of the patient and the goal of care, and not the institution or service in which she or he is treated (eg, a patient may receive geriatric evaluation and management in a hospice, or palliative care in a rehabilitation unit).
A critical finding of the study was that across the spectrum of case types and classes there is significant diversity in the cost of subacute and non-acute care for both overnight and ambulatory episodes. For example, there is a 30-fold variation in episode cost and a five-fold variation in per diem cost between the most expensive and the least expensive classes in the overnight classification, thus confirming the necessity for a classification in this area to allow for appropriate output-based funding.
AN-SNAP classification system From the study, a national classification for subacute and non-acute care was developed -- the Australian National Sub-Acute and Non-Acute Patient Casemix Classification System, or AN-SNAP classification.20
AN-SNAP version 1 (Box 1)21 classifies both overnight and ambulatory care. It has 134 classes and the classification explains 58% of the variation in all episode costs. Of this 58%, 21% is contributed by episode type and 37% by the classes. The overnight branch has 66 classes and the classification explains 47% of the variance in the cost of overnight care. The ambulatory branch has 68 classes and the classification explains 28% of the variance in the cost of ambulatory care. These results are an improvement on the performance achieved by acute-care DRGs.
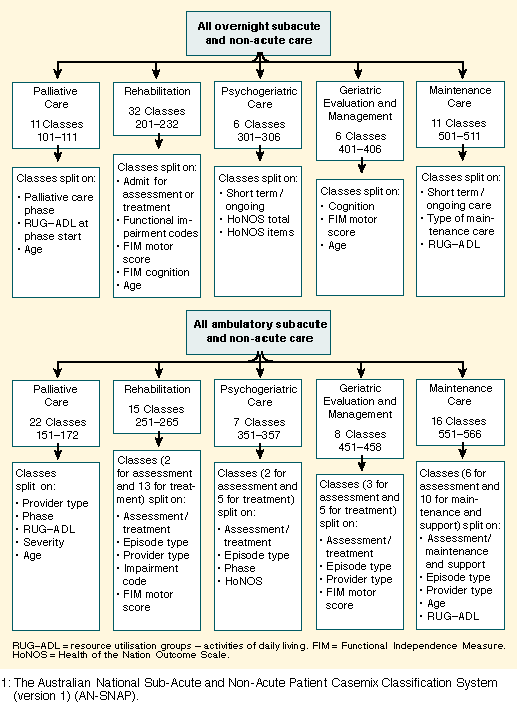
Analysis of the decision trees for overnight and ambulatory care in Box 1 shows the factors which have been incorporated into the system as predictors of cost.
- Palliative care -- phase, functional dependence as measured by
RUG-ADL (resource utilisation groups - activities of daily
living),18 and age;
- Rehabilitation -- impairment groupings, functional status as
measured by FIM (Functional Independence Measure),22 and age;
- Psychogeriatrics -- psychiatric symptom severity and functional
status as measured by the HoNOS (Health of the Nation Outcome
Scale);23
- Geriatric evaluation and management -- cognitive status in
addition to motor capacity and age; and
- Maintenance care -- functional status.
The AN-SNAP study showed that the variables driving costs in the inpatient setting are also important cost drivers in the ambulatory setting. However, community care is inherently more complex than institutional care. Common variables across institutional and community care are necessary, but are insufficient in explaining cost variations. In consequence, the classification makes use of some community variables not required in institution care (eg, provider type and assessment or treatment episode).
Implications of AN-SNAP The implementation of this classification has important implications. Firstly, a number of classifications are now available in Australia and policy decisions on the interaction between these classifications are required. Secondly, data on many of the characteristics used in AN-SNAP are currently collected by individual service providers, but most are not routinely collected by existing hospital and community information systems.
AN-SNAP, along with its further development, has been endorsed by the Australian Casemix Clinical Committee for adoption as the national classification for sub- and non-acute care. Implementation remains a State and Territory issue which requires a planned, staged approach.
Already some States, including Queensland and New South Wales, are implementing AN-SNAP, and others have indicated their intention to do so in the near future. The adoption of the system will complement the existing DRG system, as illustrated in the New South Wales approach (Box 2).
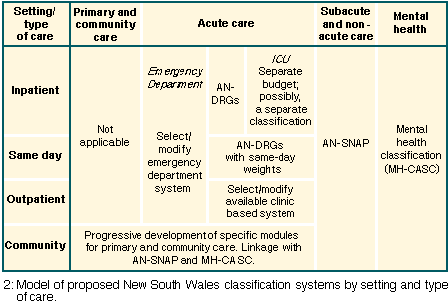
References
- Batavia AI, DeJong G. Prospective payment for medical rehabilitation: the DHSS Report to Congress. Arch Phys Med Rehabil 1988; 69: 377-380.
- Stineman MG, Escarce JJ, Goin HE, et al. A case-mix classification system for medical rehabilitation. Med Care 1994; 32: 366-379.
- Evans RL, Hendricks RD, Bishop DS, et al. Prospective payment for rehabilitation: effects on hospital readmission, home care and placement. Arch Phys Med Rehabil 1990; 71: 291-294.
- Fitzgerald JF, Fagan LF, Tierney WM, Dittus RS. Changing patterns of hip fracture care before and after implementation of the prospective payment system. JAMA 1987; 258: 218-221.
- Heinemann AW, Billeter J, Betts HB. Prospective payment for acute care: impact on rehabilitation hospitals. Arch Phys Med Rehabil 1988; 69: 614-618.
- Roberts R, McKinley S, Brooks B, et al. The Australian National Non-Acute Inpatient Project. Aust Health Rev 1993; 16: 300-319.
- Smith M, Firms P. Palliative Care Casemix Classification -- testing a model in a variety of palliative care settings -- preliminary results. Proceedings of the Sixth Australian Casemix Conference; 1994 Aug 29-31; Hobart. Canberra: Commonwealth Department of Human Services and Health, 1994.
- Baker W. Casemix in rehabilitation -- is it safe to dip into functionally related groups? Proceedings of the Sixth Australian Casemix Conference; 1994 Aug 29-31; Hobart. Canberra: Commonwealth Department of Human Services and Health, 1994.
- Lee L, Goor E, Kennedy C, et al. Non-acute casemix in the Illawarra. J Qual Clin Pract 1994; 14: 23-30.
- Coopers & Lybrand. Rehabilitation Casemix Project. Final Report. Melbourne: Victorian Department of Health and Community Services, 1995.
- Hindle D. The Victorian Palliative Care casemix project: statistical analysis and funding recommendations. Wollongong: Centre for Health Service Development, University of Wollongong, 1995.
- Eagar K, Cromwell D, Kennedy C, Lee L. Classifying sub-acute and non-acute patients: results of the NSW Casemix Area Network Study. Aust Health Rev 1997; 20: 56-74.
- Eagar K, Innes K. Standard definitions and source data for hospitals in Australia, Canberra: Commonwealth Department of Health, Housing and Community Service, 1992.
- Carey RG, Posavac EJ. Who makes the most progress in inpatient rehabilitation? An analysis of functional gain. Arch Phys Med Rehabil 1988; 69: 337-343.
- Rondinelli RD, Murphy JR, Wilson DH, et al. Predictors of functional outcome and resource utilisation in inpatient rehabilitation. Arch Phys Med Rehabil 1991; 72: 447-453.
- Stineman MG, Escarce JJ. Analysis of casemix and the prediction of resource use in medical rehabilitation. Phys Med Rehabil Clin North Am 1993: 4: 451-461.
- Stineman MG, Escarce JJ, Goin HE, et al. A case-mix classification system for medical rehabilitation. Med Care 1994; 32: 366-379.
- Fries BE, Cooney LM. Resource Utilisation Groups: a patient classification system for long term care. Med Care 1985; 23: 110-132.
- Commonwealth Department of Health, Housing and Community Services. Classification of nursing home residents. Handbook for directors of nursing. Canberra: DHHCS, 1992.
- Eagar K, et al. The Australian National Sub-Acute and Non-Acute Patient Classification (AN-SNAP): report of the National Sub-Acute and Non-Acute Casemix Classification Study. Wollongong: Centre for Health Service Development, University of Wollongong, 1997.
- Eagar K. The Australian National Sub-Acute and Non-Acute Patient (AN-SNAP) Casemix Classification. Proceedings of the Ninth Australian Casemix Conference; 1997 Sep 7-10; Brisbane. Canberra: Commonwealth Department Health and Family Services, 1997.
- Center for Functional Assessment Research, Uniform Data Set for Medical Rehabilitation. 1993 Guide to the Uniform Data Set for Medical Rehabilitation (Adult FIM), V4.0. Buffalo: State University of New York, Buffalo, 1993.
- Wing JK, Beevor AS, Curtis RH, et al. Health of the Nation Outcome Scales (HoNOS). Research and development. Br J Psychiatry 1998; 172: 11-18.
Authors' details South Eastern Sydney Area Health Service, Sydney, NSW.
Lynette A Lee, FAFRM, FRACMA, Director Clinical Services.
Centre for Health Service Development, University of Wollongong,
Wollongong, NSW.
Kathy M Eagar, MA(Psych), Associate Professor and Director.
Neringah Palliative Care Service, Sydney, NSW.
Michael C Smith, MB BS, MRACMA, Director.
Reprints will not be available from the authors.
Correspondence: Dr L
A Lee, South Eastern Sydney Area Health Service, PO Box 430, Kogarah,
NSW 1485.
E-mail: leelATsesahs.nsw.gov.au




